Endometriosis pain can feel like a deep, throbbing cramp, a constant pelvic pressure, or a sharp sting that shoots down your back or legs. Knowing how to describe that pain accurately can make a huge difference it helps doctors diagnose you faster, lets partners understand what youre going through, and gives you the confidence to ask for the right treatment.
So lets cut the medical jargon and get straight to the point. Below youll find simple ways to talk about the pain, a quick look at the symptoms you might not have heard of, practical tips for managing the discomfort, and even some reallife stories that show youre not alone.
What Causes Pain
Why does endometriosis hurt?
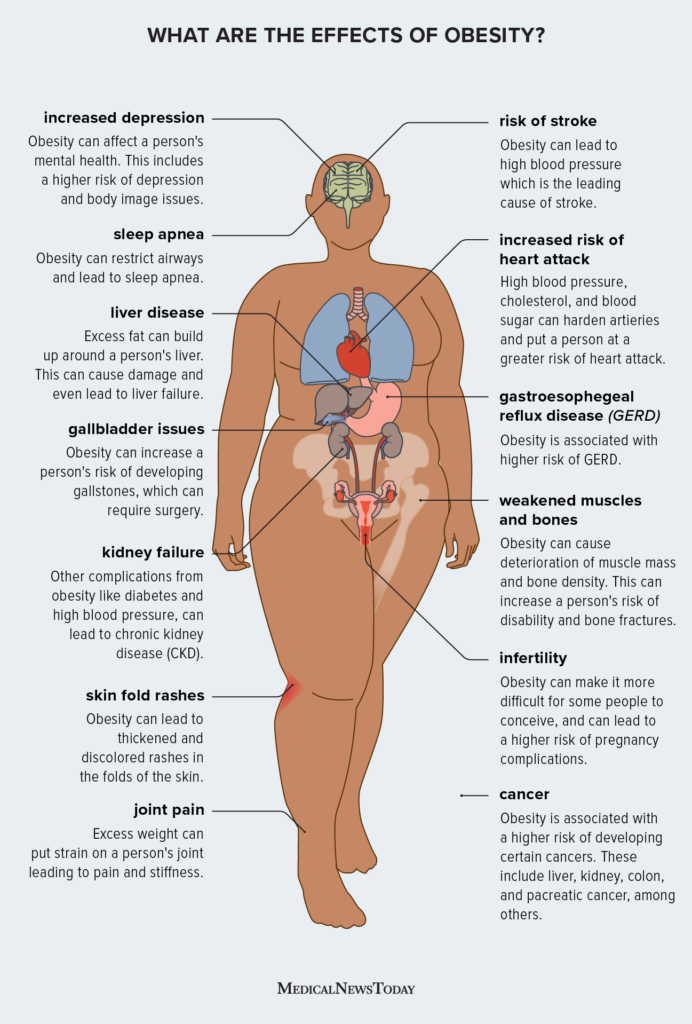
The root of the pain is tissue that looks and acts like the lining of your uterus, but it grows outside the uterus on ovaries, fallopian tubes, the bowel, even the diaphragm. Each month this outsidelining bleeds, but because it cant exit the body, it becomes inflamed and irritates nearby nerves.
How is it different from regular cramps?
Typical menstrual cramps usually peak in the first couple of days and fade away. Endometriosis pain, on the other hand, can linger for weeks, flare up on days when youre not even on your period, and often radiates to places you wouldnt expect, like your lower back, thighs, or even your shoulder tip.
Where does the pain show up?
Most people feel it in the pelvic floor, deep inside the lower abdomen, or in the lower back. Some describe it as a burning sensation that spreads to the hips or calves. According to , the location can change depending on where the tissue implants, which is why a pain map is often useful when you talk to your doctor.
Quick painlocation cheat sheet
- Pelvic floor: pressure, a feeling of fullness
- Lower back: constant ache that worsens after sitting
- Legs/thighs: throbbing or numbness, especially after sex
- Shoulder tip: occasional sharp sting a sign of diaphragmatic implants
20 Symptoms to Watch
The classic checklist
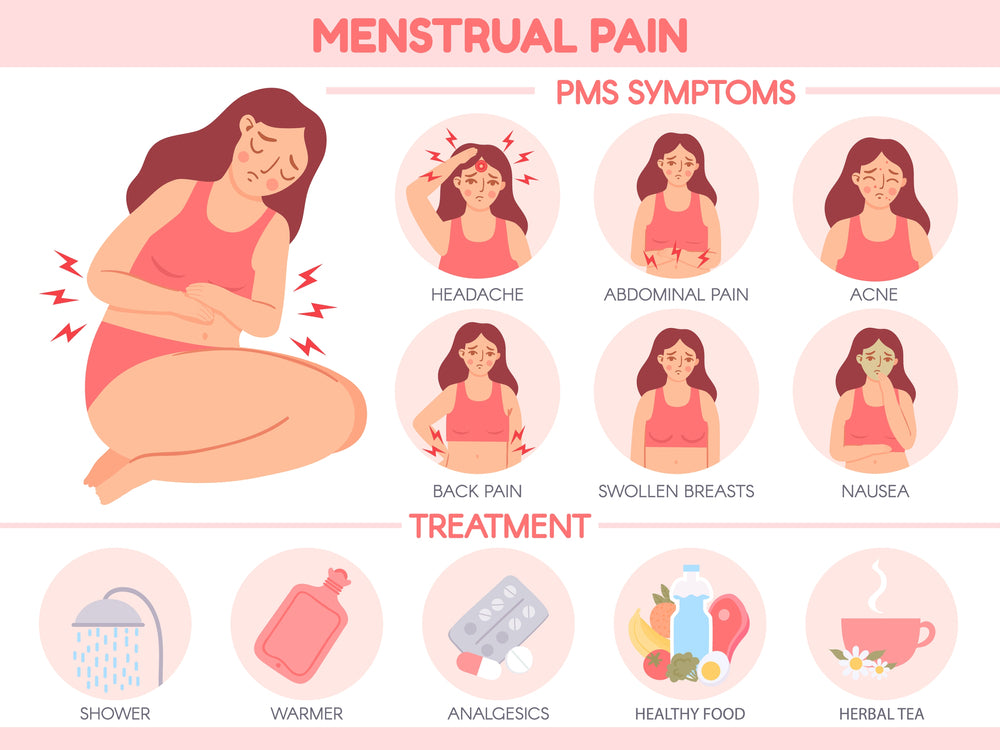
If youve ever taken a do I have endometriosis? quiz, you probably saw the usual suspects: painful periods, chronic pelvic pain, pain during sex (dyspareunia), bowel or bladder discomfort, fatigue, and trouble getting pregnant. Those are the core eighttoten symptoms most doctors start with.
Going beyond the basics
Heres a rundown of the full 20symptoms list, including some that are a bit more off the radar. Recognising the uncommon signs can help you catch the condition earlier and explain it better to anyone you need to.
| # | Symptom |
|---|---|
| 1 | Severe dysmenorrhea (painful periods) |
| 2 | Chronic pelvic pain |
| 3 | Dyspareunia (pain during or after sex) |
| 4 | Painful bowel movements or constipation during menstruation |
| 5 | Urinary urgency or pain during periods |
| 6 | Heavy or irregular bleeding |
| 7 | Fatigue that doesnt improve with rest |
| 8 | Infertility or difficulty conceiving |
| 9 | Back pain that worsens with your cycle |
| 10 | Leg pain or numbness |
| 11 | Shoulder tip pain (often linked to diaphragm implants) |
| 12 | Pain during ovulation (midcycle mittelschmerz) |
| 13 | Digestive bloating or gas |
| 14 | Weight fluctuations unrelated to diet |
| 15 | Persistent lowgrade fever during flareups |
| 16 | Skin rashes near the affected organ |
| 17 | Unexplained mood swings or anxiety spikes |
| 18 | Pelvic stiffness that limits exercise |
| 19 | Spotting between periods |
| 20 | Feeling off or different during menstruation without a clear cause |
Using a quiz responsibly
Online quizzes can be a helpful first step, but theyre not a diagnosis. A reputable source like the emphasizes that results should be discussed with a healthcare professional, not taken as a final verdict.
Talking About Pain
With a romantic partner
When youre trying to explain endometriosis pain to a guy (or anyone who hasnt experienced it), analogies work wonders. Try saying, Imagine a deep muscle cramp that never fully releases, and then it spikes whenever Im intimate or sit for long periods. Adding a simple visual like drawing a small diagram on a napkin can make the abstract feel concrete.
With friends or family
Friends tend to respond well to everyday language. You might say, Its like having a constantly tight band around my lower stomach that tightens every month, and sometimes it radiates down my legs. Keep the tone honest but light, and give them space to ask followup questions.
With your doctor
Medical professionals love specifics. Use a pain scale (010), note the exact locations, trigger points, and how long each episode lasts. For example: I rate the pelvic pain a 7/10, it starts two days before my period, peaks on day 1, and lingers for a week. It also flares after I sit for more than two hours. Bringing a small notebook or a printed painmap can streamline the conversation.
Writing it down email or portal
If you communicate through a patient portal, keep it structured:
- Date & Cycle Day: e.g., Cycle day 12 (two days before bleed).
- Pain Rating: 7/10.
- Location: Lower abdomen, right leg.
- Triggers/Relief: Worsens after sitting; eases with heat pack.
Managing the Discomfort
Lifestyle tweaks (how to prevent endometriosis progression)
While theres no guaranteed way to stop endometriosis from developing, certain habits can lessen the intensity of flareups:
- Antiinflammatory diet: Load up on leafy greens, omega3 rich fish, and turmeric.
- Regular, gentle exercise: Yoga or pilates help keep the pelvic floor supple.
- Stress reduction: Mindfulness, meditation, or even a short walk can lower cortisol, which in turn may reduce pain sensitivity.
Medication options
Overthecounter NSAIDs (like ibuprofen) are a firstline choice for shortterm relief. Hormonal therapiesbirth control pills, progestins, or GnRH agonistscan suppress the cyclic buildup of tissue, but they come with sideeffects that need a doctors guidance.
Surgical routes (endometriosis surgery)
When medication isnt enough, many turn to minimally invasive laparoscopy. Surgeons either excise (cut out) the lesions or ablate (burn) them. According to a study published in , excision tends to give longer painfree periods, especially for deep infiltrating disease.
What to expect from surgery
- Recovery time: Typically 24 weeks for light work, 68 weeks for strenuous activity.
- Success rates: 6080% report significant pain reduction, but recurrence is possible.
- Potential risks: Bleeding, infection, or adhesion formationalways discuss these with your surgeon.
Emerging therapies
Clinical trials are exploring hormonal modulators, immunotherapy, and even laser ablation techniques. If youre interested, ask your doctor about trial eligibility or check registries like .
Prognosis and Life Expectancy
Understanding staging (stage4 endometriosis)
Staging (IIV) describes how far the tissue has spread, not how severe the pain will be. Even stage4 can be managed effectively with a combination of medical and surgical care.
Is endometriosis lifethreatening?
Good news: it doesnt affect overall life expectancy. According to the World Health Organization, women with endometriosis have normal lifespans. The real challenge lies in quality of lifepersistent pain can impact work, relationships, and mental health.
Longterm outlook
With proper treatment, many people achieve symptom control for years. Ongoing monitoring, lifestyle choices, and sometimes repeat surgery are part of a lifelong management plan.
Real Stories & Expert Tips
A quick case study
Maria, a 28yearold graphic designer, spent three years feeling off during her periods. She described the pain as a knot in my lower back that wouldnt let go. After finally showing her doctor a handdrawn pain map, she was referred for laparoscopy, which revealed stageIII lesions. Postsurgery, her pain rating dropped from 8/10 to 2/10, and she finally felt comfortable sharing her experience with her partner.
Expert voice
Dr. Kossl, a pelvicfloor specialist, notes that many patients mistake pelvicfloor spasm for endometriosis pain. A thorough physical exam can differentiate the two, leading to targeted physiotherapy when appropriate. (cited from a recent symposium on pelvic health).
Where to learn more
Trusted resources include the Mayo Clinic, the Endometriosis Foundation, and the NHS website. All provide evidencebased guidelines without the sensationalism you sometimes see on forums. If youre also navigating related reproductive health issues such as fertility concerns, see practical guidance on lean PCOS fertility for tips that may be relevant to people with overlapping symptoms.
Conclusion
Understanding and explaining endometriosis pain isnt just about finding the right words its about gaining the confidence to ask for help, share your experience, and take control of your health. Remember the threestep formula: Identify the sensation, describe it clearly, and seek the right care. If youve found a phrase or a tip that works for you, drop it in the comments sharing your story could be the lifeline someone else needs.
FAQs
What are the most common ways to describe endometriosis pain?
People often compare it to a deep, throbbing cramp, constant pelvic pressure, or a sharp sting that can radiate to the back, thighs, or shoulder tip.
How can I create a pain map for my doctor?
Draw a simple outline of your lower torso and mark areas with numbers or colors indicating intensity (0‑10), timing, and triggers. Bring this to appointments.
Why does endometriosis pain sometimes appear on days without a period?
Implanted tissue can bleed and inflame at any time, irritating nearby nerves, so pain may flare outside the menstrual window.
Can lifestyle changes really reduce endometriosis pain?
Yes. An anti‑inflammatory diet, regular gentle exercise (like yoga or pilates), and stress‑reduction techniques have been shown to lessen flare‑ups for many patients.
When should I consider surgery for endometriosis?
If medication and lifestyle tweaks don’t bring pain below a 4/10 or if the pain interferes with daily life, discuss laparoscopic excision or ablation with a specialist.