If youre wondering which ulcerative colitis drugs actually work, the short answer is: theres a whole toolbox, from 5ASA pills for mild flareups to the newest biologics and JAK inhibitors for tougher cases. Picking the right medicine isnt just about stopping symptomsits about keeping you feeling yourself, avoiding nasty sideeffects, and planning for the long haul.
Skipping treatment or guessing which drug is best can quickly turn a manageable flare into a painful, exhausting battle. Lets dive into the options, the latest breakthroughs, and what cure really means, all in a friendly chat that feels like a coffeetable conversation.
Drug Classes Overview
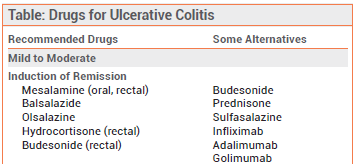
5ASA (Aminosalicylates)
These are the goto for many people with mild ulcerative colitis symptoms. They coat the lining of your colon and calm inflammation without turning your immune system upside down.
Common 5ASA Medications
| Medication | Brand | Typical Dose |
|---|---|---|
| Mesalamine | Asacol, Lialda | 2.4gdaily, divided |
| Sulfasalazine | Azulfidine | 24gdaily |
| Budesonide MMX | Uceris | 9mgdaily |
Corticosteroids
When a flare spikes, steroids can calm the storm fastbut theyre not meant for longterm use. Think of them as a rescue squad that you only call in emergencies.
Key Risks & Tapering Tips
- Weight gain, mood swings, bone thinning.
- Always follow a tapering schedule; abrupt stops can cause rebound inflammation.
Immunomodulators
Azathioprine and 6mercaptopurine work behind the scenes, training your immune system to be less aggressive. Theyre great for keeping remission steady, but they need regular blood tests.
Monitoring Checklist
- Complete blood count every 23months.
- Liver enzymes check at the same interval.
Biologics
Enter the big guns. These engineered antibodies target specific molecules that drive inflammation. If youve tried 5ASA and steroids without lasting relief, a biologic might be your next step.
Biologic Comparison (20242025)
| Drug | Target | Brand | Typical Dosing |
|---|---|---|---|
| Infliximab | TNF | Remicade | 5mg/kg IV at weeks0,2,6, then every 8weeks |
| Adalimumab | TNF | Humira | 40mg SC every 2weeks |
| Ustekinumab | IL12/23 | Stelara | 90mg SC every 8weeks |
| Vedolizumab | 47 integrin | Entyvio | 300mg IV at weeks0,2,6, then every 8weeks |
| Guselkumab | IL23 | Tremfya | 200mg SC every 8weeks |
JAK Inhibitors
These oral pills block the Janus kinase pathway, a key driver of inflammation. Theyre convenient, but the safety profile demands a careful conversation with your doctor.
Popular JAK Options
- Tofacitinib (Xeljanz) twice daily.
- Upadacitinib (Rinvoq) once daily, FDAapproved for ulcerative colitis in 2024.
- Filgotinib under review, promising early data.
Antibiotics & Emerging Therapies
Antibiotics arent a primary cure, but they play a role when infection complicates a flare or when pouchitis develops after surgery.
Typical Antibiotics Used
- Metronidazole for bacterial overgrowth.
- Ciprofloxacin often combined with metronidazole for pouchitis.
Research from the University of Chicago in 2025 suggests that targeted microbiome therapy may soon complement standard drugs, offering a gentler way to restore balance. For clinical guidelines and review articles on biologic use in inflammatory bowel disease, check this comprehensive resource on gastroenterology practice biologic therapy recommendations.
Best Medicine Options
Personalizing Best
There isnt a onesizefitsall answer to what is the best medicine for ulcerative colitis? The best drug depends on disease severity, previous response, lifestyle, and even genetics.
Decision Flowchart (Simplified)
- Mild Start with 5ASA.
- Moderate Add corticosteroids shortterm, then transition to immunomodulators or a biologic.
- Severe Jump straight to a biologic or JAK inhibitor, possibly combined with steroids for rapid control.
EvidenceBased Rankings
Metaanalyses published in show remission rates of about 60% for TNF blockers and 55% for newer JAK inhibitors. The numbers matter, but so does how each drug fits your life.
RealWorld Story
Take Anna, a 29yearold graphic designer. She started on mesalamine at 22, but after a stubborn flare at 27, her gastroenterologist switched her to ustekinumab. Within three months, her bloody stools vanished, and she could finally finish a marathon shed been training for. Stories like Annas remind us that best often means the one that works for you, not the one that looks best on paper.
Safety First
If best also means least risky, youll want to compare sideeffects. For example, steroids are powerful but can raise blood pressure and blood sugar. Biologics carry a small infection risk, especially for respiratory infections. JAK inhibitors have raised concerns about blood clots in highrisk patients.
Permanent Cure Reality
No Cure, Yet
Lets be honesttheres no permanent cure for ulcerative colitis today. What we can achieve is clinical remission, meaning your symptoms disappear and the colon heals enough to look normal on a scope.
Future Horizons
Scientists are exploring stemcell transplants and CRISPRbased gene editing. Early PhaseII trials in 2025 show promise, but were still years away from a definitive cure.
When Surgery Becomes an Option
If medications fail, surgical removal of the colon (colectomy) paired with an ileal pouchanal anastomosis (IPAA) can be lifechanging. Postsurgery qualityoflife studies report that 80% of patients stay symptomfree for five years or more.
Latest Treatment Advances
New FDAApproved Drugs
2024 saw the approval of guselkumab (Tremfya) for ulcerative colitis, expanding the IL23 inhibitor family. Early trials showed a 58% remission rate in patients who hadnt responded to older biologics.
Biosimilars Save Money
Now you can get the same therapeutic effect as Humira for a fraction of the price with biosimilars like adalimumabatto. Insurance plans love them, and many patients report smoother access.
Personalized Medicine
Fecal calprotectin levels and genetic panels are increasingly used to predict which drug will work best. Think of it as a weather forecast for your guthelping you pack the right umbrella before a storm.
Combination Strategies
Some doctors pair a biologic with a lowdose 5ASA to smooth out minor flares. The key is coordination: never start a new drug without your gastroenterologists goahead.
Balancing Benefits Risks
Efficacy vs. SideEffects
Every drug class carries its own tradeoff. Below is a quick matrix to help you weigh the pros and cons.
SideEffect Matrix
| Class | Common Benefits | Main Risks |
|---|---|---|
| 5ASA | Gentle inflammation control | Kidney stones (rare), nausea |
| Corticosteroids | Rapid symptom relief | Weight gain, bone loss, mood swings |
| Immunomodulators | Longterm remission | Liver toxicity, low white cells |
| Biologics | High remission rates | Infections, rare cancers |
| JAK Inhibitors | Oral convenience | Blood clots, cholesterol rise |
LongTerm Safety Data
The Mayo Clinics fiveyear registry shows that patients on biologics have a 2year infection risk of roughly 5%significantly lower than older steroids. Still, regular checkups are essential.
PatientCentred Decision Tools
Free printable checklists from the Crohns &Colitis Foundation help you compare cost, dosing, and sideeffects sidebyside. Knowing your priorities makes the doctorvisit feel like a partnership, not a sales pitch.
Cost & Insurance Navigation
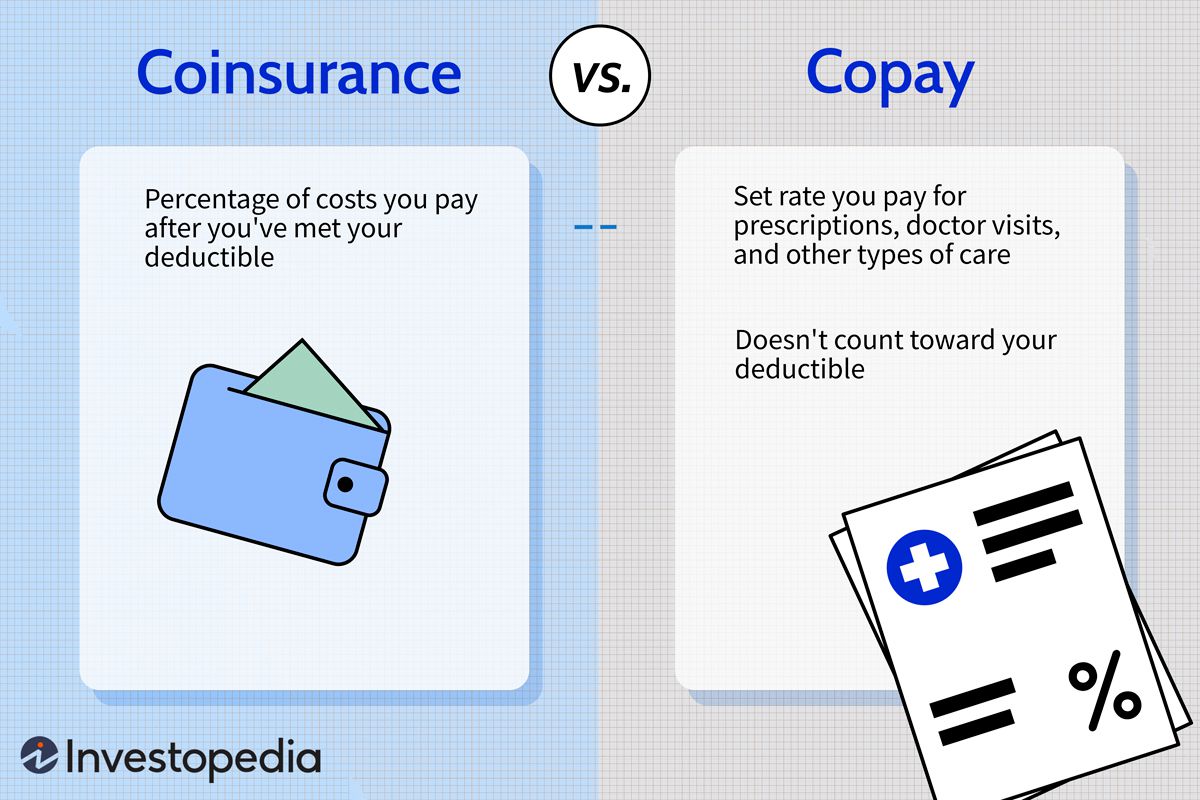
Dont let price be the silent barrier. Many drug manufacturers offer copayassistance programs, and biosimilars often qualify for lower tier coverage. A quick call to your pharmacy benefit manager can unlock significant savings.
Supporting Diet Lifestyle
Ulcerative Colitis Diet Basics
Food wont cure ulcerative colitis, but a thoughtful diet can ease medication sideeffects and reduce flare frequency. Aim for lowFODMAP foods during active flares and a balanced, fiberrich diet when youre in remission.
Sample 7Day Meal Plan
| Day | Breakfast | Lunch | Dinner |
|---|---|---|---|
| Mon | Plain oatmeal + banana | Grilled chicken salad (no onions) | Baked salmon, quinoa, steamed carrots |
| Tue | Greek yogurt + strawberries | Rice noodles with tofu & bok choy | Turkey meatballs, roasted potatoes |
| Wed | Scrambled eggs, spinach | Quinoa bowl with roasted zucchini | Grilled cod, sweet potato mash |
| Thu | Smoothie (blueberries, almond milk) | Turkey sandwich on sourdough (no whole grain) | Stirfried shrimp, bell peppers |
| Fri | Rice cereal + kiwi | Chicken broth with carrots | Lean beef steak, green beans |
| Sat | Plain toast + avocado | Salmon salad (no nuts) | Lentil soup (low fiber) |
| Sun | Banana pancakes | Egg salad on white bread | Roasted chicken, rice pilaf |
When Antibiotics Help
Antibiotics for colitis treatment are usually reserved for complications like pouchitis or a bacterial overgrowth that mimics flare symptoms. Theyre not a standalone cure, but they can clear the infection and give your meds a chance to work.
Lifestyle Hacks
- Stay hydratedaim for 2L of water daily.
- Reduce stress with short walks or mindfulness; stress can trigger flares.
- Avoid smoking; it worsens inflammation.
When Surgery Is Needed
If youve exhausted medical options, ulcerative colitis surgery can be lifesaving. The most common procedure, a colectomy with ileal pouchanal anastomosis, removes the diseased colon while preserving continence. Recovery takes 812 weeks, but many patients report a dramatic improvement in quality of life.
Conclusion
Ulcerative colitis drugs span a wide spectrumfrom gentle 5ASA tablets to powerful biologics and convenient JAK inhibitors. While a permanent cure remains out of reach, modern therapies can bring lasting remission, especially when paired with a sensible diet, lifestyle tweaks, and, when necessary, surgery. The key is a personalized plan that balances effectiveness with safety, cost, and your own daily rhythm.
Talk openly with your gastroenterologist, use decisionaid tools, and dont be afraid to ask questionsyour gut health is worth that conversation. Have you tried a particular medication that made a difference? Share your experience in the comments; together we can navigate this journey with confidence and compassion.
FAQs
What are the first‑line medicines for mild ulcerative colitis?
The go‑to drugs are 5‑ASA agents such as mesalamine (Asacol®, Lialda®) or sulfasalazine (Azulfidine®). They reduce inflammation locally without suppressing the whole immune system.
When are biologic therapies recommended?
Biologics are usually considered for moderate‑to‑severe disease that doesn’t respond to 5‑ASA, steroids, or immunomodulators, or when patients need to stay in long‑term remission.
How do JAK inhibitors differ from biologics?
JAK inhibitors (e.g., tofacitinib, upadacitinib) are oral pills that block intracellular signaling pathways, whereas biologics are injectable or IV antibodies that target specific extracellular cytokines.
What safety monitoring is needed for immunomodulators?
Patients on azathioprine or 6‑mercaptopurine need CBC and liver‑function tests every 2–3 months to catch low blood counts or liver toxicity early.
Can I combine a biologic with a 5‑ASA?
Yes. Many clinicians add a low‑dose 5‑ASA to a biologic to smooth out minor flares and possibly reduce the biologic’s dose, but any combination should be approved by your gastroenterologist.