Hey there, friend. If youre reading this, youve probably felt that unsettling flutter in your chest, the dizzy spell when you stand up, or that lingering brainfog that just wont quit. Youre not alone, and good news: there are realworld strategies that can help calm the chaos. Below youll find a friendly walkthrough of what works, what to watch out for, and how to start feeling like yourself again.
Understanding the Issue
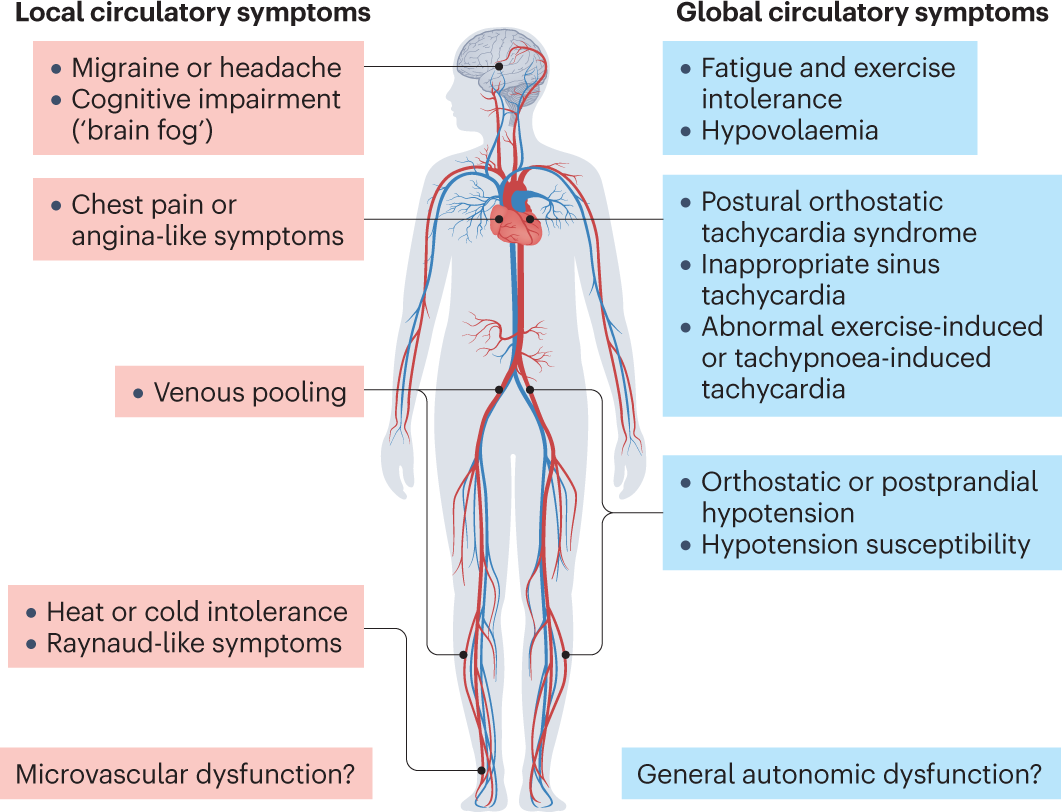
First, lets get clear on what autonomic dysfunction actually means after COVID. Your autonomic nervous system is the part of your brainbody wiring that runs in the background, controlling heart rate, blood pressure, digestion, temperature, and more. When it gets thrown offbalancesomething many survivors call long COVID dysautonomiathose background settings start acting up.
Typical symptoms include:
- Rapid heart rate (tachycardia) that spikes even when youre just sitting.
- Lightheadedness or fainting when you stand (orthostatic intolerance).
- Fatigue that isnt fixed by a good nights sleep.
- Gut upset, shaky hands, and that brainfog feeling.
One of the most common questions is how long does postCOVID tachycardia last? The answer varies: some people see improvement within a few weeks, while others may need several months of targeted care. A recent NIH RECOVER study found that the median duration of noticeable heartrate spikes was around four months when patients followed a structured treatment plan.
And what about the dreaded phrase will postCOVID POTS go away? The data is hopefulabout 70% of patients in a large AAFP review reported meaningful symptom reduction within six months when they combined lifestyle tweaks with medication when needed.
Core Treatment Pillars
Think of treating long COVID autonomic dysfunction like tuning a guitar. You can tighten a string (add salt), adjust the tension (compression garments), practice the chords (graded exercise), and sometimes use a capo (medication) to get the right pitch. Below are the six main pillars that clinicians and patients alike swear by.
Fluid & Salt Repletion
Dehydration is the villain that makes any autonomic issue worse. Aim for at least 23liters of water a day, and sprinkle in 35grams of salt (roughly one teaspoon) spread across meals. If youre on a lowsodium diet for another condition, talk to your provider about a safe adjustment.
Compression Garments
Support stockings (2030mmHg) and abdominal binders act like a gentle hug for your veins, keeping blood from pooling in your lower body. Put them on in the morning and keep them on for a few hours after you stand or exercise. Many survivors notice fewer dizzy spells within just a few days.
Graded & Isometric Exercise
Moving slowly is key. Start with recumbent bike sessions (510minutes at a comfortable pace), then graduate to standing marches. Adding isometric moveslike pressing your legs together or tightening your core for 10second burstshelps the nervous system learn how to regulate blood flow. recommends a 2week progression plan that many patients find manageable.
Medication Options
When lifestyle alone isnt enough, doctors may prescribe:
- Fludrocortisone boosts your blood volume.
- Midodrine narrows blood vessels to raise blood pressure.
- Betablockers (e.g., propranolol) calm the hearts overactivity.
These meds are usually lowdose and closely monitored. The goal isnt to mask symptoms forever but to give your body a chance to reset.
Lifestyle & Trigger Management
Small daily habits can make a world of difference:
- Rise slowly: Sit on the edge of the bed for a minute before standing.
- Stay cool: Wear breathable fabrics and avoid hot showers that can drop blood pressure.
- Limit caffeine: A cup of coffee is fine, but too much spikes heart rate.
- Consistent sleep: Aim for 79hours, and keep a regular bedtime.
Education & SelfMonitoring
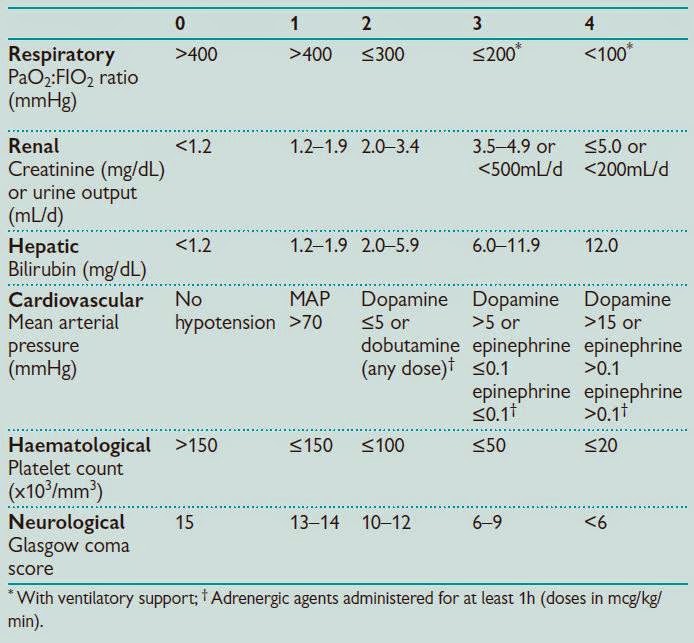
Knowledge is power. Keep a simple journal noting heart rate, blood pressure, and symptom severity. A cheap smartwatch or a Bluetooth BP cuff can give you realtime feedback, helping you see what works and what doesnt. If youre tracking organ function or severity over time, tools used for sepsis scoring and organ failure assessment like the SOFA score can be helpful models to think about when standardizing measurements across visits see a practical guide to SOFA score and SOFA calculation for reference SOFA score.
Common Patient Questions
How long does postCOVID autonomic dysfunction typically last?
Most people notice a steady decline in symptoms after 36months of consistent treatment. However, a minority may need longer, especially if they have underlying conditions like diabetes or preexisting dysautonomia.
Can I cure POTS after COVID without medication?
Yes, many patients achieve substantial relief with just salt, compression, and graded exercise. Still, a shortterm medication course can speed up recovery for those who feel stuck.
What are the biggest red flags that need urgent care?
Severe chest pain, sudden fainting, rapid heart rate over 130bpm at rest, or new arrhythmias should prompt an immediate call to your doctor or the emergency department.
Is it safe to exercise if I have orthostatic intolerance?
Absolutelyif you start lowimpact and stay hydrated. The key is to avoid rapid position changes and to incorporate the countermaneuvers (leg crossing, muscle tensing) we mentioned earlier.
Do dietary changes help dysautonomia?
Frequent, small meals that are low in refined carbs and high in electrolytes (banana, avocado, leafy greens) keep blood sugar stable and support vascular tone.
Will my symptoms disappear completely?
Most survivors experience at least a 50% improvement, and many feel back to baseline within a year. A small group may keep mild symptoms, but those are often manageable with the tools above.
Real World Stories
Patient Story: From 120bpm at Rest to Stable 70
Maria, a 38yearold teacher, woke up one morning with a heart rate hovering around 120bpm while she was still in bed. She felt like she was on a treadmill she couldnt step off. After visiting a dysautonomia clinic, she began a regiment of 3g salt daily, compression stockings, and a 10minute recumbent bike routine. Within three weeks, her resting heart rate dropped to the low 80s, and by month two she was consistently under 75bpm. It felt like my body finally remembered how to breathe, she says.
Clinician Interview: Autonomic Specialists Top 5 Tips
Dr. Patel, a neurologist at a major academic center, emphasizes:
- Start with fluid and salt before reaching for meds.
- Use a symptom journal to track trends.
- Gradually reintroduce upright activities.
- Never ignore a sudden drop in blood pressure.
- Stay connected with a support groupyoure not alone.
Comparison Table: Lifestyle vs. Medication vs. Combined
| Approach | Efficacy (Typical) | Time to Benefit | SideEffects | Cost |
|---|---|---|---|---|
| Lifestyle Only | Moderate (4060% improvement) | 48weeks | Minimal | Low |
| Medication Only | High (7080% improvement) | 13weeks | Possible dizziness, electrolyte shifts | MediumHigh |
| Combined | Very High (8090% improvement) | 24weeks | Managed with monitoring | Variable |
DIY Symptom Tracker Template
Feel free to copy this simple layout into a notebook or spreadsheet:
- Date & Time
- Heart Rate (rest & postactivity)
- Blood Pressure (standing & sitting)
- Symptoms (scale 05 for dizziness, fatigue, brain fog)
- What you ate / drank
- Medications taken
Patterns emerge quickly, and youll have concrete data to discuss with your provider.
Building a Care Plan
Find the Right Provider
Look for a clinician who specializes in dysautonomia, postviral syndromes, or cardiology with a focus on autonomic testing. Many major university hospitals now have dedicated Long COVID clinics.
Ask the Right Questions
When you sit down with your doctor, consider these five mustask items:
- What specific tests will you run to confirm autonomic dysfunction?
- Can we start with nonpharmacologic measures, and how will we measure success?
- If medication is needed, which one and at what dose?
- What redflag symptoms should prompt an immediate call?
- Are there any ongoing clinical trials I could join?
Set Realistic Goals
Shortterm: Stay hydrated, wear compression socks, and log your heart rate each morning.
Longterm: Return to a full day of work or school without feeling faint.
Stay Updated
Research on long COVID is evolving fast. The NIH RECOVER trial continuously publishes new findings, and many patient advocacy groups post weekly updates. Keeping an eye on reputable sources can give you a sense of hope and direction.
Conclusion
Living with long COVID autonomic dysfunction can feel like navigating a stormy sea, but you have a sturdy vessel at your disposal: a mix of fluid and salt strategies, compression support, gentle exercise, andwhen neededcarefully chosen medication. Most folks see meaningful improvement within a few months, especially when they partner with a knowledgeable clinician and track their progress. Remember, youre not alone on this journey. Reach out, share your story, and lets keep each other steady as we sail toward recovery.
FAQs
How long does post‑COVID autonomic dysfunction typically last?
Most people see steady improvement within 3‑6 months of consistent treatment, though some may need longer if they have other health issues.
Can POTS after COVID be cured without medication?
Yes, many patients achieve significant relief through increased salt, compression garments, and graded exercise, though short‑term meds can speed recovery if needed.
What are the red‑flag symptoms that require urgent medical care?
Severe chest pain, sudden fainting, a resting heart rate over 130 bpm, or new arrhythmias should prompt immediate medical attention.
Is it safe to exercise with orthostatic intolerance?
Exercise is safe when started low‑impact, staying well‑hydrated, and avoiding rapid position changes; use counter‑maneuvers like leg crossing to help.
Do dietary changes help with dysautonomia?
Frequent small meals low in refined carbs and rich in electrolytes (e.g., bananas, avocado, leafy greens) help stabilize blood sugar and support vascular tone.