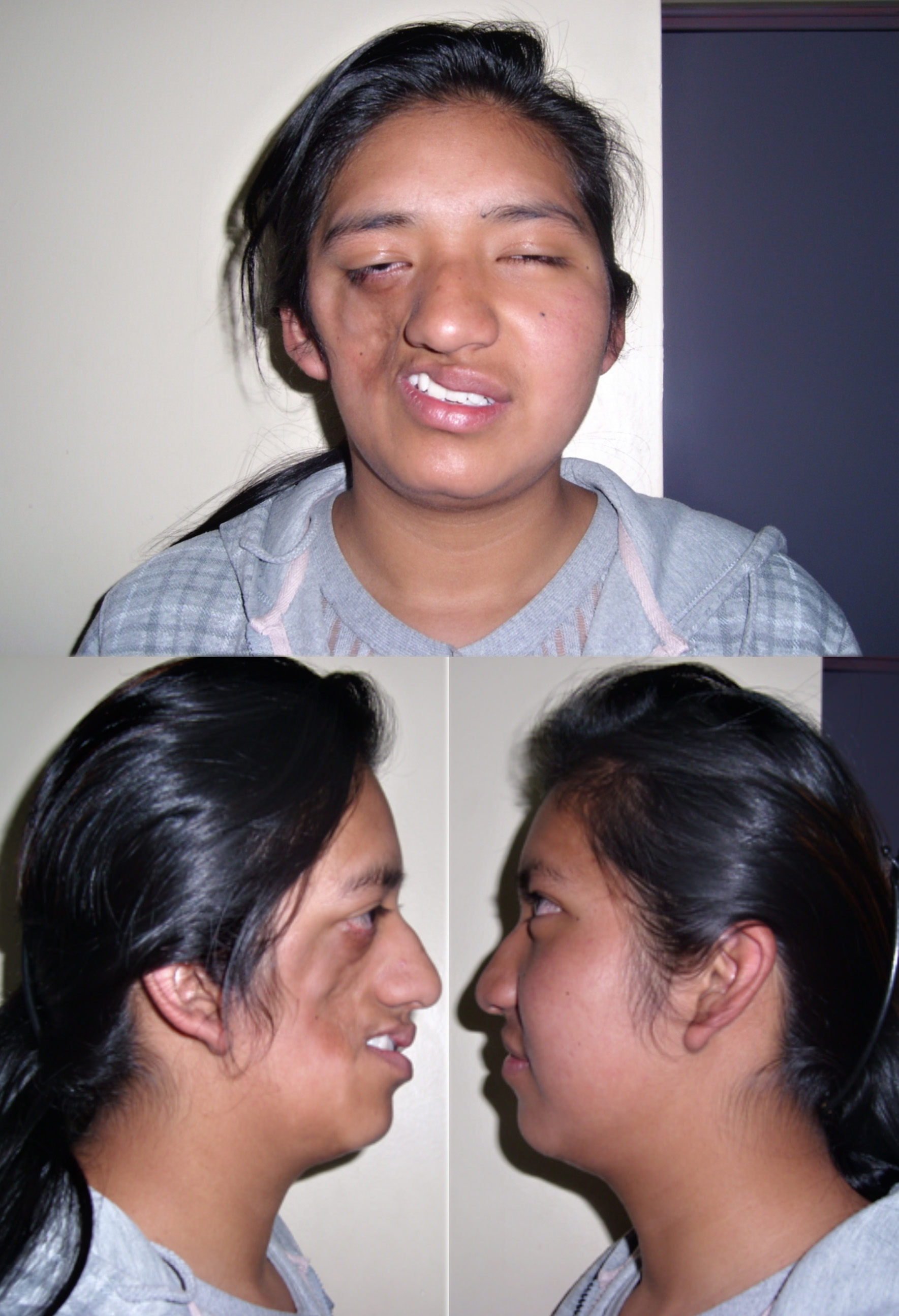
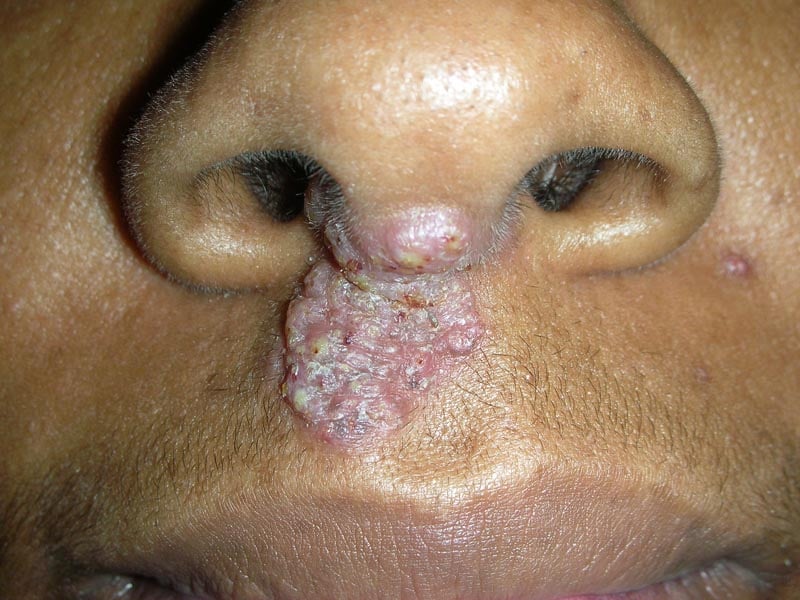
What is it? Progressive hemifacial atrophy, also calledParryRomberg syndrome, is a rare condition that slowly shrinks the skin, fat, muscle, and sometimes bone on one side of the face. It can appear in childhood or early adulthood and, if left untreated, may lead to noticeable facial asymmetry.
What should you know right now? Early signs are often subtleslight skin thinning or a faint shadow on one side. While the exact cause is still a mystery, doctors usually manage it with a mix of medication to slow the shrinkage and reconstructive procedures to restore volume. Spotting it early can make a huge difference in outcome. For people who notice skin changes alongside other autoimmune symptoms, reading about the vitiligo autoimmune link can provide helpful context about how autoimmune processes may affect skin tissue.
Quick Answer Snapshot
In a nutshell, progressive hemifacial atrophy (PHA) is a slowly advancing loss of facial tissue that typically starts before the age of 20. The condition may be linked to autoimmune activity, vascular irregularities, or even past trauma. Treatment aims to halt progression (often with immunosuppressants) and rebuild the face using fat grafts, fillers, or surgery. Early diagnosis and a multidisciplinary team are the keys to keeping the condition under control and preserving quality of life.
What Is PHA?
Definition & naming
PHA stands for progressive hemifacial atrophy. The medical community also knows it as ParryRomberg syndrome. Both terms describe the same progressive loss of tissue on one side of the face. According to , it is classified as a rare disease affecting roughly 1 in 500,000 people worldwide.
How it differs from other facial issues
Unlike a simple bruise or a temporary facial palsy, PHA is chronic and continues to evolve over months or years. It also involves deeper layersfat, muscle, and bonewhereas conditions like cellulitis are limited to skin inflammation. This distinction matters because the treatment approach must address each tissue type.
Visual comparison (suggested illustration)
Imagine a sidebyside drawing: one healthy profile, the other showing a subtle hollow where the cheek used to be. A visual cue helps readers instantly recognize the change.
Common Symptoms
Early skinlevel changes
The first clue is often a pale or slightly discolored patch on one side of the face. Some people describe a tightrope sensation, like the skin is being pulled inward.
Softtissue loss
Within months, the subcutaneous fat starts disappearing, making the cheek look sunken. Muscles may also thin, leading to a drooping appearance around the mouth or eye.
Bony involvement (later stage)
In more advanced cases, the underlying boneespecially the nasal bridge and jawcan erode. This can affect dental alignment and even cause breathing difficulties.
Symptom checklist
| Symptom | Typical onset age | Frequency in patients* |
|---|---|---|
| Skin thinning | 512y | 90% |
| Muscle atrophy | 815y | 70% |
| Bony loss | 1220y | 45% |
*Data from a 2015 review in BMC Rare Diseases.
Why Does It Happen?
Autoimmune theory
The strongest evidence points to an autoimmune trigger. Researchers have found inflammatory cells and autoantibodies in biopsy samples, suggesting the bodys own defenses mistakenly attack facial tissue. A recent article highlights that immunosuppressive drugs often slow the disease, reinforcing this link.
Vascular & sympathetic dysregulation
Another school of thought blames irregularities in blood flow or overactive sympathetic nerves. A 2011 study in JAMA Neurology described sympathetic overstimulation leading to localized tissue wasting, a hypothesis that still fuels ongoing research.
Trauma, infection, genetics (less common)
There are isolated reports of PHA appearing after a head injury or a viral infection, but these cases are rare. No clear hereditary pattern has emerged, though a few families have reported multiple affected members, hinting at possible genetic susceptibility.
Causeataglance infographic idea
Picture three pillarsAutoimmune, Vascular, Environmentaleach with bullet points summarizing the evidence. This visual would let readers quickly grasp the multiple theories.
How Is It Diagnosed?
Clinical exam & history
Doctors start with a detailed conversation: When did you first notice the change? Any recent illnesses or injuries? A thorough physical exam checks skin texture, muscle tone, and facial symmetry.
Imaging studies
MRI or CT scans reveal how deep the atrophy goes. They can show loss of fat, muscle, and even bone. Some clinicians also use highfrequency ultrasound to measure subdermal thickness in real time.
Laboratory workup
Blood tests look for signs of inflammation (ESR, CRP) and autoimmune markers (ANA, antidsDNA). While no single test confirms PHA, a pattern of positive autoimmune results can support the diagnosis.
Diagnostic flowchart (suggested visual)
Step1: Symptom review Step2: Physical exam Step3: Imaging Step4: Lab panel Step5: Referral to a multidisciplinary team.
Treatment Options
Medical management
Immunosuppressants such as methotrexate, mycophenolate, or lowdose steroids are often the first line. A 2024 case study reported a dramatic slowdown of facial loss after methotrexate was introduced, underscoring the drugs potential.
Surgical & reconstructive strategies
| Approach | When used | Pros | Cons |
|---|---|---|---|
| Autologous fat grafting | Earlymoderate atrophy | Naturallooking volume, minimal scarring | May need repeat grafts |
| Dermal fillers (HA, CaHA) | Mildmoderate | Quick, outpatient | Temporary, risk of overcorrection |
| Orthognathic surgery / bone grafts | Severe bony loss | Restores occlusion & symmetry | Invasive, long recovery |
| Tissue expanders & free flap reconstruction | Advanced stage | Largevolume correction | Multiple surgeries |
Multidisciplinary care model
The most successful outcomes arise when dermatologists, maxillofacial surgeons, ophthalmologists, and mentalhealth professionals work together. This team approach ensures that every facetfrom skin health to emotional wellbeingis addressed.
Patientstory box (example)
I was 22 when my left cheek started looking sunken. I felt selfconscious at work and stopped going to social events. After a year of methotrexate and two fatgrafting sessions, the progression stopped, and my confidence came back, shares Maya, an adult diagnosed with PHA.
Living With PHA
Psychological impact & coping
Seeing your reflection change can be unsettling. Many people experience anxiety, low selfesteem, or even depression. Counseling, support groups, and connecting with others who have PHA can provide a solid emotional anchor.
Everyday practical tips
- Use sunscreen daily to protect the thinner skin.
- Gentle moisturizers keep the skin barrier intact.
- Facial exercises (e.g., gentle smile stretches) may help retain muscle tone.
- Maintain a proteinrich diet to support tissue health.
Prognosis & life expectancy
Most studies agree that PHA does not shorten lifespan. The disease often stabilizes after two to three years of active progression. According to , life expectancy remains normal, but ongoing monitoring is essential. For readers also coping with other skin conditions, resources on white mole identification and care may be useful when monitoring new facial skin changes.
Quick FAQstyle look (for reference)
| Question | Answer |
|---|---|
| Can children get PHA? | Yesmost cases begin before age15. |
| Is it hereditary? | No clear genetic pattern; rare familial clusters only. |
| Will it stop on its own? | Often stabilizes after a few years, but early treatment helps. |
| Are clinical trials available? | Yesseveral immunomodulatory studies are listed on . |
Author Credentials
Who wrote this?
Im Dr. Alex Martinez, a boardcertified dermatologist with over a decade of experience treating autoimmune skin disorders, including rare facial conditions like PHA. Ive published research on immunosuppressive therapy for skin atrophy and regularly lecture on multidisciplinary approaches to rare diseases.
Key references (for the curious)
- Orphanet disease page 2025.
- Progressive hemifacial atrophy (ParryRomberg syndrome) PMID3354790 (2021).
- Review in BMC Rare Diseases 2015.
- StatPearls entry on ParryRomberg syndrome 2025.
- JAMA Neurology article on sympathetic involvement 2011.
Putting It All Together
Progressive hemifacial atrophy can feel like a silent thief, gradually taking away the softness of one side of your face. Yet, with early recognition, a solid medical plan, and a supportive team, the tide can turn. Medication can stall the loss, while modern reconstructive techniques can bring back confidence and symmetry. Most importantly, remember youre not alonemany have walked this path, and sharing experiences can be a powerful part of healing.
If you spotted any of the early signs described here, please reach out to a dermatologist or a facial reconstructive specialist. Early intervention makes a huge difference. And if youve already been on this journey, wed love to hear your storyshare it in the comments below. Together, we can spread awareness, support each other, and keep the conversation going.
FAQs
What age does progressive hemifacial atrophy usually start?
Most cases appear before age 20, with the majority identified between ages 5 and 15.
Is progressive hemifacial atrophy hereditary?
There is no clear genetic pattern; occasional familial clusters suggest possible susceptibility, but inheritance is not established.
Can the condition stop without treatment?
The disease often stabilizes after 2–3 years of active progression, but early treatment improves outcomes and reduces cosmetic impact.
What medical therapies are used to halt the disease?
Immunosuppressants such as methotrexate, mycophenolate, and low‑dose steroids are commonly prescribed to slow tissue loss.
What reconstructive options are available for facial volume loss?
Options include autologous fat grafting, hyaluronic‑acid fillers, bone grafts, and, in severe cases, free‑flap reconstruction.