Well, youve just gone through one of the biggest surgeries of your life, and now youre probably wondering: When can I start feeling like myself again? The short answer is that most people begin light daily activities in about three to four weeks, but a full return to normal can stretch anywhere from six weeks to three monthsespecially if lymph nodes were removed. Your recovery speed will hinge on the type of hysterectomy you had, your overall health, and any sideeffects that pop up along the way.
Were going to walk through everything you need to knowtimeline, common symptoms, ways to speed up healing, and even how your partner can be the best support system possible. Think of this as a friendly chat over a cup of tea, with a sprinkle of practical tips and a dash of encouragement.
Understanding the Surgery
What exactly is a hysterectomy for cancer?
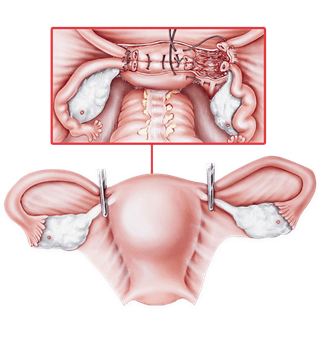
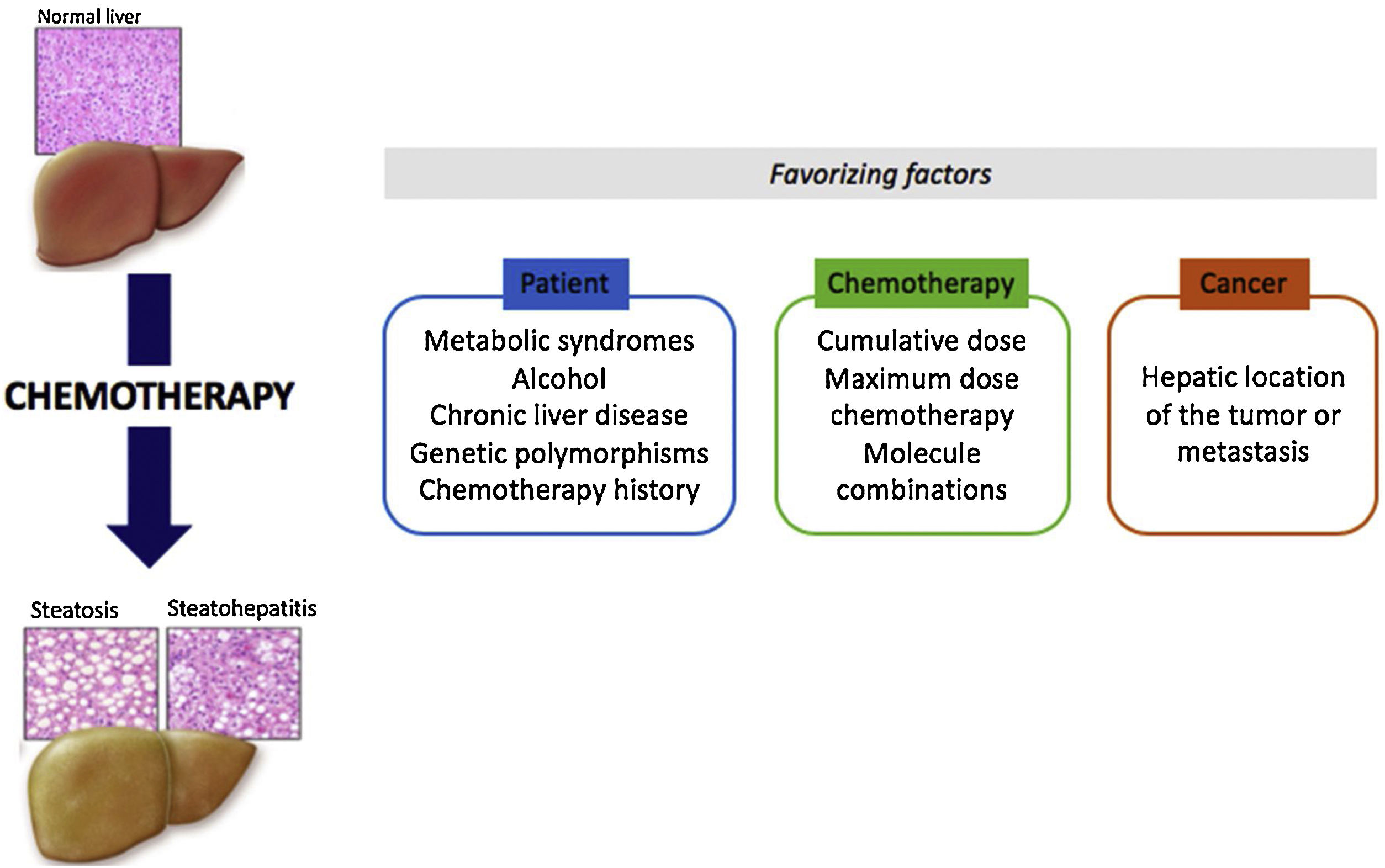
A hysterectomy is the surgical removal of the uterus, and when its done for cancer, the surgeon often takes the cervix, ovaries, and fallopian tubes as well. The procedure can be performed in three main ways:
- Abdominal (open) hysterectomy: A larger incision in the belly.
- Laparoscopic hysterectomy: Small ports and a camera guide the surgeon.
- Vaginal hysterectomy: The uterus is removed through the vagina, no belly incision.
Each technique has its own recovery profile, which well dive into later.
Why does removing lymph nodes matter?
If your cancer had a chance to spread, surgeons might also take a few nearby lymph nodes to check for cancer cells. This step is crucial for staging, but it can add a little extra baggage to your recovery because the body needs to adjust to the loss of those drainage pathways.
Typical hospital stay by surgery type
| Surgery Type | Average Length of Stay (Days) | Average Full Recovery |
|---|---|---|
| Abdominal (open) | 27 | 612 weeks |
| Laparoscopic | 13 | 48 weeks |
| Vaginal | 02 | 36 weeks |
Recovery Timeline
Day 02: The washout phase
Right after surgery, the focus is on pain control, keeping the bladder emptying properly, and getting you up and movingyes, even if you feel like a marble statue. Early ambulation (walking around the room) helps prevent blood clots and gets your lungs breathing easier.
Weeks 12: The shaky start
This is where most people feel the Im not ready for life vibe. Youll likely experience fatigue, soreness around the incision, and maybe a little constipation. Keep a glass of water by the bedside, sip often, and aim for short walks several times a day. Gentle stretching can keep your muscles from locking up.
Weeks 36: Getting back on your feet
By now you should be able to handle light household chores and maybe even return to a desk job if you sit most of the day. Pelvicfloor physiotherapy is a gamechangerthose muscles support your bladder and bowels, and strengthening them reduces leakage and discomfort.
Weeks 712: The full recovery window
Heavy lifting (anything over 10lb), intense cardio, and sexual activity should be approached with caution. Most surgeons give the green light for these after a followup exam confirms your incision is fully healed and theres no sign of infection.
Recovery checklist by phase
- 02days: Pain meds on schedule, deepbreathing exercises, short walks.
- Weeks12: Keep incisions clean, increase fluid intake, start gentle stretching.
- Weeks36: Begin pelvicfloor exercises, return to light work, monitor any unusual swelling.
- Weeks712: Gradually reintroduce heavier activity, discuss sexual activity with your doctor, schedule final postop visit.
Managing Common Side Effects
Pain and cramping
Its normal to feel a dull ache around the belly button and lower back for a few weeks. Overthecounter NSAIDs (like ibuprofen) work for mild pain, but if you need stronger medication, talk to your surgeondont let the pain dictate your day.
Swelling and lymphedema
When lymph nodes are removed, the fluid that usually travels through them can pool, causing swellingoften in the legs or groin. Compression garments, gentle lymphatic massage, and staying active are the three pillars of managing this.
Bowel and bladder changes
Constipation is a notorious sideeffect of pain meds and reduced mobility. Load up on fiber, drink plenty of water, and consider a mild stool softener if needed. For bladder training, practice doublevoiding (peeing, waiting a few minutes, then trying again) to empty the bladder completely.
Emotional ups and downs
Its perfectly okay to feel a rollercoaster of emotions after a cancerrelated hysterectomy. Some people experience a sense of loss, others feel relief. If you notice persistent sadness or anxiety, reach out to a counselor or join a support grouplike those offered by . You dont have to walk this road alone.
Reallife anecdote (optional for experience)
Jane, a 47yearold teacher, shared that her sixweek comeback felt impossible at first. By focusing on short, achievable goalslike walking to the mailbox each morningshe gradually built confidence. Within two months she was back in the classroom, using a small standing desk to ease lowerback strain.
Survival and LongTerm Outlook
Hysterectomy cancer survival rate
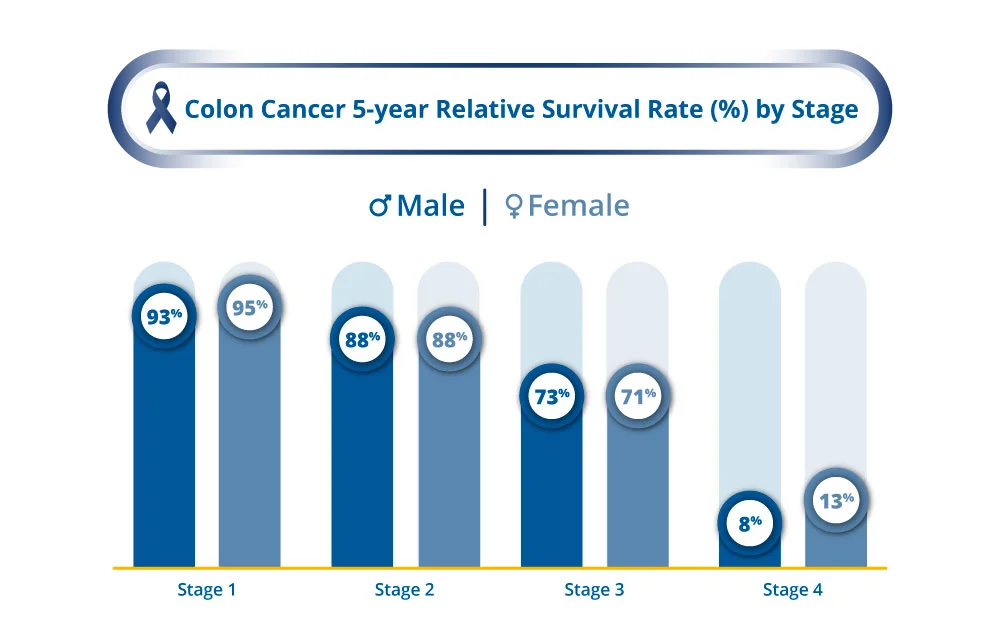
For earlystage endometrial (uterine) cancer, the fiveyear survival rate after a complete hysterectomy ranges from 85% to 90%according to data from the . This high success rate underscores why surgery remains the cornerstone of treatment.
Recurrence risk after total hysterectomy
Most recurrences happen within the first two to three years postsurgery. Regular followup appointments, imaging when indicated, and monitoring any new symptoms are essential to catch anything early.
Life expectancy after total hysterectomy
When the hysterectomy is performed for benign reasons, life expectancy isnt affected. For cancer patients, the prognosis largely mirrors the stage at diagnosisso an early detection combined with a successful surgery often means a normal lifespan.
Does a total hysterectomy increase risk of other cancers?
Current research shows no strong link between a hysterectomy and a higher risk of cancers elsewhere. However, if the ovaries are also removed (oophorectomy), you might experience earlier menopause, which can subtly shift the risk profile for bone health and heart disease. Hormonereplacement therapy (when appropriate) can help balance this.
Partner and Caregiver Support
What husbands (or partners) can do daytoday
Simple gestures go a long way. Bringing a cup of tea, handling grocery trips, or just sitting with you while you rest can lift a huge weight off your shoulders. Emotional supportlistening without trying to fix everythingcreates a safe space for you to vent.
Redflag symptoms to watch for
If you notice any of the following, call your healthcare team right away:
- Fever over 38C (100.4F) that persists.
- Heavy vaginal bleeding (soaking a pad in under an hour).
- Severe, sudden abdominal pain.
- Rapid swelling in the legs or groin.
Partner checklist (downloadable PDF idea)
Consider creating a short printable list with Medication reminder, Meal prep, and Checkin time columns. Having a visual cue helps both of you stay on track.
Lifestyle Tips to Speed Healing
Best foods for wound healing
Protein is your best friendthink lean chicken, beans, Greek yogurt. Omega3 rich foods like salmon reduce inflammation, while ironrich spinach and lentils support blood health. And dont forget hydration; aim for at least eight glasses of water a day.
Safe exercises and when to start
Walking is the gold standard from day one. After two weeks, add gentle stretching and maybe a beginners yoga video that focuses on breathing. Pelvicfloor physio, as mentioned earlier, should start around week three if you feel ready.
Sleep and stressreduction
Recovery happens while you snooze. Keep the bedroom cool, limit screens an hour before bed, and practice a short body scan meditationstarting at the toes and moving upwardto calm the mind.
Helpful Resources and Credible Sources
Building trust means linking to places that know their stuff. Here are a couple of goto sites for deepdive information and patient forums:
- uptodate stats, treatment guidelines, and support group directories.
- detailed explanations of procedures, recovery tips, and symptom checkers.
Conclusion
Recovering from a hysterectomy for cancer is a journey that blends physical healing with emotional resilience. By understanding the type of surgery you had, following a realistic timeline, managing sideeffects with proven strategies, and leaning on trusted partners and reputable resources, you set yourself up for the best possible outcome. Remember, every stepno matter how smallcounts toward getting back to the life you love. If you have questions, reach out to your care team; theyre there to help you navigate each milestone.