If you or someone you love is living with endstage chordoma, the most pressing questions are usually about the symptoms that crop up as the disease advances. In short, you can expect worsening pain right where the tumor sits, new neurological problems such as numbness or loss of bladder control, and a steady decline in mobility that makes everyday tasks feel like climbing a mountain.
Knowing these signals helps you and your care team decide when to shift the focus from aggressive cures to comfortoriented care. Below, Im breaking down the symptoms youre likely to see, why they happen, and what you can actually do about themall written in a friendly, plainEnglish style, as if we were chatting over coffee.
What EndStage Means
Defining the EndStage
In medical terms, endstage chordoma refers to a point where the tumor has either grown back after previous treatments or has spread to a degree that further surgery or radiation offers only limited benefit. Its not a sudden switch; its a gradual progression marked by the bodys decreasing ability to compensate for the tumors intrusion.
Why Location Matters
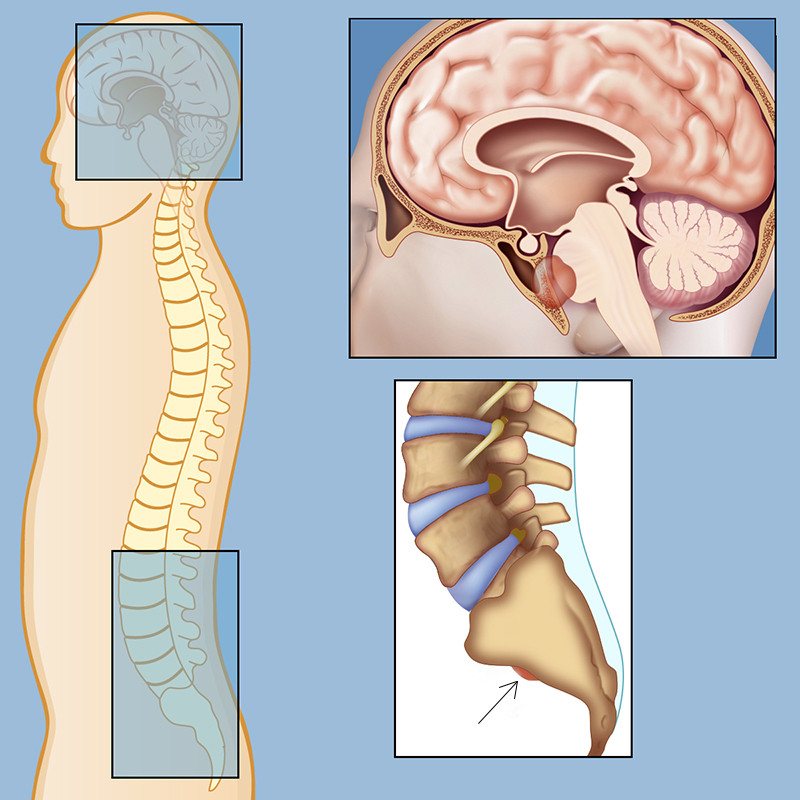
Chordomas can sit in the sacrum (the base of the spine), the clivus (a small part of the skull base), or anywhere along the mobile spine. Each spot brings its own set of symptoms because of the nerves and structures nearby. Thats why youll see different warning signs for sacral chordoma symptoms versus clival chordoma life expectancy concerns.
Typical Timeline
| Location | Common First Sign | Average Time to EndStage |
|---|---|---|
| Sacrum | Lowback or tailbone pain | 57years after diagnosis |
| Clivus | Headache or double vision | 46years after diagnosis |
| Mobile spine | Midback or rib pain | 35years after diagnosis |
Core Symptoms Overview
Pain That Wont Quit
Persistent, deepshooting pain right where the tumor lives is the hallmark of endstage chordoma. If youve already tried standard painkillers, overthecounter meds, or even radiation and the ache still hovers, thats a clear sign the disease is progressing.
Neurological Changes
As the tumor presses on nerves, you might notice tingling, numbness, or weakness in the legs, arms, or even the face. For sacral chordoma symptoms, loss of bladder or bowel control is common, while clival tumors often cause facial numbness or vision problems.
Mobility Decline
Walking up stairs starts feeling like a marathon, and simple tasks like getting out of a chair become a chore. Many people end up relying on walkers, canes, or wheelchairs as the disease advances.
Quick Symptom Checklist
- Severe, constant pain at the tumor site
- New numbness or weakness in limbs
- Bladder or bowel urgency or incontinence
- Frequent falls or need for assistive devices
- Vision or facial sensation changes (clival cases)
Symptoms by Tumor Site
Sacral Chordoma Symptoms
People with sacral chordoma often describe a deep ache behind the tailbone that radiates into the pelvis. Over time, the pain spreads, and you may notice difficulty sitting for long periods. Bowel and bladder changes are also a red flag because the sacral nerves control those functions.
Clival Chordoma Symptoms
When the tumor sits at the skull base, the first signs might be a persistent headache or double vision. As it grows, facial numbness, difficulty swallowing, or even hearing loss can appear. These symptoms tie directly into clival chordoma life expectancy discussions, because brainstem involvement can accelerate the need for palliative care.
MobileSpine Chordoma Symptoms
Thoracic or lumbar chordomas cause midback or rib pain, sometimes accompanied by a feeling of tightness around the chest. If the tumor compresses the spinal cord, you could see weakness in the legs and, in severe cases, respiratory compromise.
Comparison Table
| Site | Primary Pain Location | Neurologic Signs | Typical Onset |
|---|---|---|---|
| Sacrum | Tailbone / lower back | Bladder/bowel issues, leg numbness | Months to years |
| Clivus | Headache | Double vision, facial numbness | Months |
| Mobile spine | Midback / ribs | Leg weakness, respiratory issues | Months to years |
RedFlag Warning Signs
When to Call Your Surgeon Immediately
Some changes demand urgent medical attention. If you suddenly lose the ability to move a limb, experience uncontrolled bleeding from a tumor ulcer, or have a severe pain spike that no medication eases, call your oncology team right away. Rapid mental status changes can signal brainstem involvement, especially in clival cases.
Palliative Symptom Management
PainControl Strategies
Highdose opioids, nerve blocks, and targeted radiation are the big three for endstage pain. Many centers also employ patientcontrolled analgesia pumps, which let you manage doses without waiting for a nurse.
Neurological Relief
Physical therapy can keep muscles from atrophying, while medications like baclofen pumps help calm spasticity. Antispasmodics and lowdose antidepressants are sometimes used to ease nerverelated discomfort.
Medical Options
Even in the end stage, some patients qualify for targeted therapies that slow tumor growth. A recent study from highlighted modest improvements in pain scores for patients on experimental kinase inhibitors.
Pros/Cons Table
| Option | Benefit | Risk |
|---|---|---|
| Opioids | Strong pain relief | Constipation, sedation |
| Nerve block | Targeted, shortterm relief | Infection risk |
| Radiation | Reduces tumor size | Skin changes, fatigue |
| Targeted therapy | May slow growth | Limited data, side effects |
QualityofLife Focus
Emotional Support
Living with a rare cancer can feel isolating. Studies show that up to 30% of chordoma patients experience clinically significant depression. Counseling, support groups, and even online communities can make a huge difference.
HomeCare Resources
Homehealth nurses, occupational therapists, and adaptive equipment (like raised toilet seats) are essential for maintaining independence. Many patients find that a simple grab bar in the bathroom restores confidence.
DecisionMaking Framework
Balancing chordoma cancer life expectancy numbers with daily quality of life is tough. A useful approach is to ask: If I choose treatment X, how will my days look in the next month? This shortterm lens often clarifies whether the benefit outweighs the burden.
Common Patient Questions
Is chordoma curable in the end stage?
Unfortunately, once a chordoma reaches the end stage, curative options are extremely limited. The goal shifts to controlling symptoms and preserving dignity.
What are the first signs of sacral chordoma?
Early warning signs include persistent tailbone pain, occasional numbness in the buttocks, and mild changes in bowel habits. Recognizing these early can lead to earlier intervention, potentially delaying the endstage phase.
How long do patients typically live after reaching endstage?
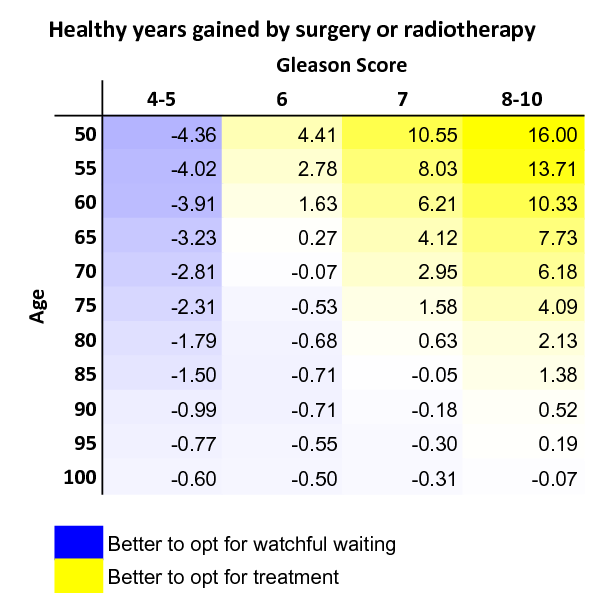
Survival varies by tumor location. Clival chordoma life expectancy after reaching end stage averages 1218months, while sacral cases often range from 1824months, according to data from the . For patients weighing treatment burden against benefit, resources on prostate cancer outlook offer useful examples of balancing prognosis and quality of life in oncology care.
Can I see real images of chordoma in the tailbone?
Yesmany reputable sites host chordoma tailbone pictures that help patients visualize whats happening inside. Seeing the tumor can make treatment discussions feel more concrete.
RealWorld Patient Stories
Sarahs Journey (Sacral Chordoma)
Sarah, a 46yearold teacher, noticed a dull ache behind her tailbone that didnt go away after a week. By the time she received a diagnosis, the tumor had already grown large enough to affect her bladder. Her story, shared on a patient forum, emphasizes how crucial early medical attention is, even when symptoms seem just a backache.
Mikes Experience with Palliative Radiation
Mike, diagnosed at 58 with a clival chordoma, reported that targeted radiation in his endstage phase reduced his headache intensity from a constant 8/10 to a manageable 3/10. He credits the multidisciplinary team for offering hope when cure was no longer an option.
Key Takeaways Box
- Early pain doesnt always mean a simple strainlisten to your body.
- Open, honest conversations with your specialist empower better decisions.
- Support networks are lifesavers; you dont have to face this alone.
Expert Guidance Resources
Why See a HighVolume Surgeon?
Surgeons like Dr. Aaron CohenGadol, who treat dozens of chordoma cases each year, have refined techniques that can extend life and improve symptom control. Their expertise often translates into fewer complications and more personalized care plans.
Top Academic Sources
For deeper dives, consult the latest research from Johns Hopkins, the Cleveland Clinic, and the Chordoma Foundation. These institutions regularly publish peerreviewed articles that keep you uptodate on evolving treatments.
Support Communities
Online forums, local patientadvocacy groups, and socialmedia circles provide spaces to share stories, ask questions, and find emotional comfort. Connecting with someone whos walked a similar path can turn fear into shared strength.
Conclusion
Endstage chordoma brings a heavier symptom load, but knowing exactly what to look forpersistent pain, neurological changes, and mobility losshelps you act swiftly and keep control over your care. By balancing palliative options with qualityoflife goals, and leaning on trusted experts like Dr. CohenGadol and reputable organizations, you can navigate this challenging phase with clearer expectations and stronger support. If you have more questions or want to share your own experience, feel free to reach out to a specialized chordoma center or join a patient community today.