Hey there, lets cut straight to the chase. If youve felt a strange lump, a persistent heaviness in the scrotum, or an odd ache radiating to your lower back, those could be the redflag signals that point to advanced testicular cancer. Spotting these signs early can make a massive difference, and you dont need a medical degree to know what to look for.
Below youll find the most commonand the sneakieradvanced symptoms, why they happen, and the exact steps you should take right now. No fluff, just the facts you need, delivered like a friend sharing something important over coffee.
Core Warning Signs
What are the 5 classic warning signs?
First up, the basics. Even though were focusing on the advanced stage, the five hallmark warnings apply across the board:
- Lump or swelling in one testicle that feels firm or rubbery.
- Heaviness or a drag sensation in the scrotum.
- Dull or sharp ache that may travel to the groin or lower abdomen.
- Sudden fluid buildup (hydrocele) causing swelling.
- Change in size, shape, or consistency of a testicle.
Imagine youre at the gym and you notice a new muscle that isnt supposed to be therethats the body trying to tell you something.
How do these signs differ in early vs. advanced stages?
| Stage | Typical Symptoms | Advanced Indicators |
|---|---|---|
| Early (Stage12) | Painless lump, mild heaviness, occasional ache. | |
| Advanced (Stage34) | Lowback pain, enlarged lymph nodes, chest pain, shortness of breath, neurological changes. |
Notice how the advanced column adds symptoms that suggest cancer has spread beyond the testicle itself.
Can testicular cancer kill you?
The short answer: it can, but the good news is that its one of the most treatable cancers when caught early. According to , the overall fiveyear survival rate sits above 95% for localized disease, and even for metastatic cases it remains encouraging thanks to modern chemotherapy regimens.
Advanced Symptom Profile
What are the hallmark symptoms of advanced (stage34) disease?
When testicular cancer moves beyond the testicle, it tends to invade nearby structures and distant organs. Heres what you might feel:
- Lowback pain caused by tumor spread to retroperitoneal lymph nodes.
- Painful or firm lumps in the abdomen or groin, indicating enlarged lymph nodes.
- Chest pain or shortness of breath a sign the disease may have reached the lungs.
- Headaches, visual changes, or neurological deficits rare, but possible if cancer spreads to the brain.
- Unexplained weight loss and persistent fatigue.
Why does lowback pain appear?
The testicles drain into a network of lymph vessels that sit deep in the abdomen. When cancer cells lodge in those nodes, they can create a pressure buildup that mimics a muscle strain in the lower back. Its like a hidden traffic jam you cant see, but you feel the congestion.
Are there visual clues (pictures) that help?
Seeing is believing. Reputable sites like showcase clear images of testicular lumps, scrotal swelling, and even ultrasound snapshots. Those pictures can demystify what abnormal really looks like, but remember: a picture is never a substitute for a professional exam.
Similar Conditions
Which benign conditions look similar?
Its easy to mistake a harmless issue for something serious. Common mimickers include:
- Epididymitis inflammation of the epididymis, usually caused by infection; it brings pain and swelling but responds to antibiotics.
- Hydrocele fluid buildup that makes the scrotum look swollen; its painless and often resolves on its own.
- Inguinal hernia a bulge that can appear in the groin area, sometimes mistaken for a testicular mass.
While these conditions are generally less dangerous, they still deserve a medical checkup to rule out cancer.
How to tell the difference without a doctor?
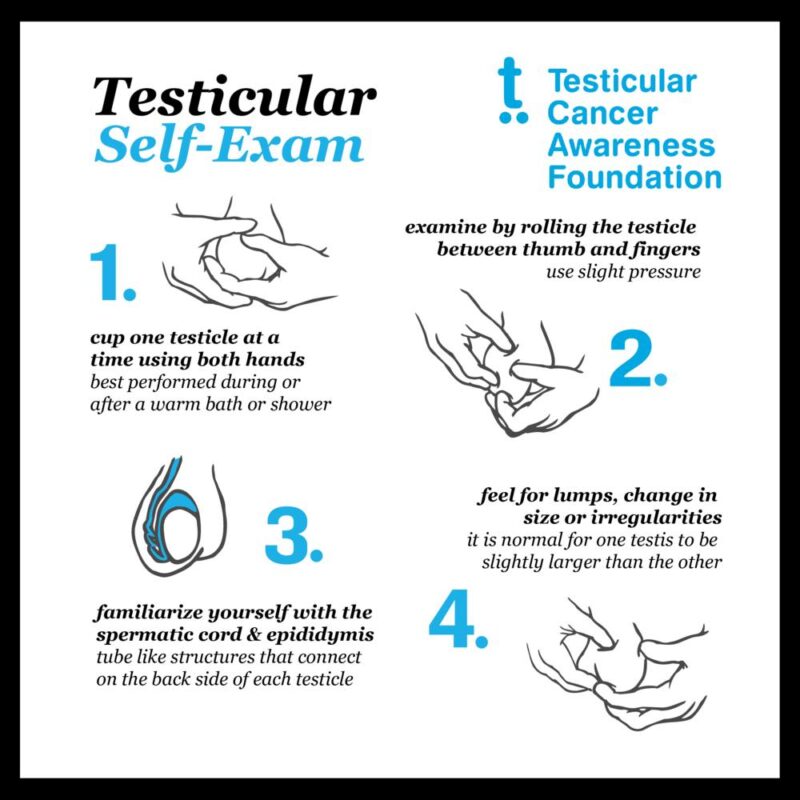
Selfexamination can be a useful first step. Heres a quick guide:
- Do it in a warm shower or after a bath when the skin is relaxed.
- Gently roll each testicle between the thumb and fingers, feeling for any hard nodules.
- Note any persistent pain, swelling, or a feeling of heaviness that doesnt go away after a few days.
If anything feels off, schedule an appointmentdont wait for the pain to go away on its own.
Diagnosis Process
Clinical exam & ultrasound basics
When you see a doctor, the first step is a physical exam followed by a scrotal ultrasound. Ultrasound uses sound waves to produce an image of the inside of the scrotum, helping doctors differentiate a solid tumor from a cyst or fluid collection.
Blood markers (AFP, hCG, LDH) and what they reveal
Three tumor markers are commonly measured:
- Alphafetoprotein (AFP) elevated in nonseminomatous tumors.
- Betahuman chorionic gonadotropin (hCG) can rise in both seminoma and nonseminoma.
- Lactate dehydrogenase (LDH) a nonspecific marker that often reflects tumor burden.
These numbers, together with imaging, give doctors a clear picture of how far the disease has progressed.
Staging explained: from stage1 to metastatic
Staging tells us where the cancer started and where its traveled. In brief:
- Stage1 confined to the testicle.
- Stage2 spread to nearby lymph nodes.
- Stage3 beyond regional nodes, possibly to lungs or liver.
- Stage4 distant organs, such as the brain or bones.
Understanding your stage is the compass for treatment decisions.
Treatment Options
Surgery (orchiectomy) why its still first line
Even for advanced disease, removal of the affected testicle (orchiectomy) is almost always the initial step. It eliminates the primary source of cancer cells and provides tissue for pathological analysis.
Chemotherapy regimens (BEP) efficacy & sideeffects
The classic BEP combo (Bleomycin, Etoposide, Cisplatin) has been the backbone of treatment for decades. It works in roughly 80% of stage3 cases, but you may experience nausea, hair loss, and temporary fatigue. Most sideeffects are manageable with supportive meds.
Radiation & targeted therapies when theyre used
Radiation is mainly reserved for seminomas, especially when the disease is limited to lymph nodes. Targeted therapies and immunotherapy are still under investigation, but clinical trials are offering hope for patients with refractory disease.
Clinical trials & emerging therapies
If youre facing advanced disease, ask your oncologist about ongoing trials. New agents like PD1 inhibitors are showing promise, and participation can give you access to cuttingedge care.
Outlook Survival
Current testicular cancer survival rate (overall & stagespecific)
The overall fiveyear survival rate exceeds 95% for all stages combined, according to the American Cancer Society. For stage3, the rate drops to around 80%, still considerably high thanks to effective chemotherapy. Early detection remains the single most important factor in improving outcomes.
Factors that improve prognosis
Heres what can tip the scales in your favor:
- Detecting the tumor while its still localized.
- Being under 40 years old (younger patients tend to respond better).
- Having a seminomatous histology, which is more radiosensitive.
- Adhering strictly to treatment schedules and followup appointments.
Living beyond diagnosis: support groups & mental health
A cancer diagnosis can feel like an emotional roller coaster. Connecting with survivorswhether through online forums, local support groups, or counselinghelps you process fear and anxiety. Many men say that hearing a single story of triumph gave them the courage to keep fighting.
Key Takeaways
Advanced testicular cancer symptoms are more than a simple ache; they can involve lowback pain, swollen lymph nodes, chest discomfort, and even neurological changes. Recognizing these signs early, seeking prompt medical evaluation, and understanding the diagnosis pathway empower you to take control.
If any of the redflags described above ring a bell, dont wait. Perform a selfexam, book that appointment, and let a qualified health professional guide you through the next steps. Remember, knowledge isnt just powerits a lifeline. For more on outlook and life expectancy after prostate-related surgeries, some readers find broader cancer survival context helpful see prostate cancer outlook for additional perspective.
FAQs
What are the most common symptoms of advanced testicular cancer?
The most common symptoms include low back pain, painful or firm lumps in the abdomen or groin, chest pain, shortness of breath, headaches, and unexplained weight loss.
Can advanced testicular cancer cause neurological symptoms?
Yes, if the cancer spreads to the brain, it can cause headaches, visual changes, confusion, or other neurological deficits.
How does advanced testicular cancer affect the lungs?
When testicular cancer spreads to the lungs, it may cause chest pain, shortness of breath, and a persistent cough.
What should I do if I notice symptoms of advanced testicular cancer?
If you notice any symptoms, especially a lump, persistent pain, or swelling, see a doctor immediately for evaluation and testing.
Are there benign conditions that mimic advanced testicular cancer symptoms?
Yes, conditions like epididymitis, hydrocele, and inguinal hernia can cause similar symptoms but are generally less serious and require medical evaluation.