If you're wondering whether the vaccine can really cause a new allergy, how to spot a reaction, or what to do if it happens, keep reading. I'll break down the data, share real stories from folks on Reddit, and give you practical steps to stay safe while still getting the protection you need.
Quick Summary
The short answer: allergic reactions to COVID19 vaccines are rare, and most are mild. According to the, anaphylaxis occurs in about 9 cases per million doses, and any type of allergic reaction shows up in roughly 43 per million. Those numbers are tiny compared to the hundreds of millions of doses already administered worldwide.
But rare doesn't mean impossible. If you've ever had a severe allergysay, to peanuts or bee stingsyou're naturally more cautious. Below we'll explore who's most at risk, what symptoms to watch for, and how to manage a reaction if it does happen. For mild skin reactions such as spreading hives or persistent itching, many people find relief with simple home care and antihistamines, while others may benefit from guidance about hives home treatment.
Recognizing Signs
Allergic reactions can show up in two main timeframes: immediate (within minutes to a few hours) and delayed (days to weeks later). Knowing the difference helps you decide whether to stay for a 15minute observation at the clinic or call your doctor later.
Immediate Reactions
Typical signs of an immediate allergy include:
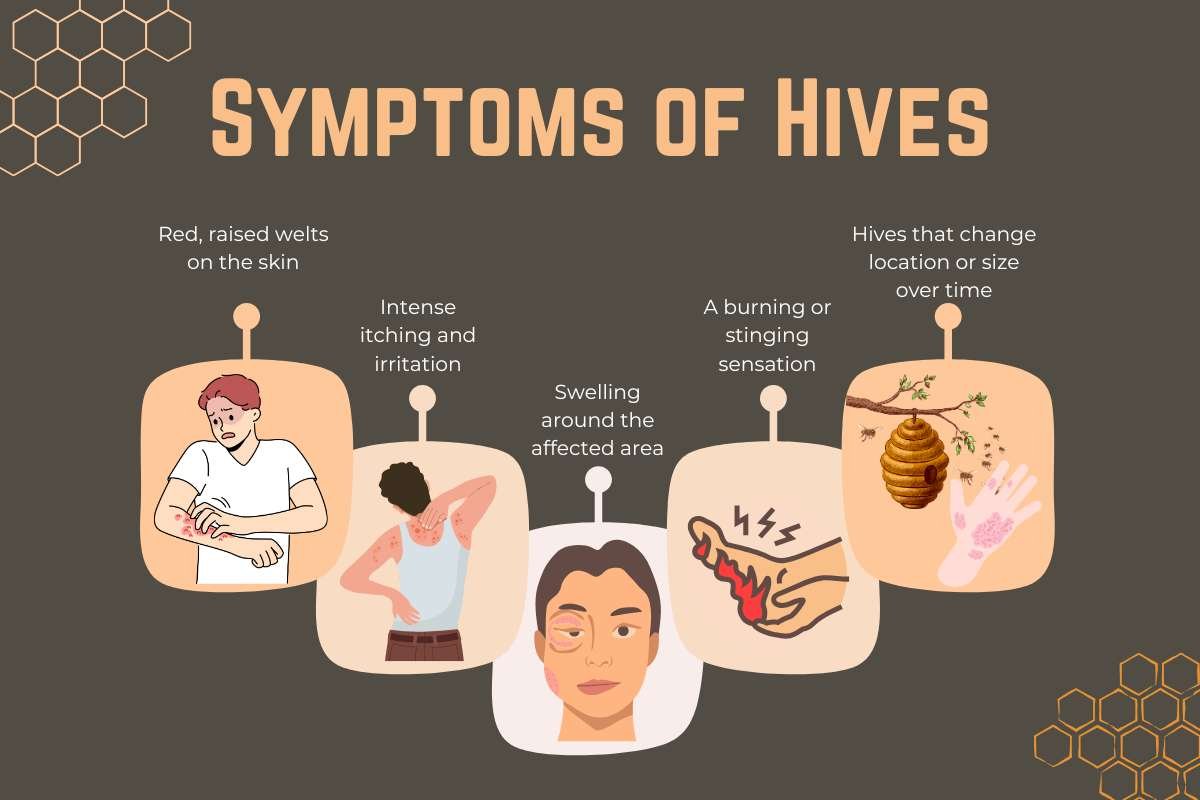
- Red, itchy hives or rash that spreads quickly
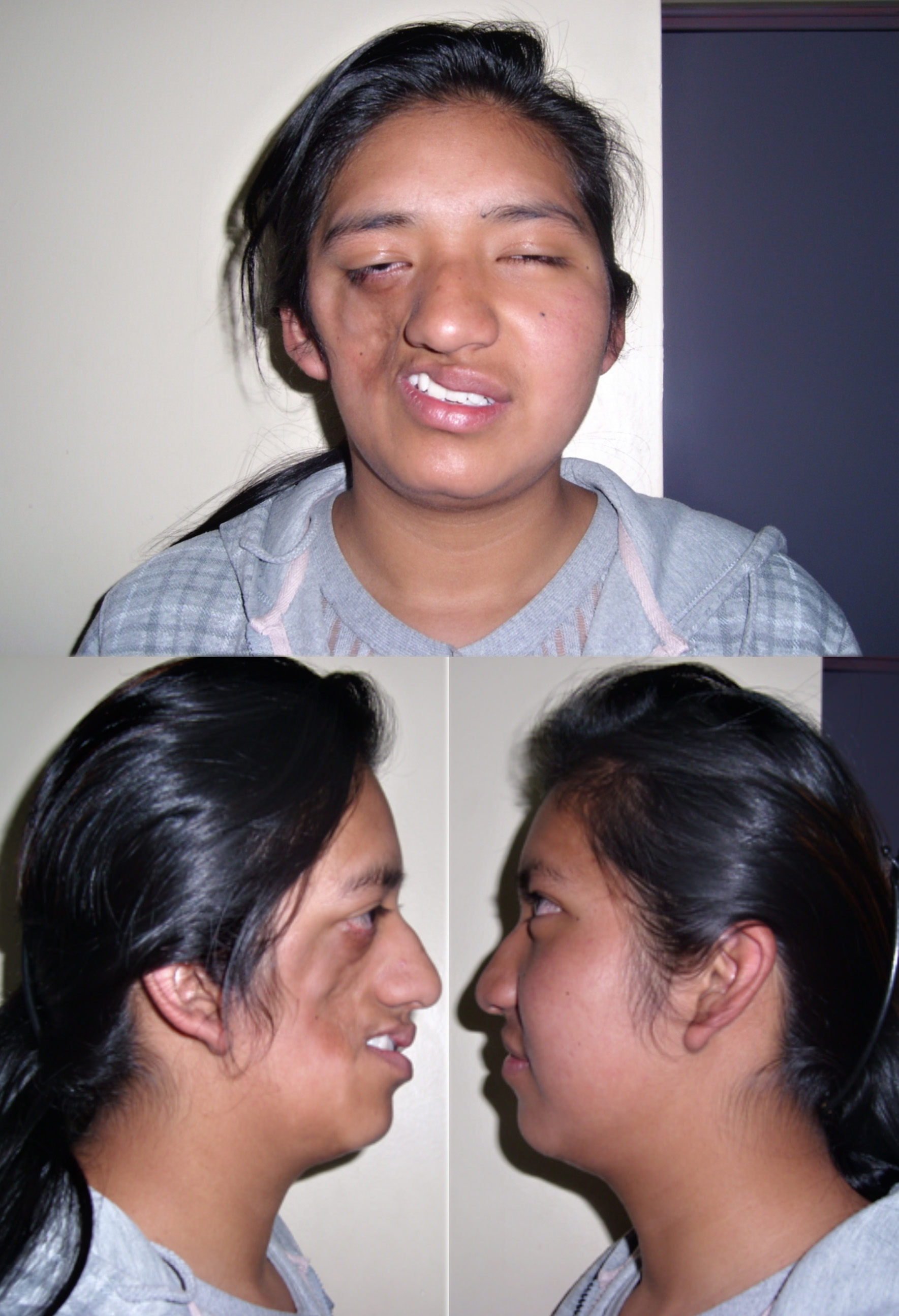
- Swelling of the face, lips, or throat
- Difficulty breathing, wheezing, or a tight chest
- Rapid heartbeat or a sudden drop in blood pressure (anaphylaxis)
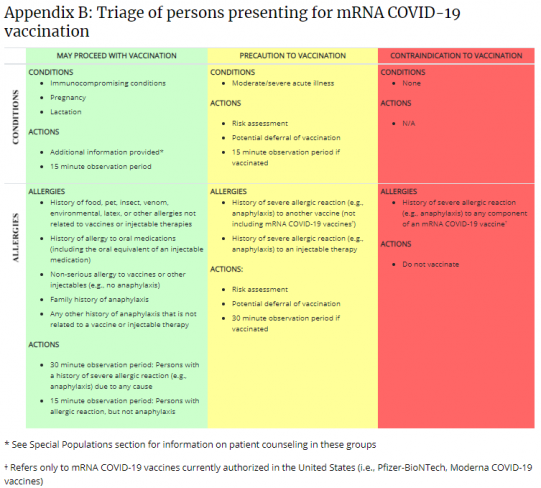
If any of these appear within the first 30 minutes, seek emergency care right away. The vaccine sites are required to have epinephrine on hand, and the recommends a 15minute observation for most people, extending to 30 minutes if you have a known severe allergy.
Delayed or Atypical Symptoms
Not all reactions happen instantly. Some people report new food allergies, sun intolerance, or longCOVIDstyle allergy symptoms weeks after the shot. For example, a handful of Reddit users described developing a sudden peanut allergy three weeks postvaccinationthough researchers haven't proved a direct link, the pattern is worth noting.
Other delayed signs include:
- Persistent itching or rash lasting more than a day
- New sensitivity to sunlight (sun allergy after covid vaccine)
- Exacerbated existing allergies (allergies worse after covid)
- Unexplained gastrointestinal upset that resembles an allergic response
These symptoms usually resolve on their own or with antihistamines, but if they linger, a followup with an allergist is wise.
Who Is Likely
Most people with no prior allergy history won't experience anything beyond a sore arm. However, certain groups have a higher chance of developing new allergies after the vaccine.
Prior Allergy History
If you've ever had an IgEmediated reactionthink hives, wheezing, or anaphylaxisto any medication or food, you're statistically more likely to have a reaction to the COVID shot. That doesn't mean you can't get vaccinated; it just means you should discuss it with your doctor and possibly get vaccinated in a setting equipped for emergencies.
Specific Risk Factors
Research from the shows that people with mast cell disorders, a history of severe drug reactions, or certain medications (like ACE inhibitors) may have a slightly elevated risk. Age and sex also play a rolewomen and younger adults appear to report more immediate reactions, though the reasons are still being studied.
Special Populations
Children, pregnant people, and those who are immunocompromised often ask if they're more vulnerable. Current data suggest that the risk profile is similar across these groups, but the benefit of protectionespecially for pregnant peoplefar outweighs the tiny allergy risk.
Managing Reactions
Preparedness is half the battle. Below is a simple whattodo roadmap you can keep on your phone or a sticky note.
OnSite Emergency Protocol
All vaccination sites follow the CDC's threestep emergency plan:
- Administer epinephrine immediately if anaphylaxis is suspected.
- Call 911 while positioning the person upright with legs slightly bent.
- Monitor vitals for at least 15 minutes after epinephrine, then longer if needed.
This protocol has saved countless lives, and it's why the observation period after the jab is nonnegotiable for highrisk individuals.
PostVaccination Care
If you notice mild itching or a small rash after leaving the clinic, try an overthecounter antihistamine like cetirizine. Keep the injection site clean, and avoid scratching. If symptoms worsen or you develop trouble breathing, don't waithead straight to the emergency department.
FollowUp with an Allergist
When should you see a specialist? If you experienced any of the following, schedule an appointment:
- Any sign of anaphylaxis, even if treated on the spot
- Persistent or spreading rash beyond 48 hours
- New food or environmental allergies that you didn't have before
Allergists can perform skinprick testing or blood work to pinpoint the culprit and discuss options like gradeddose challenges or switching to a different vaccine platform.
Future Dosing Options
For those who need a booster but had a reaction to the first dose, consider these strategies (always under medical supervision):
- Premedication with antihistamines or leukotriene blockers
- Administering the vaccine in a graded, incremental fashion (e.g., tiny dose, then intermediate dose, then full dose)
- Choosing a different vaccine type (e.g., protein subunit instead of mRNA)
These approaches have helped many people safely complete their vaccination series.
Real World Voices
Numbers are comforting, but stories speak to the heart. Below are a few anonymized snippets from the developed allergies after covid vaccine reddit threads that illustrate the range of experiences.
Reddit Themes
Many users reported a COVID arm that turned into a fullbody rash lasting several days. One commenter described a sudden peanut sensitivity that appeared three weeks after the second dose: "I never had a problem with peanuts before, but now a tiny piece makes my throat swell. I'm scared, but my allergist says it could be a coincidental timing."
Food Allergy Anecdotes
Another thread highlighted food allergies after covid vaccine where individuals experienced itching and hives when eating dairy or nuts, despite no prior issues. While not every case proves causation, the pattern prompted some researchers to explore whether the vaccine's immune activation could momentarily lower the threshold for allergic reactions.
Lessons Learned
The common thread? Most Redditors who sought medical advice received reassurance and treatment plans that helped them manage the new symptoms. A few even discovered that their new allergy was a false alarmoften a viral rash or a reaction to a medication taken at the same time. The takeaway? Don't selfdiagnose; get a professional opinion. For persistent skin reactions resembling hives, many resources recommend simple measures and, if needed, further evaluation of hives relief herbs as complementary care alongside medical treatment.
Balancing Benefits
It's easy to get caught up in the fear of a reaction, but let's put it into perspective with a quick riskbenefit snapshot.
| Factor | COVID19 Vaccine | Allergic Reaction |
|---|---|---|
| Likelihood | Prevents ~90% of severe COVID19 cases | ~9 anaphylaxis cases per 1 million doses |
| Severity | Reduces hospitalization, ICU stay, and death | Most reactions are mild; severe cases treatable with epinephrine |
| LongTerm Impact | Protects against long COVID and variants | Allergies usually resolve or become manageable |
When you stack those numbers, getting vaccinated is the safer bet for virtually everyone. If you're hesitant because allergies worse after covid, remember that the protective benefits far outweigh the minuscule risk of a severe allergy.
DecisionMaking Framework
Ask yourself:
- Do I have a history of severe allergic reactions? If yes, talk to my doctor before the appointment.
- Am I comfortable staying for observation after the shot? If not, arrange a visit at a clinic equipped for emergencies.
- What's my risk of severe COVID19? Consider age, health conditions, and community transmission rates.
Answering these honestly will guide you toward an informed, confident choice.
Expert Resources
For anyone who wants to dig deeper, these trusted sources are a gold mine:
- Uptodate statistics and emergency protocols.
- Expert recommendations for patients and providers.
- Indepth data on incidence and mechanisms.
These sites keep information transparent, cite their sources, and are regularly updatedexactly what we need for trustworthy guidance.
Conclusion
Allergic reactions to COVID19 vaccines are real but exceedingly rare, and most are mild and easily treated. By staying informed about the signs, understanding who might be at higher risk, and knowing how to respondwhether it's a quick antihistamine or an emergency epinephrine shotyou can protect yourself while still enjoying the overwhelming benefits of vaccination.
If you've ever experienced a reaction, or if you're simply curious, share your story in the comments. Your experience could help someone else decide what's right for them. And remember: when in doubt, reach out to a healthcare professionalyou deserve answers that are both compassionate and scientifically sound.
FAQs
What are the most common immediate symptoms of a COVID vaccine allergy?
Typical immediate signs include hives or a rash, swelling of the face/lips/throat, difficulty breathing, wheezing, rapid heartbeat, and in severe cases, anaphylaxis.
How rare is anaphylaxis after receiving a COVID‑19 vaccine?
According to CDC data, anaphylaxis occurs in roughly 9 cases per million doses administered, making it an extremely rare event.
Who is at higher risk for developing an allergic reaction to the vaccine?
People with a history of severe IgE‑mediated allergies, mast‑cell disorders, previous anaphylaxis to medications, or certain medications (e.g., ACE inhibitors) have a slightly elevated risk.
What should I do if I experience a delayed rash after the shot?
For a rash lasting more than a day, try an over‑the‑counter antihistamine. If it spreads, worsens, or is accompanied by other symptoms, schedule a follow‑up with an allergist.
Can I get a different COVID vaccine if I had a reaction to the first one?
Yes. Under medical supervision you can consider a different vaccine platform (e.g., protein subunit) or a graded‑dose approach to complete your series safely.