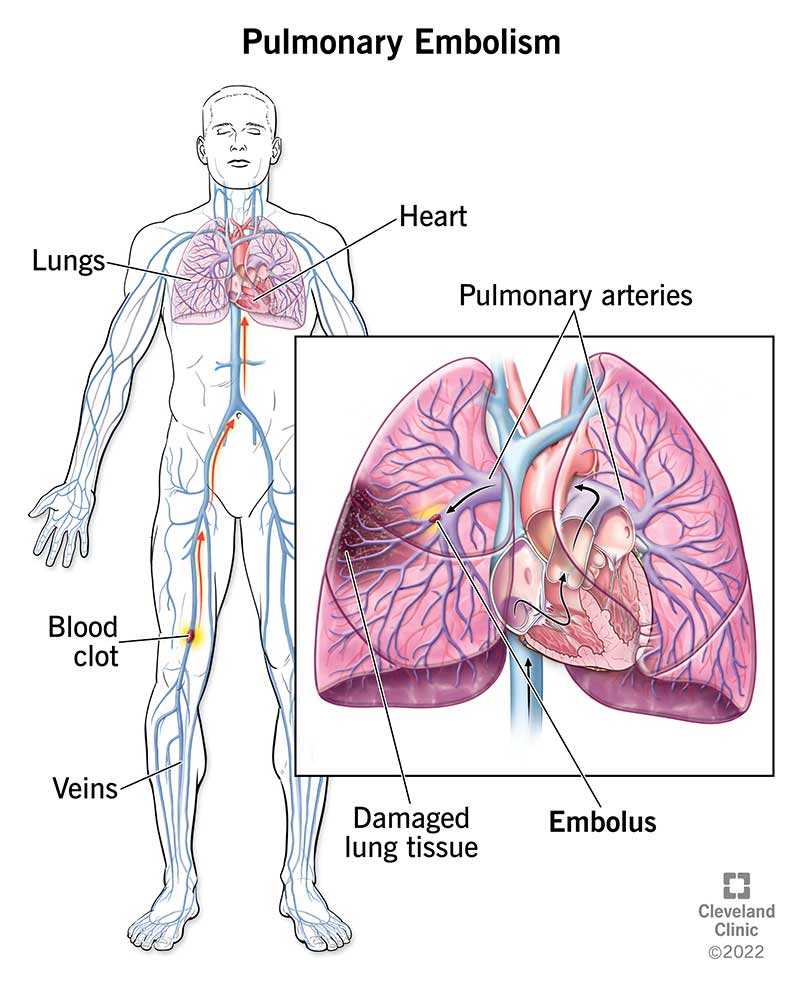
Sudden shortness of breath, a sharp chest pain that feels like a needle, and a racing heartbeatthese are the classic pulmonary embolism symptoms that demand your immediate attention. If you notice any of these signsespecially when they appear together with dizziness, coughing up bloodstreaked mucus, or an unsettling sense of doomdon't wait. Call emergency services right away.
Knowing what to look for can be the difference between a quick recovery and a lifethreatening crisis. Let's walk through everything you need to understand, from the early warning signals to treatment options, recovery timelines, and how to protect yourself in the future. For people with chronic lung conditions, such as cystic fibrosis, learning about symptom recognition and safety can be especially important; see more on cystic fibrosis safety for tailored precautions.
Why Early Detection
Ever wonder why doctors stress "time is tissue" when it comes to blood clots in the lungs? Because every minute you wait, the clot can grow, the heart works harder, and the risk of death spikes. Studies show that patients identified within the first hour of symptom onset have a survival rate over 90%, while delays beyond six hours can double mortality.
Imagine you're out for a morning jog and suddenly you can't catch your breath. That panic you feel isn't just anxietyit's your body screaming that a blockage is choking your lungs. Recognizing it early gives doctors a clear window to intervene, often with simple anticoagulants that stop the clot from getting bigger.
Common Symptoms Explained
The mystery of a pulmonary embolism lies in how its symptoms mimic everyday ailments. Below is a quickreference table that breaks down each hallmark sign, why it happens, and when you should call 911.
| Symptom | Typical Onset | Why It Happens | When to Call 911 |
|---|---|---|---|
| Sudden Shortness of Breath | MinutesHours | Clot blocks pulmonary artery, cutting oxygen flow | Any abrupt difficulty breathing |
| Sharp Chest Pain (pleuritic) | ImmediateHours | Inflamed lining of lung (pleura) rubs against clot | Pain worsens with deep breaths or coughing |
| Cough with BloodStreaked Mucus | HoursDays | Small pulmonary vessels burst under pressure | Any hemoptysis, even a few specks |
| Rapid or Irregular Heartbeat | MinutesHours | Rightventricle strain from blocked blood flow | Palpitation plus shortness of breath |
| LightHeadedness / Fainting | MinutesHours | Reduced cardiac output leads to brain hypoxia | Dizziness with chest pain or breathing trouble |
| Intense Anxiety or Feeling of Doom | Immediate | Brain senses low oxygen, triggers fightorflight | Persistent anxiety with other symptoms |
How long can you have a pulmonary embolism without knowing? In many cases, the clot can sit quietly for days or even weeks, especially if the symptoms are mild or mistaken for a flu. That's why any unexplained breathlessness deserves a professional look.
When Symptoms Overlap
It's easy to confuse a pulmonary embolism with a heart attack, panic attack, or pneumonia. Here's a quick comparison to keep you from mixing them up:
| Condition | Key Difference |
|---|---|
| Pulmonary Embolism | Sudden shortness of breath + pleuritic chest pain + possible bloodstreaked cough |
| Heart Attack | Chest pressure or heaviness, often radiating to arm/jaw; nausea and sweating common |
| Panic Attack | Rapid breathing, tingling, fear of dying, but no cough or blood in sputum |
| Pneumonia | Fever, productive cough, gradual onset over days |
Having a recent surgery, a longhaul flight, or a known clotting disorder makes the suspicion of a PE even stronger. Keep those personal risk factors frontandcenter when you're evaluating symptoms.
How Doctors Diagnose
When you walk into the ER with the above red flags, doctors have a toolbox of tests to confirm the suspicion. The first line is usually a Ddimer blood test. A normal result can rule out a clot in many lowrisk patients, while an elevated level tells the team to look deeper.
For definitive imaging, a CT pulmonary angiography (CTPA) is the gold standard. It shows the clot's exact location and size, which then guides treatment. In cases where radiation is a concern, a ventilationperfusion (V/Q) scan or a bedside ultrasound may be used instead.
Doctors also classify the clot into stages of pulmonary embolismmassive, submassive, or lowriskbased on blood pressure, heart strain, and clot burden. This staging determines how aggressive the therapy must be.
Immediate Treatment Steps
While waiting for the ambulance, there are a few things you can do to help yourself (or someone else) stay stable:
- Keep the person sitting upright; lying flat can worsen breathing.
- If you have a portable oxygen kit, use it at the highest comfortable flow.
- Stay calmpanic raises heart rate and can worsen the clot's impact.
Once in the hospital, the core pulmonary embolism treatment revolves around anticoagulation. Heparin is usually started first because it works quickly. After stabilizing, many patients switch to direct oral anticoagulants (DOACs) like apixaban or rivaroxaban, which are easier to manage at home.
In massive PE cases where blood pressure plummets, doctors may administer thrombolytics (clotbusting drugs). These carry a higher bleeding risk, so they're reserved for lifethreatening scenarios. For patients who can't receive medication, surgical embolectomy or catheterdirected therapy offers a mechanical way to remove the clot.
After the acute phase, the blood clots in lungs recovery time varies. Most people feel a marked improvement within a week, but full exercise tolerance may take 36 weeks, especially if the clot was large. Followup CT scans or ultrasound studies are scheduled to ensure the clot is dissolving and no new clots are forming.
LongTerm Outlook Guide
So, how long can you live with blood clots in your lungs? The answer depends on the clot's size and the body's response. In lowrisk PE, survival rates exceed 95% with proper anticoagulation. Massive PE raises the stakes: without treatment, mortality can reach 3050% within the first hour. That's why early intervention matters so much.
After discharge, prevention becomes the priority. Longterm anticoagulation is often prescribed for three to six months, but some highrisk patients may need indefinite therapy. Lifestyle tweaksstaying active, staying hydrated, quitting smoking, and using compression stockings after surgerygreatly reduce recurrence.
Emerging tech like home pulse oximeters and wearable heartrate monitors help patients spot early warning signs. If you notice a sudden dip in oxygen saturation (below 92%) or a rapid heartbeat while resting, give your doctor a call.
Real Stories & Tips
Emily, a 42yearold graphic designer, thought she was just dealing with a bad cold. One evening she felt an abrupt, stabbing pain in her chest and started coughing up pinktinged sputum. "I was terrified," she says, "but I remembered a friend mentioning a PE and called 911." The ER confirmed a submassive PE, and after a week of IV heparin, she switched to a DOAC and was back to painting murals within a month. Her story underscores how quickly a harmlesslooking symptom can turn serious.
Another patient, Mark, thought his mild breathlessness after a long flight was just fatigue. He ignored it for three days, and by the time he sought help, his clot had grown, leading to a nearfatal event. "If I'd listened to that little ache in my chest, I could have avoided a lot of fear," he admits. Mark's experience highlights the danger of how long can you have a pulmonary embolism without knowingthe answer can be longer than you think.
Final Thoughts & Next Steps
We've covered a lot: the telltale pulmonary embolism symptoms, how they differ from other illnesses, the diagnostic process, treatment pathways, and what to expect during recovery. The key takeaway? Trust your body's signals. If shortness of breath hits you out of the blue, if your chest feels like it's being squeezed, or if you cough up even a little blood, treat it as an emergency.
Keep a simple PE symptom checklist on your fridge or phone. Share this guide with anyone who travels long distances, recovers from surgery, or has clotting disorders. Knowledge empowers you and your loved ones to act fast, and fast action saves lives.
What's your experience with unexplained shortness of breath? Have you or someone you know navigated a pulmonary embolism? Share your story in the commentswe're all in this together.
FAQs
What are the most common pulmonary embolism symptoms?
Sudden shortness of breath, sharp pleuritic chest pain, rapid heartbeat, coughing up blood‑streaked mucus, light‑headedness, and a feeling of impending doom.
How quickly can a pulmonary embolism become life‑threatening?
Symptoms can progress within minutes; if blood pressure drops or the right ventricle fails, mortality can rise dramatically within the first hour.
Which tests are used to confirm a suspected pulmonary embolism?
Initial D‑dimer blood test, followed by imaging such as CT pulmonary angiography, ventilation‑perfusion scan, or bedside ultrasound.
What is the standard treatment for an acute pulmonary embolism?
Immediate anticoagulation with heparin, transitioning to oral anticoagulants (DOACs); severe cases may need thrombolytics, catheter‑directed therapy, or surgery.
How long does recovery typically take after a pulmonary embolism?
Most patients feel better within a week, but full return to normal activity can take 3‑6 weeks; ongoing anticoagulation may be required for 3‑6 months or longer.