Did you know that a joint infection can become a lifethreatening emergency in just a few days? Bottom line: if septic arthritis isnt treated fast, it can destroy cartilage, spread infection to other organs, andyeseven in otherwise healthy adultslead to permanent disability or death. Lets walk through what this looks like, why it matters, and how you can stay safe.
Quick Overview Guide
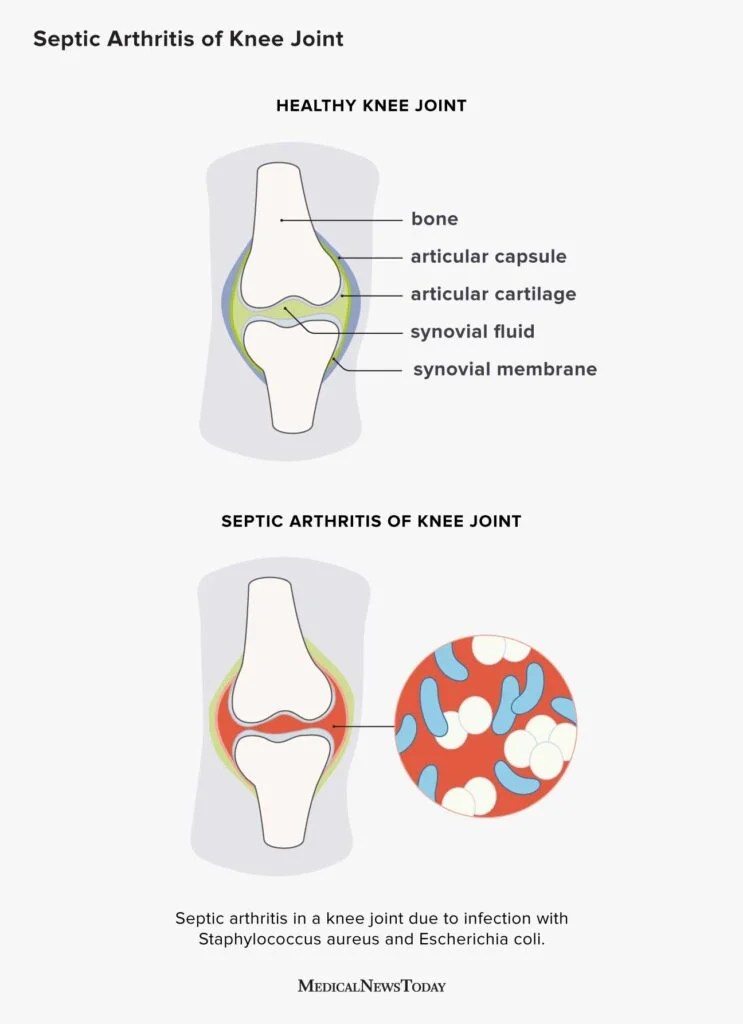
Septic arthritis is an infection inside a joint that usually arrives suddenly, with intense pain, swelling, and fever. While many people think its just a sore knee, the complications of septic arthritis can be far more serious, ranging from irreversible joint damage to systemic sepsis. For patients with underlying conditions like inflammatory spine disease, recognizing early signs is especially important similar vigilance is used when monitoring for spine inflammation.
What are the main complications?
In a nutshell, the biggest risks are:
- Cartilage destruction leading to osteoarthritis.
- Osteomyelitis (bone infection) attached to the joint.
- Sepsis and septic shockpotentially fatal.
- Chronic pain, loss of rangeofmotion, and the need for joint replacement later on.
Fasttrack list of common complications
- Joint destruction
- Osteomyelitis
- Sepsis
- Renal or cardiac failure
- Longterm disability
Common Causes & Risks
What triggers septic arthritis?
Most often a bacterial invader slips into the joint after a cut, surgery, or via the bloodstream. The usual suspects are Staphylococcus aureus (about 4050% of adult cases), Streptococcus species, and Gramnegative rods.
What is the most common cause of septic arthritis?
According to the , Staphylococcus aureus reigns supreme as the leading pathogen in both children and adults.
Whos at higher risk?
Age over 65, diabetes, immune suppression (think chemo or steroids), intravenous drug use, recent joint surgery, or having a prosthetic joint all raise the odds of both infection and its complications.
Pathogen vs. Complication Rate
| Pathogen | Typical Complication Rate |
|---|---|
| Staphylococcus aureus | 3040% joint destruction |
| Streptococcus spp. | 2030% osteomyelitis |
| Gramnegative rods | 1525% sepsis |
Key Warning Signs
Which symptoms scream complication in the making?
Besides the classic triadpain, swelling, and feverwatch for rapid loss of joint function, a spreading rash, confusion, or a sudden drop in blood pressure. Those are redflag signals that the infection may be marching beyond the joint.
Can septic arthritis kill you?
Unfortunately, yes. If the infection spirals into sepsis, mortality can climb to 515% in highrisk groups. Early antibiotics and drainage are the only lifesavers.
Types of Complications
JointSpecific Complications
When the infection gnaws at cartilage, the joint can grind down to bone. This leads to earlyonset osteoarthritis, permanent stiffness, and the dreaded need for joint replacement years later.
Case snapshot
Imagine a 12yearold who suffered a knee infection after a sports injury. The infection reached the growth plate, causing a leglength discrepancy that required corrective surgery when they hit puberty. (A study in describes a similar scenario.)
Systemic Complications
The infection doesnt stay sealed inside the joint. Bacteria can leak into the bloodstream, causing sepsis, which may trigger organ failurekidneys, lungs, or heart. Elderly patients with diabetes are especially vulnerable.
Risk chart by age group
| Age Group | Sepsis Risk | Renal Failure Risk |
|---|---|---|
| 018 | 5% | 2% |
| 1964 | 10% | 5% |
| 65+ | 20% | 12% |
LongTerm Effects
Even after the infection clears, many patients endure chronic pain, reduced mobility, and a higher chance of needing a joint prosthesis. A review in notes that up to 30% of survivors report lasting joint problems.
Early Diagnosis Steps
How do doctors spot complications early?
Imaging and lab work are the detectives best friends. Xrays reveal bone erosion, while MRI can show hidden cartilage loss. Blood tests (CRP, ESR) flag inflammation, and synovial fluid analysis confirms the offending bug.
What tests matter most?
- Synovial fluid Gram stain & culture: Gold standard for identifying the pathogen.
- CRP & ESR: Quick indicators of systemic inflammation.
- MRI: Detects early cartilage damage before Xray shows it.
Patient checklist
If you notice any of these, ask your doctor:
- Did we get a synovial fluid sample?
- Are blood cultures being done?
- Is an MRI scheduled to look for hidden damage?
Current Treatment Guidelines
What does the latest guidance say?
The Infectious Diseases Society of America (IDSA) and the American Academy of Orthopaedic Surgeons (AAOS) recommend starting intravenous antibiotics within 24 hours of diagnosis, followed by surgical drainage when needed.
Which antibiotics work?
Empiric therapy often starts with nafcillin or cefazolin for suspected S. aureus, then adjusts based on culture results. For MRSA, vancomycin is the goto.
When is surgery required?
If the joint is tense, the fluid is thick, or imaging shows pus pockets, an orthopaedic surgeon will perform arthroscopic or open drainage. Early drainage reduces the odds of cartilage loss dramatically.
Decisiontree graphic (for reference)
Imagine a simple flowchart: Symptoms Lab tests Imaging Antibiotics Drainage (if needed) Rehab.
Preventing Future Complications
How can you lower the risk?
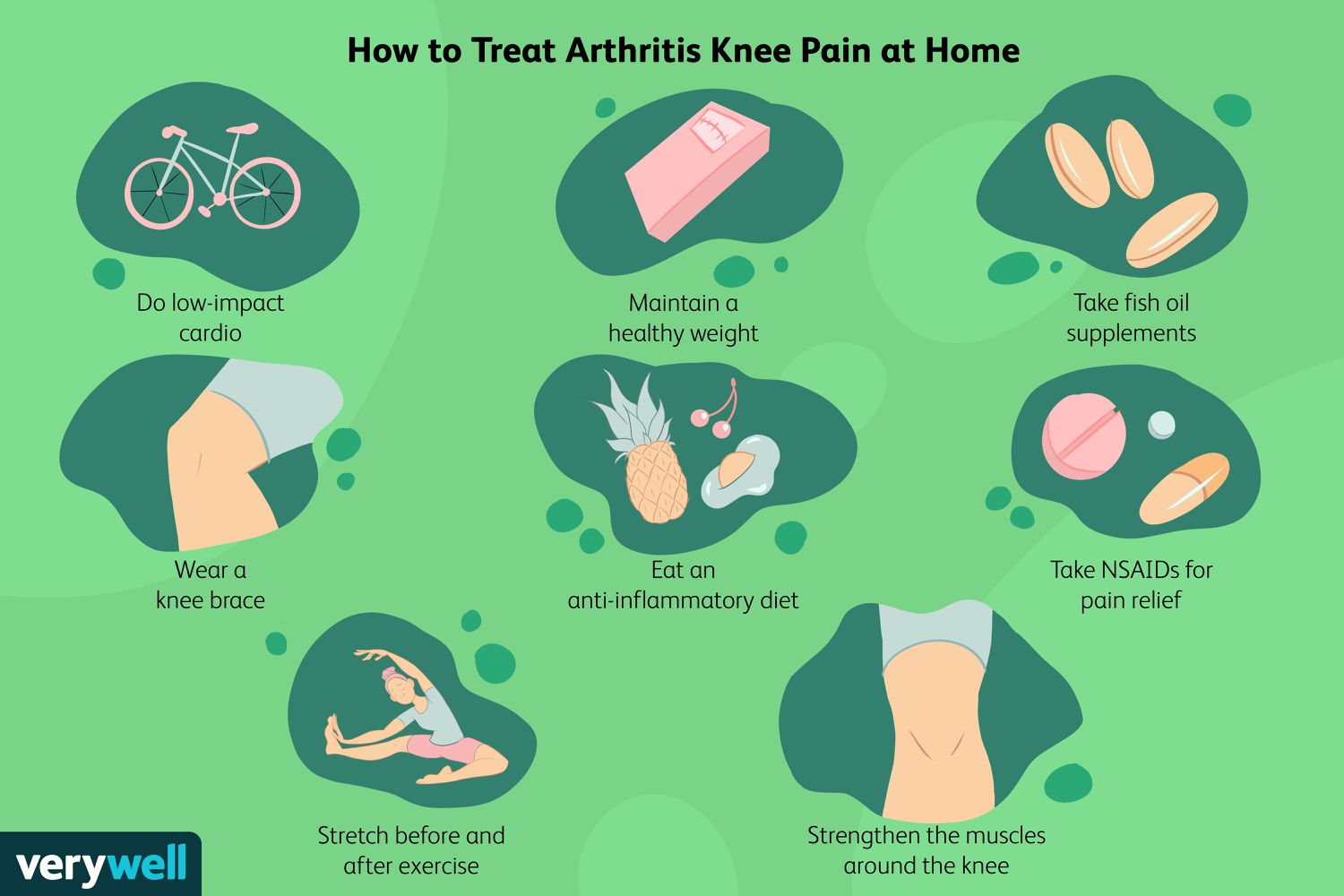
Speed is the name of the game. At the first sign of joint pain with fever, seek medical care right away. Managing chronic conditions (like diabetes) and practicing good wound hygiene after surgeries also help. Patients recovering from joint infection often benefit from coordinated care that includes assessment for conditions affecting mobility and bone health, such as osteoporosis rehab, when appropriate.
Posttreatment care matters
Even after the infection clears, a structured physiotherapy program restores motion and strengthens surrounding muscles, decreasing the chance of longterm stiffness.
Top5 DoandDont List
- Do: Keep wounds clean and covered.
- Dont: Ignore a fever that follows a joint injury.
- Do: Follow the full antibiotic courseeven if you feel better.
- Dont: Skip followup Xrays after treatment.
- Do: Engage in gentle rangeofmotion exercises as advised.
Common Questions Answered
Can septic arthritis kill you?
Yes. Untreated infection can progress to sepsis, which is lifethreatening. Early antibiotics and drainage are critical to survival.
What is the most common cause?
Staphylococcus aureus dominates, responsible for roughly half of adult cases.
What are the longterm effects?
Persistent joint pain, reduced mobility, early osteoarthritis, and sometimes the need for joint replacement.
How are complications treated?
Prompt intravenous antibiotics, surgical drainage if indicated, and a tailored rehab plan to preserve joint function.
Who is most at risk?
Elderly individuals, those with weakened immune systems, diabetics, IV drug users, and anyone with a prosthetic joint.
Patient Stories Shared
Emilys experience
Emily, a 34yearold marathon runner, thought a swollen knee was just overtraining. Within 48hours, she developed a fever. A quick ER visit led to a joint tap that grew S. aureus. She received IV antibiotics and arthroscopic drainage. Thanks to the early action, she avoided permanent damage and returned to running after six months of rehab.
Dr. Patels perspective
The difference between a good outcome and permanent disability is often a matter of hours, says orthopaedic surgeon Dr. Raj Patel. When septic arthritis is caught early, we can save the joint. Delays, even by a day, raise the odds of cartilage loss dramatically.
Conclusion
Understanding the complications of septic arthritis isnt just academicits a lifesaver. The infection can rapidly turn from a painful joint into a systemic threat, but with early recognition, aggressive treatment, and diligent followup, most people avoid lasting harm. If you ever feel sudden joint pain accompanied by fever, dont waitreach out to a healthcare professional right away. Your joints (and possibly your whole body) will thank you.
Whats your experience with joint infections? Have you or someone you know faced septic arthritis? Share your story in the commentsyour insight could help another reader act sooner.
FAQs
What are the most common complications of septic arthritis?
The most common complications include joint destruction, osteomyelitis, sepsis, chronic pain, and long-term disability.
Can septic arthritis lead to sepsis?
Yes, if left untreated, septic arthritis can spread infection into the bloodstream, causing sepsis, a life-threatening condition.
Is joint damage from septic arthritis permanent?
Without prompt treatment, septic arthritis can cause irreversible cartilage and joint damage, leading to chronic pain and reduced mobility.
What increases the risk of complications from septic arthritis?
Risk factors include delayed treatment, older age, diabetes, immune suppression, and infection with aggressive bacteria like Staphylococcus aureus.
How are complications of septic arthritis treated?
Treatment involves antibiotics, surgical drainage if needed, and physical therapy to restore joint function and prevent long-term disability.