Short answer: vitaminD alone wont magically fix osteoporosis, but getting enough of it (along with calcium) can slow bone loss, modestly improve bonemineral density, and lower your fracture risk. Think of it as a supportive teammate, not a solo MVP.
Why does this matter? Because many of us hear headlines like VitaminD cures osteoporosis and rush to take huge doses that may do more harm than good. Knowing the real science lets you use vitaminD safely, combine it with the right foods, and keep your skeleton strong without unnecessary risk.
Quick Verdict
Can vitamin D alone reverse osteoporosis?
In short, no. The consensus from major health organizationsNIH, the World Health Organization, and the International Osteoporosis Foundationstates that vitaminD is a necessary part of bone health, but it isnt a standalone cure. The best you can expect is a slower rate of bone loss and a small bump in bonedensity numbers when you pair it with adequate calcium and healthy lifestyle habits.
What does reverse really mean?
When doctors talk about reversing osteoporosis, they usually mean two things: raising the bonemineral density (BMD) score enough to move from the osteoporotic range into the osteopenic or even normal range, and reducing the chance of fractures. VitaminD helps with the first part, but the improvement is modestoften just a few percent over a year. The bigger win is the reduction in fracture risk that comes from stronger bones and better calcium absorption.
Bone Basics
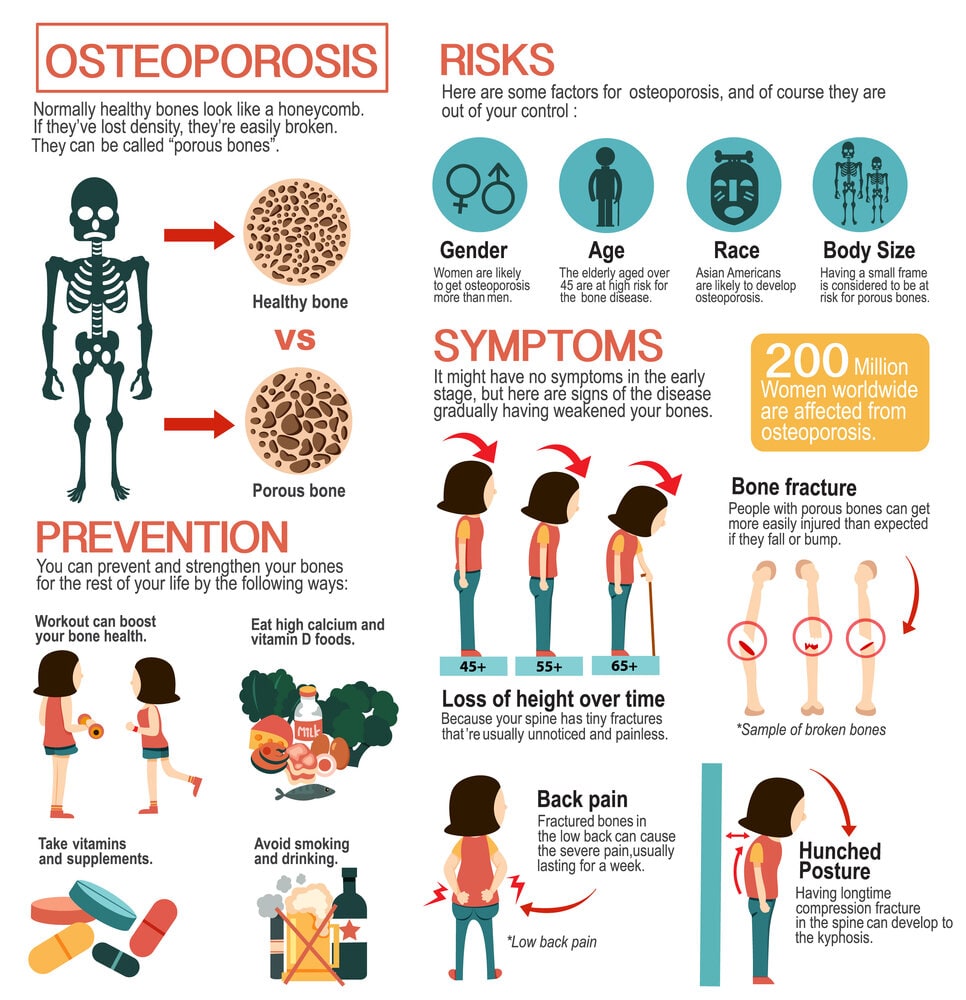
What is osteoporosis?
Osteoporosis is a condition where your bones become porous and fragile, making them prone to breaks. Its usually diagnosed via a DXA scan that measures BMD and gives you a Tscore. A score of 2.5 or lower means osteoporosis; between 1.0 and 2.5 is called osteopenia, a warning zone before fullblown osteoporosis.
How does vitamin D help bones?
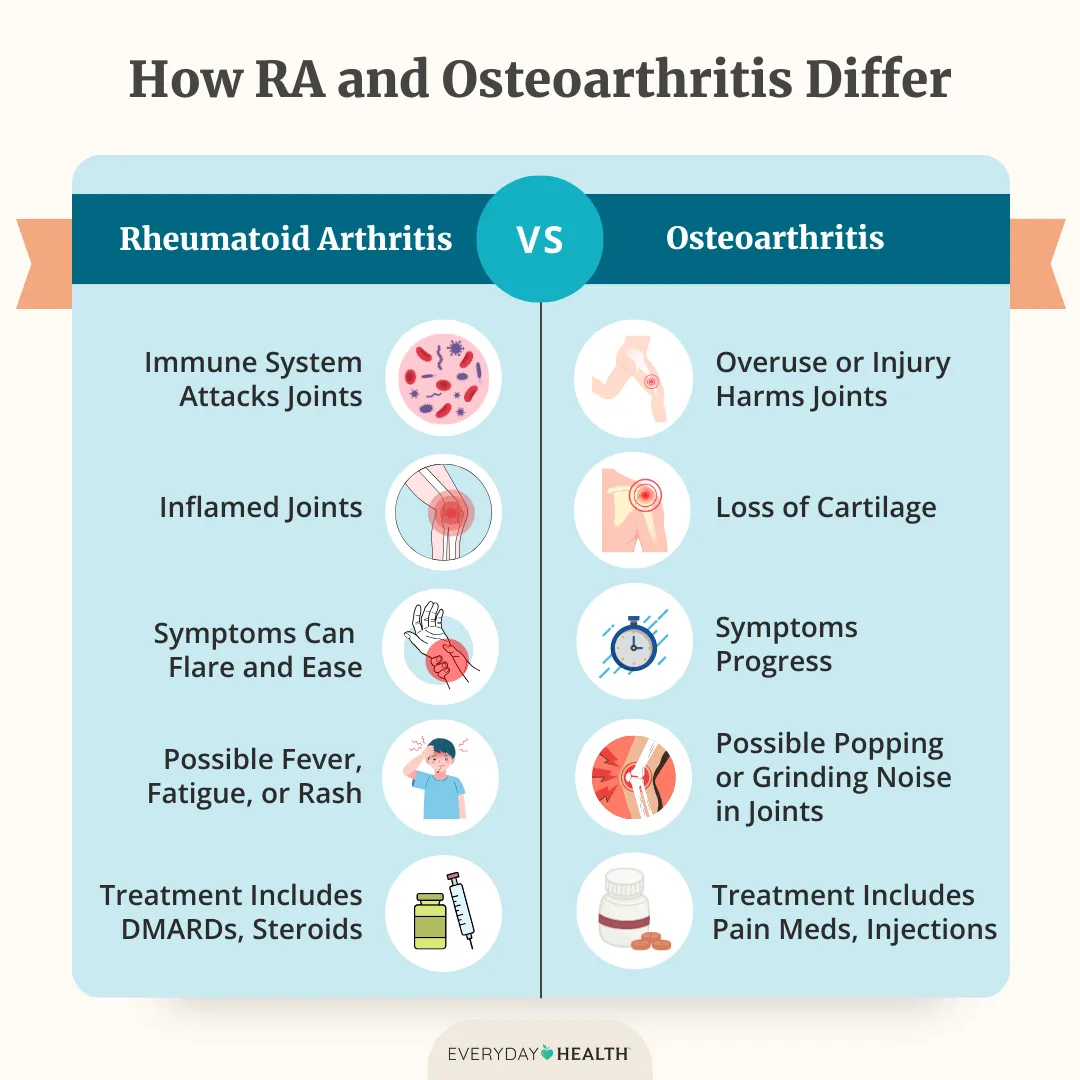
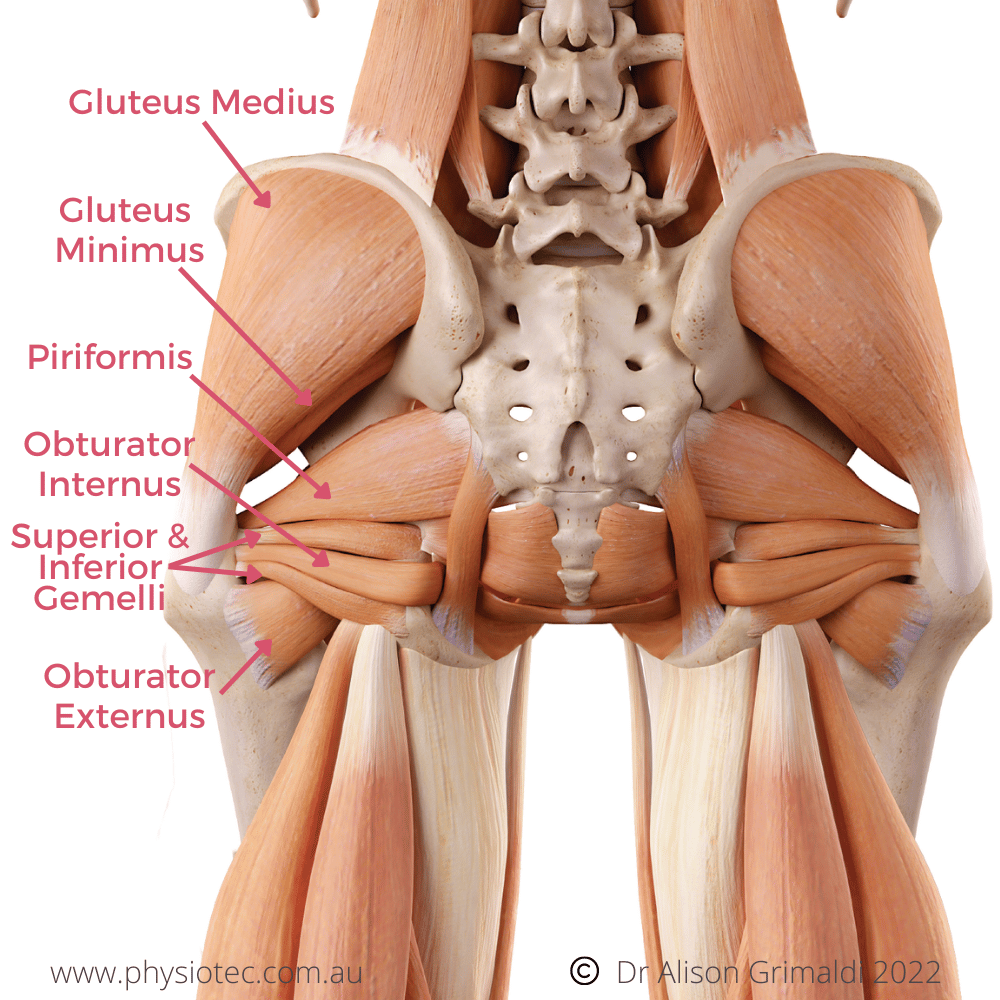
VitaminD isnt a bonebuilding hormone itself; its more like a traffic controller. It tells your intestines to absorb calcium from food, helps the kidneys keep calcium in the blood, and reduces the secretion of parathyroid hormone (PTH), which, when high, can leach calcium out of bones. In short, without enough vitaminD, the calcium you eat often ends up in the bathroom instead of your skeleton. If you have other inflammatory conditions that affect posture or mobility (for example, spine inflammation), keeping vitaminD and calcium optimized can help support mobility and reduce secondary bone loss.
Science Evidence
Key clinical trials
Several large metaanalyses from the past five years have looked at vitaminD supplementation in people with low BMD. A 2022 review of 33 randomized controlled trials (over 20,000 participants) found that combined calcium+vitaminD modestly improved BMD by about 12% compared with placebo, but highdose vitaminD (>4,000IU/day) added no extra benefit and sometimes increased the risk of hypercalcemia.
Another study published in showed that participants who corrected a vitaminD deficiency (<20ng/mL) saw a small but measurable rise in spine BMD after 12 months, especially when they also took the recommended 1,200mg of calcium daily.
Does vitamin D affect bonedensity test results?
VitaminD itself doesnt change the DXA machines reading, but low vitaminD can lead to secondary hyperparathyroidism, which accelerates bone loss and may result in lower BMD scores. In other words, if youre deficient, your test could look worse than it would if you had optimal vitaminD levels.
Dosage Details
Recommended intake for osteoporosis
Heres a quick cheatsheet you can keep on your fridge:
| Age / Condition | Calcium (mg/day) | VitaminD (IU/day) | Notes |
|---|---|---|---|
| Women50yrs (osteoporosis) | 1,200 | 8001,000 | Check blood level; adjust up to 2,000IU if deficient |
| Men70yrs (osteoporosis) | 1,200 | 8001,000 | Same as women |
| Osteopenia (any adult) | 1,0001,200 | 600800 | Focus on diet first |
These numbers follow the and are a solid starting point.
Highdose vitaminD: pros and cons
Highdose usually means 4,000IU+per day. Some doctors prescribe it for a short loading period if youre severely deficient, but the evidence says the benefits plateau after you hit a serum 25OHD level of about 30ng/mL. Going higher can raise calcium too much, leading to kidney stones, nausea, or even calcification of soft tissues. The safest route is to aim for the recommended range, test your blood after 812 weeks, and adjust only under medical supervision.
Benefits vs Risks
Potential side effects of excess vitaminD
When you exceed the tolerable upper intake level (4,000IU for most adults), you risk hypercalcemiasymptoms include excessive thirst, frequent urination, weakness, and in severe cases, heart rhythm problems. Its rare, but it does happen when people selfprescribe megadoses based on internet hype.
Interactions with osteoporosis medicines
If youre on bisphosphonates (like alendronate) or denosumab, make sure you take calcium and vitaminD as directedusually 30minutes before the medication. Some boneactive drugs actually work better when calcium and vitaminD levels are optimal, so think of these nutrients as the fuel your medication needs to run efficiently.
Realworld case study
Meet Linda, a 68yearold retired teacher. Her DXA scan in 2021 showed a Tscore of 2.7 (osteoporosis). Her doctor ordered a 25OHD testresult: 15ng/mL, clearly deficient. Linda started taking 1,000IU of vitaminD daily plus 1,200mg of calcium, and began weightbearing exercises (walking, light resistance bands). After 12 months, her serum vitaminD rose to 32ng/mL, and her spine BMD improved by 1.8%. She didnt cure osteoporosis, but she slowed the decline and reduced her fracture risk. Lindas story illustrates how a balanced approachadequate nutrients, safe dosing, and activitymakes a real difference.
Practical Tips
Best food sources of vitaminD
Sunlight is the cheapest source, but if you live in a cloudy climate or spend most of your day indoors, youll need dietary help. Fatty fish (salmon, mackerel), fortified dairy or plant milks, and UVtreated mushrooms are top picks. A simple threeday meal plan could look like this:
- Breakfast: fortified oatmeal with a splash of almond milk.
- Lunch: grilled salmon salad with leafy greens and a squeeze of lemon.
- Dinner: sauted mushrooms with a side of broccoli and quinoa.
That combo gives you roughly 400600IU of vitaminD plus a solid calcium boost.
Choosing the right supplement
When you shop, look for vitaminD3 (cholecalciferol) rather than D2, because D3 raises blood levels more reliably. Pick a product thats USPverified or has a thirdparty seal (NSF, InformedChoice). Common doses on the market range from 400IU to 5,000IU per capsule. For most adults with normal levels, 8001,000IU is enough; if youre deficient, a doctor may suggest 2,000IU for a short period. If you also have concerns about bone strength related to overall bone density and therapy options, consider reading more about bone density therapy to understand broader management strategies: bone density therapy.
CalciumvitaminD synergy
Timing matters. Calcium competes with iron and zinc for absorption, so take your calcium supplement at a different meal than ironrich foods (like red meat). VitaminD can be taken any time of day, but pairing it with your biggest calciumrich meal (breakfast or dinner) helps your gut absorb the calcium more efficiently.
Lifestyle boosters
Beyond nutrients, weightbearing activity (walking, dancing, slow jogging) sends a mechanical signal to bone cells to strengthen. Aim for at least 30 minutes most days. Also, a daily 10minute sunlight exposure (arms and face) in the spring or summer can add 1,0002,000IU of vitaminD naturally. Quit smoking, limit excessive alcohol, and keep a healthy weightthese factors all protect bone health.
Bottom Line
Key takeaways
- VitaminD alone cannot reverse osteoporosis, but it is essential for slowing bone loss and modestly improving BMD when combined with calcium.
- Follow the recommended intake (8001,000IU daily for most adults with osteoporosis; up to 2,000IU if youre deficient) and avoid highdose experiments unless a doctor advises.
- Balance is criticalpair vitaminD with adequate calcium, regular weightbearing exercise, and a diet rich in vitaminD foods.
- Monitor blood levels after a few months; adjust only under professional guidance to stay safely within the tolerable upper intake.
In short, think of vitaminD as a trustworthy sidekick rather than a superhero. Keep the doses reasonable, listen to your body, and work with a health professional to craft a personalized plan. If youre wondering whether you need a blood test or how to fit supplements into your daily routine, reach out to your doctor or a qualified nutritionist. Your bones will thank you for the thoughtful, balanced approach.
FAQs
Can vitamin D alone reverse osteoporosis?
No, vitamin D alone cannot reverse osteoporosis. It helps slow bone loss and modestly improve bone mineral density when taken with calcium and healthy lifestyle habits, but it is not a standalone cure.
How does vitamin D support bone health in osteoporosis?
Vitamin D aids bone health by promoting calcium absorption in the intestines, reducing calcium loss through kidneys, and controlling parathyroid hormone levels that can otherwise cause bone calcium loss.
What is the recommended vitamin D dose for osteoporosis?
Adults with osteoporosis typically need 800-1,000 IU of vitamin D daily, with up to 2,000 IU if deficient, combined with about 1,200 mg of calcium daily, following medical guidance.
Are high doses of vitamin D beneficial for osteoporosis?
High-dose vitamin D (above 4,000 IU daily) has not shown additional bone benefits and may cause harm such as hypercalcemia; safe supplementation within recommended doses is advised.
Can vitamin D supplements reduce fracture risk?
Combined vitamin D and calcium supplementation modestly reduces fracture risk—studies show about 6% reduction in any fracture and 16% reduction in hip fractures when taken consistently over years.