Most people think pain is just a random ouch. In reality its a pinpointed alarm system, shouting that something in your body needs attention. Below youll discover the 7 most common pain causes, how they differ, what symptoms to watch for, and when its time to call a professional all laid out in a friendly, chatlike style.
Quick Look
What is pain, really?
Pain is the brains interpretation of signals from special nerve fibers called nociceptors. When tissue is damaged or a nerve is irritated, these fibers fire, and the brain translates the electrical storm into the sensation we call pain. According to the National Institute of Neurological Disorders and Stroke, pain exists to protect us, but it can become a problem when the signal sticks around longer than needed.
Why do we need to know the cause?
Understanding the exact pain cause lets you treat the problem at its root, not just mask the feeling. Targeted treatment speeds recovery, reduces medication reliance, and prevents the pain from turning chronic. Ignoring the cause, on the other hand, can lead to worsening injury, prolonged disability, and even mentalhealth strain. For example, managing chronic inflammatory conditions like those that meet ankylosing spondylitis remission criteria requires careful handling to reduce ongoing pain.
How many paincausing categories exist?
Broadly, pain falls into two families:
- Nociceptive pain triggered by actual tissue damage (think sprains or burns).
- Neuropathic pain caused by nerve dysfunction, often described as burning, tingling, or electricshocklike.
Both categories can coexist, and many of the 7 causes of pain well explore sit somewhere in between.
Common Causes
1. Strained or overused muscles
Ever feel a tight knot after a long day at the desk or after an intense workout? Thats classic muscle strain. Repetitive motions, poor posture, or a sudden increase in activity overload the muscle fibers, prompting nociceptors to fire. The notes that the pain is usually localized, worsens with movement, and eases with rest or gentle stretching.
Quick selfcheck
- Did the pain start after a specific activity?
- Is it tender to touch?
- Does heat, massage, or light movement provide relief?
2. Acute injuries (cuts, fractures, burns)
When you accidentally cut your finger or break a bone, the bodys alarm system goes into overdrive. Tissue disruption releases chemicals like prostaglandins that sensitize nociceptors, creating sharp, immediate pain. If the injury is severe (deep cut, obvious deformity, or uncontrolled bleeding), head straight to the ER; otherwise, clean the wound, apply a cold compress, and keep the area immobilized.
3. Dental work & oral infections
A throbbing tooth isnt just a nuisanceits a sign that nerves inside the tooth or surrounding gums are irritated. Common culprits include cavities, abscesses, or recent dental procedures. The pain often radiates to the jaw or head, making it feel like a facial migraine. NINDS explains that untreated oral infections can spread, so prompt dental care is key.
4. Surgical procedures & childbirth
Postoperative pain is expected; its the bodys way of protecting healing tissues. The intensity usually peaks within the first 2448hours and then gradually drops. Childbirth pain follows a similar pattern, driven by uterine contractions and tissue stretching. Managing this pain with prescribed medication, gentle movement, and supportive breathing techniques helps prevent chronic pain development.
5. Infections (viral, bacterial, fungal)
When a pathogen invades, the immune system releases inflammatory mediators that sensitize nerves. Think of the deep ache you get with flu, the sharp pang of a urinary tract infection, or the burning of a fungal toe. If pain is accompanied by fever, swelling, or redness, its a red flagseek medical attention promptly.
6. Chronic inflammatory conditions
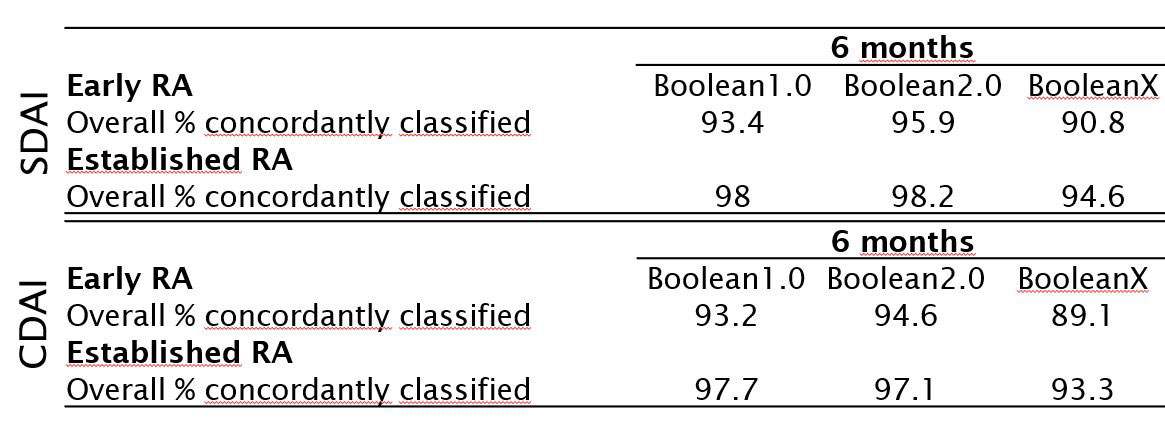
Arthritis, inflammatory bowel disease, and lupus fall into this group. Persistent inflammation keeps nociceptors activated, resulting in a dull, constant ache that can ebb and flow. Lifestyle tweaks (diet, gentle exercise), antiinflammatory meds, and regular monitoring with a rheumatologist are the usual game plan. For those dealing with conditions like ankylosing spondylitis, knowing the ankylosing spondylitis criteria can guide effective symptom management.
7. Neuropathic pain (nerve damage)
When nerves themselves are injuredby diabetes, shingles (postherpetic neuralgia), or a pinched spinal discthe pain can feel like burning, tingling, or electric shocks. This is the what causes pain in the body scenario that isnt tied to visible injury. According to the CDC, neuropathic pain often requires medications that target nerve pathways, such as gabapentin or duloxetine, rather than standard painkillers.
Pain Types
What are the 12 types of pain?
Medical literature often lists twelve distinct pain sensations. Below is a quick snapshot:
| Type | Description | Typical Cause |
|---|---|---|
| Sharp | Quick, piercing sensation | Acute injury, cuts |
| Dull | Heavy, gnawing ache | Muscle strain, arthritis |
| Throbbing | Pulsating, rhythmic | Headaches, migraines |
| Burning | Hot, stingy feeling | Neuropathy, shingles |
| Stabbing | Sudden, knifelike | Kidney stones, nerve impingement |
| Cramping | Muscle tightenandrelease | Menstrual pain, spasms |
| Pressure | Heavy weight sensation | Inflammation, organ swelling |
| Radiating | Spreads outward from a point | Herniated disc, sciatica |
| Electric | Shocklike jolts | Neuropathic pain, multiple sclerosis |
| Gnawing | Persistent, nagging ache | Chronic inflammation |
| Cold | Icelike sensation | Raynauds, some neuropathies |
| Floating | Diffuse, vague discomfort | Functional pain syndromes |
Nociceptive vs. Neuropathic vs. Psychogenic pain
Heres a sidebyside look at the three major families:
| Aspect | Nociceptive | Neuropathic | Psychogenic |
|---|---|---|---|
| Cause | Actual tissue damage | Nerve injury or dysfunction | Emotional/psychological factors |
| Typical Sensation | Sharp, throbbing, aching | Burning, tingling, electric | Diffuse, variable |
| Common Conditions | Sprains, fractures, dental pain | Diabetic neuropathy, shingles | Somatic symptom disorder |
| FirstLine Treatment | Rest, NSAIDs, physical therapy | Gabapentinoids, SNRIs, nerve blocks | Cognitivebehavioral therapy |
Symptoms & Risks
How do I know if pain is extreme?
Medical professionals often use a 010 visual analog scale (VAS). Scores of 710 usually signal severe or extreme pain, especially when it interferes with sleep, appetite, or daily tasks. Redflag symptomssudden loss of function, night pain that wakes you, or pain that spreads rapidlyshould prompt an urgent medical visit.
What are the hallmark symptoms of each pain type?
- Sharp: Sudden onset, usually linked to a clear injury.
- Dull/aching: Persistent, lowgrade, often from inflammation.
- Burning: Indicates nerve involvement; common in neuropathy.
- Radiating: Pain travels along a nerve path (e.g., sciatica).
- Electric: Short, jolting bursts, typical of multiple sclerosis or pinched nerves.
Effects of pain on the body (shortterm & longterm)
Acute pain triggers the fightorflight response, releasing cortisol and adrenaline. This shortterm boost can protect you from further injury. However, chronic pain keeps the stress system on high gear, leading to sleep disturbances, mood swings, weakened immunity, and even cardiovascular strainsomething highlighted in an NIH study.
Finding the Source
Should I do a selfcheck first?
Yes! A quick fivestep selfassessment can guide you toward the right help:
- Location: Where exactly does it hurt?
- Onset: When did it start? Sudden or gradual?
- Triggers: What makes it worse or better?
- Quality: Sharp, dull, burning, etc.
- Relief: Does heat, rest, or medication help?
When is imaging needed?
If the pain is severe, persists beyond a few weeks, or is accompanied by neurological deficits (numbness, weakness), imaging can clarify the cause. Xrays are great for bone injuries, MRIs reveal softtissue and nerve issues, while EMG studies assess nerve electrical activity.
What questions should I ask my doctor?
- Is my pain nociceptive, neuropathic, or a mix?
- What tests do you recommend and why?
- What are the shortterm and longterm treatment options?
- Are there lifestyle changes that could reduce my pain?
- When should I return for a followup?
Tools & apps for tracking pain
Many people find that a simple pain diarywhether a notebook or a smartphone apphelps spot patterns. Apps like PainScale or MyPainTracker let you log intensity, type, and triggers, creating a visual timeline you can share with your clinician.
Balanced Takeaway
Benefits of identifying the cause
When you know the exact pain cause, treatment becomes precisewhether thats a targeted stretch, a nervespecific medication, or a lifestyle tweak. Youll likely recover faster, use fewer pills, and lower the odds of pain becoming chronic.
Risks of misdiagnosis or selftreatment
Trying to just live with it or relying on generic overthecounter meds can mask symptoms while the underlying issue worsens. In worstcase scenarios, untreated infections spread, fractures heal improperly, or neuropathic pain spirals into debilitating chronic pain.
How to stay informed without selfdiagnosing
Stick to reputable sourcesNIH, Mayo Clinic, Cleveland Clinic, and peerreviewed journals. Use the information as a conversation starter with your healthcare provider, not as a final verdict. Remember, youre the expert on how you feel; your doctor is the expert on whats happening inside.
Conclusion
Understanding pain causes is the first step toward turning ouch into Im on the road to feeling better. Whether its a strained muscle, an infection, or a nerve glitch, spotting the exact trigger lets you take smart, targeted action. Keep a simple pain diary, watch for redflag symptoms, and dont hesitate to seek professional help when you need it. Got a story about a strange pain you figured out? Share it in the commentsyour experience could be the clue someone else needs!
FAQs
What are the most common causes of muscle pain?
Typical culprits include strained or over‑used muscles from repetitive motions, poor posture, sudden increases in activity, and minor injuries like pulls or tears.
How can I tell if my pain is neuropathic rather than nociceptive?
Neuropathic pain often feels burning, tingling, or electric‑shock‑like and may occur without an obvious injury. Nociceptive pain is usually sharp, throbbing, or aching and linked to tissue damage.
When should I seek medical help for sudden sharp pain?
Seek immediate care if the pain follows a serious injury (deep cut, obvious deformity, uncontrolled bleeding), if you notice swelling, numbness, loss of function, or if the pain is severe and doesn’t improve with basic first‑aid measures.
What home treatments work best for minor strains and over‑use injuries?
Rest the affected area, apply ice for the first 24‑48 hours, gentle compression, and elevation. After swelling subsides, light stretching, heat, and over‑the‑counter NSAIDs can help relieve discomfort.
Can keeping a pain diary really help in diagnosing the cause?
Yes. Recording pain intensity, location, triggers, and relief methods creates a clear pattern that you can share with a healthcare professional, making diagnosis and treatment planning much more accurate.