Imagine feeling constantly exhausted, waking up with joint pain that feels like youve run a marathon, and seeing a mysterious rash on your face. You finally see a doctor, and the words lupus land on the table. Its scary, right? The good news is that with the right treatment plan you can still live a full, active life. Below youll find straighttothepoint answers and a friendly guide that will help you understand the most effective lupus treatment options, their benefits and risks, and how to make the best choices for your own health.
Quick Start Answers
What is the most effective treatment for lupus?
The backbone of most successful regimens is hydroxychloroquine (Plaquenil). It helps control skin rashes, joint pain, and protects the kidneys. In many cases its combined with a personalized steroid taper or an immunosuppressive medication when organ involvement is present. Newer biologics such as belimumab or anifrolumab are added for patients whose disease doesnt respond to the basics.
Can lupus kill you?
Modern medicine has turned lupus from a potentially lifethreatening disease into a manageable chronic condition for most people. The danger comes when the disease attacks vital organsespecially the kidneys, heart, or lungsand treatment isnt started early enough. Timely, appropriate therapy dramatically reduces mortality risk.
Lupus Overview Basics
What causes lupus?
Lupus is an autoimmune disorder, meaning your immune system mistakenly attacks healthy tissue. Genetics play a rolecertain gene patterns run in familiesbut hormones, especially estrogen, and environmental triggers like sunlight, infections, or certain medications can set it off. Think of it as a perfect storm where multiple factors collide.
Early signs of lupus in females
Women are three times more likely to develop lupus, and the early clues often appear between the ages of 15 and 45. Common signs include:
- Extreme fatigue that doesnt improve with rest
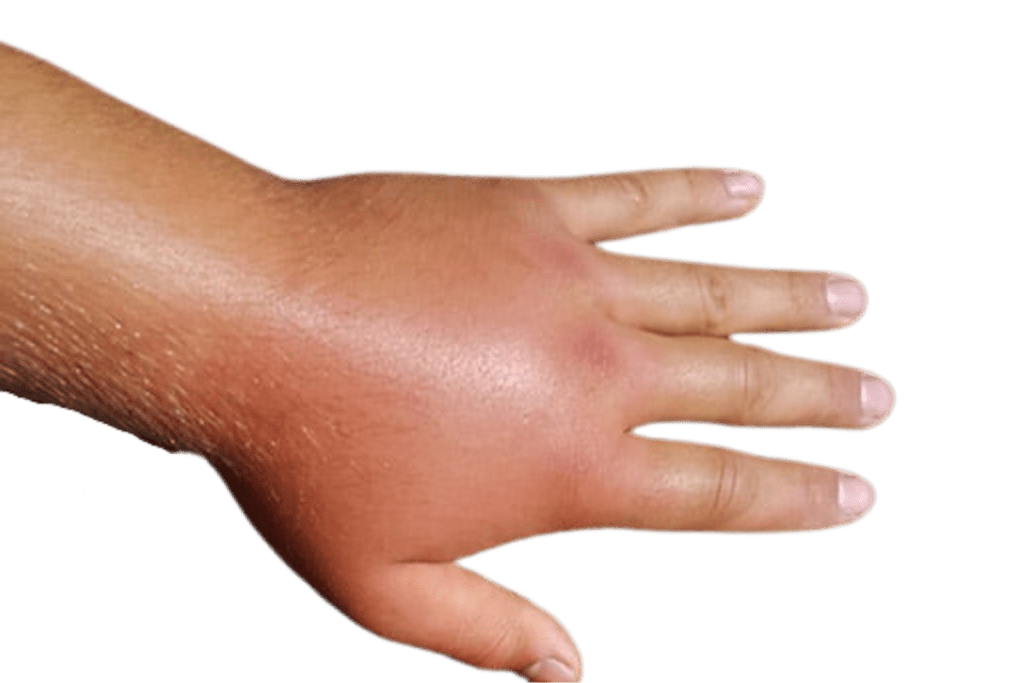
- Joint pain or swelling, especially in the hands and wrists
- A butterfly rash across the cheeks and nose
- Fever without an obvious infection
- Sensitivity to sunlight (photosensitivity)
If you notice a combination of these symptoms, a visit to a rheumatologist is worth considering.
How is lupus diagnosed?
Diagnosis is a mix of clinical observation and lab tests. Doctors look for at least four of the 11 criteria set by the American College of Rheumatology, which include the symptoms above plus blood work showing antinuclear antibodies (ANA) and specific antibodies like antidsDNA. An ultrasound or kidney biopsy may be ordered if organ involvement is suspected.
Realworld example
Anna, a 27yearold graphic designer, first thought her facial rash was a reaction to a new cleanser. After months of fatigue and joint aches, a rheumatologist ran an ANA test that came back positive. With a diagnosis of systemic lupus erythematosus, she started hydroxychloroquine and saw her flareups drop dramatically within three months.
Main Treatment Options
Medication lineup
| Medication | What it does | Typical dose | Major benefit | Key risk / sideeffect |
|---|---|---|---|---|
| Hydroxychloroquine (Plaquenil) | Reduces flares, protects skin & kidneys | 200400mg daily | Proven longterm survival benefit | Retinal toxicity eye exam yearly |
| Corticosteroids (Prednisone) | Fast antiinflammatory | 530mg daily (taper) | Quick symptom control | Weight gain, bone loss, glucose spikes |
| Immunomodulators (Mycophenolate, Azathioprine) | Steroidsparing maintenance | Varies by drug | Controls organ involvement | Infection risk, liver labs |
| Biologic agents (Belimumab, Voclosporin) | Targeted Bcell or calcineurin pathways | Injection/infusion | Helps refractory disease | Cost, infusion reactions |
| Newwave drugs (Anifrolumab, Deucravacitinib) | Block interferon pathways | Clinical trials (2025) | Promise for skindominant lupus | Still under study |
Expert insight
According to , the choice between hydroxychloroquine and a biologic hinges on disease severity, organ involvement, and how well the patient tolerates steroids. A rheumatologist will weigh these factors carefully.
Lupus treatment infusion options
Infusions are usually reserved for moderate to severe disease or when oral medications fail. Common infusions include:
- Belimumab (Benlysta) given intravenously every 24 weeks.
- Rituximab a Bcell depleting drug, often used offlabel for lupus nephritis.
- Voclosporin approved for lupus nephritis, administered as a weekly infusion.
Infusion centers provide monitoring for reactions, which are rare but can include mild fever or headache. Some patients receive home infusions through specialized nursing services, adding convenience.
Nondrug therapies
Medications are powerful, but they work best when paired with lifestyle habits:
- Physical therapy to keep joints supple. Many patients find osteoporosis physical therapy helpful when steroids have affected bone health, and targeted osteoporosis exercises can be safely incorporated into a routine.
- Stressreduction techniquesyoga, meditation, or simple breathing exercises.
- Avoiding excessive sun exposure; wear SPF 30+ sunscreen daily.
- Quit smokingtobacco worsens cardiovascular risk in lupus.
Lupus treatment diet
While theres no magic lupus diet, certain foods can help tamp down inflammation and protect organs:
- Omega3 rich fish (salmon, sardines) antiinflammatory.
- Leafy greens (spinach, kale) high in antioxidants.
- Calciumrich dairy or fortified alternatives bone health, especially if youre on steroids.
- Lowsodium foods protect kidney function.
- Plenty of water helps flush the system.
Heres a quick 7day sample plan (just a sketch, not a prescription):
- Monday: Grilled salmon, quinoa, roasted broccoli.
- Tuesday: Lentil soup, mixed greens with oliveoil vinaigrette.
- Wednesday: Turkey stirfry with bell peppers and brown rice.
- Thursday: Greek yogurt with berries and a handful of almonds.
- Friday: Baked cod, sweet potato mash, steamed asparagus.
- Saturday: Spinach omelet, wholegrain toast, sliced avocado.
- Sunday: Chickpea salad with cucumbers, tomatoes, feta.
Balancing Risks Benefits
How to monitor treatment safety
Regular checkups keep the therapy on track. Typical labs include:
- Complete blood count (CBC) watches for low white cells.
- Comprehensive metabolic panel (CMP) checks liver and kidney function.
- Urine protein/creatinine ratio watches for kidney inflammation.
- Eye exam every 12 months if youre on hydroxychloroquine.
Make a calendar reminder for these appointments; theyre the compass that tells you whether youre sailing smoothly or need to adjust course.
When to adjust or switch therapy
If you notice any of the following, its time to have a conversation with your doctor:
- Frequent flares despite medication.
- New organ symptomspersistent swelling, chest pain, shortness of breath.
- Sideeffects that interfere with daily life (e.g., severe weight gain, mood swings).
- Abnormal lab results that persist across two visits.
Switching might mean tapering steroids, adding a biologic, or trying a newer drug from the newwave category.
Decisionmaking checklist (downloadable PDF)
- Are my symptoms under control?
- Are my lab values stable?
- Are sideeffects tolerable?
- Does my treatment fit my lifestyle?
Print this list and bring it to every appointment; it helps you and your physician make informed choices together.
Common Questions Answered
Can lupus kill you?
Only if it leads to severe organ damage that isnt treated promptly. With early diagnosis and a tailored treatment plan, the 5year survival rate exceeds 95% according to recent studies. The key is vigilance and partnership with a specialist.
What is the most effective treatment for lupus?
The most effective varies per person, but a typical hierarchy looks like this:
- Hydroxychloroquine foundation for mildtomoderate disease.
- Lowdose steroids for rapid control of flares.
- Immunosuppressants when kidneys, brain, or heart are involved.
- Biologics for refractory cases.
Think of it as building a house: hydroxychloroquine lays the foundation, steroids are the temporary scaffolding, immunosuppressants reinforce the walls, and biologics add the hightech security system.
Is there a cure for lupus?
At present, no cure exists, but many patients achieve longterm remission. Remission means the disease is under control, with minimal or no symptoms, and labs are stable. Ongoing research into targeted therapies continues to bring hope for even better outcomes.
How long does a lupus treatment infusion last?
Infusion times differ by drug. Belimumab usually takes about 30minutes for the first dose and 5minutes for subsequent doses. Rituximab can be 24hours, reflecting the slower infusion rate needed to avoid reactions. Your infusion center will give you exact timing.
Patient Stories Shared
From diagnosis to daily management
Mark, a 42yearold teacher, was diagnosed after a kidney biopsy revealed lupus nephritis. He started a regimen of mycophenolate, lowdose prednisone, and hydroxychloroquine. Within six months his proteinuria (protein in urine) dropped to normal levels, and he could return to fulltime teaching. He says the biggest lesson was listen to your body and never skip the annual eye exam.
Top 3 questions rheumatologists love to hear
- What are the goals of my treatment plan? Knowing the target (e.g., zero proteinuria) keeps you motivated.
- How will we monitor sideeffects? A clear monitoring schedule builds trust.
- What lifestyle changes will make the biggest difference? Nutrition, sun protection, and stress management often top the list.
Trusted Sources Listed
When youre navigating a complex disease, reliable information is priceless. Below are a few goto resources that reverify what weve discussed:
- CDC Lupus Basics detailed symptom and treatment overview.
- Mayo Clinic uptodate guidance on newer biologics and infusion protocols.
- Johns Hopkins Lupus Center research articles on dietary impact and disease activity.
- Peerreviewed 2024 study on belimumab efficacy (available via PubMed).
Conclusion
Choosing the right lupus treatment is a journey, not a onetime decision. The most effective plan usually starts with hydroxychloroquine, adds steroids or immunosuppressants when needed, and may incorporate biologics or infusions for tougher cases. Pairing medication with a lupusfriendly diet, sun protection, and regular monitoring creates a safety net that dramatically lowers the risk of serious complications. Remember, youre not alonerheumatologists, nutritionists, and supportive communities are ready to walk beside you.
Ready to take the next step? Download the decisionmaking checklist, talk openly with your doctor about your goals, and keep an eye on those lab results. Your health is a partnership, and with the right tools you can keep living the life you love.
FAQs
What is the most effective treatment for lupus?
The primary treatment is hydroxychloroquine, which controls symptoms and protects organs. Steroids, immunosuppressants, or biologics may be added based on disease severity and organ involvement.
Can lupus be fatal?
Lupus can be life-threatening if it severely damages vital organs like kidneys, heart, or lungs and is not treated promptly. Early diagnosis and treatment greatly reduce mortality risk.
Are there non-drug therapies to help with lupus?
Yes, physical therapy, stress reduction, sun protection, and quitting smoking complement medication to improve quality of life and reduce disease flares.
How often should I have monitoring tests during lupus treatment?
Regular labs such as blood counts, kidney and liver function, and urine tests are essential. Annual eye exams are important if taking hydroxychloroquine to monitor for retinal toxicity.
Are new lupus treatments available?
Recent approvals include biologics like belimumab, voclosporin, and obinutuzumab (Gazyva) for lupus nephritis. New therapies targeting specific immune pathways are in clinical trials, showing promise for better outcomes.