Why Deficiencies Occur
Inflammation is the villain in this story. When the colons lining is inflamed, it cant absorb nutrients the way it used to. A study in shows that patients with active UC lose up to 30% of their ironabsorbing capacity. Add to that the fact that many common UC medicationsespecially steroids and 5ASA drugscan interfere with vitaminD metabolism, and you have a perfect storm of deficiencies.
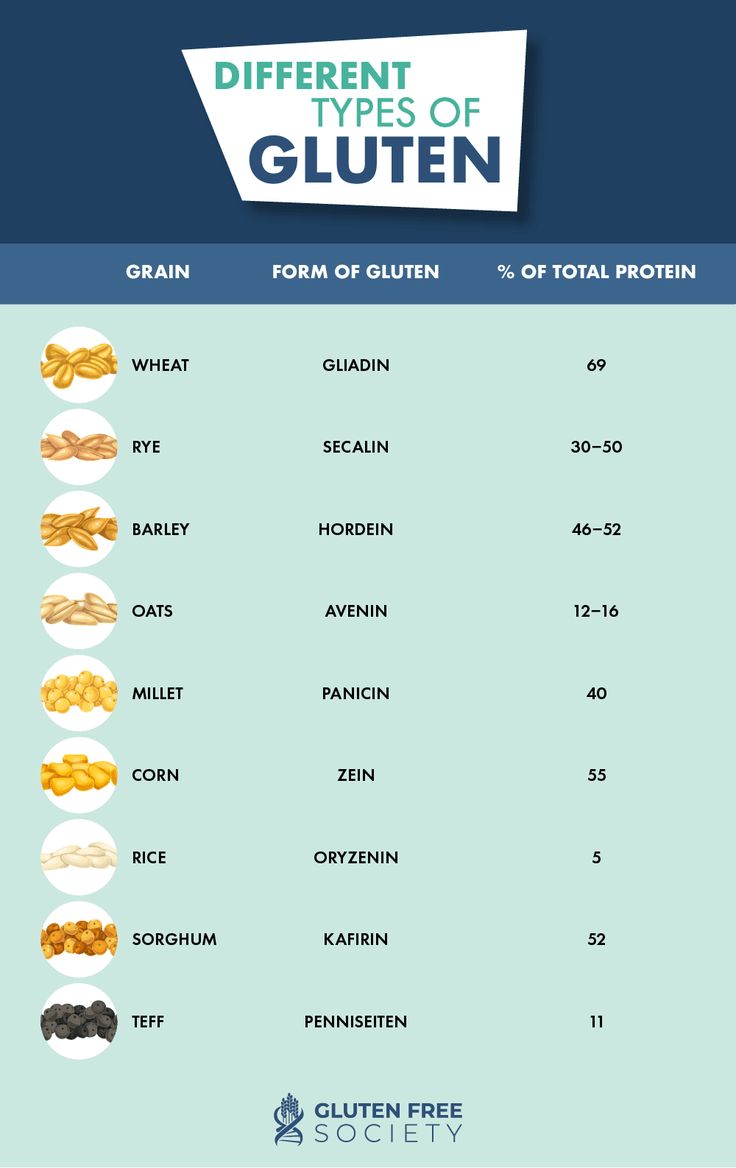
And then theres the food fear factor. When youre constantly worrying about triggering a flare, you might avoid dairy, gluten, or highfiber foods. While this can keep symptoms in check, it also means youre missing out on calcium, vitaminD, and even natural iron sources.
In short, its a triple whammy: inflamed gut, medication sideeffects, and restrictive eating habits. Knowing this helps you understand why a simple blood test can reveal a whole cascade of missing nutrients.
Inflammation vs. Absorption
| Nutrient | How Inflammation Affects It |
|---|---|
| Iron | Reduced duodenal uptake; chronic blood loss from lesions |
| VitaminD | Impaired conversion in the liver; higher catabolism |
| VitaminB12 | Damage to ileum where B12 is absorbed |
| Calcium | Less dietary intake; decreased active transport |
| Zinc | Increased urinary loss during flares |
Common Deficiencies Signs
Spotting the signs early can save you a lot of frustration. Here are the most frequent culprits and what they feel like.
Iron Deficiency
Fatigue that wont quit, pale skin, and brittle nails are classic irondeficiency signals. According to the , more than half of UC patients experience low ferritin levels at some point.
VitaminD Deficiency
Think bone pain, mood swings, and a higher risk of flareups. If youve been asking how much vitamin d to take for ulcerative colitis, youre not alone. Most experts suggest 1,0002,000IU daily, but blood levels should guide the exact dose.
VitaminB12 Deficiency
Numbness in hands or feet, trouble concentrating, and that foggy feeling? B12 deficiency can sneak up on you, especially if the terminal ileum has been damaged.
Calcium & Magnesium Shortfalls
Joint aches, occasional cramping, and a subtle sense of shakiness point to low calcium or magnesium. Both are essential for bone healthsomething UC patients need to watch closely.
Zinc & Selenium Deficits
Weak immunity, slower wound healing, and a lingering sense of being off can stem from low zinc or selenium. These minerals help your gut repair itself after a flare.
Quick RedFlag Checklist
- Unexplained fatigue or shortness of breath
- Persistent bone or joint pain
- Numbness, tingling, or memory lapses
- Frequent infections or slow healing
- Hair loss or brittle nails
Testing & Diagnosis
The best way to know what youre missing is to ask for the right labs. Dont settle for a generic CBC. Talk to your gastroenterologist and request a targeted panel.
Blood Panels You Should Request
- CBC with ferritin and transferrin saturation (iron status)
- 25OHVitaminD level
- Serum vitaminB12 and folate
- Zinc and selenium levels (often sent to a specialty lab)
- Calcium, magnesium, and albumin
Stool Tests for Malabsorption
If youre in a flare, a stool calprotectin test can confirm inflammation, while a fecal fat test can hint at broader malabsorption issues.
When to Test
- At diagnosis baseline snapshot
- During a flare to see whats dropping
- After remission to ensure youve rereplenished
Sample Lab Report (Illustrative)
| Marker | Normal Range | Your Result | Interpretation |
|---|---|---|---|
| Ferritin | 30400ng/mL | 12ng/mL | Iron deficiency |
| 25OHD | 30100ng/mL | 18ng/mL | Deficient |
| B12 | 200900pg/mL | 150pg/mL | Low |
| Zinc | 70120g/dL | 55g/dL | Low |
Safe Supplement Strategies
Supplementation isnt a onesizefitsall game. The mantra is start low, go slow. Heres a roadmap for the most common nutrients.
VitaminD Dosage
Most clinicians start you at 1,000IU daily and recheck levels after 8 weeks. If youre severely deficient, you might need 2,0004,000IU, but only under supervision. Remember, vitaminD is fatsolubletake it with a meal that contains healthy fats.
Iron Supplement Options
Ferrous gluconate is gentler on the gut than ferrous sulfate, but it delivers less elemental iron. For those with active inflammation, a chelated form like ferrous bisglycinate can be easier to tolerate.
Best Iron Supplement for Ulcerative Colitis
| Product | Form | Elemental Iron | GI Tolerance | Price (per month) |
|---|---|---|---|---|
| Ferrous Gluconate | Salt | 35mg | Moderate | $$ |
| Ferrous Bisglycinate | Chelate | 28mg | High | $$$ |
| Carbonyl Iron | Particles | 45mg | Low | $ |
B12 Delivery
If your ileum is scarred, oral cyanocobalamin may not absorb well. Sublingual tablets or monthly injections (often covered by insurance) are reliable alternatives.
Calcium + VitaminD Combo
Aim for 1,200mg of calcium split into two doses (breakfast and dinner) and pair it with your vitaminD pill. Avoid calcium carbonate on an empty stomachit can cause bloating.
General Safety Checklist
- Check for highdose vitaminA or K if youre on blood thinners.
- Avoid iron and calcium together; they compete for absorption.
- Start with half the suggested dose, monitor tolerance, then increase gradually.
Best Multivitamins for UC
Finding a multivitamin that respects a sensitive gut is like hunting for a unicornbut there are a few that actually deliver.
What to Look For
- Gentle, highly bioavailable forms (e.g., methylfolate, methylcobalamin)
- Low filler content no artificial colors or excessive magnesium oxide
- Added zinc, selenium, and a modest iron dose (if youre irondeficient)
- Thirdparty testing (USP, NSF)
Top Picks
| Brand | Key Nutrients | Special Feature | Price |
|---|---|---|---|
| Garden of Life MyKind Organics | VitaminD3, B12, Iron (as bisglycinate) | Certified organic, glutenfree | $$$ |
| Thorne Research Basic Nutrients 2/Day | VitaminD3 2,000IU, Zinc, Selenium | Hypoallergenic, no unnecessary fillers | $$ |
| Pure Encapsulations O.N.E. Multivitamin | VitaminD3 2,500IU, Bcomplex, Iron (as carbonyl) | Ideal for sensitive stomachs | $$$ |
Best Multivitamin for Women with Ulcerative Colitis
Women often need extra iron and calcium, especially if theyre premenopausal. The Pure Encapsulations O.N.E. formula includes 18mg of iron and 500mg of calcium, making it a solid choice.
Best Multivitamin for Someone with Ulcerative Colitis
Thornes Basic Nutrients 2/Day offers a balance of highabsorption Bcomplex, vitaminD, and zinc without overloading on ironperfect if you already supplement iron separately.
Best Multivitamin for IBD (General)
The Garden of Life MyKind Organics line is praised by gastroenterologists for its clean label and inclusion of wholefood derived nutrients.
Best Multivitamins for Crohns Disease
While Crohns and UC share many nutrient challenges, Crohns patients often need higher B12. recommends a B12rich formula like Metagenics Active One. The principles, however, are identical.
Can I Take Multivitamins with Ulcerative Colitis?
Yesjust choose a product that avoids excessive iron or vitaminA, and always check with your doctor if youre on steroids or immunosuppressants.
Supplements to Avoid
Not everything marketed as gutfriendly is safe for UC. Here are the red flags.
HighDose Calcium & VitaminK
If youre on blood thinners (e.g., warfarin), massive calcium or vitaminK doses can interfere with clotting.
Heavy Prebiotic Fiber Blends
While probiotics can be helpful, adding large amounts of inulin or chicory root can cause gas and bloating during flareups.
Herbal Extracts That Interact with Meds
St.Johns wort, ginkgo, and some turmeric extracts can affect the metabolism of mesalamine or biologics. Stick to clinically tested options.
NoGo Quick List
- VitaminA megadoses (>10,000IU)
- Certain calcium carbonate powders without magnesium
- Prebiotic blends >5g per serving
- Herbal blends with unknown drug interactions
Practical Nutrition Tips
Supplements are only part of the puzzle. Your everyday meals can bridge many gaps naturally.
Boost Iron Without the GI Upset
Try cooked spinach, lentils, and lean turkey. Pair them with vitaminCrich foods (bell peppers, citrus) to improve absorption.
VitaminD From Food + Sun
Fatty fish (salmon, mackerel), fortified plant milks, and egg yolks are good sources. A short 1015minute walk in the sun (if safe for your skin) can add a natural boost.
Gentle B12 Sources
Clams, lowfat Greek yogurt, and fortified cereals are easy on the gut. If you avoid animal products, fortified nutritional yeast is a tasty alternative.
CalciumRich Snacks
Almond butter on wholegrain toast, a small cheese stick, or a cup of fortified soy milk can keep calcium levels steady without dairy overload.
MealTiming Trick
Take fatsoluble vitamins (D, E, A, K) with your largest meal of the dayusually dinnerto maximize absorption.
Tracking Tools
Apps like MyFitnessPal or Cronometer let you log micronutrients day by day. Seeing a visual trend can motivate you to keep up with your supplement routine.
Sample 7Day Meal Plan (Key Nutrients Highlighted)
| Day | Breakfast | Lunch | Dinner | Key Micronutrients |
|---|---|---|---|---|
| Mon | Greek yogurt + berries + chia | Grilled chicken salad w/ spinach, orange slices | Salmon, quinoa, steamed broccoli | VitaminD, Iron, Calcium |
| Tue | Fortified oat milk smoothie (banana, spinach, protein powder) | Turkey sandwich on glutenfree bread + avocado | Beef stirfry with bell peppers, brown rice | Zinc, B12, VitaminC |
| Wed | Scrambled eggs + cheese + tomato | Lentil soup + side kale salad | Cod, sweet potato, green beans | Iron, VitaminD, Selenium |
| Thu | Almond butter toast + apple | Quinoa bowl w/ chickpeas, cucumber, feta | Chicken curry (coconut milk) + cauliflower rice | Calcium, Magnesium, VitaminD |
| Fri | Fortified cereal + soy milk | Grilled shrimp salad w/ mixed greens | Lean pork loin, roasted carrots, peas | VitaminB12, Iron, Zinc |
| Sat | Protein pancakes (whole wheat) + maple syrup | Veggie wrap (glutenfree tortilla) + hummus | Turkey meatballs, tomato sauce, zucchini noodles | Calcium, VitaminD, VitaminC |
| Sun | Smoothie bowl (acai, berries, almond butter) | Salmon sushi bowl (brown rice, avocado) | Roast chicken, parsnips, spinach | Omega3, Iron, VitaminD |
When to Seek Help
Supplements are powerful, but theyre not a substitute for professional guidance. Here are the red flags that mean its time to pick up the phone.
Symptoms That Require a Doctors Visit
- Persistent fatigue despite iron supplements
- Bone pain or frequent fractures
- Neurological symptoms (numbness, tingling)
- Unexplained weight loss or severe swelling
- Any new medication interaction concerns
Working with the Right Team
Ideally, youll have a gastroenterologist who understands nutrientloss patterns, plus a registered dietitian (RD) who can finetune your food and supplement plan. The RD can also suggest lowFODMAP or specific elimination diets that preserve nutrient intake.
Preparing for Your Appointment
- Bring a copy of your recent lab results
- List all supplements (including overthecounter vitamins)
- Write down questionse.g., How much vitamin d should I take for ulcerative colitis? or Can I take multivitamins with ulcerative colitis?
Being organized shows your provider that youre proactive and helps them give you the most accurate advice.
Conclusion
Living with ulcerative colitis can feel like walking a tightropeone misstep and nutrients slip away. By understanding why deficiencies happen, getting the right labs, and choosing smart, gutfriendly supplements, you can keep iron, vitaminD, B12, calcium, and zinc where they belong: supporting your body, not triggering another flare. Remember to pair supplements with a balanced, nutrientdense diet, and never hesitate to bring your questions to a gastroenterologist or dietitian. Your gut may be sensitive, but with the right knowledge and a dash of patience, you can stay nourished, empowered, and ready for whatever comes next.
For recommendations on specific ulcerative colitis supplements and a practical supplement strategy tailored to UC, see this guide: ulcerative colitis supplements.
FAQs
What vitamins are commonly deficient in ulcerative colitis?
People with ulcerative colitis often have low levels of iron, vitamin D, vitamin B12, calcium, and zinc due to inflammation and dietary restrictions.
How does ulcerative colitis cause vitamin deficiency?
Ulcerative colitis leads to vitamin deficiency through poor nutrient absorption, chronic blood loss, medication effects, and dietary limitations.
Can vitamin deficiency worsen ulcerative colitis symptoms?
Yes, vitamin deficiencies can worsen symptoms like fatigue, anemia, bone pain, and slow healing, making it harder to manage ulcerative colitis.
How do I know if I have a vitamin deficiency with UC?
Blood tests for iron, vitamin D, B12, calcium, and zinc can identify deficiencies. Symptoms like fatigue, numbness, or bone pain may also signal a problem.
Should I take supplements for ulcerative colitis vitamin deficiency?
Supplements can help, but should be guided by a healthcare provider to avoid side effects and ensure proper dosing for your needs.