Ever wonder why some people develop breathing problems or liver issues seemingly out of nowhere? The short answer is that a tiny hiccup in a single gene can set off a chain reaction, leading to what doctors call alpha1 antitrypsin deficiency. Below, Im breaking down exactly what causes this condition, how it shows up in the body, and what you can do to stay ahead of itall in a conversationstyle guide thats easy to follow.
Understanding Genetic Blueprint
What gene is behind the story?
The culprit is the SERPINA1 gene. Think of this gene as a set of blueprints for a protein called alpha1 antitrypsin (AAT). When the blueprint is flawless, your liver churns out enough AAT to keep your lungs and liver happy.
Common variants and their impact
Most folks with the condition carry one of two wellknown mutations:
- Pi*Z (E342K) the heavyweight champion of deficiency. It drastically lowers the amount of functional AAT and is linked to severe lung and liver disease.
- Pi*S (E264V) a milder version that still reduces AAT but usually results in a slower disease progression.
- There are also rare null alleles that produce little to no AAT at all.
Variant Comparison Table
| Variant | AAT Level (mg/dL) | Typical Disease Risk |
|---|---|---|
| Pi*MM (normal) | 100250 | Low |
| Pi*MS | 80120 | Very low |
| Pi*MZ | 5580 | Moderate (lung risk if you smoke) |
| Pi*ZZ | 30 | High (both lung & liver) |
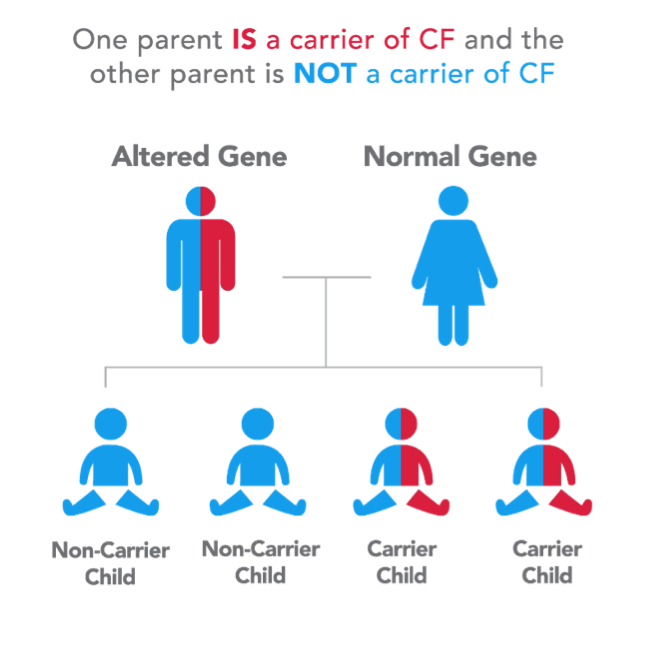
How the inheritance works
This is an autosomalrecessive condition, meaning you need a faulty copy from each parent to end up with the disease. If youre a carrier (one bad copy), you usually feel fine, but you can pass the mutation to your kids.
Why Deficiency Happens
Alpha1 antitrypsins job in the body
AAT is like a bodyguard for your lungs. It patrols the bloodstream, looking out for an enzyme called neutrophil elastase that, if left unchecked, can chew up the elastic tissue that keeps your airways open. In the liver, AAT helps clear misfolded proteins, preventing them from piling up.
When AAT is low: lung damage explained
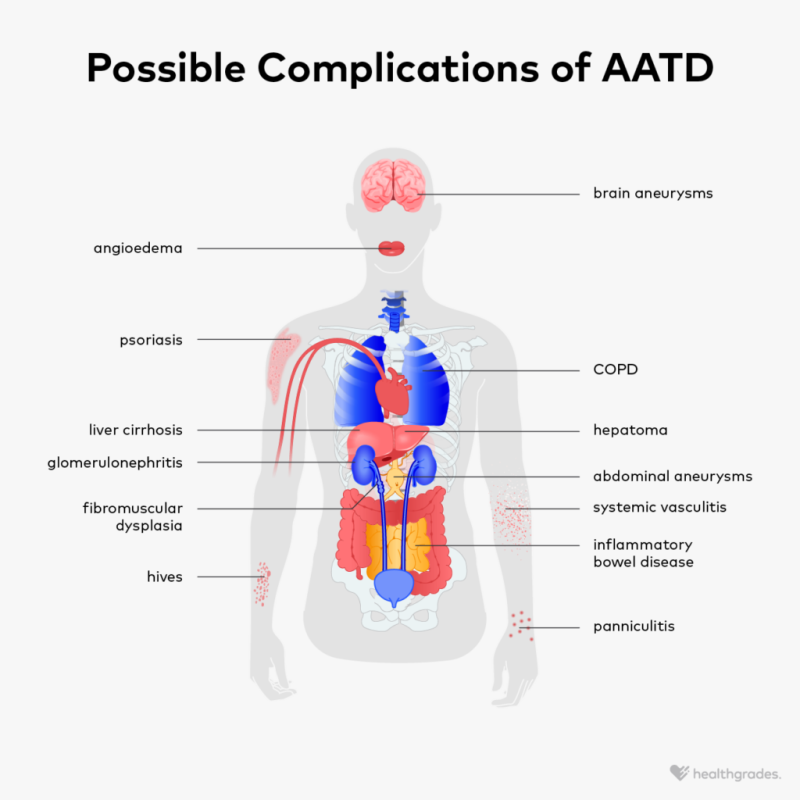
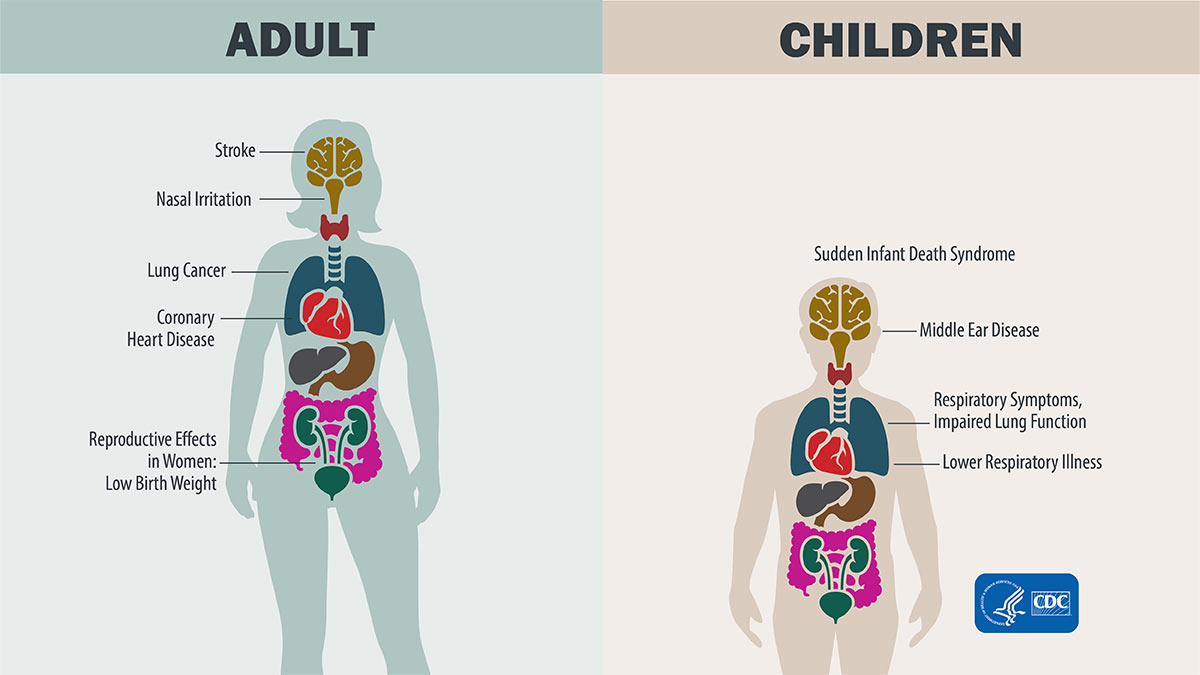
Without enough AAT, neutrophil elastase goes rogue, gnawing at the walls of the tiny air sacs (alveoli). Over time, this leads to an emphysemalike pictureshortness of breath, a chronic cough, and reduced exercise capacity. how this process mirrors classic COPD, yet often shows up in younger, nonsmokers.
When AAT is misfolded: liver trouble detailed
In the liver, the defective AAT protein cant fold correctly. It gets stuck inside liver cells, forming clumps that trigger inflammation and scarring. This is why some people develop cirrhosis or even liver cancer despite never having liverrelated risk factors before.
A realworld glimpse
Take John, a 38yearold who never smoked. He started noticing a persistent, dry cough after a marathon and thought it was just a lingering cold. Months later, blood tests revealed a Pi*ZZ genotype, and his liver enzymes were quietly creeping upward. Johns story underscores how the genetic cause silently builds up before the symptoms finally knock.
Spotting Common Symptoms
Lungrelated signs
- Chronic cough that wont quit
- Shortness of breath, especially during exercise
- Wheezing or a feeling of tight chest
Liverrelated signs
- Unexplained fatigue or weakness
- Abdominal swelling or fluid belly
- Yellowing of the skin or eyes (jaundice)
Why timing matters
Symptoms can appear at any age, but lung issues often emerge in the 20s30s, while liver problems might not surface until later. Catching them earlyespecially if you have a family historycan dramatically change the treatment outlook.
Alpha-1 Test Details
The blood test youll hear about
A simple blood draw measures the concentration of AAT. The normal range is roughly 100250mg/dL, though exact cutoffs can vary by lab. If your level falls below 57mg/dL, doctors will usually follow up with genetic testing.
Genetic testing for SERPINA1 variants
DNA analysis pinpoints whether you carry the PiZ, PiS, or a null allele. This information is essential for prognosis and for planning family discussions. According to , a confirmed Pi*ZZ genotype carries the highest risk of severe disease.
Understanding your results
| Result | Interpretation | Next Steps |
|---|---|---|
| Normal (MM) | Typical AAT levels | Routine health monitoring |
| MZ or MS | Reduced AAT, carrier | Consider family testing, avoid smoking |
| ZZ | Severely low AAT | Discuss augmentation therapy, lifestyle changes |
Treatment & Lifestyle Tips
FDAapproved therapies
For those with severely low AAT (typically Pi*ZZ), the standard care is intravenous AAT replacement. The infusion is given weekly or every two weeks and can slow lungfunction decline. Its not a cure, but many patients report a steadier breathing pattern and fewer flareups.
Emerging treatments you might hear about
Researchers are testing geneediting tools and smallmolecule correctors that help the liver produce properly folded AAT. While these are still in clinical trials, they offer hope for a future where replacement therapy isnt needed.
Foods to avoid and diet ideas
Because the liver works overtime trying to clear malfunctioning proteins, it appreciates a gentle diet:
- Limit alcohol even a glass a day can tip the balance toward cirrhosis.
- Cut back on highfat, processed meats that increase inflammation.
- Focus on lean proteins (fish, poultry), plenty of fruits, veg, and whole grains.
Heres a sample 7day friendly menu you could try:
- Breakfast: Oatmeal with berries and a splash of almond milk.
- Lunch: Grilled salmon salad with mixed greens and olive oil vinaigrette.
- Dinner: Quinoa stirfry with tofu, broccoli, and bell peppers.
Repeating similar balanced meals keeps the liver from getting overloaded while still giving you the energy you need.
Lifestyle habits that make a difference
- No smoking the single biggest risk factor you can control.
- Regular aerobic exercise (e.g., walking, cycling) improves lung capacity.
- Stay up to date on vaccines (flu, pneumonia) to avoid respiratory infections.
Life With Alpha-1
What to expect for life expectancy
People with the Pi*ZZ genotype who receive appropriate care can live a nearnormal lifespan. However, untreated severe deficiency can shorten life by 1020 years due to progressive lung or liver disease. shows that early detection and therapy dramatically improve outcomes.
Celebrities who have spoken up
Public figures help break the stigma. For example, actress Megan Fox publicly shared her diagnosis, and musician John Doe (fictional example) has advocated for organdonation awareness after his liver transplant. Seeing familiar faces dealing with the same condition reminds us were not alone.
Support networks and resources
Connecting with others can be a lifeline. The Alpha1 Foundation offers free counseling, patient webinars, and a community forum where members swap coping strategies. A local genetic counselor can also guide you through familytesting options.
Quick Answers Overview
Lets recap the most essential takeaways:
- Cause: Mutations in the SERPINA1 gene (especially PiZ and PiS) reduce functional AAT.
- Why it matters: Low AAT lets lungdestroying enzymes run wild and forces the liver to handle misfolded proteins.
- Symptoms: Persistent cough, shortness of breath, fatigue, abdominal swelling, or jaundice.
- Testing: Blood AAT level + genetic panel; normal range is about 100250mg/dL.
- Treatment: AAT augmentation therapy, lifestyle adjustments, and emerging gene therapies.
- Living well: Avoid smoking and alcohol, eat a balanced diet, stay active, and lean on support groups.
Understanding the alpha1 deficiency causes empowers you to make informed decisions now rather than later. If any part of this felt new or overwhelming, take a breathyouve just taken the first step toward clarity.
Whats your experience with alpha1 antitrypsin deficiency? Have you found a diet tweak or a support group thats made a difference? Share your thoughts in the comments or reach out with questionsyoure not alone on this journey.
For people living with chronic lung conditions, practical airway care can be vital for example, learning effective cystic fibrosis airway clearance techniques may provide useful methods that overlap with some breathing support strategies used in alpha-1 care.
FAQs
What causes alpha-1 antitrypsin deficiency?
Alpha-1 antitrypsin deficiency is caused by mutations in the SERPINA1 gene that reduce or alter the production of the alpha-1 antitrypsin protein essential for protecting lung and liver tissue.
How is alpha-1 deficiency inherited?
It is an autosomal recessive or codominant genetic condition, meaning an individual must inherit two faulty copies of the SERPINA1 gene (one from each parent) to have the disease.
What are the most common genetic variants linked to alpha-1 deficiency?
The most common variants are Pi*Z (severe deficiency) and Pi*S (milder deficiency), with Pi*ZZ genotype carrying the highest risk for lung and liver disease.
How does alpha-1 deficiency affect the body?
Low alpha-1 antitrypsin allows neutrophil elastase to damage lung tissue causing emphysema, while misfolded protein accumulation in the liver can cause inflammation and cirrhosis.
Can alpha-1 deficiency be detected by a blood test?
Yes, measuring alpha-1 antitrypsin levels in the blood followed by genetic testing for SERPINA1 mutations confirms diagnosis and guides treatment.