Quick Answer Overview
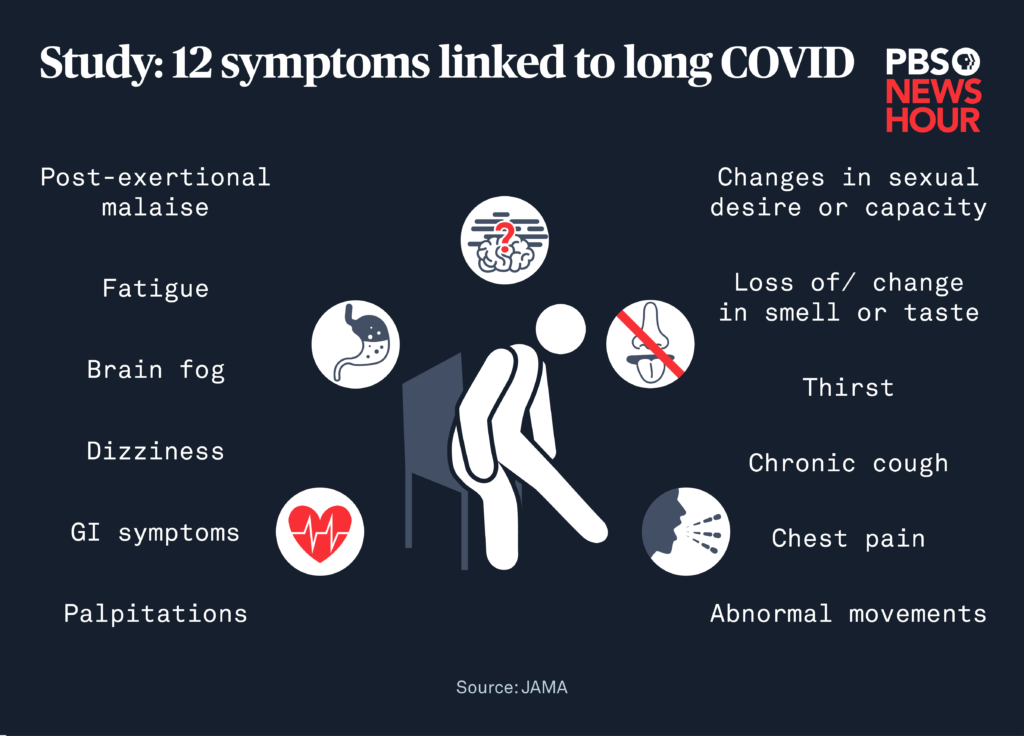
In a nutshell, the 12 most common longCOVID symptoms are extreme fatigue, brain fog, shortness of breath, chest pain or palpitations, persistent cough, loss or change of taste and smell, headaches, dizziness, sleep problems, joint and muscle pain, gastrointestinal issues, and mood changes. If any of these linger for more than four weeks after your initial infection, you might be dealing with long COVID and its a good idea to talk to a health professional.
Why It Matters
Knowing these symptoms isnt just triviait can be the difference between weeks of uncertainty and a clear path to recovery. Early recognition lets you seek targeted care, which many studies show can speed up healing and prevent complications. On the flip side, overmedicalising every ache can cause unnecessary anxiety, so its important to stay balanced and realistic about what each symptom really means.
Balancing Benefits and Risks
Spotting a symptom early does give you a head start on treatment, but assuming every headache is long COVID could lead you to unnecessary tests. The sweet spot? Pay attention, stay informed, and let a qualified clinician confirm the diagnosis.
RealWorld Example
Take Maria, a 38yearold teacher. She brushed off her crushing fatigue as postvacation tiredness until her GP asked specifically about the 12 key longCOVID signs. A referral to a specialised clinic later helped her get a tailored rehab plan, and shes back in the classroom now.
The 12 Core Symptoms
Below is a friendly guide that breaks each symptom down into what to look for and when to get help. Think of it as your personal checklist.
| Symptom | What to Look For | When to Seek Help |
|---|---|---|
| Extreme Fatigue | Persistent exhaustion that isnt cleared by rest. | If fatigue stops you from daily tasks for more than two weeks. |
| Brain Fog | Difficulty concentrating, memory lapses, mental fuzziness. | Sudden worsening or safetycritical tasks affected. |
| Shortness of Breath | Feeling winded after light activity or at rest. | New or worsening chest pain, oxygen saturation below 94%. |
| Chest Pain / Palpitations | Tightness, racing heart, skipped beats. | Any pain radiating to arm/jaw, or fainting. |
| Persistent Cough | Dry or wet cough lasting more than four weeks. | Cough with blood, severe wheeze, or fever. |
| Loss / Change of Taste or Smell | Partial or total loss, distortion (e.g., metallic taste). | If it persists beyond three months. |
| Headaches | Newonset or changed pattern, often tensiontype. | Sudden severe thunderclap headache. |
| Dizziness / Orthostatic Intolerance | Lightheadedness on standing, brainfogginess. | Falls, fainting, or worsening with activity. |
| Sleep Problems | Insomnia, restless sleep, vivid dreams. | If sleep deprivation starts affecting mental health. |
| Joint & Muscle Pain | Aching joints, myalgia not linked to activity. | Swelling, redness, or severe limitation. |
| GI Issues | Nausea, diarrhoea, abdominal pain. | Blood in stool, vomiting blood, or severe dehydration. |
| Mood & MentalHealth Changes | Anxiety, depression, irritability. | Suicidal thoughts or inability to function. |
Expert Insight
Prevalence numbers come from the , the , and the latest surveys, which all agree that fatigue tops the list, showing up in roughly 70% of cases.
How Long It Lasts
Everyones timeline looks a little different, but research gives us a useful framework:
- 412 weeks: The postviral phase where many people start feeling better.
- 36 months: The most common window for chronic symptoms.
- Beyond 12 months: About 1015% of patients remain symptomatic, often called longhaul COVID.
What Influences Duration?
Age, severity of the initial infection, vaccination status, and preexisting health conditions all play a role. A 2024 analysis from the found that fully vaccinated individuals who still got infected were about 50% less likely to experience symptoms beyond six months.
Diagnosing and Testing
When should you start looking for a formal diagnosis? If youve been dealing with any of the 12 symptoms for more than four weeks and you notice any redflag signs (like chest pain, severe shortness of breath, or blood in stool), its time to get tested.
Recommended Tests
Doctors typically order a combination of blood work and functional assessments:
- CBC & CRP: Checks for inflammation or hidden infections.
- Ddimer: Screens for clotting issues.
- Pulmonary function tests: Measures lung capacity, especially useful for shortness of breath.
- Cardiac MRI or ECG: For chest pain and palpitations.
- Smelltest kits: Objective way to assess loss of smell.
Expert Quote
Dr. Elena Rossi, a pulmonologist at a leading UK university hospital, notes, A thorough workup not only validates the patients experience but also helps us rule out other conditions that might mimic long COVID.
Managing and Treating
There isnt a onesizefitsall prescription for long COVID, but a blend of general care principles and symptomspecific strategies can make a huge difference.
General Care Principles
- Pacing: Break activities into small chunks and rest between them.
- Nutrition & Hydration: Balanced meals and plenty of water support recovery.
- Sleep Hygiene: Consistent bedtime, cool dark room, limiting screens.
SymptomSpecific Strategies
| Symptom | Treatment Option | Evidence Source |
|---|---|---|
| Fatigue | Pacing, CBTbased energy management | |
| Brain Fog | Cognitive rehab, vitamin B12 check | |
| Shortness of Breath | Breathing exercises, pulmonary rehab | NIH research |
| Chest Pain/Palpitations | ECG, betablockers if indicated | American Heart Association |
| Persistent Cough | Inhaled steroids, ENT evaluation | CDC guidance |
| Loss of Taste/Smell | Olfactory training (fourstep) try guided smell training programs to retrain sensing neurons; see SOFA score for unrelated ICU scoring context if you are being assessed in hospital settings. | NIH Smell & Taste study |
| Headaches | NSAIDs, hydration, trigger diary | Mayo Clinic |
| Dizziness | Tilttable test, increase fluids | Cleveland Clinic |
| Sleep Problems | CBTI, melatonin (3mg) | NHS sleep clinic |
| Joint/Muscle Pain | Physical therapy, lowdose steroids | NHS |
| GI Issues | Probiotics, diet modifications | Cleveland Clinic |
| Mood Changes | Counseling, SSRIs if needed | CDC mentalhealth guidance |
Personal Touch
When I first heard about postviral fatigue, I imagined a gentle tiredness that a good nights sleep could fix. The reality was a bonedeep exhaustion that made climbing stairs feel like scaling a mountain. The first step that helped mealong with countless otherswas simply admitting, Im not fine, and then building a schedule that respected my new limits.
Real World Stories
Case #1: The Teachers Tale
Maria, 45, returned to her classroom after a mild COVID infection. Within weeks she was battling brain fog and a pounding headache. A referral to a longCOVID rehab program introduced her to paced learning modules, breathing exercises, and weekly counseling. Six months later, she reports 80% improvement and is now an advocate for early symptom recognition.
Case #2: The Young Athlete
Jacob, 22, a semiprofessional cyclist, experienced chest palpitations and shortness of breath after his infection. Cardiac MRI revealed mild myocarditis. After a supervised cardiac rehab plan, he gradually rebuilt his stamina. He credits open communication with his doctor and a structured rehab timeline for getting back on the bike.
Helpful Resources Guide
Feeling a little overwhelmed? Here are some trustworthy places to turn to:
- NHS Long COVID Clinics: Find a local service through the .
- CDC Long COVID Guidance: Uptodate recommendations on testing and care .
- Patient Support Groups: Communities like LongCOVIDSOS and various Facebook groups offer peer advice and emotional support.
- Research Updates: The and publish the latest studies on prevalence and treatments.
Wrapping It Up
The 12 hallmark symptoms of long COVIDfatigue, brain fog, breathing trouble, chest discomfort, lingering cough, taste or smell changes, headaches, dizziness, sleep issues, joint and muscle aches, gastrointestinal upset, and mood shiftscan linger for months after the virus has left the acute stage. Recognising them early, seeking professional assessment, and applying evidencebased management can dramatically improve quality of life. If any symptom feels out of the ordinary or worsens, reach out to your GP or a specialised longCOVID clinic. Youre not alone on this journey; theres a growing community, solid research, and compassionate clinicians ready to help.
Whats your experience with long COVID? Have you found a particular strategy that works wonders for you? Drop a comment below, share your story, and lets support each other on the road to feeling better.