Hey there! If youve been Googling cushing syndrome vs cushing disease and feel a little lost, youre not alone. In a nutshell, Cushing disease is just one specific type of Cushing syndromethe kind that comes from a tiny tumor in your pituitary gland that makes way too much ACTH. Everything else that raises cortisol levels falls under the broader umbrella of Cushing syndrome. Knowing this distinction can be the difference between months of frustrating tests and getting the right treatment fast.
Quick Answer Summary
Short answer: Cushing disease = pituitarydriven ACTH excess; Cushing syndrome = any other cause of excess cortisol (adrenal tumors, ectopic ACTH, steroids, etc.).
Why it matters: The cause determines which lab tests youll need, which imaging study is appropriate, and ultimately which treatment will give you the best chance at recovery.
Understanding Cushing Syndrome
What the term really means
Think of Cushing syndrome as a catchall label for anything that leads to high cortisol in the body. Cortisol is the stress hormone that helps us handle emergencies, but when its stuck at high levels all the time, it starts wreaking havocweight gain, high blood pressure, mood swings, you name it.
Common causes (nonpituitary)
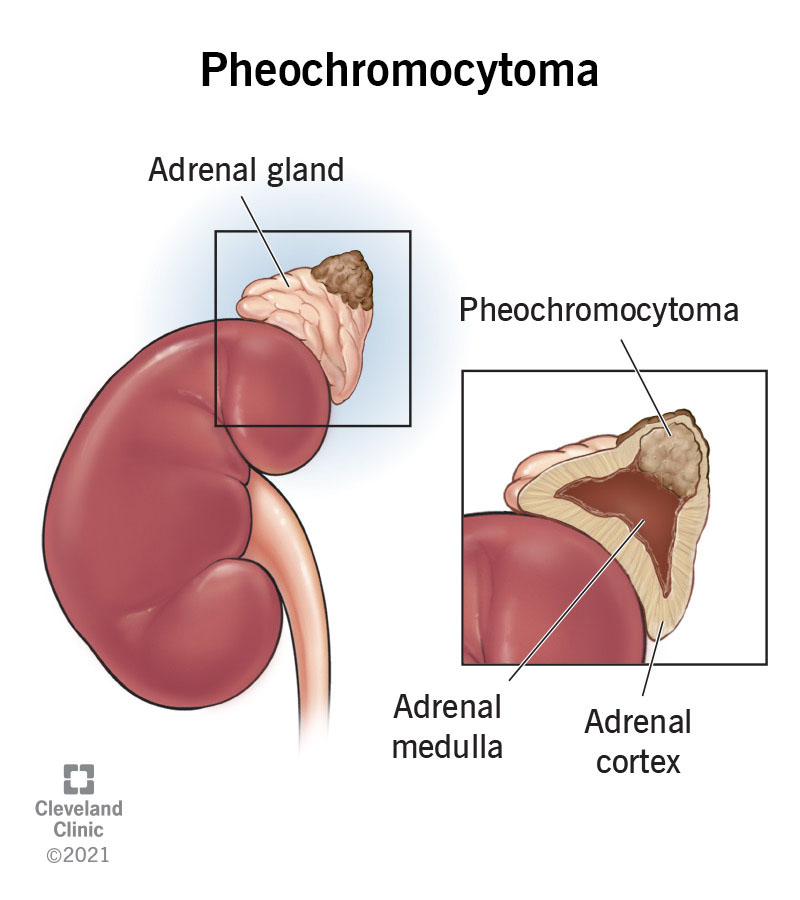
- Adrenal adenoma or carcinoma: A tumor in the adrenal gland makes cortisol on its own, so ACTH (the hormone that usually tells the adrenals what to do) is low.
- Ectopic ACTH secretion: Certain cancers, like smallcell lung cancer or neuroendocrine tumors, produce ACTH outside the pituitary, flooding the adrenals with signals.
- Iatrogenic (exogenous) steroids: Longterm use of prescription steroids (for asthma, arthritis, etc.) can mimic the syndrome perfectly.
Diseases that mimic Cushings syndrome
Not every Cushinglike picture is true Cushing. Conditions such as polycystic ovary syndrome (PCOS), severe depression, alcoholism, and even obesity can produce similar signsthink moon face or buffalo humpbut the hormonal tests look different. Keeping these mimickers in mind prevents unnecessary worry and invasive procedures.
Understanding Cushing Disease
Why the name matters
Cushing disease is a special case of Cushing syndrome where a benign pituitary adenoma (a tiny, noncancerous tumor) secretes excess ACTH. This extra ACTH tells the adrenal glands to pump out more cortisol, leading to the classic symptoms.
How common is it?
About 70% of all endogenous (originating inside the body) Cushing cases are actually Cushing disease. It tends to affect women more often than men, typically in their 20s40s, and many patients notice rapid weight gain or menstrual irregularities as early clues.
Quick fact box
- Typical age of diagnosis: 3045years
- Femaletomale ratio: roughly 3:1
- Success rate of firsttime pituitary surgery: 7085%
Key Symptom Comparison
Both conditions share a core set of signs because they both involve too much cortisol. The differences are subtle but important, especially when you discuss your symptoms with a doctor.
| Feature | Cushing Syndrome (general) | Cushing Disease (pituitary) |
|---|---|---|
| Primary source of ACTH | Variable (adrenal, ectopic, exogenous) | Pituitary adenoma |
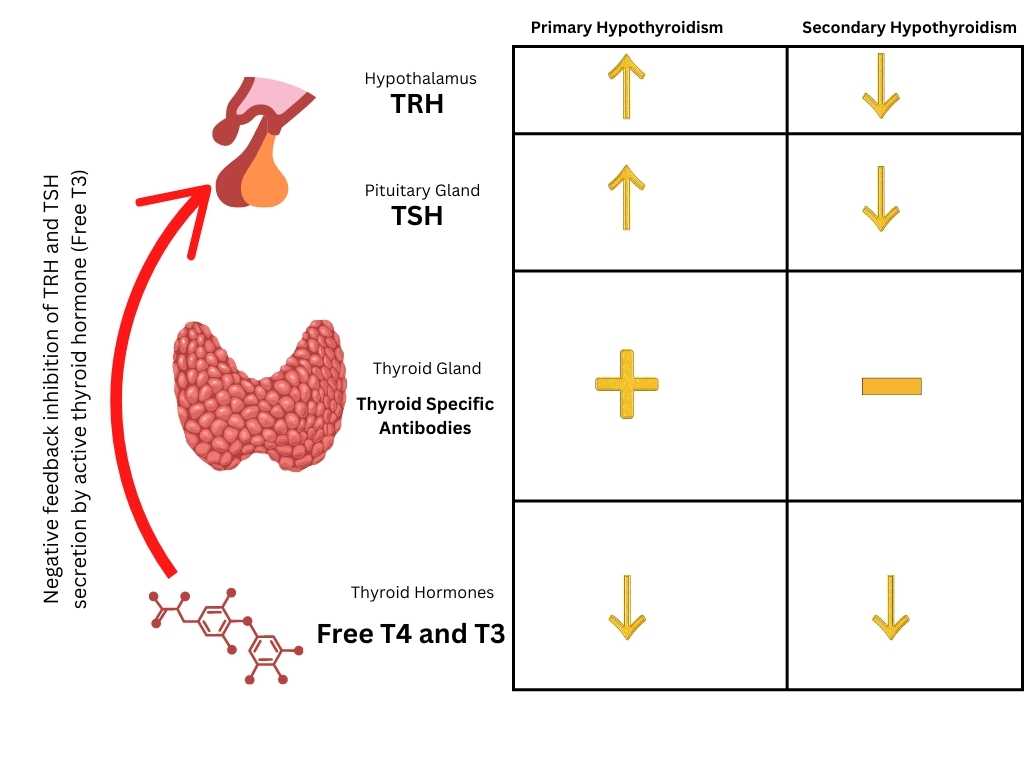
| ACTH level | Low/normal (adrenal) or high (ectopic) | High, but suppressible with highdose dexamethasone |
| Dexamethasone suppression test | No suppression at low or high dose | Suppressed at high dose |
| Common age group | Any age, often older adults | 2040y, female predominance |
| Imaging focus | Adrenal CT/MRI, chest/abdomen for ectopic source | Pituitary MRI |
Notice how the dexamethasone suppression test acts like a detectives magnifying glasspinpointing whether the ACTH surge is coming from the pituitary or elsewhere.
How to Diagnose
Stepbystep algorithm
- Screening tests: 24hour urinary free cortisol, latenight salivary cortisol, or a lowdose dexamethasone suppression test. Any one of these thats abnormal sends you down the diagnostic rabbit hole.
- Measure ACTH: This tells you whether youre dealing with ACTHdependent (Cushing disease or ectopic ACTH) or ACTHindependent (adrenal tumor, exogenous steroids) disease. cushing syndrome vs cushing disease acth is a common search phrase at this stage.
- Highdose dexamethasone test: If ACTH is high, a highdose suppression test helps separate pituitary from ectopic sources.
- Imaging: Pituitary MRI for suspected Cushing disease; adrenal CT for ACTHindependent cases; chest/abdomen CT if ectopic ACTH is on the radar.
- Special procedures: When imaging is equivocal, inferior petrosal sinus sampling (IPSS) can pinpoint pituitary production with remarkable accuracy.
Expert tip
According to the , If the highdose dexamethasone test is inconclusive, IPSS is the gold standard for confirming Cushing disease. Its a mouthful, but essentially it means drawing blood from veins that drain the pituitaryvery clever, very precise.
Effective Treatment Options
Pituitary (Cushing Disease)
- Transsphenoidal surgery: A minimally invasive approach through the nose to remove the tumor. Firstline and offers the highest remission rates.
- Medical adjuncts: Medications like pasireotide, cabergoline, ketoconazole, or metyrapone can control cortisol while waiting for surgery or if surgery isnt curative.
- Radiation therapy: Used for residual tumor tissue or when surgery is not possible.
Other Causes (Cushing Syndrome)
- Adrenal tumor: Laparoscopic adrenalectomy usually cures the problem.
- Ectopic ACTH source: Remove the primary cancer (lung, pancreas, etc.) and manage cortisol spikes with steroidogenesis inhibitors.
- Iatrogenic steroids: Gradual tapering under physician supervision is keynever quit cold turkey.
Quicklookup treatment table
| Treatment | Indication | Typical Success Rate |
|---|---|---|
| Transsphenoidal surgery | Pituitary adenoma (Cushing disease) | 7085% remission |
| Laparoscopic adrenalectomy | Adrenal adenoma/carcinoma | >90% cure |
| Ketoconazole / Metyrapone | Medical control (any cause) | 6070% cortisol reduction |
| Radiation therapy | Postsurgical residual disease | 3050% longterm control |
Special Topics Overview
Cushing syndrome vs Addison disease
While Cushing pushes cortisol levels skyhigh, Addison disease does the oppositeleaving you cortisoldeficient. The two can look like opposite sides of the same coin, which is why doctors often run both sets of labs when the clinical picture is muddy.
Cushing disease vs Cushings syndrome dexamethasone
The dexamethasone test is like a loyalty check. Lowdose dexamethasone should suppress cortisol in a healthy person. In Cushing disease, cortisol remains high on lowdose but drops on highdose. In other forms of Cushing syndrome, even a high dose wont suppress.
Cushing syndrome vs Cushing disease in dogs
Our furry friends arent exempt. Dogs usually develop a pituitary pars intermedia tumor (PPIT) that mirrors human Cushing disease, or an adrenal tumor similar to human Cushing syndrome. Treatment mirrors humanssurgical removal, medical control with trilostane, or radiationthough the dosage and approach differ.
Diseases that mimic Cushings syndrome (expanded)
- Severe depression or anxiety (stressinduced cortisol spikes)
- Alcohol dependence (pseudoCushing)
- Obesity metabolic syndrome (overlapping signs)
- PCOS (especially in women with irregular periods and central obesity)
Realworld story
Sarah, a 35yearold graphic designer, spent two years battling unexplained weight gain and persistent fatigue. Her primary care doctor initially chalked it up to stress, but after a friend mentioned moon face, Sarah pushed for hormone testing. Lowdose dexamethasone didnt suppress her cortisol, ACTH was high, and a highdose test finally tipped the scales toward Cushing disease. After a successful transsphenoidal surgery, her energy returned, and she finally felt herself again. Stories like Sarahs remind us that listening to our bodiesand advocating for deeper testingcan change outcomes dramatically.
When to Seek Help
If you notice any of the redflag signs below, its time to talk to a healthcare professional:
- Rapid, unexplained weight gain (especially around the torso)
- Pronounced moon face or buffalo hump
- Easy bruising, purple stretch marks, or thinning skin
- High blood pressure or newonset diabetes
- Persistent muscle weakness or fatigue
- Irregular menstrual cycles (for women) or decreased libido (for men)
Before your appointment, bring a symptom diary (dates, severity, any medication changes) and a list of current prescriptionsincluding overthecounter steroids or inhalers. This helps your doctor decide which tests (like the overnight saliva cortisol) are most appropriate.
Wrapping It Up
Bottom line: Cushing disease is a specific, pituitarydriven form of Cushing syndrome. Understanding that distinction guides the right labs, imaging, and treatment pathway, giving you (or a loved one) the best chance at a speedy recovery. If any of the symptoms we discussed sound familiar, dont ignore themearly detection is key. And remember, youre not alone; countless patients have walked this path, and the medical community continues to refine both diagnostic tricks and surgical techniques. Stay curious, stay proactive, and reach out to an endocrinologist if you suspect something isnt quite right. Your health is worth it.