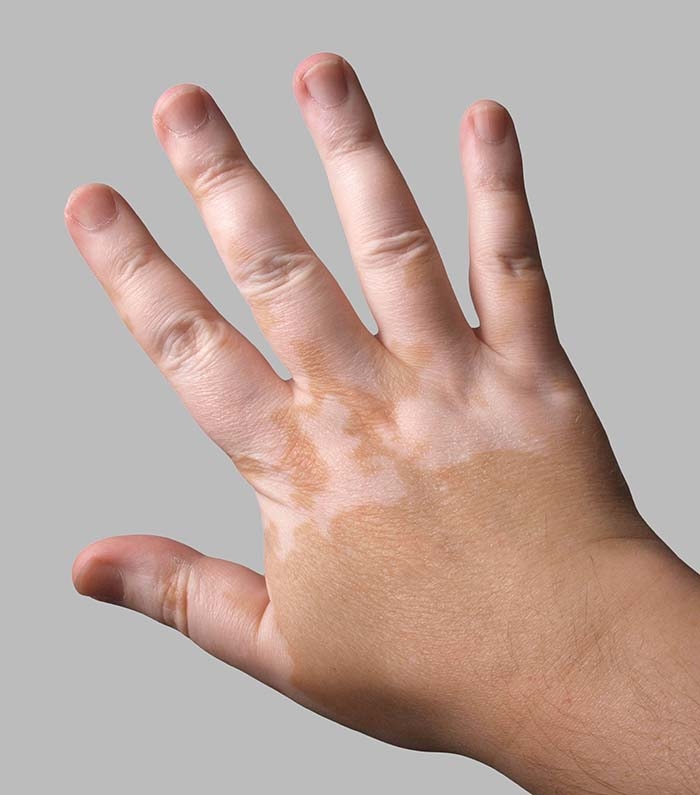
Seeing a new white patch appear on your arm can feel like your skin is sending you an urgent, silent SOS. Youre probably wondering: whats actually causing this? The short answer is that vitiligo is usually the result of three big players an overactive immune system, your genetic blueprint, and certain environmental hits. Knowing these triggers not only clears up the mystery, it also gives you the power to spot early signs, manage risk, and choose the right treatment path.
In the next few minutes well walk through the science, share realworld stories, and give you practical tips to keep vitiligo from spreading all in a friendly, nojargon way. Ready? Lets dive in.
QuickHit Triggers
Autoimmune Attack
At its core, vitiligo is an autoimmune condition. This means the bodys defense troops mistakenly target melanocytes the skin cells that produce melanin, the pigment that gives us our color. When these cells are destroyed, the skin loses its pigment, creating the characteristic white patches.
Research from the notes that people with vitiligo often have other autoimmune diseases like thyroid disorders or type1 diabetes, underscoring how the immune system can go offtrack in multiple ways.
Genetic Predisposition
Family history matters. If a close relative has vitiligo, your odds of developing it rise to roughly 2030%. Scientists have identified several genes NLRP1, PTPN22, and certain HLADR variants that increase susceptibility. These genes are more common in people of South Asian, African, and Hispanic ancestry, which is why vitiligo appears more frequently in those groups.
According to a 2023 study published in Nature Genetics, twins who share all their DNA are about three times more likely to both have vitiligo compared to nonidentical siblings, further cementing the genetic link.
Environmental Hits
Even with the right genes and an overactive immune system, vitiligo often needs a spark to appear. Common environmental triggers include:
- Sunburn or intense UV exposure paradoxically, while UV light is a treatment tool, uncontrolled exposure can accelerate pigment loss.
- Chemical irritants phenols, catechols, and certain cleaning agents can harm melanocytes.
- Physical trauma cuts, burns, friction, or even a tattoo can set off the , where new patches form at sites of skin injury.
- Severe stress chronic emotional stress can influence immune regulation, making the skin more vulnerable.
Deeper Dive
Autoimmune Disorders & Vitiligo
When you have vitiligo, its smart to screen for related autoimmune conditions. Thyroid disease is the most common companion, affecting up to 30% of vitiligo patients. Other links include pernicious anemia and Addisons disease. Regular blood tests can catch these early, giving you a headstart on treatment.
Genetic Factors & Heredity
Specific gene variations change how your immune system recognizes melanocytes. For example, the NLRP1 gene influences inflammasome activity, a key component in autoimmune inflammation. While you cant change your DNA, knowing your family history lets you and your doctor stay vigilant.
Environmental Triggers
Lets break down the most frequent culprits:
Chemical Exposure
Household products containing phenols (like certain detergents) can be absorbed through the skin. If you work in an industry that uses industrial dyes or phenolic compounds, consider protective gloves and frequent hand washing.
Sunlight & UV Damage
Excessive sun can cause oxidative stress that harms melanocytes. Yet, controlled narrowband UVB therapy is a cornerstone treatment because it encourages repigmentation. The key is moderation: use broadspectrum SPF50+, wear hats, and avoid sunburn at all costs.
Physical Trauma (Koebner Phenomenon)
Ever noticed a new white spot after a cut? Thats the Koebner response in action. Even minor friction from tight clothing or sports equipment can trigger it.
Oxidative Stress & NeuroChemical Factors
Melanocytes are vulnerable to free radicals. When the balance tips toward oxidative stress, pigment cells die faster. Antioxidantrich diets (berries, leafy greens) and topical creams with vitamins C and E may offer supportive care, though theyre not standalone treatments.
AgeSpecific Causes
Vitiligo in children often appears spontaneously, while adultonset vitiligo is more frequently linked to new autoimmune diagnoses or heightened stress levels. Recognizing this can guide doctors toward appropriate tests for underlying conditions.
Is Vitiligo Dangerous?
On its own, vitiligo isnt lifethreatening. However, because it can signal other autoimmune disorders, its a flag that warrants a comprehensive health check. Psychologically, the visible changes can affect confidence, so mentalhealth support is an essential component of care.
How It Spreads
The Koebner Phenomenon Explained
When skin is injured, inflammatory signals flare up. In people predisposed to vitiligo, these signals mistakenly direct immune cells to attack nearby melanocytes, creating fresh patches that follow the line of the injury. Thats why even a tiny scratch can become a new white streak.
Sunburn & UV Exposure
Unprotected sun can speed up depigmentation. UV rays generate reactive oxygen species, amplifying the oxidative stress that already threatens melanocytes. This explains why many patients report rapid spread after a beach day gone wrong.
Stress & Hormonal Shifts
Longterm stress releases cortisol, which can dysregulate immune function. A 2022 longitudinal study found that patients who reported high stress levels experienced a 40% faster spread of vitiligo patches compared to lowstress peers.
RealWorld Story
Maria, a 34yearold graphic designer, noticed a small white spot on her forearm after a stressful deadline. Within weeks, the patch expanded, and similar spots appeared on her neck. After a dermatologist confirmed vitiligo, she started stressmanagement techniques (mindfulness, yoga) alongside phototherapy, and her spread slowed dramatically.
Prevention & Risk Reduction
Lifestyle Tweaks
Simple daily habits can make a big difference:
- Apply broadspectrum SPF50+ every morning, even on cloudy days.
- Wear protective clothing (long sleeves, hats) when outdoors.
- Avoid harsh chemicals choose gentle, fragrancefree skin products.
- Stay hydrated; healthy skin is more resilient.
Medical Monitoring
If you have a family history of vitiligo or an existing autoimmune condition, schedule regular checkups. Blood panels that screen for thyroid antibodies, glucose levels, and adrenal function can catch associated disorders early.
Early Intervention Strategies
Spot a new white patch? Dont wait months. Book a dermatologist appointment within three months. Early treatment optionstopical steroids, calcineurin inhibitors, or narrowband UVBwork best before the patch becomes fully depigmented.
QuickStart Checklist for New Spots
| Action | Why It Helps |
|---|---|
| Schedule dermatologist visit (within 3 months) | Early-stage treatments are more effective |
| Ask about topical steroids or calcineurin inhibitors | Reduce immune attack on melanocytes |
| Discuss phototherapy options | Stimulates repigmentation safely |
| Check thyroid and autoimmune labs | Identify hidden health issues |
Treatment Overview Linking Causes to Therapy
Why Knowing the Cause Matters
When you understand whether autoimmunity, genetics, or environmental factors are driving your vitiligo, you can choose treatments that target those mechanisms. For example, if autoimmunity is dominant, immunomodulating drugs like topical steroids or JAK inhibitors become frontline options.
Current GoldStandard Options (2025)
- Topical corticosteroids reduce inflammation and immune activity.
- Calcineurin inhibitors (tacrolimus, pimecrolimus) especially useful on delicate facial skin.
- Narrowband UVB phototherapy stimulates melanocyte migration.
- Excimer laser targeted light therapy for small, resistant patches.
- JAK inhibitors (tofacitinib, ruxolitinib) newer drugs that block inflammatory pathways.
- Surgical grafts (minipunch grafting) for stable vitiligo not responding to other treatments.
Emerging Treatments Tied to Causes
Scientists are exploring geneediting approaches that could correct the underlying genetic susceptibility, though these are still in early trials. Antioxidant creams and microbiomemodulating shampoos are also showing promise for supporting melanocyte health.
Whats the buzz on JAK inhibitors?
| Pros | Cons |
|---|---|
| Effective for rapidly spreading vitiligo | Potential systemic side effects; requires monitoring |
| Can be used topically (ruxolitinib cream) | Cost may be high without insurance |
| Targets immune pathway directly | Longterm safety data still limited |
Balancing Benefits & Risks
Every treatment carries a tradeoff. Topical steroids can thin the skin if used longterm, while phototherapy requires repeated clinic visits and strict eye protection. The best approach is a personalized plan crafted with your dermatologist, your medical history, and your lifestyle in mind.
Putting It All Together
Understanding vitiligo causes isnt just an academic exerciseits the first step toward proactive care. Whether the trigger is an overzealous immune system, a familylinked gene, or a sunburn you forgot to treat, you now have a roadmap:
- Know the triggers autoimmunity, genetics, environment.
- Watch for early signs any new white patch deserves attention.
- Protect your skin sunscreen, gentle products, avoid trauma.
- Get checked regular labs for related autoimmune conditions.
- Seek early treatment the sooner you act, the better the outcome.
Remember, youre not alone on this journey. Millions worldwide navigate vitiligo daily, and the medical community is constantly unlocking new ways to manage it. If anything in this guide sparked a question or you have a story to share, drop a comment below. Your experience could be the encouragement someone else needs.
Take the first step today: protect your skin, stay informed, and partner with a trusted dermatologist. Together, we can turn uncertainty into confidence. For readers dealing with itchy skin reactions that sometimes accompany autoimmune conditions, gentle natural options like hives relief herbs may provide symptom support always check with your clinician before starting any herbal remedy.
FAQs
What are the main causes of vitiligo?
Vitiligo is primarily linked to an over‑active immune system that attacks melanocytes, genetic susceptibility, and environmental triggers such as sunburn, chemicals, and skin trauma.
Can vitamin deficiencies cause vitiligo?
While vitamin deficiencies alone don’t cause vitiligo, low levels of antioxidants (like vitamins C and E) can worsen oxidative stress, which may accelerate pigment loss in susceptible individuals.
Is stress really a factor in vitiligo development?
Yes. Chronic emotional stress can disrupt immune regulation, making the skin more vulnerable to autoimmune attacks and potentially speeding up the spread of white patches.
Does sun exposure make vitiligo worse?
Uncontrolled UV exposure can increase oxidative stress and accelerate depigmentation, although controlled narrow‑band UVB therapy is used as a treatment to stimulate repigmentation.
Should I get screened for other autoimmune diseases if I have vitiligo?
Absolutely. About 30 % of people with vitiligo also have thyroid disease or other autoimmune conditions, so regular blood tests are recommended to catch any related issues early.