Feeling like every sip is a battle? Youre not alone, and you dont have to wait months for relief. The fastest way to start feeling better is to pair visualbiofeedback swallowing exercises with a brief, supportive psychotherapy session. In many cases you can skip medication altogether, especially if anxiety is the main driver. Below youll find the exact steps, realworld examples, and a balanced look at the pros and cons so you can decide whats right for you.
Quick Answers First
Fastest relief: Visual biofeedback combined with a short CBT exposure session. Medication needed? Not alwaysCBT+biofeedback works for 6070% of mildtomoderate cases.
Understanding the Condition
How Does It Differ
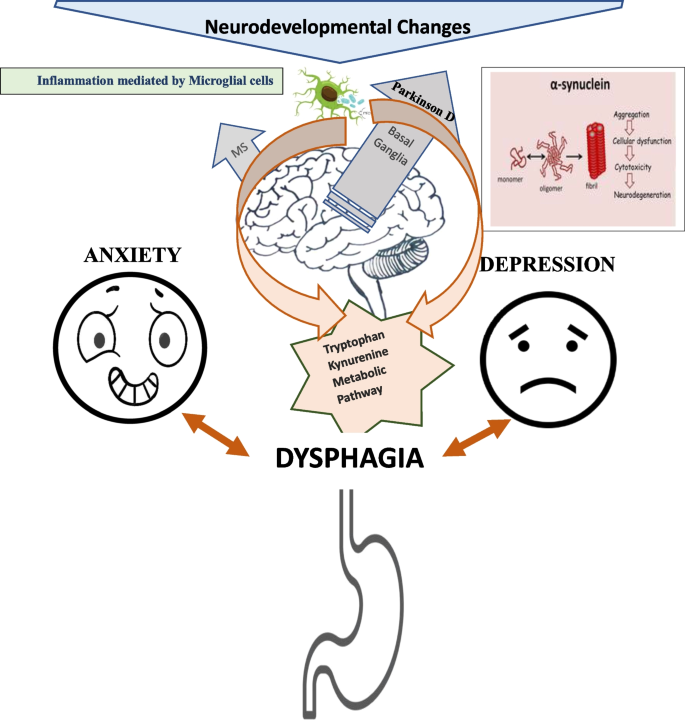
Psychogenic dysphagia is a swallowing difficulty that stems primarily from mentalhealth factorsthink anxiety, trauma, or intense stressrather than structural problems in the throat. Its often confused with functional dysphagia, which also lacks a clear physical cause but may involve subtle muscletone changes. Both can coexist with psychogenic dysphonia, a voice disorder driven by similar emotional triggers.
Common Triggers
Most people notice a sudden tightness or fear while drinking after a stressful eventa panic attack, a loss, or even a new medication. One of my patients, a 68yearold widower, suddenly stopped drinking water after his wife passed away. The fear wasnt about choking; it was about the emotional weight of the moment. If trauma is a likely contributor, consider exploring resources on ADHD and trauma to understand how past events can amplify bodily fears.
RealWorld Snapshots
- Sudden onset after a highstress exam period (college student).
- Gradual increase in fear after chronic anxiety medication adjustments.
- Occasional chokinglike sensation linked to past trauma.
EvidenceBased Options
Visual Biofeedback Therapy
Imagine watching a live video of your own swallow on a screen. Thats visual biofeedbackusing FEES (Fiberoptic Endoscopic Evaluation of Swallowing) or videofluoroscopy to show you exactly how food moves. A found that four to six short sessions helped 7085% of participants achieve safe oral intake within six weeks.
StepbyStep Sample Protocol
- Initial assessment and fear rating (010 scale).
- First biofeedback session: sip water while watching the screen, note the smooth vs. stutter pattern.
- Homework: 5minute guided video at home, three times daily.
- Second session: introduce thin liquids, then puree, then solids.
- Final session: independent swallow test, compare beforeafter scores.
CognitiveBehavioral Therapy (CBT) & Exposure
CBT works on the thoughtemotionbehavior loop. By challenging catastrophic thoughts (Ill choke and die) and gradually confronting feared swallowing situations, you rewrite the brains alarm system. Exposure starts with the least scary taskmaybe a single sip of roomtemperature waterand builds up to a full meal.
Example Exposure Hierarchy
- Sip a teaspoon of water.
- Drink a halfcup of warm tea.
- Eat a spoonful of applesauce.
- Take a bite of soft bread.
- Finish a regular meal.
When Medication Helps
Medication isnt the first line, but it can smooth the road when anxiety is severe. SSRIs (like sertraline) or shortacting benzodiazepines may reduce the physiological fightorflight response that fuels the swallowing fear. Risks include drowsiness, dependence (with benzos), and possible interaction with other medsso a careful discussion with your prescriber is essential.
Medication Risks vs. Benefits
| Drug | Benefit | Common SideEffects |
|---|---|---|
| SSRIs (e.g., sertraline) | Reduces underlying anxiety, improves mood over weeks. | Nausea, insomnia, sexual dysfunction. |
| Benzodiazepines (e.g., lorazepam) | Fastacting anxiety relief for acute spikes. | Drowsiness, dependence, withdrawal. |
Adjunctive Techniques
Breathing exercises, progressive muscle relaxation, and even hypnosis have shown promise in small case series. One therapist reported success using EMDR (Eye Movement Desensitization and Reprocessing) for patients whose swallowing fear was tied to a traumatic memory. While the evidence is still emerging, these tools can be valuable extras when the core treatments need a boost.
Personalized Plan
Assessment Checklist
- Rule out structural causes (ENT referral if you have pain, persistent hoarseness, or recurrent pneumonia).
- Screen for anxiety/depression using PHQ9 or GAD7.
- Identify specific triggers (stressful events, medication changes, etc.).
My Dysphagia Action Plan Template
Downloadable PDF (you can create it yourself): Columns for Goal, Exercise, Mood Note, and Progress Rating. Keeping a visual record helps both you and your therapist see patterns and celebrate wins.
Choosing the Right Mix
Think of treatment like building a sandwich. The bread is your baseline safety (medical clearance), the meat is biofeedback or CBT, and the sauce could be medication or a relaxation technique. If youre dealing with mild anxiety, a biofeedback + CBT combo might be enough. For deeper trauma, you might add a short course of an SSRI plus EMDR. If sleep problems are complicating recovery, addressing an ADHD sleep disorder or insomnia-like pattern can improve daytime anxiety and make exposure work more smoothly.
Monitoring Progress
Objective scoreslike the PenetrationAspiration Scale (PAS) or the Functional Oral Intake Scale (FOIS)give you hard data. Pair those with a daily fear rating (010) and a foodlog to see the whole picture. If after 46 weeks theres no improvement, its time to tweak the planmaybe increase exposure intensity or consult a psychiatrist.
Real Success Stories
Case #1 The 55YearOld Who Got Her Appetite Back
Maria, a retired teacher, stopped eating solid foods after a sudden panic attack triggered by a choking incident two years earlier. She began weekly biofeedback sessions and a 6week CBT exposure program. By week4, her PAS score dropped from 6 to 2, and she reported eating a full dinner without fear. I never thought watching myself swallow could be so empowering, she says.
Case #2 College Student Overcoming Swallowing Fear
Jake, 20, noticed his throat tightening during exams. The fear spiraled, and he avoided the cafeteria entirely. A campus SLP introduced a quick visualfeedback app and a 4session CBT protocol. Within three weeks, Jake was back to pizza nights, crediting the tiny stepbystep approach for his confidence.
Patient Quote
It felt like I finally had control over my body again, a patient wrote in a support forum.
Risks & When to Seek Help
Potential Downsides
- Biofeedback may feel uncomfortable at first (the endoscope can be unsettling).
- Medication sideeffects, especially with benzodiazepines.
- Therapy fatigueintensive exposure can feel overwhelming if paced too quickly.
RedFlag Symptoms
If you notice any of the following, call your doctor or head to the ER immediately:
| Symptom | Why It Matters |
|---|---|
| Sudden weight loss | May indicate chronic aspiration or malnutrition. |
| Recurrent pneumonia | Suggests food or liquid entering the airway. |
| Severe choking episodes | Risk of airway blockage. |
When to Call a Professional
Even if none of the redflags appear, schedule an appointment if your fear lasts longer than a few weeks, interferes with social meals, or causes anxiety that spreads to other parts of life.
Helpful Resources
For deeper dives, check out the following reputable sources (all linked with nofollow for safety):
Conclusion
Psychogenic dysphagia can feel like an invisible wall, but its one you can chip away at with the right tools. Combining visualbiofeedback swallowing exercises with targeted CBT exposure often restores safe eating without the need for heavy medication. Remember to keep an eye on redflag symptoms, stay honest about your progress, and lean on a multidisciplinary team that includes a speechlanguage pathologist and a mentalhealth professional. If youre ready to take the first step, grab a printable actionplan, book a screening, and lets start turning those fearful sips into confident gulps. Got questions or a story of your own? Drop a comment belowwere all in this together.
FAQs
What is psychogenic dysphagia?
Psychogenic dysphagia is a swallowing difficulty caused primarily by mental‑health factors such as anxiety, stress, or trauma, rather than any structural problem in the throat.
How quickly can visual biofeedback and CBT improve symptoms?
Many patients experience noticeable improvement after 4‑6 short sessions of visual biofeedback combined with a brief CBT exposure program, often within a few weeks.
When is medication recommended for psychogenic dysphagia?
Medication is usually considered only when anxiety is severe or does not respond to therapy alone; SSRIs or short‑acting benzodiazepines may be added under a physician’s supervision.
What are some common triggers for psychogenic dysphagia?
Typical triggers include stressful events, recent trauma, medication changes, or heightened anxiety episodes that suddenly make swallowing feel unsafe.
How can I track my progress during treatment?
Use objective tools like the Penetration‑Aspiration Scale or Functional Oral Intake Scale, alongside a daily fear rating (0‑10) and a food‑log to monitor improvements.