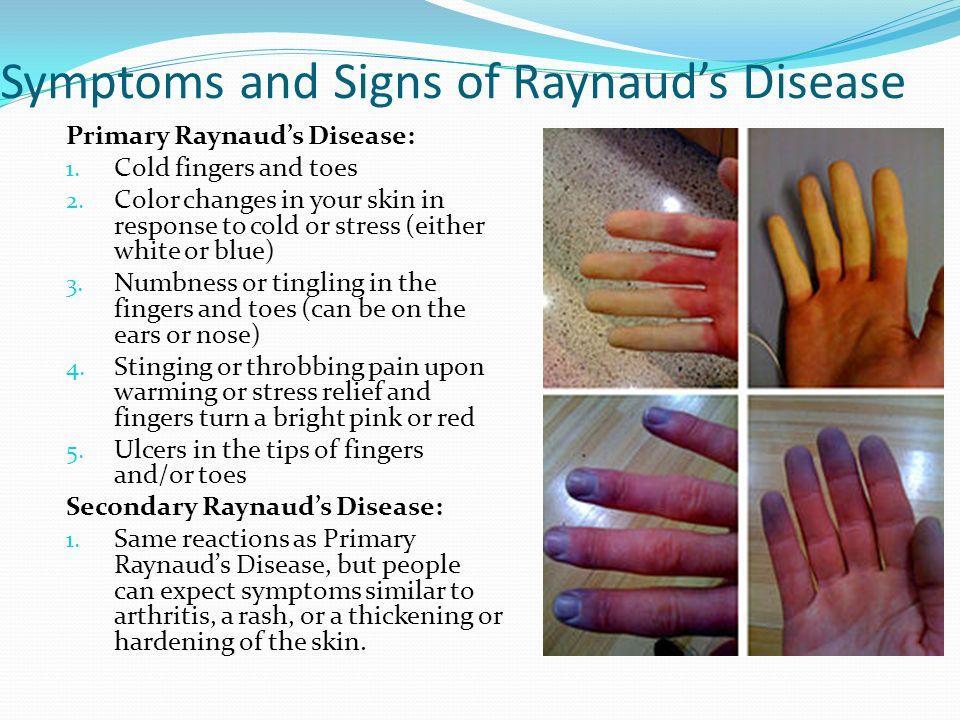
If your fingers turn whitebluered whenever it gets chilly or youre stressed, you might be wondering whether lupus is behind it. The short answer: inflammation of nerves or tiny blood vessels caused by lupus is the main trigger of Raynauds in these patients.
Knowing why this happens, spotting it early, and learning what you can actually do about it can stop the panic and give you a clear path forward. Lets walk through everything you need to know, side by side, like a friend sharing a cup of tea.
Quick-Fire Facts
| Question | Answer |
|---|---|
| What is Raynauds phenomenon? | A vascular response where small arteries spasm, causing color changes (white blue red) in fingers, toes, ears, or nose. |
| How common is Raynauds in lupus? | About onethird of people with lupus experience secondary Raynauds, according to the . |
| Main cause of Raynauds in lupus? | Immunemediated inflammation damages the lining of small vessels and irritates nerves, leading to vasospasm when exposed to cold or stress. |
| Do cold and stress matter? | Yes. Both trigger sympathetic nervous system activity, tightening the already vulnerable vessels. |
| Is Raynauds a sign of severe lupus? | Not always, but frequent episodes can hint at higher systemic inflammation and may merit a treatment review. |
Underlying Biology
Understanding the science helps demystify the why. In lupus, your immune system mistakenly attacks healthy tissue, including the tiny blood vessels (the endothelium). That attack releases cytokines like interferon, which makes the vessel walls stiff and prone to spasm. At the same time, the sympathetic nerves become overactive, shouting shut down! to those vessels whenever you feel cold or anxious.
Theres also a hormonal angle women are hit harder because estrogen can amplify the immune response. Thats why the early signs of lupus in females often include Raynauds alongside fatigue, joint aches, and photosensitivity.
Latest research (see a 2024 study in ) confirms that endothelial damage and nerve irritation work together, creating that classic colorchange cascade.
Early Signs
Picture this: youre holding a cold drink, and suddenly your fingertips turn ghostwhite, then a deep blue, and finally a bright pink as blood rushes back. Its startling, but its also a clue.
- Color sequence: White (no blood flow) Blue (low oxygen) Red (reoxygenation).
- Accompanying lupus clues: Unexplained fatigue, joint pain, a rash after sun exposure, and swollen lymph nodes.
- When to act: If episodes last longer than 15minutes, happen daily, or cause pain, its time to see a rheumatologist.
One reader told me, I was misdiagnosed with lupus for years, but the real breakthrough came when my doctor linked my coldinduced finger changes to Raynauds. Thats when we finally got the right treatment. Real stories like that remind us how crucial early detection is.
Diagnosing Raynaud
Diagnosing secondary Raynauds (the type tied to lupus) isnt just about watching your fingers turn colors. Doctors will run a battery of tests:
- Blood work: ANA, antidsDNA, and other autoantibodies to confirm lupus activity.
- Capillaroscopy: A noninvasive nailfold exam that reveals damaged capillaries typical of lupusrelated Raynauds.
- Doppler ultrasound: Checks blood flow in the small arteries.
Distinguishing primary from secondary Raynauds hinges on those lab markers and the presence of an underlying disease. A rheumatology specialist at often emphasizes that secondary Raynauds needs both vascular and autoimmune management.
Treatment Options
Good news: there are plenty of ways to keep those episodes in check. Think of treatment as a twopronged approachwarm your hands, and calm the immune system.
Lifestyle First
- Dress in layers; gloves that cover fingertips are a lifesaver.
- Stay stressfree with gentle yoga, meditation, or even a favorite playlist.
- Quit smokingnicotine narrows vessels even more.
Medication Matters
When lifestyle tweaks arent enough, doctors turn to medicines that dilate vessels:
- Calciumchannel blockers (e.g., amlodipine) firstline for most patients.
- PDE5 inhibitors (e.g., sildenafil) useful if blockers fall short.
- Lowdose aspirin reduces clot risk in severe cases.
Because the root cause is lupus, lupusspecific therapies also help:
- Hydroxychloroquine tames the immune system and often eases Raynauds.
- Immunosuppressants (mycophenolate, azathioprine) reserved for more aggressive disease.
When ulcers or tissue loss appear, a vascular surgeon might consider prostacyclin analogues or even surgical revascularizationrare, but lifesaving.
Risks & Complications
Most people wonder, Can you die from Raynauds disease? The short answer is rarely. Raynauds itself isnt fatal, but untreated secondary Raynauds can lead to digital ulcers, infections, or, in extreme cases, gangrene.
Several rare diseases mimic lupusrelated Raynauds, such as scleroderma or mixed connectivetissue disease. A quick comparison helps keep the picture clear:
| Condition | Key Distinguishing Feature | Typical Raynauds Pattern |
|---|---|---|
| Lupus | Positive ANA, antidsDNA, skin rash | Intermittent, often triggered by stress |
| Scleroderma | Skin thickening, CREST syndrome | More severe, may cause digital ulcers |
| Mixed CTD | Overlap of lupus & scleroderma antibodies | Variable, can be chronic |
If you notice pain lasting over 15minutes, skin color that doesnt return to normal, or open sores, treat it as urgent and seek medical help immediately.
Bottom Line
The primary lupus Raynaud cause is inflammationdriven vasospasm of tiny blood vessels and nerves, usually set off by cold or stress. Recognizing early signs, getting the right tests, and blending lifestyle measures with targeted medication can keep episodes mild and protect your digits.
Dont let a mysterious color change dictate your life. Talk to your rheumatologist about any fingerturning episodes, grab a RaynaudsReady checklist, and stay connected with a community that understands what youre going through. If you have questions or want to share your own story, drop a comment belowyour experience could be the light someone else needs.
FAQs
What is the primary cause of Raynaud’s in people with lupus?
Inflammation of the tiny blood‑vessel lining and irritation of the nerves by lupus‑driven immune activity cause the vessels to spasm, producing the classic white‑blue‑red color changes.
How can I tell if my Raynaud’s episodes are linked to lupus?
Look for additional lupus signs such as fatigue, joint pain, a photosensitive rash, or abnormal blood‑test results (positive ANA, anti‑dsDNA). A rheumatologist may also use nail‑fold capillaroscopy to spot lupus‑specific capillary damage.
Which medications are most effective for lupus‑related Raynaud’s?
First‑line agents are calcium‑channel blockers (e.g., amlodipine). If needed, PDE‑5 inhibitors (sildenafil) or low‑dose aspirin can be added. Treating the underlying lupus with hydroxychloroquine or immunosuppressants also reduces episodes.
Can lifestyle changes lessen the frequency of attacks?
Yes. Keeping hands warm, avoiding rapid temperature changes, managing stress with relaxation techniques, and quitting smoking dramatically cut the number and severity of episodes.
When should I seek urgent medical care for Raynaud’s?
Seek help immediately if pain lasts more than 15 minutes, the skin does not return to normal color, or you develop ulcers or sores, as these can signal tissue damage that needs prompt treatment.