Hey there, friend. If youve just had a knee replacement and feel that strange, electric tingle or burning behind your knee, youre not alone. It can feel like the surgery fixed the joint but left a new, unwanted guest called nerve pain. The good news? There are realworld strategies that actually worksome you can start today, and others you can explore if the pain sticks around.
In this post well walk through why nerve pain happens after a total knee replacement, what the most common symptoms are, andmost importantlywhat helps nerve pain after knee replacement. Ill share the kind of advice Ive heard from surgeons, physical therapists, and patients whove been exactly where you are now. Lets dive in and get you on the road to relief.
Understanding Nerve Pain
Why does nerve pain occur after a total knee replacement?
During knee replacement surgeons cut through skin, muscle, and sometimes even a bit of cartilage to fit the new implant. That journey can irritate or even stretch the surrounding nervesmost often the sciatic, femoral, or peroneal nerves. Inflammation, scar tissue, or a little pressure from the prosthetic can also trigger neuropathic sensations, which feel different from the dull ache of regular postop soreness.
How common is nerve damage after knee replacement?
Studies suggest that about 15% of patients experience some form of nerve irritation after the surgery. While that sounds low, consider the millions of knee replacements performed each yearthose percentages translate to thousands of people dealing with tingling, burning, or numbness.
Typical symptoms and timeline
Watch for these red flags:
- Tingling or pinsandneedles in the calf, shin, or foot.
- Sharp, electricshock pain that may flare when you bend or straighten the knee.
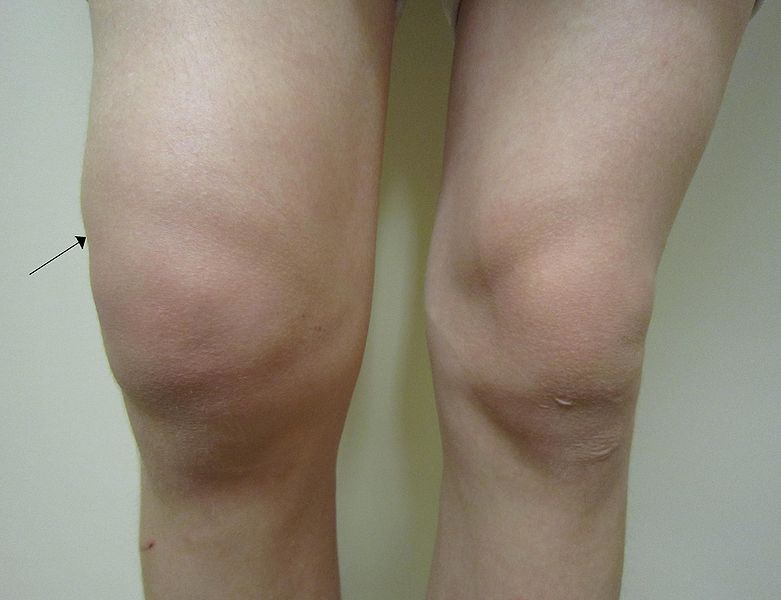
- Numbness or reduced sensation especially around the knee cap or down the leg.
- Foot neuropathya feeling of asleep in the foot that can linger weeks or months later.
The symptoms can surface right after surgery, pop up around six months later, or become a chronic issue lasting a year or more. Knowing when they appear helps you and your care team choose the right treatment.
FirstLine Relief
Physical therapy & movementbased therapies
Getting movingstrategicallyis one of the most effective ways to calm irritated nerves. A good PT program does three things:
- Boosts circulation to clear inflammation.
- Strengthens supporting muscles (quadriceps, hip abductors) so the joint isnt overworking the nerves.
- Reeducates gait to prevent abnormal pressure on the sciatic or femoral nerves.
Sample PT routine (3day/week)
| Day | Exercise | Reps / Sets |
|---|---|---|
| Monday | Stationary bike, low resistance | 10min steady |
| Monday | Quad sets (tighten thigh muscle) | 315sec hold |
| Wednesday | Sidelying hip abduction | 212 each side |
| Wednesday | Gentle hamstring stretch | 320sec |
| Friday | Balance board (light) | 230sec |
| Friday | Walking on level surface | 15min, easy pace |
Medications that target neuropathic pain
If the nerves are firing off in overdrive, a doctor may prescribe meds that calm that electrical storm:
- Gabapentin (Neurontin) or Pretabalin (Lyrica)often the first line for postsurgical nerve pain.
- Topical agents like capsaisin patches, which gently desensitize the skin over weeks. that a 3month course can cut burning sensations by half.
- NSAIDs or acetaminophen for the inflammatory backdropthese wont fix nerve pain alone but can make other treatments more tolerable.
Dosing basics & safety
Older adults often start low (e.g., gabapentin 300mg at night) and titrate up to avoid dizziness. Always discuss kidney function with your doctorsome meds need dose adjustments.
Adjunctive modalities
Beyond meds and PT, you might try:
- Transcutaneous Electrical Nerve Stimulation (TENS)tiny electrical pulses that confuse pain signals. A 2022 study found a 30% reduction in neuropathic scores when used 20minutes twice daily.according to a recent study.
- Heat & ice therapyalternate a warm pack (10min) with a cold compress (10min) to modulate blood flow.
- Massage or myofascial releasegentle pressure can loosen scar tissue that might be pinching a nerve.
MidTerm Solutions
Advanced therapies for persistent pain (3months)
If youve stuck with PT, meds, and TENS for a few months and the tingling still wont quit, consider these options:
- Peripheral Nerve Stimulation (PNS)tiny electrodes placed near the affected nerve deliver mild pulses. Patients report up to 70% relief within weeks.
- PlateletRich Plasma (PRP) injectionsconcentrated platelets release antiinflammatory growth factors that may soothe irritated nerves.
- Targeted corticosteroid injections around scar tissueuseful when inflammation is the main driver.
Conservative vs. Interventional vs. Surgical (Comparison Table)
| Approach | Typical Cost | Recovery Time | Success Rate |
|---|---|---|---|
| Physical therapy & meds | Low | Weeksmonths | 6070% |
| Peripheral Nerve Stimulation | MediumHigh | Sameday implant | 7080% |
| Revision surgery (rare) | High | Months | 5060% (if caused by implant) |
Lifestyle & selfmanagement tips
Even the most hightech treatments work better when you support them with daily habits:
- Maintain a healthy weightextra pounds increase pressure on the knee and nerves.
- Lowimpact cardio like swimming or elliptical keeps blood flowing without hammering the joint.
- Nutrition for nervesomega3 fatty acids, vitaminB12, and magnesium help nerve repair.
- Footwear & orthoticsa good supportive shoe can prevent foot neuropathy from worsening.
When to seek specialist care
If you notice any of these, call your surgeon or a pain specialist right away:
- Sudden worsening pain or new weakness.
- Signs of infection (redness, fever, drainage).
- Pain that doesnt improve after 3months of conservative care.
- Persistent numbness that interferes with walking.
Early referral means youll have more treatment options and a better chance of full recovery.
Balancing Benefits & Risks
Pros & cons of each treatment modality
Heres a quick reality check:
- Physical therapy High benefit, almost no risk, but requires commitment.
- Neuropathic meds Effective for many, yet can cause drowsiness, dizziness, or stomach upset.
- Interventional procedures Powerful relief, but involve needles, possible infection, and higher cost.
Shared decisionmaking checklist
Before you choose a path, ask yourself:
- How severe is the pain on a 010 scale?
- Do I have other health conditions (diabetes, kidney issues) that affect medication safety?
- What outcome matters most to mepain relief, quick return to activity, or avoiding surgery?
Bring these answers to your next appointment; clinicians love a wellprepared patient.
Resources & Further Reading
For deep dives and evidencebased guidelines, check out these trusted sources (theyre all free to read):
Conclusion
Living with nerve pain after a knee replacement can feel like an unwelcome sideeffect, but you have tools to tame it. Start with gentle movement, partner with a knowledgeable PT, and consider neuropathic meds or topical patches if the tingling persists. If months go by without improvement, discuss advanced options like peripheral nerve stimulation with your surgeon. Remember, every step you takewhether its a short walk, a balanced meal, or a quick chat with your doctoradds up to a smoother, less painful journey back to the life you love.
Whats worked for you? Have you tried a TENS unit, a specific stretch, or a medication that finally gave you relief? Share your experience in the conversation below, and lets help each other heal.