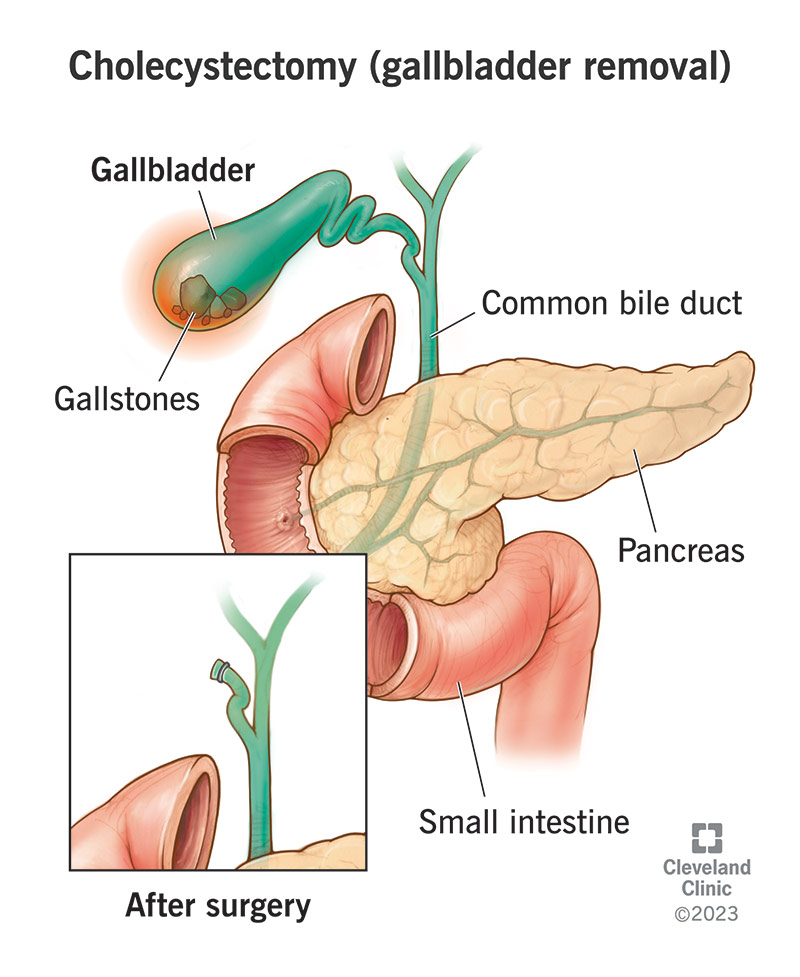
Most folks feel a huge relief once the gallbladder is out those painful attacks finally stop, and life feels back on track. But for a sizable slice of patients, the story doesnt end there. Up to 30% notice lingering digestive quirks, occasional rightside aches, or even subtle liver changes years after the surgery.
Understanding the balance between the good and the notsogood helps you stay on top of any symptoms, tweak your diet, and know exactly when a doctors visit is the right move. Lets walk through what you might experience, why it happens, and what you can do about it all in a friendly, downtoearth way.
Common LongTerm Symptoms
What Is PostCholecystectomy Syndrome?
Postcholecystectomy syndrome (PCS) is a blanket term for persistent symptoms after gallbladder removal. It can include bloating, gas, diarrhea, and a lingering intolerance to fatty foods. Studies suggest PCS affects roughly 1020% of patients, though the exact number varies by how strictly researchers define persistent.
Persistent RightSide Pain Two Years Later
Feeling a dull or sharp ache on the right side two years after the operation can feel baffling. Common culprits include:
- Residual bileduct stones that escaped detection.
- Sphincter of Oddi dysfunction the valve that controls bile flow can become overactive.
- Scar tissue (adhesions) irritating nearby nerves.
If the pain is new, severe, or accompanied by fever, its time to call your healthcare provider. Even a mild, ongoing ache deserves a checkup to rule out complications.
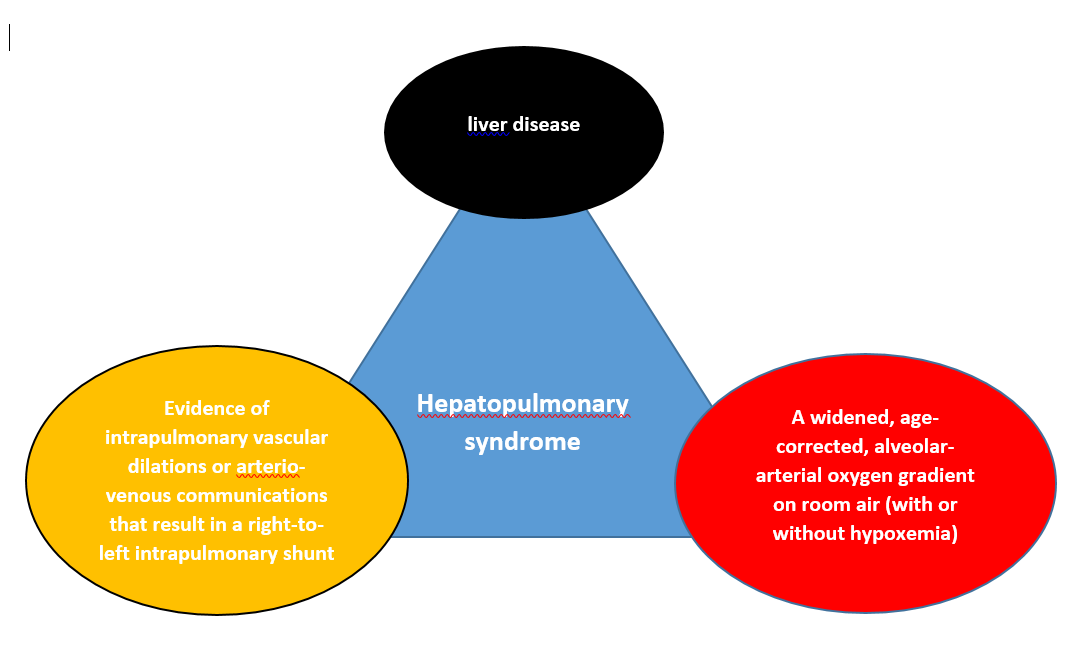
LiverRelated Problems After Gallbladder Removal
Although the liver itself isnt touched during a cholecystectomy, the way bile drains can shift, sometimes nudging liver enzymes upward. A overview notes that mild elevations in ALT or AST are observed in a minority of patients, usually without symptoms. However, persistent elevation or jaundice warrants deeper investigation.
How Often Do Liver Issues Appear?
Recent research published in Digestive Diseases and Sciences (2022) found that about 5% of patients showed a measurable rise in liver enzymes six months postsurgery, and only 12% continued to have abnormal results after one year. Most of those cases were linked to underlying metabolic conditions rather than the surgery itself.
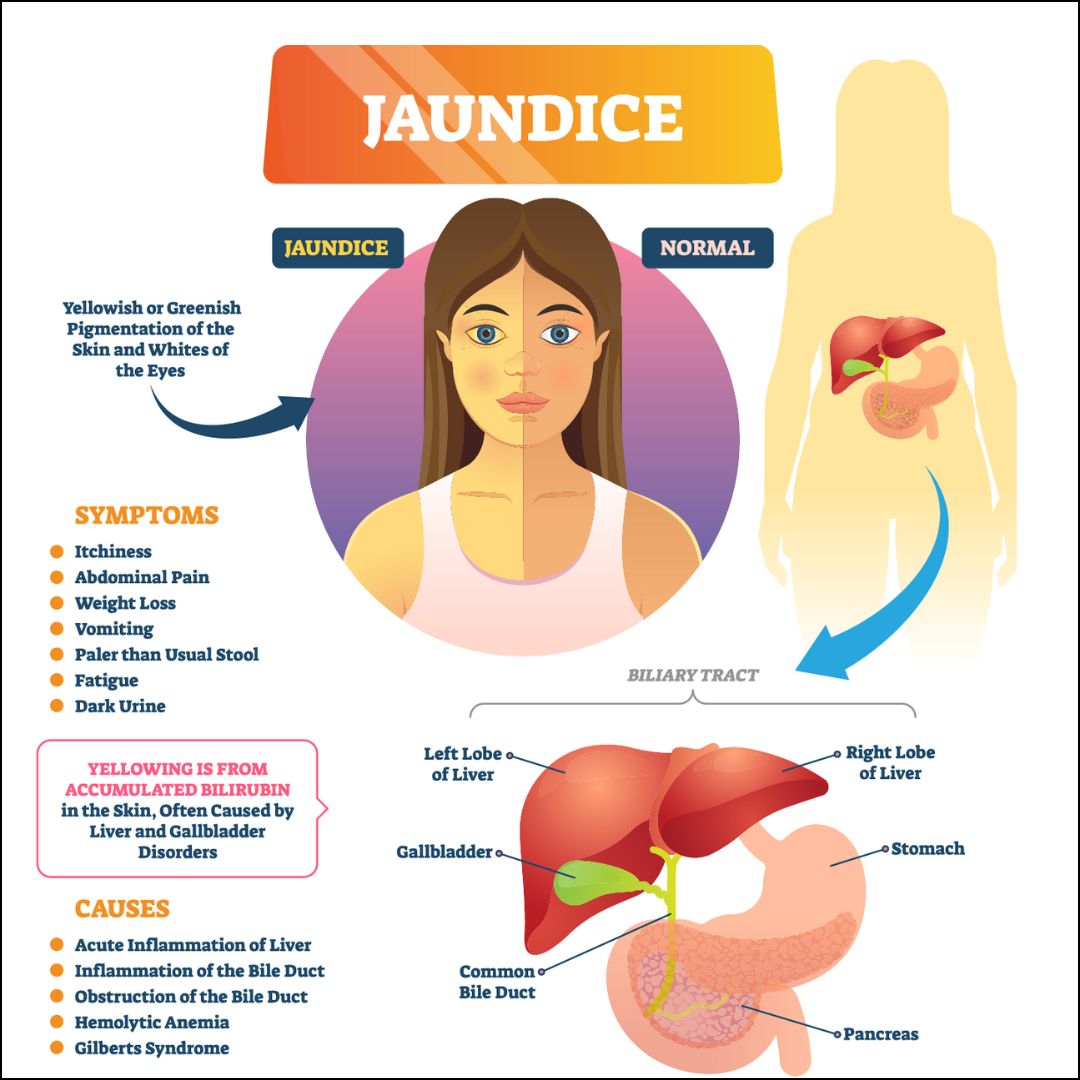
Red Flags to Watch For
Keep an eye on these warning signs:
- Yellowing of the skin or eyes (jaundice).
- Unexplained fatigue that doesnt improve with rest.
- Persistent abdominal pain that feels different from typical postop soreness.
- Abnormal lab results on routine blood work.
Diet and Recovery
GallbladderRemoval Diet Myths vs. Reality
Right after surgery, doctors often suggest a lowfat, bland diet to give the digestive system a chance to adjust. The myth is that you must stay lowfat forever. In reality, the body can handle moderate fat once the bile flow stabilizes, usually within a few weeks.
Foods That May Trigger Symptoms
Even years later, certain foods can stir up trouble:
- Fried foods (think french fries, onion rings).
- Heavy cream, butter, and fullfat cheeses.
- Spicy, heavily seasoned dishes that irritate the gut.
- Processed sugars and refined carbs that ferment and cause gas.
Sample 7Day Meal Plan
| Day | Breakfast | Lunch | Dinner |
|---|---|---|---|
| Mon | Oatmeal with berries & a splash of almond milk | Grilled chicken salad with olive oil vinaigrette | Baked salmon, quinoa, steamed broccoli |
| Tue | Smoothie (spinach, banana, Greek yogurt) | Turkey wrap with wholewheat tortilla | Stirfried tofu, brown rice, mixed veggies |
| Wed | Wholegrain toast, avocado, poached egg | Lentil soup, side of mixed greens | Lean pork tenderloin, sweet potato, green beans |
| Thu | Greek yogurt, honey, sliced almonds | Quinoa bowl with roasted veggies & chickpeas | Grilled shrimp, couscous, asparagus |
| Fri | Scrambled eggs with spinach | Chicken Caesar salad (light dressing) | Vegetable lasagna (lowfat cheese) |
| Sat | Fruit parfait with lowfat granola | Bean chili, side of cornbread | Grilled tilapia, wild rice, sauted kale |
| Sun | Protein pancakes, fresh fruit | Turkey chili, mixed salad | Roasted chicken, mashed cauliflower, carrots |
Probiotics & Fiber Do They Really Help?
Adding a daily probiotic and boosting soluble fiber can smooth out digestion for many people. A review in Clinical Nutrition (2021) found that a combination of and 2530g of fiber daily reduced bloating in 60% of participants who had undergone cholecystectomy. Think of fiber as the gentle brush that keeps things moving without a sudden rush of bile.
Whos Most at Risk
Female Gallbladder Surgery Recovery Time & LongTerm Effects
Women often report a slightly longer recovery period, partly due to hormonal fluctuations that can affect bile viscosity. On average, female patients notice a 46 week settling phase before symptoms stabilize, compared to 34 weeks for men.
AgeRelated Considerations
Older adults tend to have a higher chance of developing liverrelated issues years after the procedure. Agerelated declines in liver regenerative capacity and a higher prevalence of metabolic syndrome can compound the subtle shifts in bile flow.
Underlying Conditions That Worsen Outcomes
Having diabetes, irritable bowel syndrome (IBS), or obesity can amplify postoperative symptoms. These conditions already tweak digestion, so removing the gallbladder adds another variable to the mix.
Case Study: Jennys 5Year Journey
Jenny, a 42yearold teacher, had her gallbladder removed at 36. For the first year, she felt fine. At year three, she began experiencing intermittent rightside pain after meals rich in butter. A gastroenterologist identified a minor bileduct stone and prescribed a lowdose ursodeoxycholic acid. With diet tweaks (more omega3, less saturated fat) and a probiotic regimen, Jennys symptoms faded by year five. Her story illustrates how a proactive approach can turn a lingering issue into a manageable one.
When to Seek Help
RedFlag Symptoms Worth a Doctors Visit
If any of these appear, pick up the phone sooner rather than later:
- Sudden, severe abdominal pain that doesnt ease with overthecounter meds.
- Yellowing of skin or eyes (jaundice).
- Persistent vomiting or inability to keep food down.
- Unexplained weight loss or night sweats.
Diagnostic Tools & What They Reveal
Doctors typically start with blood work to check liver enzymes (ALT, AST) and bilirubin. Imaging might include:
- Abdominal ultrasound good for spotting residual stones or biliary dilation.
- Magnetic resonance cholangiopancreatography (MRCP) gives a detailed view of the bile ducts without radiation.
- Endoscopic retrograde cholangiopancreatography (ERCP) both diagnostic and therapeutic if stones need removal.
Treatment Options for Persistent Issues
Depending on the root cause, treatment can range from simple lifestyle changes to medical or endoscopic interventions:
- Ursodeoxycholic acid helps dissolve tiny bileduct stones.
- Endoscopic sphincterotomy relieves sphincter of Oddi dysfunction.
- Targeted dietary counseling often the first line for PCS.
- In rare cases, reexploration surgery may be considered.
Expert Quote
According to a gastroenterology specialist at the Mayo Clinic, Most longterm complaints after cholecystectomy can be managed conservatively. Early identification of the exact causewhether its a stone, functional disorder, or dietary triggerhelps avoid unnecessary surgeries.
The good news is that the majority of patients enjoy lasting relief after gallbladder removal, and serious complications are relatively uncommon. Still, a meaningful minority will notice digestive changes, occasional rightside discomfort, or subtle liverrelated shifts years down the road.
Understanding both the benefits and the potential longterm effects empowers you to spot warning signs early, adopt a balanced diet, and have informed conversations with your healthcare team. If you ever feel uncertain about a symptom, trust your instincts and reach out for a professional opinionyou deserve clarity and peace of mind.
Whats your experience with postgallbladder life? If youve discovered a helpful tip or a question thats still lingering, consider learning about specific supplements that can support gut healthfor example, ulcerative colitis supplements may offer useful probiotic and fiber approaches that overlap with postcholecystectomy care. Together, we can navigate the journey with confidence and compassion.
FAQs
What are the most common long-term effects of gallbladder removal?
The most common long-term effects include digestive changes like bloating, gas, diarrhea, and intolerance to fatty foods. Some people also experience ongoing right-side pain or mild liver enzyme changes.
Can gallbladder removal cause liver problems?
Yes, some people may see mild, temporary increases in liver enzymes after gallbladder removal. Persistent changes or symptoms like jaundice should be checked by a doctor.
How long do digestive symptoms last after gallbladder removal?
Most digestive symptoms improve within a few weeks to months, but some people may have ongoing issues, especially after eating fatty foods.
What diet is best after gallbladder removal?
A balanced diet with moderate fat, plenty of fiber, and probiotics is often best. Avoiding fried, greasy, and heavily processed foods can help reduce symptoms.