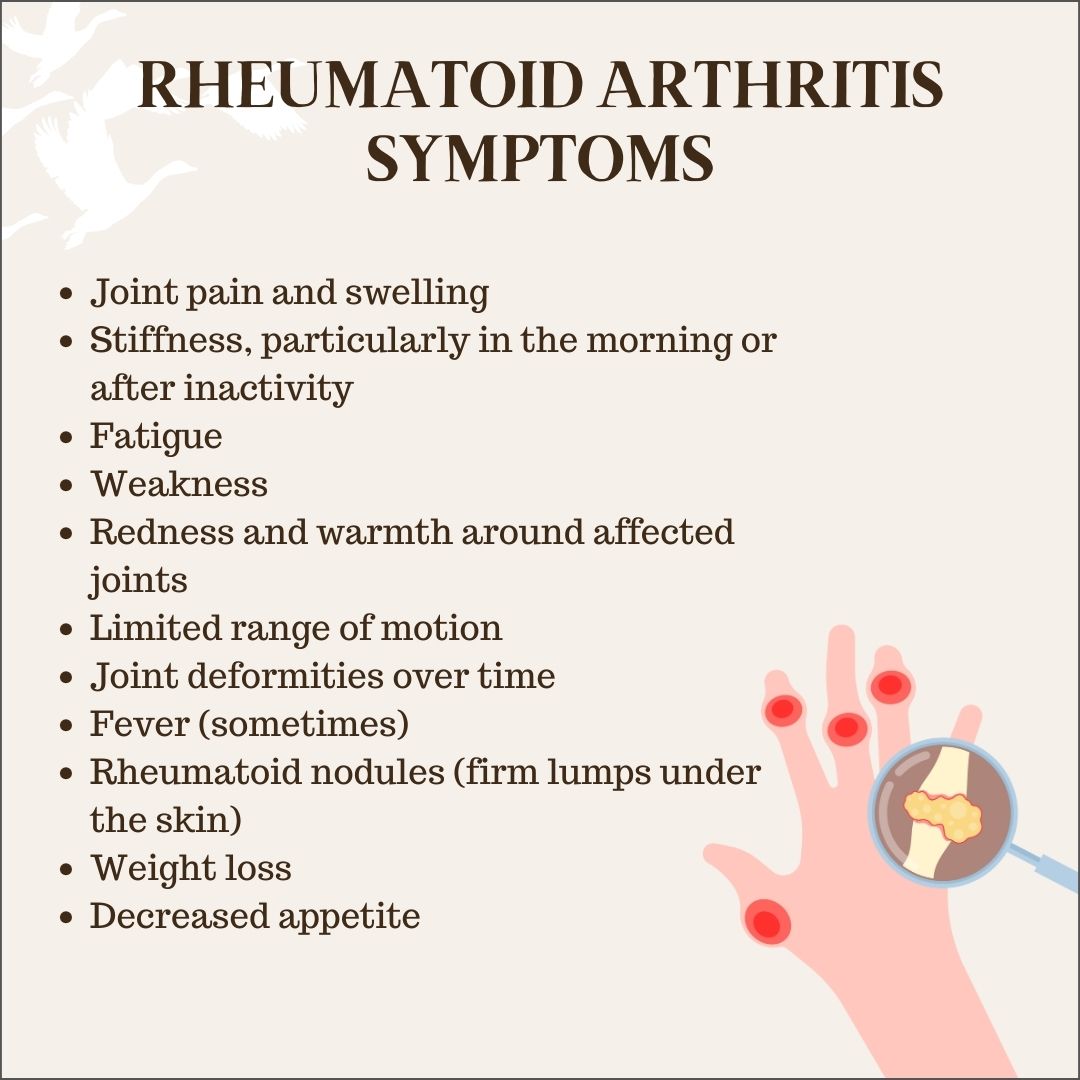
Most people with rheumatoid arthritis (RA) think that pain and stiffness are just part of the daily grind, but there are moments when those signs turn into a real medical emergency. If you ever wonder whether a sudden fever, severe joint swelling, or chest discomfort means you should rush to the hospital, the answer is right hereno fluff, just what you need to know.
We'll walk through the exact symptoms that demand urgent attention, explain when a flareup can be managed at home, and give you practical tools to decide what to do next. All of this is backed by rheumatologists and the latest research, so you can feel confident about the choices you make.
Red Flag Symptoms
What Makes an RA Situation an Emergency?
In the world of RA, emergency means a symptom that could threaten your life or cause permanent damage if left untreated. Think of it as a fire alarm for your joints and organs: when it sounds, you don't waityou act fast. According to the septic arthritis complications guidance, red-flag signs include high fever, sudden swelling of a single joint, chest pain, or any neurological change.
Quick DecisionTree
| Symptom | Action |
|---|---|
| Fever >101F lasting >48hrs | Call doctor ASAP; consider ER if worsening |
| Severe joint swelling/pain (one joint) | Urgentcare call or head to ER |
| Chest pain, shortness of breath | ER immediately |
| New vision loss or facial weakness | ER immediately |
| Persistent lowgrade fever + mild flare | Contact rheumatologist; manage at home |
Classic Emergency Signs
These are the hallmarks that should set off an alarm:
- Sudden high fever (often above 101F) that doesn't come down with over-the-counter meds.
- Severe chills or night sweats that accompany the fever.
- Acute, unilateral joint swellingespecially if it's dramatically larger or more painful than your usual flare.
- Chest pain, pressure, or shortness of breath, which may signal pericarditis or a lung complication.
- Neurological changes such as sudden numbness, facial droop, or loss of coordination, pointing to possible vasculitis.
Unusual but Urgent Symptoms
RA can be a sneaky troublemaker, sometimes showing up in places you wouldn't expect. Keep an eye out for:
- Rapid, unexplained weight loss.
- Persistent rash or mouth sores.
- Sudden loss of motion in a single joint that feels locked.
- Severe, unexplained fatigue that makes daily tasks feel impossible.
If any of these accompany the classic signs, treat them as emergenciescall your doctor or head to the ER right away.
Typical Flare Symptoms
FlareUp Symptoms in the Hands
When RA flares in the hands, you'll notice swollen knuckles, stiffness that lasts more than 30 minutes, and a painful gripping sensation. It's the kind of pain that makes opening a jar feel like moving a small boulder.
Managing Hand Flares
- Apply a warm compress for 1015 minutes to loosen the joints.
- Gentle range-of-motion exercisesthink hand yogato keep the fingers mobile.
- Consider a splint at night if swelling is pronounced; it helps protect the joints while you sleep.
- If swelling exceeds 2cm or persists beyond 48hrs, give your rheumatologist a call.
FlareUp Symptoms in the Feet
Feet flares often present as sore heels, swollen toes (sometimes called sausage toes), and trouble walking. It can feel like you've stepped on a cactus hidden under a carpet.
Foot Care Tips
- Soak your feet in lukewarm water with Epsom salts for 15 minutes.
- Use orthotic inserts or supportive shoes to reduce pressure.
- Elevate your feet whenever you can to decrease swelling.
- If pain stops you from bearing weight, treat it like an emergency and head to urgent care.
FluLike RA FlareUps
Sometimes a flare masquerades as the flufever, chills, body aches, and joint pain all rolled into one. This can be confusing because infections also trigger fevers.
Here's a quick way to tell them apart: if the fever spikes above 101F and stays high for more than 48 hours, or if the joint pain is unusually intense, you're likely dealing with an RA flare that needs medical oversight. Always check your white-blood-cell count with a doctor to rule out infection.
When Flare Symptoms Stay Safe
Not every flare demands a hospital visit. Most routine flares include:
- Morning stiffness lasting less than 30 minutes.
- Low-grade fever (under 100.4F).
- Joint warmth that eases with rest and NSAIDs.
For these, a short course of steroids (under doctor guidance), rest, and the self-care steps above usually keep you comfortable until your next scheduled appointment.
Systemic Warning Signs
Signs Rheumatoid Arthritis Is Getting Worse
RA isn't just a joint issue; it's a systemic disease that can affect lungs, heart, eyes, and even the skin. Warning signs that your RA is progressing include:
- Increasing number of painful joints, especially if they become symmetrical.
- Persistent fatigue that doesn't improve with sleep.
- Dry eyes or mouthoften a sign of secondary Sjgren's syndrome.
- Shortness of breath or persistent cough, suggesting lung involvement.
- Chest discomfort, which could indicate pericarditis.
When you notice a cluster of these, schedule an appointment fastearly intervention can slow disease progression.
What Are the 4 Stages of Rheumatoid Arthritis?
| Stage | Typical Features |
|---|---|
| Stage1 Early | Synovial inflammation, mild joint pain, minimal damage on X-ray. |
| Stage2 Moderate | Increased swelling, occasional erosions, functional limitations appear. |
| Stage3 Severe | Significant joint erosion, deformities, extra-articular involvement (lungs, heart). |
| Stage4 Advanced | Severe deformities, extensive organ involvement, high disability. |
Unusual Symptoms of Rheumatoid Arthritis
Beyond the joints, RA can cause a range of surprising symptoms:
- Hearing loss or ringing in the ears.
- Skin nodules that feel like tiny hard bumps under the skin.
- Frequent headaches or migraines.
- Depression or anxietychronic pain takes a toll on mental health.
These off-target signs are real, and acknowledging them helps your care team treat the whole person, not just the joints.
Decision Guide
ImmediateCall Symptoms
If you experience any of the following, pick up the phone now:
- Fever >101F that doesn't subside.
- Sudden, intense swelling of one joint.
- Chest pain, pressure, or trouble breathing.
- New neurological signs (blurred vision, facial weakness).
HospitalNeeded Symptoms
These symptoms merit a direct trip to the emergency department:
- Uncontrolled pain that prevents you from moving.
- Swelling that becomes red, hot, and rapidly expandingsigns of possible infection.
- Persistent high fever for more than 48 hours.
- Any sign of heart involvement (chest tightness, palpitations).
WatchandWait Flare Symptoms
When symptoms are milder, you can monitor and manage them at home, but keep a close eye on any changes:
- Low-grade fever (<100.4F).
- Mild joint pain that improves with NSAIDs or rest.
- Stiffness lasting under 30 minutes.
Document these in a flare-log and share the trend with your rheumatologist at your next visit.
Printable Checklist
| Symptom | Urgency |
|---|---|
| Fever >101F | Call doctor / ER if >48hrs |
| Severe joint swelling (one joint) | ER immediately |
| Chest pain or shortness of breath | ER immediately |
| New neurological signs | ER immediately |
| Mild flare (pain, low-grade fever) | Home care, monitor |
Home Management Tips
Medication Adjustments
Never change your disease-modifying antirheumatic drug (DMARD) dosage without talking to your specialist. However, a short course of oral steroids (e.g., prednisone 1020mg daily) is often prescribed during a flare, but only under doctor supervision. Over-the-counter NSAIDs can relieve pain, but remember to protect your stomachtake them with food or a proton-pump inhibitor.
Physical SelfCare
Movement is medicine, even when your joints feel like they're on fire. Gentle stretching, water aerobics, or tai chi keep joints lubricated without adding stress. Heat therapy (warm showers, heating pads) relaxes stiff muscles, while ice packs reduce acute swelling.
Lifestyle and Support
Eating a diet rich in omega-3 fatty acidsthink salmon, walnuts, and flaxseedhas been shown to lower inflammation. Sleep hygiene matters too; aim for 79 hours of restful sleep, and consider a cool, dark bedroom to reduce nighttime stiffness.
Beyond the physical, emotional support is crucial. Joining an online RA community, chatting with a therapist, or simply sharing experiences with a trusted friend can lower stress, which in turn reduces flare frequency. According to a study in the medical literature, patients who engage in regular peer support report fewer severe flares.
Conclusion
Understanding RA emergency symptoms isn't just about avoiding a trip to the ER; it's about staying in control of a chronic condition that can suddenly become life-threatening. By recognizing red-flag signshigh fever, sudden joint swelling, chest pain, or neurological changesand knowing when a flare can be safely managed at home, you empower yourself to act quickly and wisely.
Keep the printable checklist nearby, talk openly with your rheumatologist about any new or worsening symptoms, and don't hesitate to seek urgent care when the warning bells ring. Your health is a partnership, and the more you know, the stronger that partnership becomes.
What have you experienced that surprised you about RA? Share your story in the comments or reach out to your health care teamyou're not alone on this journey.
FAQs
What are the most common RA emergency symptoms?
High fever over 101°F, sudden severe swelling of a single joint, chest pain or shortness of breath, and new neurological changes such as vision loss or facial weakness.
When should I go straight to the ER for RA issues?
If you experience uncontrolled pain, a rapidly expanding red hot joint, persistent high fever for more than 48 hours, or any sign of heart involvement, go to the emergency department immediately.
How can I tell the difference between an infection and an RA flare?
Infections usually cause a higher, sustained fever and may be accompanied by elevated white‑blood‑cell counts. An RA flare often has lower‑grade fever and joint pain that improves with rest or NSAIDs.
Can chest pain be related to rheumatoid arthritis?
Yes. RA can cause pericarditis or lung involvement, leading to chest pressure, pain, or shortness of breath. Any chest discomfort should be treated as an emergency.
What home‑care steps are safe for a mild RA flare?
Use warm compresses, gentle range‑of‑motion exercises, OTC NSAIDs with food, and ensure adequate rest. Keep a flare‑log and contact your rheumatologist if symptoms worsen or last beyond 48 hours.