Hey there, friend. If youve ever felt a sudden tingle around your mouth, muscle cramps out of nowhere, or a racing heartbeat that just wont calm down, you might be wondering whats going on. Those odd sensations can be your bodys SOS for dangerously low calcium levels symptoms. In this friendly guide well break down what those symptoms look like, why they happen, and what you can do right now to stay safe and feel better.
Quick Overview Guide
What counts as dangerously low calcium?
Normal total serum calcium in the blood usually sits between 8.510.5mg/dL. When it drifts below 7.5mg/dL, doctors start calling it severe or dangerously low. The sweet spot for borderline low is roughly 8.08.4mg/dL. These numbers matter because the bodys nerves, muscles, and heart all rely on calcium to keep the rhythm right.
Why should you care?
Calcium isnt just the stuff that builds strong bonesits the spark that lets every nerve fire and every muscle contract. When levels dip too far, you can get everything from harmless tingling to lifethreatening heart arrhythmias. Knowing the warning signs means you can get help before a small problem turns into a medical emergency.
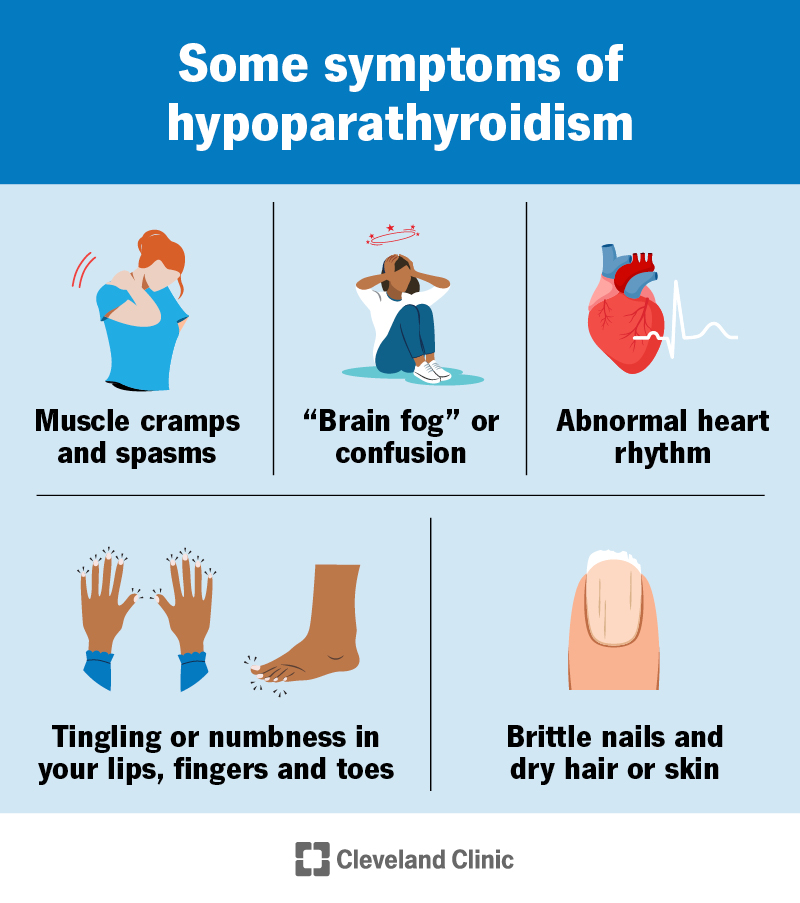
Key Symptoms Overview
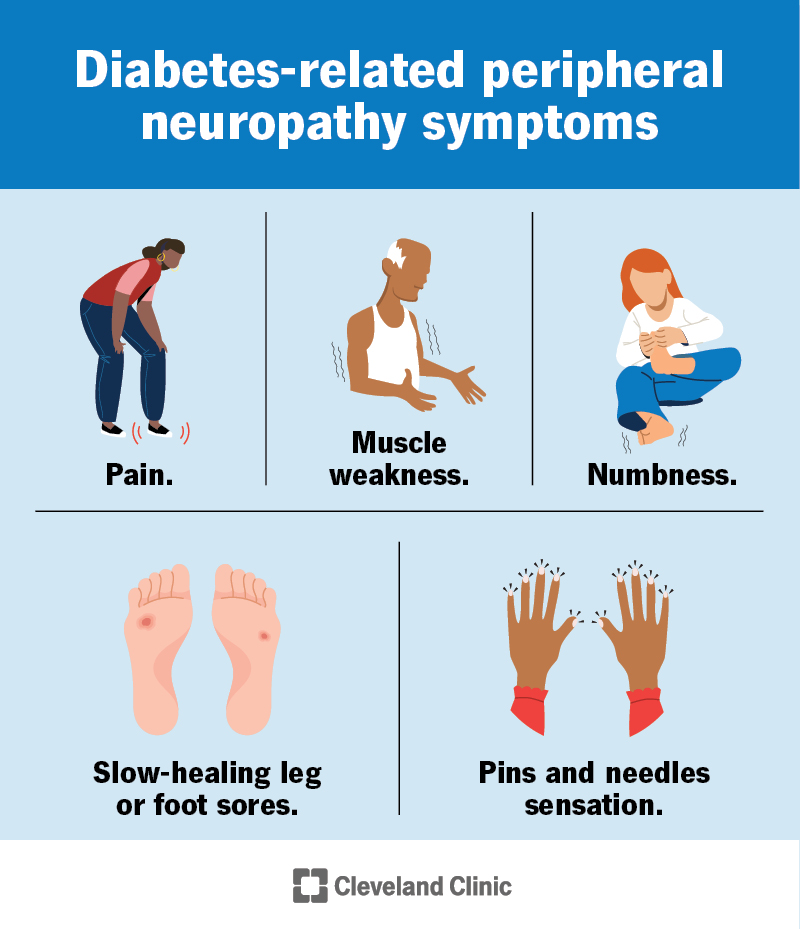
Tingling & Paresthesia
Imagine that little pinsandneedles feeling you get when a foot falls asleepbut it shows up around your lips, fingertips, and toes. Thats a classic sign of low calcium. Many people describe it as a buzz or electric shock that pops up out of nowhere.
Realworld snapshot
Sarah, a 42yearold graphic designer, thought the sensation was just anxiety. One morning she woke up with a constant buzz around her mouth, and a quick blood test revealed a calcium level of 7.2mg/dL. Once she started calcium supplements, the tingling faded within a week.
Muscle Cramps, Spasms & Tetany
Sudden, painful cramps in the calves, back, or arms are another red flag. In severe cases, involuntary muscle contractionscalled tetanycan cause the hands to curl into a clawlike position.
What you might see
Picture yourself reaching for a coffee mug and your fingers stiffen as if theyre holding an invisible rope. Thats tetany, and it signals the nervous system is screaming for more calcium.
Cardiac Effects Arrhythmia & Palpitations
The heart loves calcium because it helps the muscle contract in a coordinated way. When calcium drops, you might feel fluttering or notice an irregular beat. On an ECG, doctors often spot a prolonged QT intervala sign that the hearts electrical system is out of sync.
Quick check
If you ever feel your heart skip a beat while also experiencing tingling or cramps, treat it as a warning and seek medical care right away.
Neurologic & Cognitive Signs
Low calcium can cloud your thinking, cause mild confusion, or even trigger seizures in extreme cases. Mood shiftslike sudden irritability or anxietycan also be linked to calcium imbalances.
Personal story
Tom, 68, thought his forgetfulness was just agerelated. After a fall that left him with a wrist fracture, blood work showed a calcium level of 7.4mg/dL. With vitaminD and calcium therapy, his mental clarity improved noticeably within a month.
Dermatologic Clues
Though less dramatic, brittle nails, dry skin, and hair loss sometimes accompany calcium deficiency. These clues are subtle, but when they appear alongside the other symptoms they add valuable pieces to the puzzle.
Typical Causes Explained
Primary medical conditions
Several health issues can knock calcium out of balance:
- Hypoparathyroidismoften after thyroid surgery or due to autoimmune damage.
- VitaminD deficiencywithout enough vitaminD your gut cant absorb calcium well ().
- Chronic kidney diseasethe kidneys cant convert vitaminD to its active form, limiting calcium absorption.
Medications & Lifestyle
Some drugs are sneaky calcium thieves:
- Loop diuretics (e.g., furosemide) increase calcium loss in urine.
- Bisphosphonates, used for osteoporosis, can sometimes lower blood calcium.
- Highdose phenytoin (an antiseizure medication) interferes with vitaminD metabolism.
Agerelated factors What causes low calcium levels in elderly?
As we get older, our intestines become less efficient at absorbing calcium, we spend less time outdoors getting sunshine, and many seniors juggle multiple medications that can affect calcium balance. All these contribute to a higher risk of dangerously low calcium levels symptoms in the elderly.
Rare but serious red flags Is low calcium a sign of cancer?
In rare cases, cancers like multiple myeloma or certain lung cancers produce substances that mimic parathyroid hormone, pulling calcium out of the blood. If low calcium appears alongside unexplained weight loss, bone pain, or persistent fatigue, a thorough cancer workup might be warranted ().
| Cause | Typical Calcium (mg/dL) | Key Lab Findings |
|---|---|---|
| Hypoparathyroidism | 6.57.5 | Low PTH, low vitaminD |
| VitaminD deficiency | 7.08.2 | Low 25OHvitaminD, normal PTH (early) |
| Chronic kidney disease | 7.58.5 | Elevated phosphorus, low active vitaminD |
| Medicationinduced | 7.89.0 | Depends on drug, often normal PTH |
| Paraneoplastic (cancer) | 6.07.0 | Low PTH, high PTHrelated protein |
What Happens Inside
Physiology snapshot
Calcium acts like a master key for the body:
- Nerve signaling Calcium channels let nerves fire and reset.
- Muscle contraction From a blink to a sprint, calcium bridges the gap.
- Blood clotting Calcium is essential for the cascade that stops bleeding.
When levels dip, each of these processes stutters. Thats why you can feel tingling (nerve issue), cramps (muscle issue), and even a shaky heart (muscle of the heart itself). Understanding this cascade helps you see why a single lab value can cause such a wide range of symptoms.
Diagnosis Basics Guide
Reading the calcium test
When your doctor orders a calcium panel, they usually check total serum calcium. However, total calcium can be misleading if your albumin (a protein) is low. In those cases, doctors apply a correction formula or order an ionized calcium test, which measures the physiologically active fraction.
Complementary labs
To get to the root cause, doctors often request a bundle of tests:
- PTH (parathyroid hormone) High PTH suggests the parathyroids are trying to raise calcium; low PTH points toward hypoparathyroidism.
- 25hydroxyvitaminD Checks vitaminD status.
- Magnesium and phosphorus Imbalances here can also tip calcium levels.
- Renal function (creatinine, eGFR) Kidney disease affects calcium metabolism.
When to repeat testing
If your first result lands in the borderline zone, doctors may repeat the test in a week, especially if youre on supplements or have an acute illness that could temporarily shift calcium. Consistency over multiple draws is key to a solid diagnosis.
Effective Treatment Options
Immediate emergency care
When calcium falls below 7mg/dL and you have severe symptoms (like tetany or cardiac arrhythmia), emergency departments usually give intravenous calcium gluconate. The infusion is carefully monitored with continuous ECG to avoid overcorrection, which could cause the opposite problemhigh calcium.
Shortterm oral supplementation
For milder cases, oral calcium works wonders. Two common forms are:
- Calcium carbonate Best taken with meals because stomach acid helps absorption.
- Calcium citrate Works well even on an empty stomach and is gentler on the stomach.
Typical adult dosing ranges from 1,000mg to 1,500mg of elemental calcium per day, split into two doses for better absorption.
Longterm strategies
Beyond pills, lifestyle tweaks can keep calcium steady:
Diet
Fill your plate with calciumrich foods: dairy (milk, yogurt, cheese), fortified plant milks, leafy greens (kale, bok choy), and canned fish with bones (sardines, salmon).
VitaminD
Sunlight is the cheapest vitaminD sourceabout 1015 minutes of midday sun a few times a week can boost production. If sunlight is limited, a daily supplement of 8001,000IU is often enough, but talk to your doctor for personalized dosing.
Sample 7Day Meal Plan
Heres a quick, friendfriendly menu to hit about 1,200mg of calcium daily:
- Day 1: Breakfast Greek yogurt with berries; Lunch Kale salad with feta; Dinner Baked salmon with broccoli.
- Day 2: Breakfast Fortified almond milk oatmeal; Lunch Sardine sandwich on whole grain; Dinner Stirfried bok choy with tofu.
- Day 3: Breakfast Scrambled eggs with cheese; Lunch Spinach smoothie (milk, banana, chia); Dinner Chicken curry with cauliflower.
- continue similarly for Days 47.
Monitoring & followup
After starting treatment, your doctor will likely check calcium levels every 46 weeks until they stabilize. Adjustments to dosage, diet, or vitaminD intake are common, so keep a symptom journal and bring it to each visit.
Borderline vs Dangerous
When do symptoms outpace the numbers?
Some people feel tingling at a borderline calcium of 8.2mg/dL, while others tolerate a level of 7.8mg/dL without any complaints. Individual sensitivity, concurrent electrolyte imbalances (like low magnesium), and overall health status all play a role.
Redflag moments when to call the doctor or head to the ER
Seek immediate care if you experience any of the following:
- Severe muscle cramps or tetany that wont ease.
- Persistent palpitations, dizziness, or fainting.
- Confusion, seizures, or sudden mood swings.
- Rapid onset of multiple symptoms together.
Even if your lab results are just borderline, these symptoms merit urgent evaluation because they indicate that your bodys calciumdependent systems are under serious stress.
Expert Insights Today
Weve gathered a handful of toptier resources to back up the information here. The offers a clear symptom checklist and treatment algorithm. The breaks down the link between vitaminD and calcium absorption in an easytoread format. Finally, the provides the deepdive physiology that clinicians love.
When you combine these expert voices with realworld stories, the picture becomes crystal clear: dangerously low calcium levels symptoms are a signal, not a trivia fact. Recognizing them early, getting proper testing, and following a balanced treatment plan can keep your heart, nerves, and muscles humming smoothly.
Conclusion
Weve walked through the tingling, the cramps, the racing heart, and the lessobvious skin cluesall the ways your body tells you calcium is running low. Knowing the difference between borderline and dangerous levels, understanding the common culprits (from vitaminD deficiency to medication sideeffects), and taking action with proper testing and treatment can protect you from serious complications.
Now its your turn: have you ever felt any of these symptoms? What did you do next? Share your experience in the comments, download our free symptomtracker checklist, and dont hesitate to reach out to a healthcare professional if anything feels off. Your health is worth the extra minute of awarenesslets keep those calcium levels in the safe zone together.
FAQs
What are the most common early signs of dangerously low calcium levels?
Early signs often include tingling around the mouth and fingertips, muscle cramps, and occasional heart palpitations. These arise because nerves and muscles aren’t receiving enough calcium to fire properly.
How do doctors confirm that calcium levels are dangerously low?
Doctors order a serum calcium test. If total calcium is below 7.5 mg/dL they may repeat the test, check ionized calcium, and add labs such as PTH, vitamin D, magnesium, and phosphorus to find the underlying cause.
When should low calcium be treated as an emergency?
If calcium drops below 7 mg/dL and the person experiences severe muscle tetany, seizures, or cardiac arrhythmias (e.g., prolonged QT), emergency care with IV calcium gluconate is required.
What lifestyle changes can help prevent dangerously low calcium levels?
Include calcium‑rich foods (dairy, fortified plant milks, leafy greens, sardines), get 10‑15 minutes of midday sun a few times a week, and take a vitamin D supplement (800‑1,000 IU daily) if sun exposure is limited.
Can any medications cause dangerously low calcium levels?
Yes. Loop diuretics (e.g., furosemide), high‑dose phenytoin, and some bisphosphonates can increase urinary calcium loss or interfere with vitamin D metabolism, leading to low serum calcium.