Quick Answer
What is pediatric SIRS? Its the presence ofat least two of the four physiological abnormalitiestemperature, heart rate, respiratory rate, and whitebloodcell countplus a suspected or proven infection. When these signs line up, youve got the first red flag that could turn into sepsis or septic shock.
Core Components
Temperature
Kids dont always run a fever the way adults do. In the sirs criteria pediatrics, a temperature>38.5C or<36C counts as abnormal. For neonates, even a modest rise can be worrisome, so keep an eye on those tiny thermometers.
Heart Rate
Whats a fast heart rate for a toddler? Generally, its any rate more than2standard deviations above the ageadjusted mean. Roughly speaking, thats >180bpm for infants under one year and >140bpm for kids 15years old. (You can doublecheck exact cutoffs with the .)
Respiratory Rate
Rapid breathing>2SD above age normsor a need for mechanical ventilation meets the respiratory criterion. Below is a handy reference table you can print and stick on your workstation.
| Age | Normal Temp (C) | HR (bpm) | RR (breaths/min) | WBC (10/L) |
|---|---|---|---|---|
| 01mo | 36.538.0 | 120160 | 3060 | 930 |
| 112mo | 36.538.0 | 100150 | 3060 | 520 |
| 15yr | 36.538.0 | 80130 | 2030 | 415 |
| 612yr | 36.538.0 | 70110 | 1525 | 412 |
| 1318yr | 36.538.0 | 60100 | 1220 | 411 |
WhiteBloodCell Count
Leukocytosis>12000/L, leukopenia<4000/L, or10% immature bands hit the lab box. Remember, a single abnormal value isnt enoughcombine it with the other signs to trigger the SIRS flag.
From SIRS to Sepsis
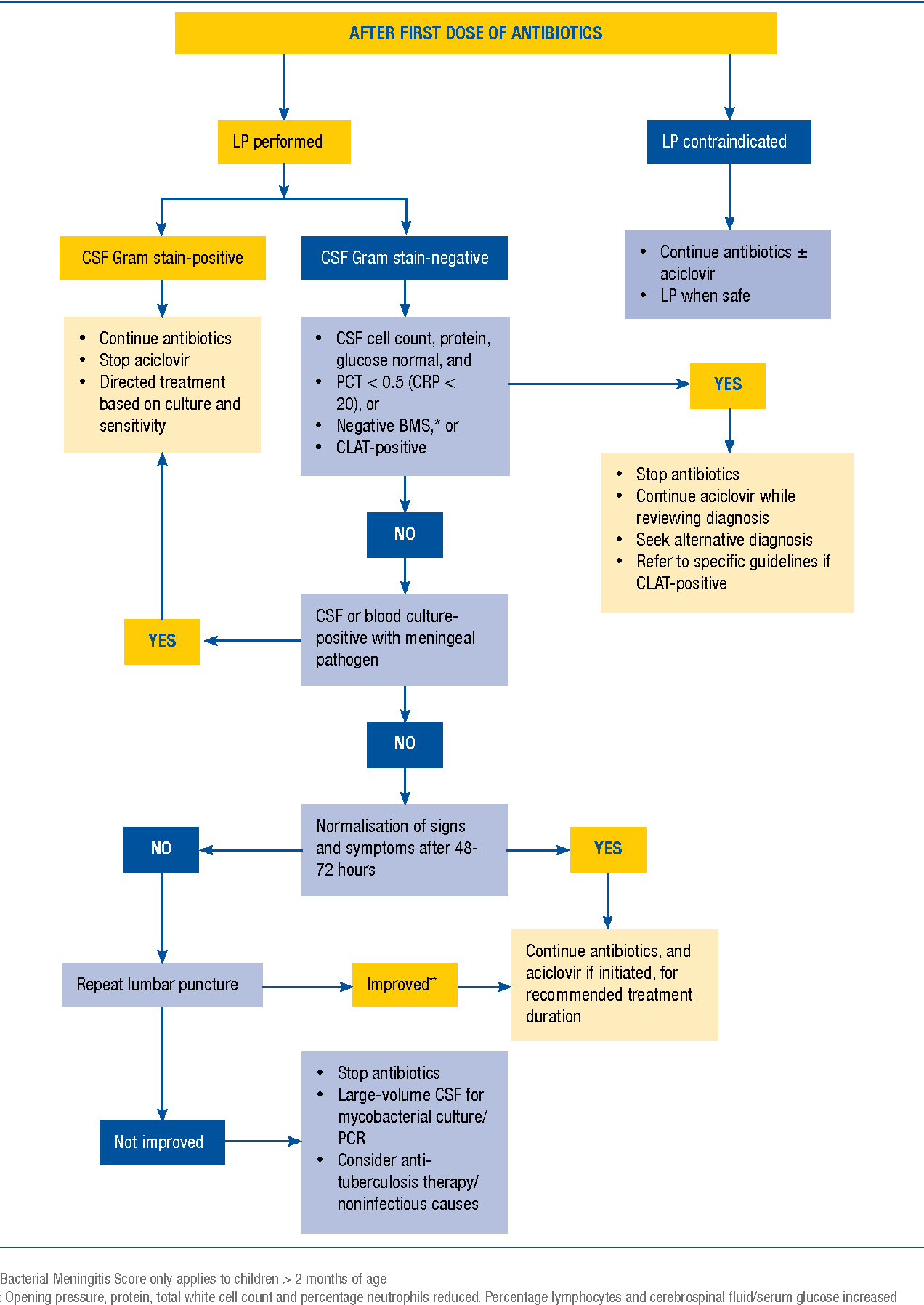
Once youve identified SIRS, the next step is to ask, Is there an infection? If yes, youre looking at sepsis. The spells this out clearly: two or more SIRS criteria+suspected infection equals sepsis, and you need to start broadspectrum antibiotics within the first hour.
Septic Shock
Septic shock is sepsis that wont back down. Its defined by persistent hypotension or the need for vasoactive medications despite adequate fluid resuscitation. Think of it as the storm that wont clear. The same guidelines give a simple decisiontree you can paste on the back of a chart:
- Is SIRS present? Yes
- Is infection suspected? Yes
- Is perfusion abnormal (cold extremities, altered mental status, rising lactate)? Yes Treat as septic shock.
Phoenix Score
If youve been following the International Consensus Criteria for Pediatric Sepsis and Septic Shock (JAMA, 2024), youve likely heard about the Phoenix sepsis score. It adds a layer of organdysfunction weighting on top of SIRS, making the diagnosis a bit more precise.
How It Works
The Phoenix tool awards one point for each of these:
- Elevated lactate (>2mmol/L)
- Capillary refill>2seconds
- Altered mental status
- Low urine output (<0.5mL/kg/h)
- Use of vasoactive meds
A score of2or more, combined with SIRS, confirms pediatric sepsis according to the 2024 consensus. Its like having a second opinion from a seasoned intensivistright in your pocket.
RealWorld Example
Emily, a 3yearold, was brought in with a temperature of 39.2C, heart rate 140bpm, respiratory rate 38, and a WBC of 13000. She met three SIRS criteria. Her lactate was 3.1mmol/L and she had delayed capillary refill, giving her a Phoenix score of 2. The team flagged her for early fluid bolus and antibiotics, and within hours her vitals started to stabilize. Stories like Emilys remind us why marrying SIRS with Phoenix can save lives.
Balancing Benefits & Risks
Every diagnostic tool has a bright side and a shadow. Lets break it down.
Benefits
- Speed. You can identify a potentially septic child in minutes.
- Standardization. Everyone on the floor speaks the same language.
- Evidencebased. Rooted in the latest pediatric sepsis guidelines 2024 pdf and peerreviewed studies.
Risks
- Overtriage. Viral infections can meet SIRS thresholds, leading to unnecessary antibiotics.
- Missed atypical cases. Immunocompromised kids may not mount a fever, slipping through the cracks.
Mitigation Strategies
Combine SIRS with clinical judgment and objective biomarkers like lactate or procalcitonin. Use watchful waiting protocols for lowrisk patientsmonitor vitals closely, repeat labs, and involve families in the decisionmaking process.
| Pros | Cons |
|---|---|
| Rapid screening, evidencebased, easy EMR integration | Potential falsepositives, may miss atypical presentations |
Trusted Resources
When youre building your own SIRS toolkit, rely on sources you can trace back to the original research:
- free and regularly updated.
- JAMAs (2024) the goldstandard reference.
- The your bedside companion.
- Seattle Childrens research on the Phoenix criteria accessible through the hospitals openaccess repository.
Practical Takeaways
- Download the pediatric sepsis guidelines 2024 pdf today and bookmark the agespecific SIRS table.
- Use the free MDCalc tool at the bedside for instant scoring.
- Integrate the Phoenix score into your EMR order set for children with suspected infection.
- Educate the whole care team about both the strengths and the pitfalls of SIRS to avoid overtriage.
- Share your own storieswhether a case where SIRS saved a life or where it led to an unnecessary antibiotic. The community learns from each other.
Conclusion
In the whirlwind of pediatric emergency care, the sirs criteria pediatrics acts like a trusted compass, pointing you toward the early signs of sepsis. Pair it with the Phoenix sepsis score, stay current with the pediatric sepsis guidelines 2024 pdf, and youll have a robust, evidencebased approach that balances speed with safety. Remember, every child is uniqueuse the criteria as a guide, not a rule, and always blend data with your clinical gut feeling.
Whats your experience with pediatric SIRS? Have you tried the Phoenix score in your unit? Drop a comment below, share a story, or ask a question. Together well keep sharpening the tools that protect our youngest patients.
FAQs
What are the four components of the pediatric SIRS criteria?
The criteria include abnormal temperature, elevated heart rate, increased respiratory rate (or need for ventilation), and an abnormal white‑blood‑cell count, with at least two present plus a suspected infection.
How does SIRS differ from sepsis in children?
SIRS is the physiological response (the four signs) and can occur without infection. When SIRS occurs together with a proven or suspected infection, it meets the definition of pediatric sepsis.
When should I order a white‑blood‑cell count for a febrile child?
Obtain a CBC when the child shows two or more SIRS signs, especially if the fever is >38.5 °C or <36 °C, or if the clinical picture suggests a possible bacterial infection.
What is the Phoenix score and how is it calculated?
The Phoenix score adds one point for each of these: lactate >2 mmol/L, capillary refill >2 seconds, altered mental status, urine output <0.5 mL/kg/h, and use of vasoactive meds. A score ≥ 2 together with SIRS confirms pediatric sepsis.
What are common pitfalls when using SIRS criteria in pediatrics?
Over‑triage can occur because viral infections often meet SIRS thresholds, leading to unnecessary antibiotics. Conversely, immunocompromised or neonates may not mount a fever, risking missed cases. Combine SIRS with clinical judgment and biomarkers like lactate to mitigate these issues.