Short answer: yesCOVID19 can make your heartbeat race, slow down, or feel irregular, both while youre sick and weeks after the virus seems to have left your lungs.
Why does it matter? A sudden jump to a heart rate of 120bpm, unexpected palpitations, or a dangerously low pulse can signal inflammation, dehydration, or lingering heart damage that deserves attention before it turns into something more serious.
How COVID Impacts Heart
How the virus stresses the cardiovascular system
When the virus invades, it doesnt just settle in your lungs. It triggers a cascade of immune responses that can tug at the hearts wiring. Fever alone can push your heart rate upsometimes past 100bpm, even hitting 120bpm during a high fever. Thats a normal, temporary reaction, but its worth knowing why it happens.
Feverdriven tachycardia
Every degree Celsius your temperature climbs can raise your resting heart rate by about 10bpm. So a modest fever of 38C (100.4F) might nudge a typical 70bpm resting rate up to 80 or 90bpm. In severe cases, especially if youre battling a high fever, hitting 120bpm isnt uncommon.
Inflammatory response and myocarditis
Beyond fever, the immune system can cause inflammation of the heart musclemyocarditis. This condition can make the heart beat irregularly or feel fluttery. Research from shows that a small percentage of people with longCOVID experience myocarditis, which can linger for months.
Common heartrelated symptoms after COVID
People frequently report palpitations (that racing heart sensation), a steady high resting heart rate, or the oppositean unusually slow pulse. One friend of mine, after a mild bout of COVID, woke up at night with an unmistakable whoosh feeling in his chest. He thought it was anxiety at first, but a quick check with his smartwatch showed his heart hovering around 115bpm while he lay still. He later learned that postCOVID palpitations can be a sign of autonomic nervous system disruption.
How Common Are Heart Changes
Statistics & prevalence
Current data from the suggest that roughly 1015% of longCOVID sufferers notice a change in their resting heart rate. A large smartwatch study published in JAMA Network Open found that participants who had recovered from COVID were 25% more likely to experience a sustained increase of 5bpm or more compared to preinfection baselines.
Incidence of myocarditis & palpitations
While severe myocarditis remains rareless than 1% of infectionsmilder forms that produce palpitations or a modest tachycardia are far more frequent. The Lancet reports that among hospitalized patients, about 7% develop clinically significant heart rhythm disturbances.
Who is most at risk?
- Older adults (60+)
- People with preexisting cardiovascular disease
- Those who experienced severe COVID symptoms (hospitalization, oxygen support)
- Individuals who are physically inactive during recovery
Quick selfcheck: Is your heart rate normal?
| Resting HR | Typical Meaning |
|---|---|
| < 60bpm | Possible bradycardiawatch for dizziness or fainting. |
| 60100bpm | Normal range for most adults. |
| > 100bpm | Elevated; could be fever, dehydration, or postCOVID tachycardia. |
Red Flags vs Normal
Sudden increase in resting heart rate
If your resting heart rate shoots up to 120bpm without an obvious cause (like fever or exercise), treat it as a red flag. Especially if you feel lightheaded, short of breath, or notice chest discomfort.
When to worry
- HR>120bpm at rest for more than 24hours
- Palpitations that last longer than a few minutes
- Chest pain, pressure, or tightness
- New onset shortness of breath that doesnt improve with rest
Comparison: Feverrelated vs Pathological Tachycardia
| Feature | Feverrelated | Pathological |
|---|---|---|
| Onset | During fever spikes | Any time, often at rest |
| Duration | Resolves as fever drops | Persists >24hrs |
| Accompanying symptoms | Chills, sweating | Chest pain, dizziness |
Dangerously low heart rate (bradycardia)
While most of us worry about a racing pulse, a heart rate that dips below 50bpmespecially if you feel weak, faint, or confusedcan be just as concerning. COVIDrelated autonomic dysfunction can sometimes push the heart into a slowed rhythm, which may require a pacemaker in extreme cases.
Symptoms of low HR
- Unexplained fatigue
- Lightheadedness or fainting spells
- Shortness of breath with minimal activity
- Chest discomfort
When to seek medical help
Call your doctor or head to urgent care if you notice any of the redflag symptoms above. If youre unsure, a quick telehealth consult can help decide whether an inperson ECG or a Holter monitor is needed.
Recovering Heart Health
Lifestyle habits that support a healthy heart rate
Give your heart a gentle reboot. Think of it like easing back into a favorite song after a breakslow tempo at first, then gradually picking up the beat.
Gradual aerobic reconditioning
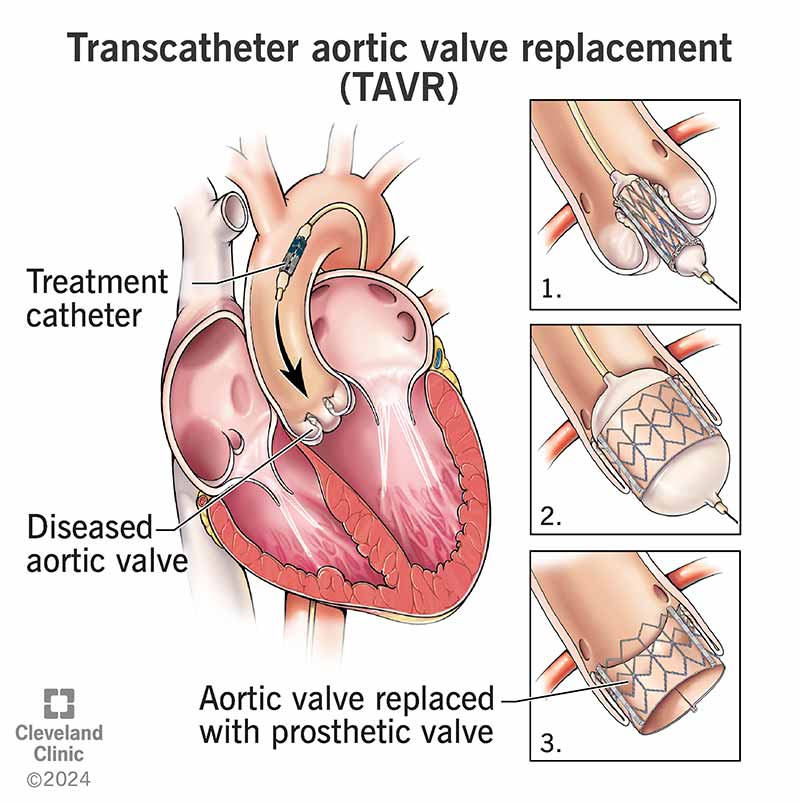
Start with 10minute walks, three times a week. Once youre comfortable, add short intervals of light jogging or cycling. The goal is to increase your hearts efficiency without overtaxing it. For people recovering from significant valve procedures, guidance on heart valve recovery can help shape a safe activity plan.
Hydration & electrolytes
Dehydration can raise heart rate, so keep a water bottle handy. Consuming potassiumrich foodsbananas, avocados, leafy greenshelps maintain a stable rhythm.
How to improve heart health after COVID
Nutrition tips
Omega3 fatty acids found in salmon, walnuts, and flaxseed support cardiac tissue repair. Pair them with antioxidantrich berries to combat lingering inflammation.
Stressreduction techniques
Stress triggers the fightorflight hormone adrenaline, which can spike your pulse. Simple breathing exercisesinhale for four counts, hold for four, exhale for sixcan calm the nervous system. Even a 5minute mindfulness session each morning makes a difference.
Medical tools and monitoring
Wearable tech for tracking trends
Smartwatches and fitness bands can show nightly resting heart rate trends. A study from found that continuous monitoring helped identify postCOVID tachycardia earlier than routine checkups.
Advanced testing when needed
If symptoms linger, doctors may recommend a cardiac MRI or a 24hour Holter monitor. These tools can spot subtle inflammation or irregular beats that a quick office ECG might miss. If swelling or fluid retention accompanies heart symptoms, consider reading about heart failure edema and treatment approaches.
Putting It All Together
COVID can certainly shake up your heart rhythm, but most changes are manageable with awareness, selfmonitoring, and a few lifestyle tweaks. Recognize the warning signslike a steady 120bpm resting rate, persistent palpitations, or a pulse that drops below 50bpmand act promptly. At the same time, give your heart room to heal: stay hydrated, move gently, fuel it with heartfriendly foods, and keep stress in check.
If anything in this article resonates with you, or if youve experienced postCOVID heart palpitations yourself, Id love to hear your story in the comments. Sharing helps us all feel less alone on this recovery journey. And rememberwhen in doubt, reach out to a healthcare professional. Your heart deserves the best care, and you deserve peace of mind.
FAQs
Can COVID really change your heart rate?
Yes, COVID-19 can cause your heart rate to increase, decrease, or become irregular, both during the infection and weeks after recovering[1][2][6].
Why does COVID make your heart race?
Fever and inflammation from COVID-19 can raise your heart rate. In some cases, the infection may directly inflame the heart muscle or disrupt normal heart rhythm[1][2][3].
Are heart palpitations after COVID common?
Heart palpitations and changes in resting heart rate are among the more common cardiovascular symptoms reported after COVID-19, especially in those with long COVID[2][3][5].
Who is most at risk for COVID-related heart issues?
People over 60, those with pre-existing heart conditions, and individuals who had severe COVID symptoms are at higher risk for post-COVID heart rate changes and complications[2][3].
When should I be concerned about my heart rate after COVID?
Seek medical attention if you have a resting heart rate consistently above 120 bpm, below 50 bpm, persistent palpitations, chest pain, dizziness, or new-onset shortness of breath[1][6].