Ever felt that annoying tingling in your fingertips or a constant muscle cramp that just wont quit? You might have brushed it off as just stress, but for some people its actually a signal from the parathyroid glands especially when autoimmunity is in play. Below youll find the straighttothepoint rundown of what to watch for, why it matters, and what steps you can take right now.
Quick Answer Snapshot
What are the most common autoimmune parathyroid disease symptoms?Typical signs include tingling or numbness around the lips and fingertips, muscle spasms (often called tetany), unexplained fatigue, and occasional brain fog.
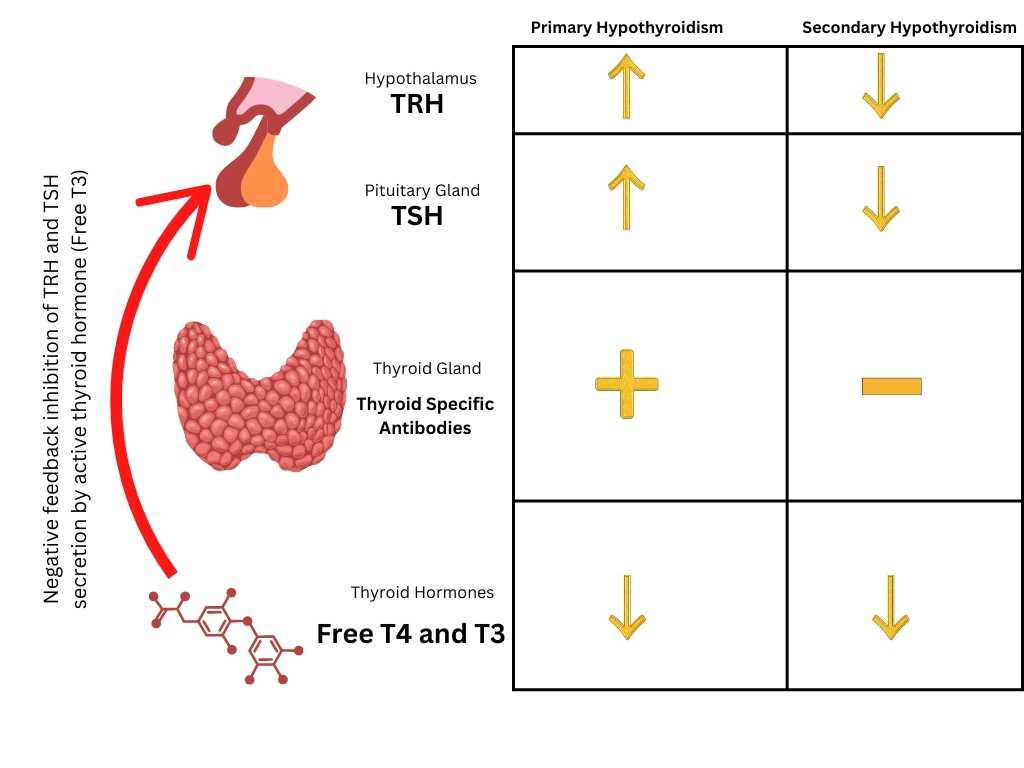
How do they differ from regular hypo or hyperparathyroidism?Autoimmune forms tend to pop up alongside other autoimmune conditions (like thyroiditis), and they may fluctuate as the immune system attacksandreleases the glands.
When should you see a doctor?If tingling, cramps, or persistent fatigue last more than a week, or if blood tests show low calcium, its time to schedule an appointment with an endocrinologist.
Autoimmune Disease Overview
What makes a parathyroid disorder autoimmune?
In an autoimmune scenario, your immune system mistakenly targets the tiny parathyroid glands (usually four). This attack can damage the cells that produce parathyroid hormone (PTH), leading to erratic calcium regulation. Genetics, a prior viral infection, or having another autoimmune disease (like Hashimotos) often set the stage.
According to a study in PubMed, autoantibodies against the calciumsensing receptor are a reliable marker for autoimmune parathyroid disease.
How does autoimmunity affect hormone levels?
When the immune system damages the glands, PTH production drops, resulting in low parathyroid hormone symptoms. Low PTH means calcium cant be pulled from bones or absorbed in the gut, which fuels most of the clinical signs well discuss.
In rarer cases, the gland may overreact before it quits, creating a brief spike in PTH that mimics hyperparathyroidism symptoms. Thats why a proper lab workup is crucial youll want to see both calcium and PTH numbers together.
RealWorld Example
Meet Maria, a 38yearold graphic designer. After a bout of flu, she began noticing a persistent pinsandneedles sensation in her fingertips and sudden muscle cramps during long meetings. Blood work revealed low calcium and low PTH. Her doctor ordered an autoantibody panel, which came back positive confirming an autoimmune cause. Within weeks of calcium and calcitriol supplementation, her symptoms faded, and she could finally focus on her designs again.
Complete Symptom Checklist
| Category | Specific Symptom | Typical Onset | Notes (autoimmune link) |
|---|---|---|---|
| Neurologic | Tingling or numbness (lips, fingers, toes) | Gradual | Often the first clue of low parathyroid hormone symptoms |
| Neurologic | Muscle cramps, spasms, twitching | Intermittent | Can be mistaken for anxiety or dehydration |
| Neurologic | Brain fog, confusion, memory lapses | Episodic | Calcium is essential for neurotransmission |
| Skeletal / Muscular | Bone pain, joint stiffness | Persistent | Overlap with hyperparathyroidism pain patterns |
| Skeletal / Muscular | General weakness, easy fatigue | Daily | Reflects chronic calcium deficiency |
| Cardiovascular | Irregular heartbeat, palpitations | Sporadic | Calcium influences cardiac muscle contraction |
| Gastrointestinal | Nausea, abdominal pain, constipation | Variable | Often overlooked as a digestive issue |
| Dermatologic | Dry skin, brittle nails, occasional rashes | Occasional | Common in many autoimmune disorders |
| Psychological | Anxiety, mood swings, mild depression | Ongoing | Calcium shortage can affect mood regulation |
Use this checklist as a quick selfscreen. If you tick several boxes, its worth chatting with a healthcare professional.
Condition Comparison Guide
Low Parathyroid Hormone (Hypoparathyroidism) vs. Autoimmune Form
Both share symptoms like tingling, cramps, and fatigue. The key differentiator is the presence of autoantibodies or a known autoimmune backdrop (e.g., lupus, rheumatoid arthritis). Regular hypoparathyroidism is often surgical (postthyroidectomy) or genetic, while the autoimmune version comes with a broader immunesystem narrative.
Hyperparathyroidism Symptoms Checklist
When PTH is too high, you might notice kidney stones, excessive thirst, bone thinning, and stomach ulcers. These are the classic hyperparathyroidism symptoms that stand in stark contrast to the lowcalcium picture of autoimmune disease. Knowing the difference helps your doctor order the right labs.
Parathyroid Cancer Symptoms in Females
Rare, but if you encounter a rapid neck mass, hoarseness, or severe, unrelenting neck pain, seek medical attention immediately. While most parathyroid issues are benign, these redflag signs point toward a possible malignancy.
Quick DecisionTree (Suggested Graphic)
Start with tingling? Check calcium level Low calcium Test PTH Low PTH Autoantibody panel Positive? Autoimmune parathyroid disease. If any step shows high values, pivot toward hyperparathyroidism workup.
Your Treatment Team
When it comes to who can guide you through this maze, the answer is usually an endocrinologist. They specialize in hormone regulation, calcium balance, and the nuances of autoimmune disorders. In some cases, you might also see a rheumatologist (especially if you have multiple autoimmune conditions) or a surgeon if a parathyroidectomy becomes necessary.
So, if you ever wondered what kind of doctor treats parathyroid disease, the short answer is: start with an endocrinologist, and theyll refer you to other specialists as needed.
Diagnostic Process Overview
Blood Tests & What They Reveal
- Serum calcium low in autoimmune disease.
- Parathyroid hormone (PTH) usually low or inappropriately normal.
- Phosphate often high when calcium is low.
- Vitamin D deficiency can worsen symptoms.
- Autoantibody panel looks for antibodies against the calciumsensing receptor.
Imaging Options
Most people wont need imaging unless surgery is on the table. A neck ultrasound or a Sestamibi scan can show if a gland is enlarged or if theres an unexpected mass. MRI is reserved for rare cases where a tumor is suspected.
Biopsy & Histology (Rare)
Only considered if cancer is on the differential. A fineneedle aspiration can help, but its seldom needed for autoimmune disease.
Credible Source Reminder
According to , a thorough lab panel combined with clinical assessment is the gold standard for diagnosing hypoparathyroidism, whether autoimmune or not.
Management Options Overview
Hormone Replacement
Most patients benefit from calcitriol (active vitamin D) and calcium supplements. The goal is to keep serum calcium in the lownormal range to avoid spikes that could cause kidney stones.
Immunomodulatory Therapies
In cases where autoimmunity is aggressive, lowdose steroids or newer agents like rituximab have been tried. These are specialistlevel decisions and require close monitoring.
Lifestyle Adjustments
- Boost vitamin D through safe sun exposure or fortified foods.
- Include calciumrich foods like dairy, leafy greens, and fortified plant milks.
- Stay hydrated dehydration can amplify muscle cramps.
- Gentle exercise (walking, yoga) supports bone health.
- Stressreduction techniques (meditation, deep breathing) may calm the immune system.
Patient Success Story (Experience)
John, a 45yearold teacher, was diagnosed after a series of lab tests revealed low calcium and low PTH. With a blend of calcitriol, a modest calcium supplement, and monthly checkins with his endocrinologist, his tingling disappeared within two months. He also joined a local autoimmune support group, which he says helped him feel less isolated and more proactive.
Final Takeaway Summary
Autoimmune parathyroid disease isnt just a medical curiosity its a real, everyday challenge for many people who are told to just drink more calcium. The hallmark signs tingling, muscle cramps, fatigue, and that hazy brain fog are warning lights that deserve attention. Early detection, accurate lab work, and a caring team of specialists (primarily an endocrinologist) can turn a confusing symptom list into a manageable plan.
If any of the symptoms above resonate with you, dont wait. Jot them down, get a blood test, and schedule a visit with an endocrinologist. Knowledge is power, and the sooner you act, the faster you can reclaim that vibrant, painfree feeling you deserve.
FAQs
What are the main symptoms of autoimmune parathyroid disease?
Tingling or numbness around the lips, fingers and toes, muscle spasms or cramps (tetany), fatigue, brain fog, bone pain and irregular heartbeat are common due to low calcium from damaged glands.[1]
How does autoimmune parathyroid disease differ from regular hypoparathyroidism?
Autoimmune form involves immune attack on glands with autoantibodies, often linked to other autoimmune conditions like Hashimoto's, unlike surgical or genetic causes of regular hypoparathyroidism.[1]
When should you see a doctor for these symptoms?
Seek an endocrinologist if tingling, cramps or fatigue persist over a week, especially with low calcium on blood tests, to confirm autoimmune parathyroid disease.[1]
What blood tests diagnose autoimmune parathyroid disease?
Key tests include low serum calcium, low or normal PTH, high phosphate, vitamin D levels and autoantibody panel against calcium-sensing receptor.[1]
What treatments help autoimmune parathyroid disease symptoms?
Calcium and calcitriol supplements restore levels, with lifestyle changes like vitamin D-rich foods; aggressive cases may use immunomodulators under specialist care.[1]