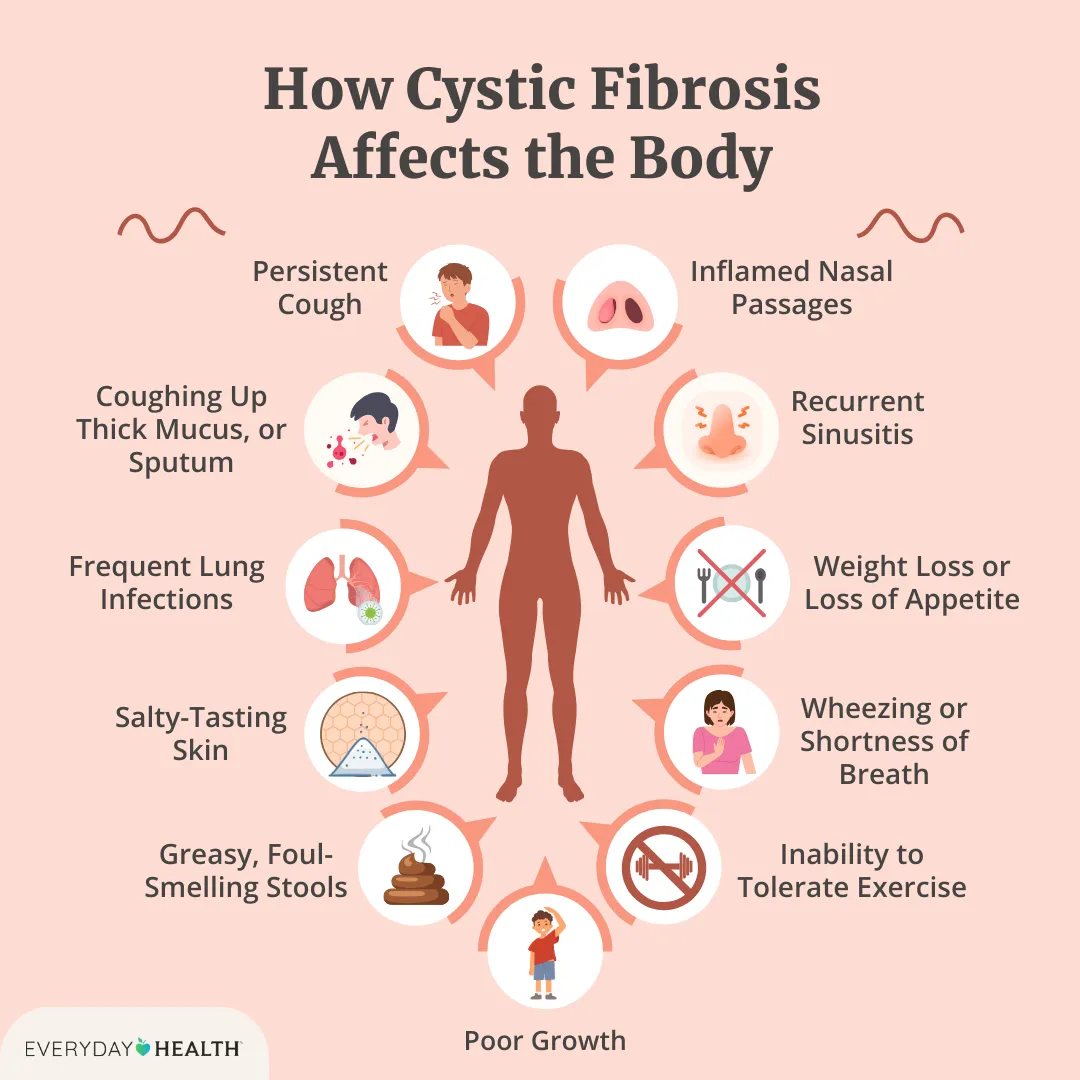
Ever caught yourself thinking a wheeze is just a cold and then discovered it's actually asthma lung inflammation? It feels like a hidden fire breathing down your throat, right? In the next few minutes, we'll clear the smoke: what sparks the inflammation, why type2 inflammation matters, and which treatments actually calm the blaze before it harms your lungs. Understanding such respiratory conditions can also help highlight the importance of managing chronic conditions like cystic fibrosis relationships and cystic fibrosis safety, where airway management is crucial.
Quick Answer Snapshot
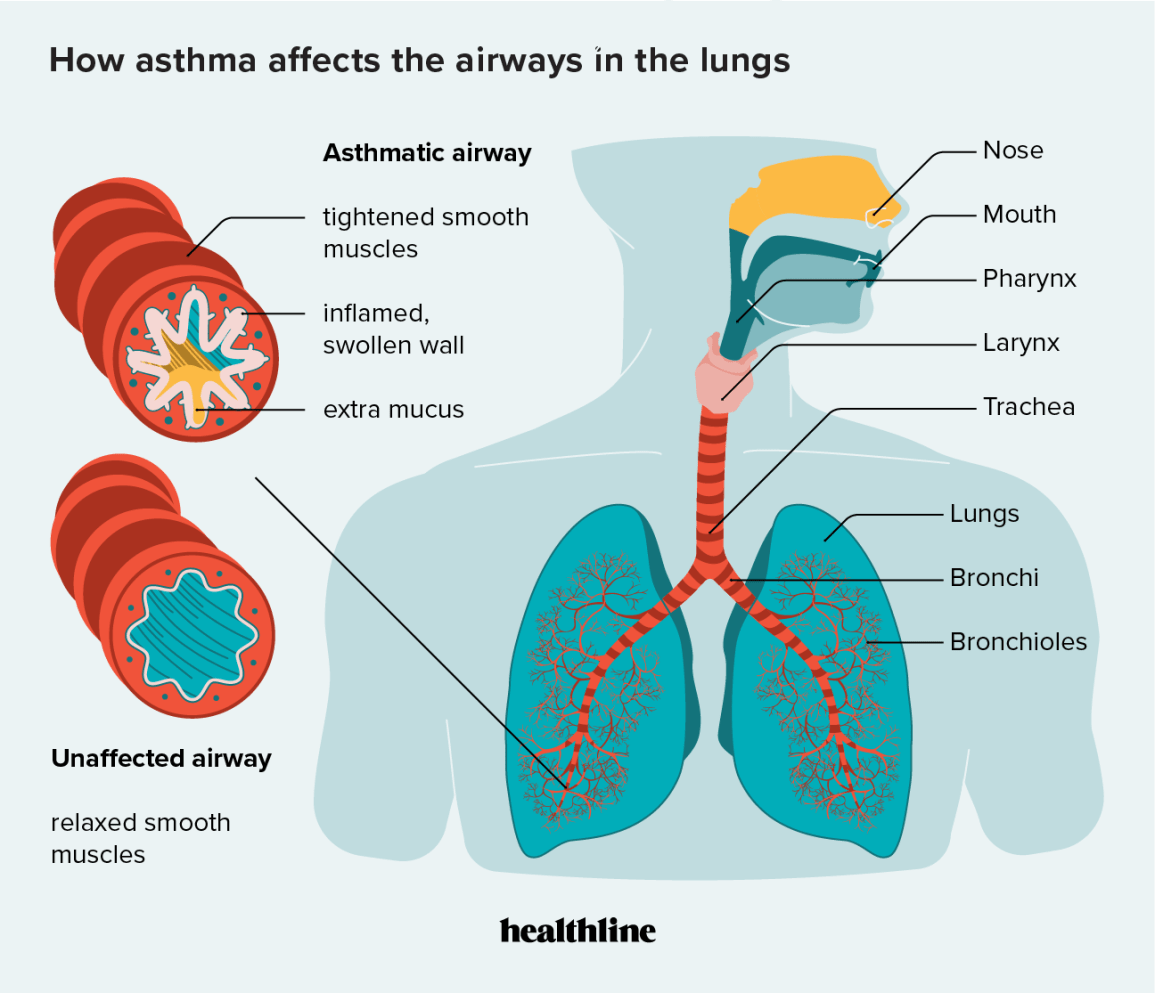
What is asthma lung inflammation?
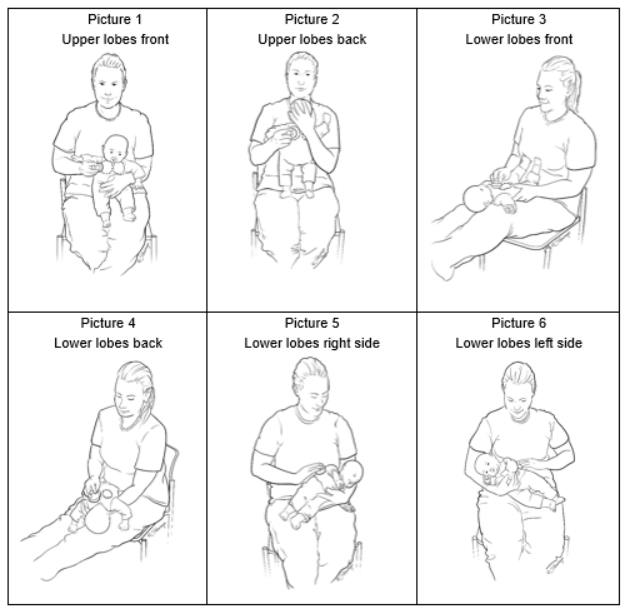
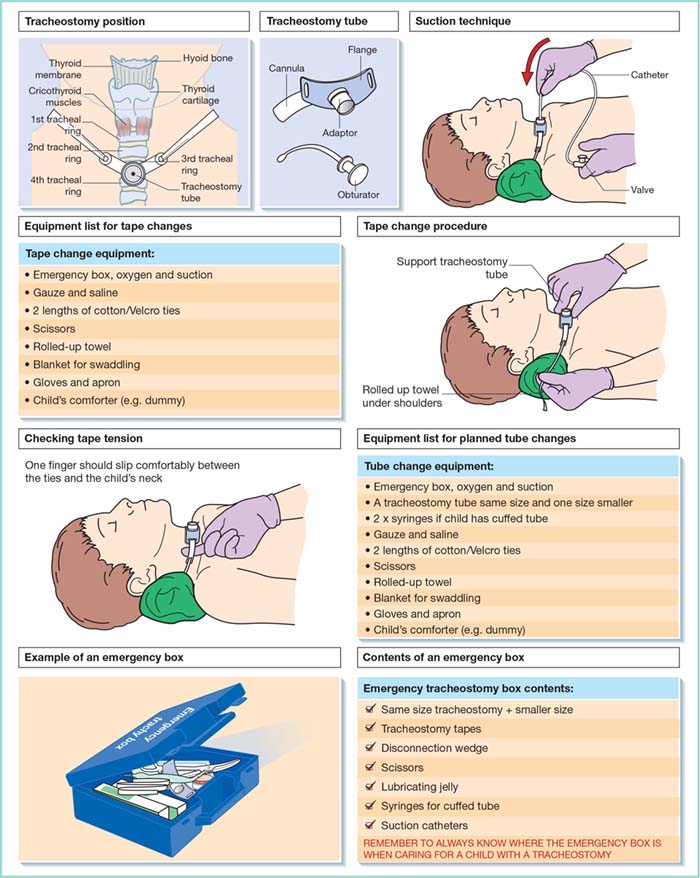
In plain terms, it's the chronic swelling of the airways that makes breathing feel like pushing a straw through a clogged pipe. The lungs aren't broken; they're inflamed, reacting to triggers that convince the immune system to overreact. For conditions like cystic fibrosis, maintaining clear airways is essential for preventing infections, often through techniques like cystic fibrosis airway clearance.
How common is type2 inflammation?
About 50-70% of people with asthma show a type2 patternthat's the allergy-driven pathway involving cytokines like IL4, IL5, and IL13. Recognizing this subset is crucial for picking the right therapy.
Can asthma kill you?
Severe asthma attacks can be life-threatening, especially when inflammation spikes and the airways close off. The good news? Proper control and early treatment dramatically cut that risk.
Key risk factors
Age (young children & seniors), high-dose steroid use, smoking, and comorbid conditions like chronic sinusitis or obesity can turn a manageable flare into an emergency.
FAQs
What exactly is asthma lung inflammation?
It is the chronic swelling of the airway walls that makes breathing feel like pushing a straw through a clogged pipe, driven by immune‑cell activity.
How does type 2 inflammation differ from other asthma types?
Type 2 inflammation is allergy‑driven, marked by high IL‑4, IL‑5, IL‑13, eosinophils and FeNO, and usually responds well to inhaled steroids and biologics.
Which triggers are most likely to worsen asthma lung inflammation?
Common triggers include pollen, dust‑mites, pet dander, smoke, strong odors, cold air, and respiratory infections.
When should I consider a biologic medication for my asthma?
If you have persistent high eosinophils or frequent exacerbations despite high‑dose inhaled corticosteroids, a biologic targeting IL‑5, IL‑4Rα or IgE may be appropriate.
What are the emergency signs of a life‑threatening asthma attack?
Inability to speak full sentences, bluish lips, or a peak‑flow reading below 50 % of your personal best require immediate emergency care.