FAQs
What does ultrasound reveal in cervical cancer assessment?
Trans‑vaginal ultrasound provides a quick, non‑invasive look at the cervix, detecting hypoechoic masses, assessing size, and evaluating blood flow with Doppler. It’s ideal for initial screening, especially in low‑resource settings.
Why is MRI considered the gold standard for cervical cancer staging?
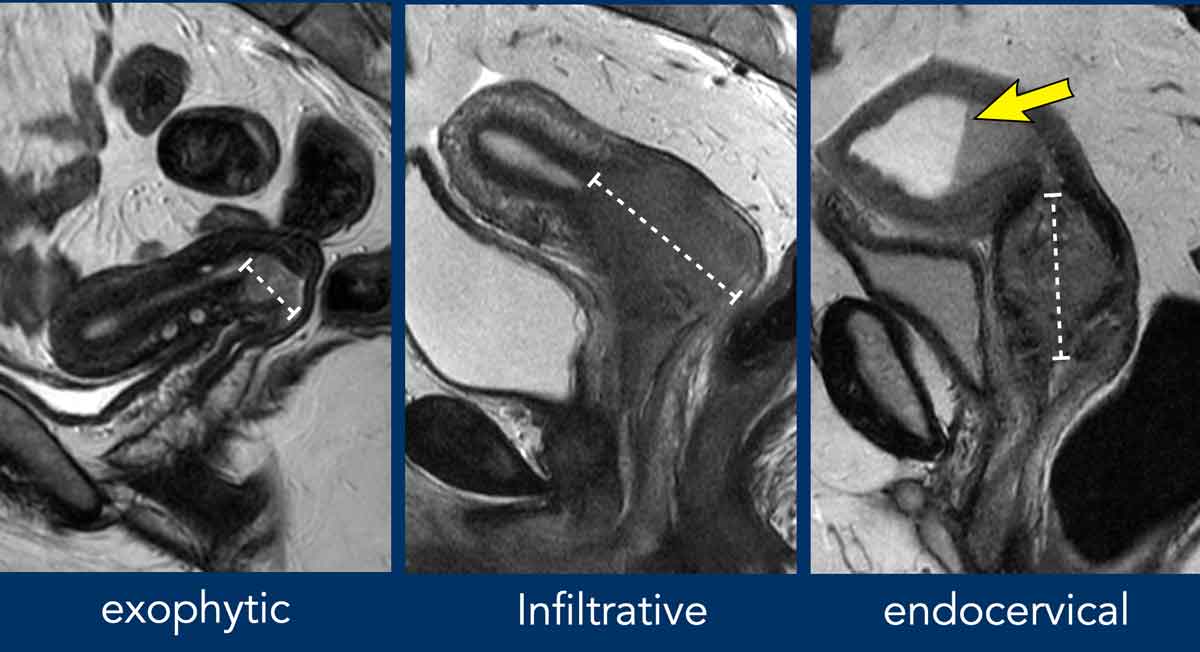
MRI offers superior soft‑tissue contrast and multiplanar imaging, allowing precise evaluation of tumor size, parametrial invasion, uterine involvement, and lymph node status—critical factors for FIGO staging and treatment decisions.
How does imaging influence treatment planning for cervical cancer?
Accurate imaging defines tumor boundaries for surgery or radiation. MRI data are used to contour radiotherapy targets and to decide if a patient is a candidate for fertility‑preserving surgery versus definitive chemoradiation.
Are there any risks or limitations associated with these imaging modalities?
Ultrasound is operator‑dependent and may miss deep lesions behind bowel gas. MRI contraindications include certain metal implants, severe claustrophobia, and rare gadolinium reactions in patients with poor kidney function.
Can cervical cancer be detected early using imaging alone?
While imaging can identify suspicious lesions, early detection still relies on routine screening (Pap smear, HPV testing). Imaging confirms and stages a lesion once clinical suspicion arises.