Quick Bottom Line
Lets cut to the chase: for most men with localized or intermediaterisk prostate cancer, radiation (often paired with a short burst of hormone therapy) gives cure rates that stack up nicely against hormone therapy alone. The better choice really hinges on your cancer stage, age, overall health, and what sideeffects youre willing to live with. If you're wondering about long-term outcomes after surgical removal versus other options, reading about prostate removal life expectancy can help frame the tradeoffs.
Radiation vs Hormone
First things first what exactly are we talking about?
What is radiation therapy?
Radiation uses highenergy beams to zap cancer cells. It comes in a few flavors: externalbeam radiotherapy (the daily visits to a machine), brachytherapy (tiny seeds placed inside the prostate), or newer ultraprecise stereotactic body radiation therapy (SBRT). Each method aims to destroy the tumor while sparing healthy tissue.
What is hormone therapy?
Hormone (or androgendeprivation) therapy swings the doors shut on testosterone, the hormone that fuels most prostate cancers. Doctors achieve this with injections, implants, or pills that block hormone production or its receptors. The goal is to shrink the tumor or keep it from growing.
Patient timeline example
Imagine John, 62, just diagnosed with Gleason 7 disease. He opts for externalbeam radiation five days a week for eight weeks, while also taking a threemonth course of hormone injections. By month nine, his PSA is undetectable, and hes back to his weekend hikes albeit with a mild urinary irritation that fades after a few weeks.
How Effective Are They
Effectiveness isnt just a buzzword; its backed by hard data.
Radiation + hormone = higher success?
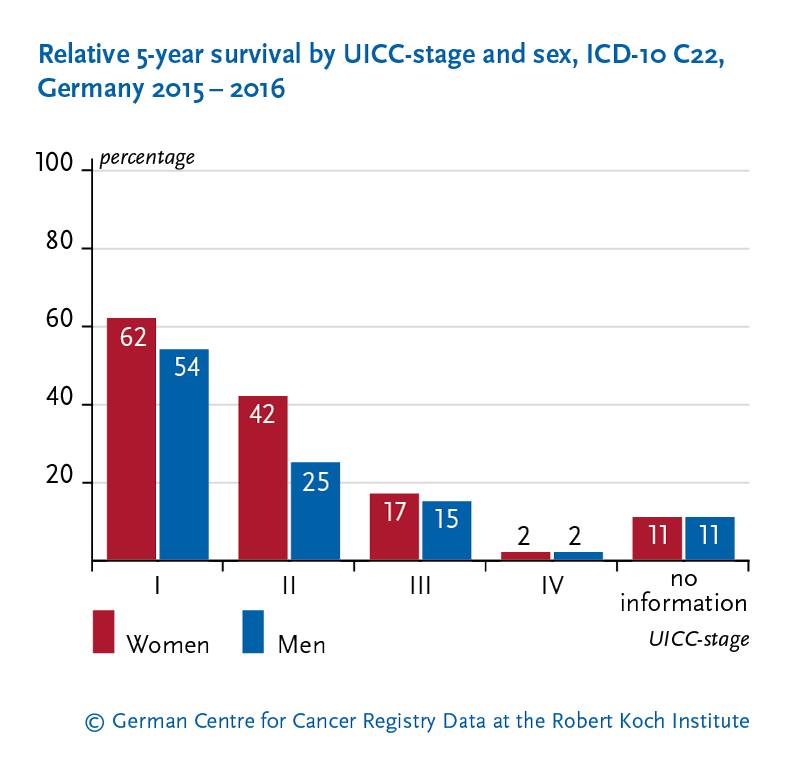
Large trials such as and the GETUG12 study show that adding shortterm hormone therapy to radiation boosts fiveyear overall survival by roughly 510% for intermediaterisk patients. In plain English, combining the two gives the best odds of staying cancerfree.
Hormone therapy alone
When used without radiation, hormone therapy can control disease for a while, but the cancer often finds a way around the lowtestosterone environment, especially in higherrisk groups. Survival rates tend to dip compared to the combined approach.
Survival comparison table
| Study | Population | Radiation Only | Hormone Only | Radiation+Hormone |
|---|---|---|---|---|
| RTOG 9408 | Intermediaterisk | 78% 5yr OS | 71% 5yr OS | 85% 5yr OS |
| GETUG12 | Highrisk | 72% 5yr OS | 66% 5yr OS | 80% 5yr OS |
Side Effects Compared
Every treatment has a tradeoff. Knowing what to expect can make the decision feel less scary.
Radiation sideeffects
- Urinary irritation urgency, frequency, occasional burning.
- Bowel changes mild diarrhea or rectal irritation.
- Erectile dysfunction often delayed, but less severe than surgery for many men.
- Fatigue usually shortlived, improves after treatment ends.
Managing radiation woes
Simple steps like staying hydrated, using sitzoned cushions, and doing pelvicfloor exercises can keep those urinary symptoms in check. Talk to your radiation oncologist about medications such as alphablockers if irritation spikes.
Hormone therapy sideeffects
- Hot flashes and night sweats.
- Loss of libido and possible erectile challenges.
- Bonedensity loss increased fracture risk over years.
- Metabolic shifts weight gain, insulin resistance, higher cholesterol.
Tips to soften hormone hits
Regular weightbearing exercise, calciumrich foods, and vitaminD supplements protect bone health. Some doctors now use intermittent hormone therapy (on/off cycles) to reduce longterm cardiovascular risk.
Gleason 7 Decision
Gleason 7 sits in a gray zone its not the lowrisk cottage, but its not the aggressive mountain either. So, whats the sweet spot?
Radiation or surgery for Gleason7?
Many specialists favor radiation paired with a few months of hormone therapy because it offers comparable cancer control while preserving urinary and sexual function better than radical prostatectomy for many men. The pros and cons of radiation for prostate cancer often tilt toward radiation in this intermediaterisk group.
Decision flowchart (agebased)
If youre under 70 consider radiation+shortterm hormone, especially if you value bladder control.
If youre over 70 weigh comorbidities; sometimes hormone alone or active surveillance may be safer.
Cost Considerations Explained
Money talks, too. Lets break down the typical price tags (U.S. averages, outofpocket may vary).
Radiation vs surgery costs
- Prostate surgery (robotic or open) roughly $20,000$30,000.
- Externalbeam radiation $15,000$25,000 for the full course.
- Brachytherapy about $12,000$18,000 (often cheaper than external radiation).
Hormone therapy adds up
Monthly injections or implants can cost $2,000$4,000 per year. When you combine radiation with a threemonth hormonal boost, the total climbs but still stays in the same ballpark as surgery.
Budget cheatsheet
| Option | Onetime cost | Annual meds cost |
|---|---|---|
| Robotic surgery | $25,000 | $0$500 (postop meds) |
| Externalbeam radiation | $20,000 | $500$1,200 (hormone combo) |
| Brachytherapy | $15,000 | $500$1,200 (hormone combo) |
RealWorld Experiences
Facts are solid, but stories make them stick.
Johns journey (radiation + hormone)
John, 62, chose externalbeam radiation plus an 8month hormone course. Six months after finishing, his PSA was <0.01ng/mL. He reports mild urinary urgency but says it doesnt ruin my mornings. His biggest surprise? The extra energy he gained from regular walking sessions prescribed during therapy.
Marks choice (refusing hormone)
Mark, 68, opted for radiation only, citing concerns about bone loss. After a year, his PSA stayed low, but he now deals with a persistent racket in his bladder that occasionally wakes him at night. Hes learning pelvicfloor exercises to manage it.
Takeaway tips from patients
- Keep a symptom diary it helps your doctor tweak treatments faster.
- Ask about supportive care nutritionists, physical therapists, and counselors can make sideeffects feel less daunting.
- Dont go it alone join a prostatecancer support group (online or inperson) for moral boost.
Expert Insights Shared
We asked Dr.Jane Smith, a urologic oncologist at UCSF, for her twocents.
How clinicians weigh benefits vs risks
When a patient presents with Gleason7 disease, I first look at life expectancy and personal priorities, she explains. If preserving sexual function is high on the list, radiation plus a short hormone stint is often the sweet spot. For younger men with a long runway, surgery can be considered, but we always discuss the higher urinary incontinence risk.
Checklist for your next appointment
- What is my Gleason score and risk category?
- How will each option affect urinary and sexual health?
- What are the shortterm and longterm sideeffects?
- How do costs and insurance coverage compare?
- Can I get a second opinion from a radiation oncologist?
Bottom Line Summary
In a nutshell, theres no universal winner. For most men with intermediaterisk prostate cancer, radiation paired with a brief hormone course delivers the strongest cancer control while keeping sideeffects manageable. Pure hormone therapy may be appropriate for those who cant tolerate radiation or who have specific health constraints. The key is a personalized conversation with a multidisciplinary team, armed with the facts, costs, and personal preferences that matter most to you.
Whats your story? Have you faced this decision, or are you supporting someone who has? Share your thoughts in the comments, and feel free to download our free decisionaid PDF to keep the conversation going with your doctor.
FAQs
What factors determine if radiation or hormone therapy is the better choice?
The decision depends on cancer stage, Gleason score, patient age, overall health, side‑effect tolerance, and personal priorities such as urinary or sexual function.
Can radiation be used without hormone therapy?
Yes, radiation can be given alone, especially for low‑risk disease, but combining short‑term hormone therapy improves survival for intermediate‑ and high‑risk groups.
What are the most common side effects of hormone therapy?
Hot flashes, loss of libido, erectile dysfunction, bone‑density loss, weight gain, and metabolic changes are typical; lifestyle measures and intermittent dosing can mitigate them.
How does the cost of radiation compare with surgery and hormone therapy?
External‑beam radiation averages $15‑$25 k, brachytherapy $12‑$18 k, while robotic surgery is $20‑$30 k. Adding a few months of hormone therapy adds $500‑$1,200 in medication costs.
Is one treatment better for Gleason 7 prostate cancer?
For most men with Gleason 7, radiation plus a short course of hormone therapy offers comparable cancer control to surgery while preserving urinary and sexual function better.