Got irregular, heavy periods that just wont quit? Youre not alone, and there are solid options to get things back under control. Below is a friendly, stepbystep walkthrough of the most reliable treatment for DUBfrom meds you can pick up at the pharmacy to procedures that change the game. Lets dive in, arm you with the facts, and help you feel confident about the next move.
Understanding DUB
What is DUB?
DUB stands for dysfunctional uterine bleeding. In plain English, its abnormal bleeding that isnt caused by a structural problem like fibroids or polyps. Instead, it usually stems from hormonal imbalances that throw the lining of the uterus offtrack. Sometimes, conditions like lean PCOS can contribute to hormone disruption and menstrual irregularity, highlighting the importance of a thorough evaluation.
DUB Causes
Think of your menstrual cycle as a wellorchestrated dance. When the music (hormones) gets out of sync, the steps get messy. Common triggers include:
- Fluctuating estrogen and progesterone levels
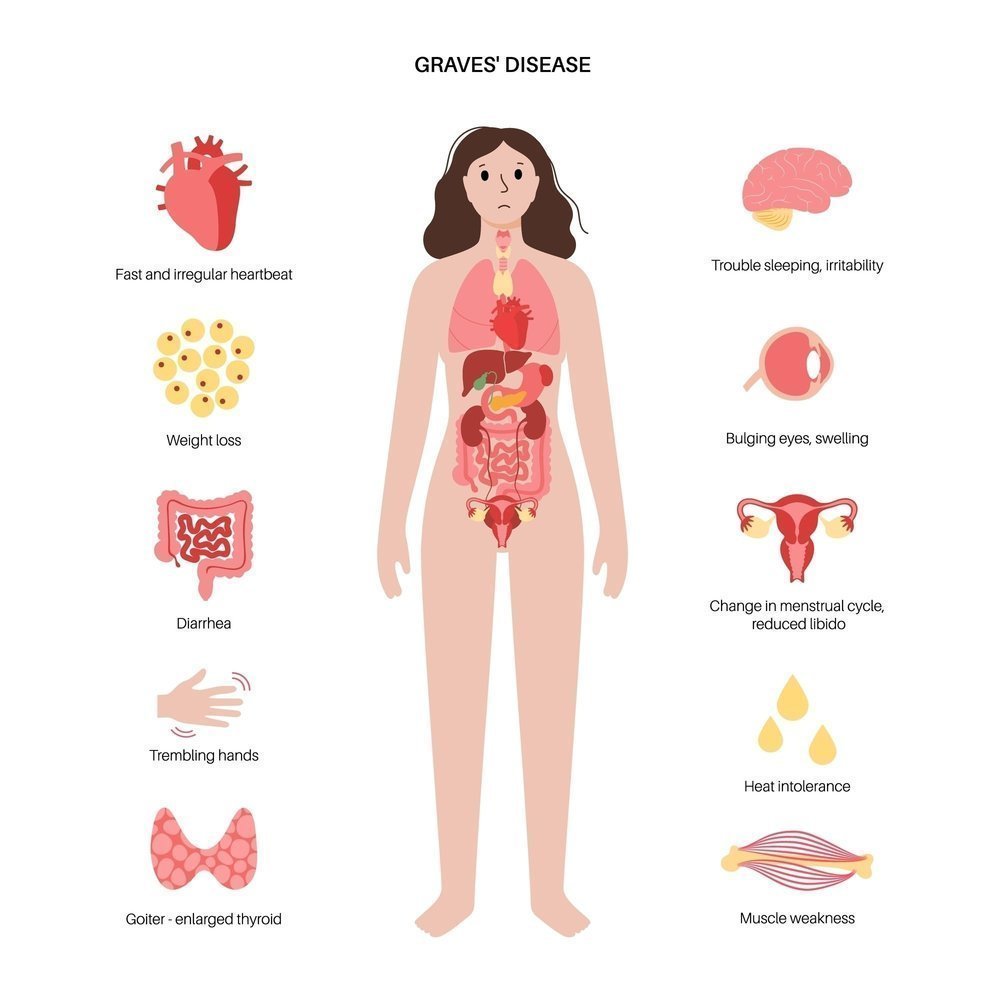
- Thyroid disorders
- Bloodclotting issues
- Stress or drastic weight changes
- Medications that interfere with hormone balance
When to Seek Help
Spotting a pattern matters. If you notice any of these red flags, reach out to your clinician sooner rather than later:
- Bleeding that soaks through a pad or tampon every hour
- Severe anemia symptomsfatigue, shortness of breath, pale skin
- Pain that feels more than typical menstrual cramps
- Bleeding during pregnancy or after a recent miscarriage
How Doctors Diagnose DUB
Diagnosis is a team effort. Your doctor will likely order:
- Blood tests (CBC, thyroid panel, clotting studies)
- Pelvic ultrasound to rule out fibroids or polyps
- Endometrial biopsy if the bleeding is prolonged or the patient is over 45
These steps ensure the treatment you receive hits the right target.
FirstLine Medical Therapies
Tranexamic Acid (TXA)
TXA is the goto stopthebleed pill for many. It works by slowing down the breakdown of clots, giving your uterus a chance to stabilize.
How to Use It
Typical dose: 1.01.5g taken orally every 8hours for the first five days of your period. Studies show a reduction in blood loss of up to 54% according to a 2025 review.
SideEffects & Contraindications
- Minor nausea or diarrhea
- Rarely, bloodclotting concernsavoid if you have a history of thrombosis
Combined Oral Contraceptives (COC)
COCs combine estrogen and progestin to keep the uterine lining thin and regular. Theyre a popular dub treatment progesterone option because they also double as birth control. Some may consider Yaz birth control or similar formulations for dual benefits in cycle regulation and contraception.
Typical Regimen
Take one active pill daily for 21days, followed by 7days of placebo. Youll likely notice lighter periods within a couple of cycles.
Benefits Beyond Bleeding
- Reduced acne
- Lower risk of ovarian cysts
- Consistent menstrual timing
ProgestinOnly Options
Cyclic Medroxyprogesterone Acetate (MPA)
MPA is taken for 1014days each month, mimicking the natural luteal phase. Its especially useful when estrogen isnt advisable.
LevonorgestrelReleasing Intrauterine System (LNGIUS)
Think of the LNGIUS (brand name Mirena) as a tiny, hormonefilled plug that releases 20g of levonorgestrel daily. It can cut menstrual blood loss by up to 90% and works for 35years.
Who Benefits Most?
If you want a lowmaintenance solution and arent actively trying to conceive, the LNGIUS often tops the list.
NSAIDs & Adjuncts
Ibuprofen or naproxen not only relieve cramps but can also modestly reduce bleeding by inhibiting prostaglandin production.
Quick Comparison
| Option | Bleed Reduction | Typical Duration | Major Risks | Ideal For |
|---|---|---|---|---|
| TXA | 3050% | Cyclebycycle | GI upset, rare thrombosis | Acute heavy bleed |
| COC | 2040% | Ongoing | VTE, bloodpressure rise | Want contraception |
| LNGIUS | 8090% | 35years | Cramping, expulsion | Longterm control |
| Endometrial Ablation | 90%+ | Onetime | Uterine perforation | 45yr, no future fertility |
| Hysterectomy | 100% | Single surgery | Major surgery risks | Completed childbearing, refractory DUB |
Procedural & Surgical Options
LevonorgestrelReleasing IUD (LNGIUS) StepbyStep
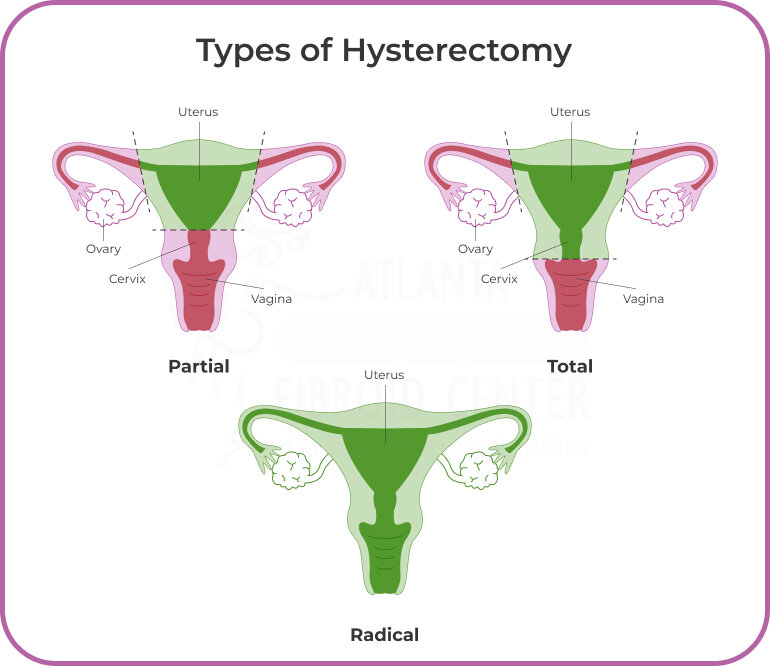
Insertion takes about 510minutes in a clinic. After placement, youll experience a few days of mild crampingnothing you cant handle with a heating pad and ibuprofen. For those exploring uterus-sparing options or seeking more permanent solutions, understanding the hysterectomy types available might help align treatment with future fertility goals.
Cost & Insurance
Many plans cover the device as a contraceptive, which often means a lower outofpocket cost than a surgical procedure.
Endometrial Ablation
Ablation destroys the uterine lining, dramatically reducing or eliminating periods. There are firstgeneration (balloon, microwave) and secondgeneration (thermal, radiofrequency) devices.
Whos a Candidate?
Women under 45 who dont plan future pregnancies and have tried (or cant tolerate) medical therapy.
Recovery Timeline
Most return to light activities within 12days. Full recovery is usually a week, and youll get a followup ultrasound to confirm the linings been addressed.
Hysterectomy & UterineSparing Surgeries
When bleeding is truly refractory, a hysterectomy offers a definitive cure. Todays minimally invasive approacheslaparoscopic or roboticmean smaller incisions, less pain, and quicker discharge.
When to Consider It?
- Severe anemia despite maximal medical therapy
- Concurrent large fibroids or adenomyosis
- Patients desire for a permanent end to bleeding
Emerging Techniques
Uterine artery embolization (UAE) and MRguided focused ultrasound are making headlines as uteruspreserving options for select patients. While still not firstline for DUB, theyre worth mentioning as the field evolves.
Nursing & SelfManagement Tips
Assessment Checklist for Nurses
When you (or your nurse) review a patient with DUB, a quick checklist helps keep things on track:
- Vital signs & hemodynamic stability
- Hemoglobin/hematocrit trend
- Bleeding diary (days, pad count, clots)
- Medication adherence review
- Psychosocial stressors and lifestyle factors
Patient Education Highlights
Empowerment comes from knowledge. Heres what to tell anyone navigating DUB:
- Iron intake: Include leafy greens, beans, or a gentle iron supplement to replenish losses.
- Hydration & diet: A balanced diet stabilizes hormones; excessive caffeine or alcohol can worsen bleeding.
- Stress management: Mindbody practices (yoga, meditation) have shown modest benefits on menstrual regularity.
When to Escalate Care
If a patients hemoglobin drops below 8g/dL, or if they report sudden, profuse bleeding (>1pad per hour for 2hours), an urgent referral to a gynecologist is warranted.
Sample PPT Slide Titles
For clinicians who love visual aids, consider these slide headings for a Nursing Management of Dysfunctional Uterine Bleeding presentation:
- Pathophysiology of DUB
- FirstLine Pharmacologic Options
- Algorithm for Treatment Escalation
- Case Study: From TXA to LNGIUS
Balancing Risks, Benefits & Making the Right Choice
Weighing Pros & Cons
Every treatment comes with a tradeoff. Below is a quick, balanced look at the most common options.
- TXA: Fast, inexpensive, but not a longterm solution.
- COC: Dual benefit of contraception; watch for bloodclot risk if you smoke.
- LNGIUS: Longlasting and highly effective; insertion can be uncomfortable for some.
- Ablation: Great for those who dont want future periods; not reversible.
- Hysterectomy: 100% cure but major surgeryconsider only after exhausting other routes.
Shared DecisionMaking Tool
Print out (or download) a simple flowchart that asks three questions:
- How severe is the bleeding? (Mild, moderate, severe)
- Do you want future pregnancies?
- Are you comfortable with hormones or prefer a nonhormonal route?
Your answers guide you toward the most suitable option. Its a collaborative conversation, not a onesizefitsall prescription.
Cost & Insurance Snapshot
Medication (TXA, COC) usually falls under pharmacy benefitslow copay in most plans. The LNGIUS often qualifies as a contraceptive device, meaning many insurers cover the upfront cost. Procedures like ablation or hysterectomy may have higher outofpocket expenses, but many health plans cover a large portion if deemed medically necessary.
Putting It All Together
Lets recap the journey:
- Identify whether your bleeding truly fits the definition of DUB.
- Start with the simplest, evidencebacked medsTXA, COC, or a progestin regimen.
- If medication isnt enough, consider the LNGIUS or an ablative procedure.
- Reserve surgery for cases where other routes have failed or arent appropriate.
- Throughout, keep a bleeding diary, monitor iron levels, and stay in touch with your healthcare team.
Remember, youre not alone in this. Every step you takewhether its ordering a pharmacy refill or scheduling a clinic visitbrings you closer to a steadier, more comfortable cycle.
Conclusion
Dealing with dysfunctional uterine bleeding can feel overwhelming, but a clear roadmap existsfrom inexpensive TXA tablets to longlasting hormonal IUDs and, when necessary, minimally invasive surgeries. Weve highlighted the most effective treatment for DUB, weighed benefits against risks, and offered practical tools to help you discuss options with your clinician. Download the cheatsheet, start a conversation, and take charge of your health today. Your wellbeing is worth the effortlets get those periods back on track together.
FAQs
What is the first‑line medication recommended for DUB?
Tranexamic acid (TXA) is often the initial drug of choice because it quickly reduces menstrual blood loss by stabilizing clots, usually taken for the first five days of the period.
Can combined oral contraceptives (COCs) treat DUB?
Yes. COCs regulate the hormonal cycle, thin the uterine lining, and often lessen bleeding while also providing contraception.
How does the levonorgestrel‑releasing IUD help with DUB?
The LNG‑IUS releases a low dose of levonorgestrel locally, cutting menstrual blood loss by up to 90 % and works continuously for 3–5 years without daily pills.
When should a patient consider endometrial ablation?
Endometrial ablation is suitable for women under 45 who have persistent heavy bleeding despite medication and do not desire future pregnancies.
What are the main risks of a hysterectomy for DUB?
While it provides a 100 % cure, hysterectomy carries typical surgical risks such as infection, bleeding, injury to surrounding organs, and a longer recovery period.