Quick answer: You can get papulopustular rosacea under control with a blend of prescription meds (oral doxycycline, macrolides, or even isotretinoin), topical creams (metronidazole, azelaic acid, ivermectin), lifestyle tweaks, andif neededlaser or lightbased therapy. Picking the right combo lets you calm flareups, shrink those stubborn bumps, and keep your skin looking as natural as possible without endless trialanderror.
Why it matters: The right treatment plan reduces redness, eases itching, and saves you from the emotional rollercoaster that comes with unpredictable breakouts. Lets dive into what works, what to avoid, and how to build a plan that feels right for you.
Understanding Papulopustular Rosacea
What is papulopustular rosacea?
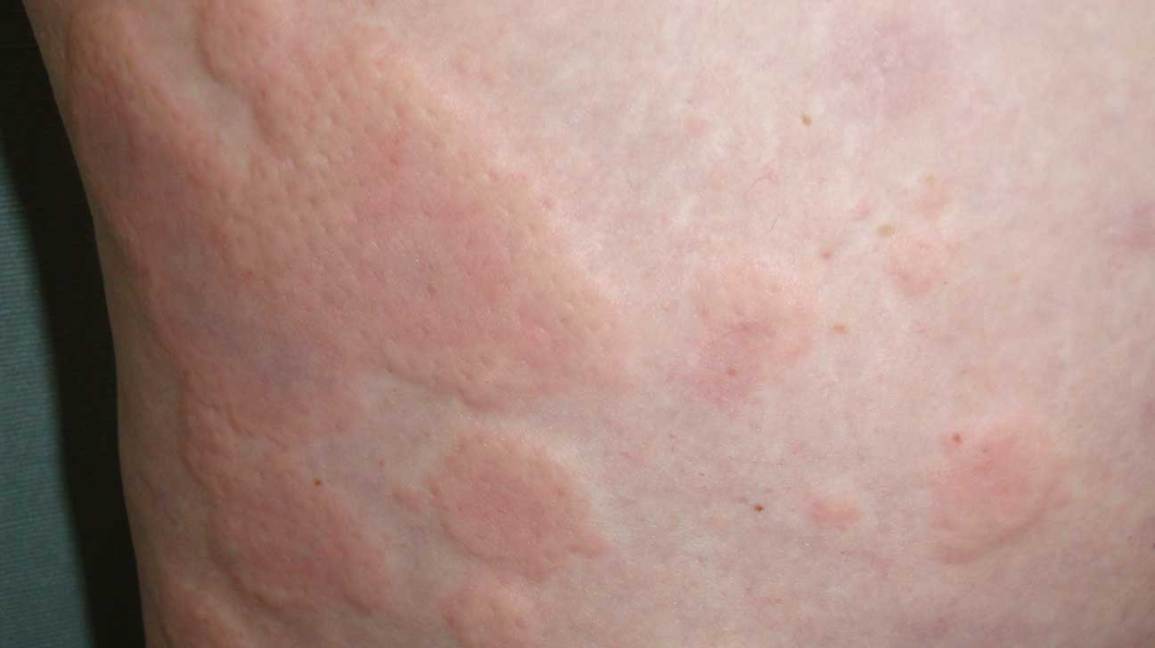
In plain English, papulopustular rosacea is the acnelike version of rosacea. Youll notice a persistent red base (erythema) dotted with painful papules (solid bumps) and pusfilled pustules. Its different from the flushing type (erythematotelangiectatic rosacea) and the thickenedskin type (phymatous rosacea). The good news? Knowing the exact subtype helps you zeroin on the treatment that actually works.
Common causes & triggers
Scientists still debate the exact cause, but heres the current thinking:
- Genetic predisposition rosacea often runs in families.
- Skinbarrier dysfunction a weak barrier allows irritants to slip in.
- Demodex mites tiny organisms that love oily skin and can inflame pores.
- Vascular dysregulation blood vessels overreact, causing redness.
- External triggers spicy food, hot drinks, alcohol, extreme temperatures, stress, and harsh skincare products.
Quick checklist Am I dealing with papulopustular rosacea?
Ask yourself:
- Do I have persistent redness with red bumps or pusfilled spots?
- Do flareups get worse after certain foods or weather?
- Is my skin sensitive to typical acne treatments?
If you answered yes to most, youre likely looking at papulopustular rosacea.
FirstLine Medical Options
Oral antibiotics the backbone of therapy
For many, a short course of oral antibiotics does the trick. The magic isnt just killing bacteria; its the antiinflammatory effect.
- Doxycycline (subantimicrobial dose) 40mg once daily. The low dose tackles inflammation without fostering antibiotic resistance. Most patients notice a calmer complexion within 24 weeks.
- Other tetracyclines (minocycline, tetracycline) useful if you cant tolerate doxycycline.
- Macrolides (azithromycin, erythromycin) a backup when tetracyclines arent an option, though they may be slightly less effective for rosacea.
Isotretinoin & other systemic options
When the standard trio (doxycycline + topical + lifestyle) falls short, dermatologists may turn to isotretinoin the same drug that transformed severe acne treatment. A low dose (0.5mg/kg) can shrink stubborn papules, but it comes with strict monitoring (liver enzymes, pregnancy tests).
Other systemic agents that occasionally pop up in research include:
- Metronidazole (oral) antiinflammatory.
- Betablockers (propranolol, carvedilol) calm vascular flareups.
- Gabapentin helps when itching is a big problem.
- Hydroxychloroquine, secukinumab, rifaximin, zinc supplements used offlabel in niche cases.
Dosage table quick reference
| Drug | Typical Dose | Duration | Key SideEffects |
|---|---|---|---|
| Doxycycline | 40mg once daily | 812 weeks (maintenance can follow) | GI upset, photosensitivity |
| Isotretinoin | 0.5mg/kg daily | 46 months | Dry lips, liver test changes, teratogenic |
| Azithromycin | 500mg once daily | 57 daysrepeat as needed | Stomach upset, QT prolongation (rare) |
According to the , combining an oral antibiotic with a topical medication gives the fastest, most sustained improvement.
Topical Skincare Solutions
Metronidazole, Azelaic Acid & Ivermectin
These three are the heavyhitters for papulopustular rosacea:
- Metronidazole 0.75% antiinflammatory, wellstudied, safe for longterm use.
- Azelaic Acid 15% reduces redness, lightens postinflammatory hyperpigmentation, and unclogs pores.
- Ivermectin 1% targets Demodex mites while calming inflammation; excellent for patients who notice miterelated flareups.
Other topicals worth knowing
- Brimonidine 0.33% and Oxymetazoline 1% vasoconstrictors that give an instant rednessmasking effect for special occasions.
- Combination formulas (e.g., metronidazole + azelaic) can simplify the routine and improve adherence.
Sidebyside comparison chart
| Product | Mechanism | Strengths | Common Irritation |
|---|---|---|---|
| Metronidazole 0.75% | Antiinflammatory | Extensive safety data, works long term | Mild stinging |
| Azelaic Acid 15% | Keratolytic + antiinflammatory | Helps with pigment & bumps | Burning in sensitive skin |
| Ivermectin 1% | Demodex mite control | Fast relief for mitedriven flareups | Rare itching |
Laser & Procedural Care
When to consider laser or light therapy?
If youve been consistent with meds and still see persistent redness, visible telangiectasia (spider veins), or papules that just dont budge, it might be time to explore procedural options. Think of laser treatment as the finetuning stage after youve already set the foundation with meds.
Types of lasers & IPL that work
- Pulsed Dye Laser (PDL) gold standard for flushing redness; targets blood vessels without harming surrounding skin.
- Nd:YAG Laser penetrates deeper, good for larger vessels.
- Intense Pulsed Light (IPL) broadspectrum light that can address both redness and pigmentation in one go.
What to expect treatment timeline & aftercare
Most clinicians recommend 35 sessions spaced 46 weeks apart. After each session, youll notice a mild pinkness that fades within a few days. Postprocedure care is simple but crucial:
- Apply a gentle, fragrancefree moisturizer.
- Use a broadspectrum SPF30+ every morning (physical sunscreens are best).
- Avoid hot tubs, saunas, and harsh exfoliants for at least a week.
According to a review in , laser and IPL can reduce persistent flushing by up to 70% when combined with a maintenance topical regimen.
OTC & Natural Remedies
OTC options that actually help
Not everything has to be prescriptiononly. Some overthecounter (OTC) products can complement your regimen:
- Sulfurcontaining creams antibacterial and mildly keratolytic.
- Niacinamide serums strengthen the barrier and reduce redness.
- Zinc oxide moisturizers soothe irritation and provide a protective layer.
Natural/DIY remedies myths vs. evidence
Everyone loves a good kitchen cure, but lets separate fact from folklore:
- Tea tree oil has some Demodexkilling properties in lab studies, yet skin irritation is common. Use only a diluted 0.5% solution.
- Aloe vera gel soothing, but it wont clear papules on its own.
- Honey masks antimicrobial, good for shortterm calm but not a standalone treatment.
Sample doanddont checklist for OTC & natural care
| Do | Dont |
|---|---|
| Use a fragrancefree, nonsoap cleanser twice daily. | Scrub aggressively it damages the barrier. |
| Apply a sunscreen (SPF30+) every morning. | Skip moisturizer dryness can trigger flareups. |
| Try lowdose zinc supplements if your doctor approves. | Rely only on home remedies for severe disease. |
Diet & Lifestyle Hacks
Papulopustular rosacea diet foods to watch
While no single diet cures rosacea, many people notice a clear link between certain foods and flareups. Consider a trial period where you eliminate the following for two weeks and monitor your skin:
- Spicy foods (chili, hot sauce)
- Hot beverages (coffee, tea) especially if served piping hot.
- Alcohol, particularly red wine.
- Histaminerich foods (aged cheese, cured meats, fermented products).
If your skin improves, reintroduce items one at a time to pinpoint the trigger.
Skincare routine for calm skin
- Cleanse with a gentle, pHbalanced cleanser (e.g., Cetaphil Gentle Skin Cleanser).
- Moisturize with a ceramiderich cream containing niacinamide.
- Protect using a mineral sunscreen (zinc oxide or titanium dioxide).
- Treat with your prescription or OTC topical as directed.
7day RosaceaFriendly meal plan (sample)
| Day | Breakfast | Lunch | Dinner | Snack |
|---|---|---|---|---|
| Monday | Oatmeal with blueberries & almond milk | Grilled chicken salad (mixed greens, cucumber, olive oil) | Steamed salmon, quinoa, roasted carrots | Apple slices with almond butter |
| Tuesday | Greek yogurt (plain) with honey drizzle | Quinoa bowl with roasted zucchini, chickpeas, tahini | Turkey meatballs, brown rice, steamed broccoli | Carrot sticks |
| Wednesday | Smoothie (spinach, banana, oat milk) | Lentil soup, side of wholegrain bread | Grilled shrimp, sweet potato mash, green beans | Handful of walnuts |
Building Your Personal Plan
Stepbystep decision tree (describe the flow)
Imagine youre standing at a crossroads. Heres a simple mental map to guide you:
- Assess severity Mild (mostly redness) topical + OTC. Moderate (papules + some redness) add oral antibiotic. Severe (persistent bumps, visible telangiectasia) consider isotretinoin or laser.
- Identify triggers Keep a skin diary for two weeks, note foods, weather, stress, products.
- Start treatment Pick one oral (e.g., doxycycline) and one topical (e.g., metronidazole). Use consistently for at least four weeks.
- Reevaluate After 46 weeks, check improvement. If >50% better, continue; if not, discuss alternatives with your dermatologist.
- Consider procedural boost If redness persists, ask about PDL or IPL.
Sample starter kit for beginners
- Prescription: Doxycycline 40mg (once daily, prescribed by dermatologist).
- Topical: Metronidazole 0.75% cream (apply twice daily).
- Cleanser: Gentle, fragrancefree option (e.g., Cetaphil).
- Moisturizer: Ceramide + niacinamide blend.
- Sunscreen: Mineral SPF50+ (zinc oxide).
Remember: always discuss any new supplement or OTC product with your healthcare provider before adding it to your routine.
Conclusion
Effective papulopustular rosacea treatment rests on three pillars: targeted medication (topical+oral), smart lifestyle choices, and, when needed, procedural care. By understanding the underlying triggers, selecting the right combination of proven therapies, and staying consistent with a gentle skincare routine, you can calm flareups and reclaim confidence in your skin. Every face is unique, so work closely with a boardcertified dermatologist to tailor a plan that feels safe, realistic, and sustainable. Ready to start your clearskin journey? Dive into one of the steps above, keep a diary of what works, and rememberyoure not alone in this. Feel free to share your experiences or ask questions; were all in this together.
FAQs
What is papulopustular rosacea?
Papulopustular rosacea is the acne-like version of rosacea, featuring persistent redness with painful papules and pus-filled pustules, distinct from flushing or thickened skin types.[1]
What are the first-line treatments for papulopustular rosacea?
First-line treatments include topical metronidazole 0.75%, azelaic acid 15%, ivermectin 1%, and oral doxycycline at a subantimicrobial 40mg dose for inflammation control.[2][7]
Can laser therapy help with papulopustular rosacea?
Laser therapies like pulsed dye laser (PDL), Nd:YAG, or IPL target persistent redness and blood vessels after medical treatments, often reducing flushing by up to 70% with maintenance.[1]
What lifestyle changes help manage papulopustular rosacea?
Avoid triggers like spicy foods, alcohol, hot drinks, stress, and harsh products; use gentle cleansers, moisturizers, and mineral SPF30+ sunscreen daily.[3][9]
When is isotretinoin used for papulopustular rosacea?
Isotretinoin at low doses (0.5mg/kg) is for severe, refractory cases unresponsive to antibiotics and topicals, requiring monitoring for side effects like dry skin and liver changes.[2][8]