Quick Check Summary
Core Symptom Checklist
Grab a pen (or your phone) and see if any of these ring true for you:
- Persistent cough that doesnt improve with usual inhalers.
- Wheezing or a tightchest feeling, especially at night or after exercise.
- Shortness of breath on minimal exertion (e.g., climbing a flight of stairs).
- Frequent chest infections or excess mucus production.
- Noticeable drop in response to rescue inhalers.
AirwayRemodeling Symptom Radar
| Symptom | Severity (05) |
|---|---|
| Chronic cough | 0 |
| Wheezing | 0 |
| Shortness of breath | 0 |
| Infection frequency | 0 |
| Inhaler response | 0 |
Score each item based on how often you experience it. A total above 8 usually means its time to chat with a healthcare professional.
Why Symptoms Appear
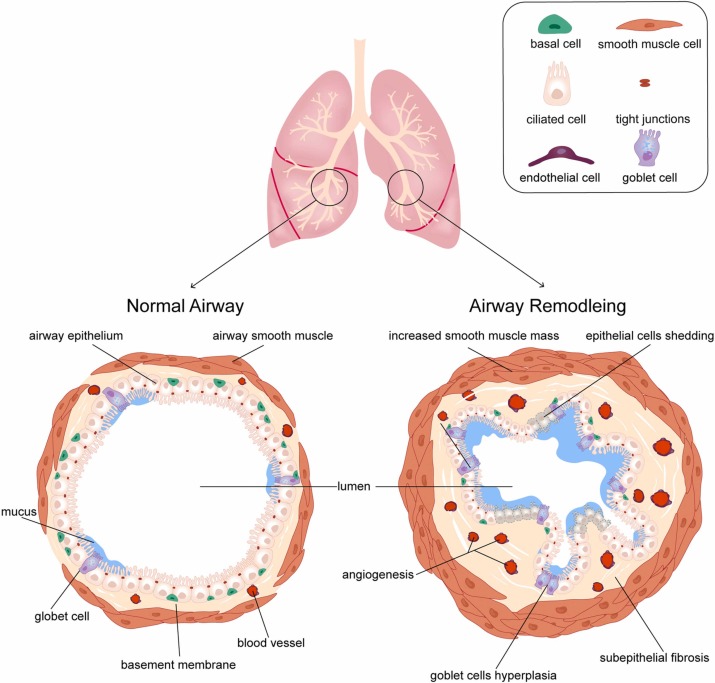
Whats Really Happening Inside Your Lungs?
Imagine your airways as tiny, flexible tubes. In a healthy lung, those tubes stay open, letting air glide in and out effortlessly. With airway remodeling, repeated inflammation makes the walls of those tubes thicker, the smooth muscle tighter, and scarlike tissue builds up. The result? Narrowed passages that trigger the symptoms we just listed.
The Science, Made Simple
Three main changes drive the symptoms:
- Muscle tighteningthe airway smooth muscle contracts more often, causing that classic wheeze.
- Wall thickeningextra collagen and other proteins add bulk, making the airway less flexible.
- Mucus overloadinflamed lining produces more sticky mucus, leading to cough and infections.
According to a recent study , confirming that early detection is key.
RealWorld Insight
Take Anna, a 42yearold teacher who has lived with asthma since her teens. She thought her worsening cough was just a bad cold, but once she noticed the patternespecially the lack of relief from her inhalershe consulted her doctor. The diagnosis? Airway remodeling after years of uncontrolled inflammation. Annas story shows how personal experience can spotlight the need for professional help.
Remodeling In Diseases
Asthma vs. COPD
| Condition | Typical Symptoms | Remodeling Pattern |
|---|---|---|
| Asthma | Cough, wheeze, night-time chest tightness | Smallairway thickening, hyperresponsiveness |
| COPD | Chronic bronchitis, dyspnoea, frequent sputum | Largerairway fibrosis, mucus hypersecretion |
| AsthmaCOPD overlap | Variable, often severe | Combination of both patterns |
What Causes Airway Remodeling in Asthma?
Its a nasty combo of chronic inflammation, repeated flareups, and sometimes, simply not sticking to your medication plan. Allergens, smoke, and viral infections all fan the flames, nudging the airway walls toward permanent change.
Is It Permanent?
Great question! Earlystage remodeling can be slowedor even partially reversedwith aggressive treatment, but once scar tissue builds up, those changes tend to stick around. Thats why catching it early matters.
Impact On Life
ShortTerm Effects
Beyond the obvious breathlessness, many people find that sleep quality drops (those nighttime wheezes are brutal) and daily activities feel like climbing a mountain. You might notice youre reaching for your inhaler more often, which can be stressful.
LongTerm Outlook & Life Expectancy
Research shows that severe, unchecked remodeling can shave a few years off life expectancy, mainly because of chronic respiratory compromise. However, the impact is highly individualgood control can keep you feeling vibrant well into later years.
Practical Tips for Daily Living
- Schedule gentle walking or swimming sessions to improve lung capacity without overexertion.
- Practice breathing techniques (like pursedlip breathing) to ease shortness of breath.
- Keep a symptom diary to spot patterns before they become emergencies.
Diagnosis Basics
How Doctors Confirm Remodeling
Diagnosing isnt just about listening to your wheeze. Doctors often use a mix of tools:
- Highresolution CT scansshow wall thickness and any fibrosis.
- Spirometry trendsa steady decline in FEV over months signals trouble.
- Biomarkerslike periostin or blood eosinophils, which hint at ongoing inflammation.
Questions to Ask Your Provider
Feeling a little nervous? Here are some readymade questions you can bring:
- Can you show me my CT results and explain what they mean for my airway health?
- How often should we repeat spirometry to monitor progression?
- Are there any biomarkers that could guide my treatment plan?
Effective Treatment Options
Pharmacologic Tools
When it comes to taming remodeling, medication is the first line of defense. Heres a quick cheatsheet:
- Inhaled corticosteroids (ICS)the cornerstone; they reduce inflammation and can soften early remodeling.
- Longacting agonists (LABA) + ICS comboshelp keep airways open around the clock.
- Biologics (antiIL5, antiIL4R)target specific immune pathways; studies show they can blunt structural changes in severe asthma.
NonPharmacologic Strategies
Medication alone isnt enough if you keep exposing your lungs to irritants. Consider these lifestyle moves:
- Quit smoking (or avoid secondhand smoke like the plague).
- Identify and steer clear of personal allergensdust mites, pet dander, pollen.
- Enroll in a pulmonary rehabilitation program; the guided exercise and education boost lung efficiency.
Comparison: Standard meds vs. Biologics
| Feature | Standard Inhalers | Biologic Therapy |
|---|---|---|
| Mechanism | Broad antiinflammatory | Targeted immune pathway |
| Effect on Remodeling | Modest, best early | Significant reduction in severe cases |
| Administration | Daily inhalation | Monthly injection/subcutaneous |
| Cost | Lowmoderate | High (often insurancecovered) |
| Sideeffects | Thrush, hoarseness | Injection site reactions, rare infections |
Expert Insight
Dr. Martinez, a boardcertified pulmonologist, always says, Treating remodeling is like renovating a houseyou need to fix the foundation before you paint the walls. His advice underscores the importance of early, aggressive therapy.
Balancing Benefits & Risks
Why Aggressive Therapy Can Be Worth It
When you curb remodeling, you protect lung function, reduce flareups, and improve quality of life. In many cases, patients notice fewer nighttime symptoms and a drop in emergency visits.
Potential Downsides
Highdose steroids can lead to weight gain, bone thinning, or higher blood sugar. Biologics, while powerful, are pricey and can mildly increase infection risk. Thats why a shared decisionmaking conversation with your doctor is essential.
ProsCons Worksheet (Downloadable Idea)
Picture a simple twocolumn table you could fill out: Pros (better breath, fewer attacks) vs. Cons (cost, sideeffects). Having it on paper makes your next appointment feel more purposeful.
Monitoring Your Progress
Daily Symptom Diary
Keep track of three things each day:
- Peak flow reading (if you have a device).
- Severity of cough/wheeze on a 010 scale.
- Any triggers you noticed (smoke, pollen, stress).
This habit not only spots trends early but also arm you with concrete data when you talk to your clinician.
When to Call the Doctor
- Sudden increase in shortness of breath.
- Symptoms persist despite using rescue inhaler.
- More than two infections in a month.
Helpful Tools
There are a handful of reputable mobile apps that let you log peak flow, set medication reminders, and even share the data directly with your provider. recommend using technology to empower patients. For people with chronic lung conditions like cystic fibrosis, following guidance on cystic fibrosis safety can also help reduce exposure risks and protect fragile airways.
Conclusion
Understanding airway remodeling symptoms is the first step toward taking control of your breathing again. Those lingering coughs and wheezes arent just in your headtheyre signals that your airways are changing, and you have the power to influence that change. By recognizing the signs early, getting a solid diagnosis, and pairing proven treatments with lifestyle tweaks, you can protect your lungs, improve daily comfort, and keep your life expectancy on track. If anything here resonated with you, consider chatting with a respiratory specialist and start a symptom diary today. You deserve breath that feels easy, not a constant battle.