Got that flippingflopping feeling in your chest and wondering if its something to worry about? Thats often the first sign of lone atrial fibrillationan irregular heartbeat that shows up in otherwise healthy, younger adults. In short, its AF without the usual culprits like high blood pressure or heart valve disease. Below youll find everything you need to know: why it happens, how dangerous it really is, the best ways to treat it, and practical steps to keep it from crashing your life again.
Stick around, because well break it down in plain language, sprinkle in a few reallife stories, and give you a simple action plan you can start using today.
What Is Lone AF?
Definition at a Glance
Lone atrial fibrillation (often just called lone AF) is atrial fibrillation that occurs in people under about 60years old who have no structural heart disease, hypertension, thyroid problems, or other clear triggers. The term was first coined in the 1950s, but modern guidelines still use it to flag patients who need extra attention despite looking otherwise healthy ().
Who Gets It?
Most cases pop up in young to middleaged adults, with a slight male predominance. Think of Emily, a 34yearold marketing manager who felt a sudden whoosh in her chest during a yoga class. A quick ECG at her doctors office confirmed lone AF, and shes been managing it ever since.
Symptoms
Typical Feelings
People with lone AF often describe a rapid, fluttering heartbeat, occasional dizziness, shortness of breath, or an unsettling chest sensation. Some call it a racecar engine in the chest. Not every episode feels dramaticup to 30% of patients are completely asymptomatic, which is why routine heart checks can be a lifesaver.
When Its Silent
If you never notice any weird palpitations, you might still have lone AF. An opportunistic ECG during a routine physical can catch those silent cases before they turn into a bigger problem.
Causes & Triggers
Genetic Links
Family history matters. Recent genomewide studies have identified several gene variants that increase the odds of developing AF even in the absence of heart disease (). If your dad or sibling had AF, keep a closer eye on yourself.
Lifestyle Factors
- Excess caffeine or alcohol binge drinking can spark an episode.
- Sleep apnea the nightly oxygen dips are a hidden AF trigger.
- Intense endurance training marathon runners sometimes develop AF from chronic heart stress.
- Stress & anxiety the fightorflight hormones love to mess with heart rhythm.
Lone AF vs. Paroxysmal AF
| Feature | Lone AF | Paroxysmal AF |
|---|---|---|
| Age typical | <60 years | Any age |
| Underlying disease | None detected | Often present |
| Recurrence | Variable, may stop | Episodes end spontaneously |
| Management focus | Identify hidden triggers | Control rhythm & rate |
Diagnosis
How Doctors Confirm It
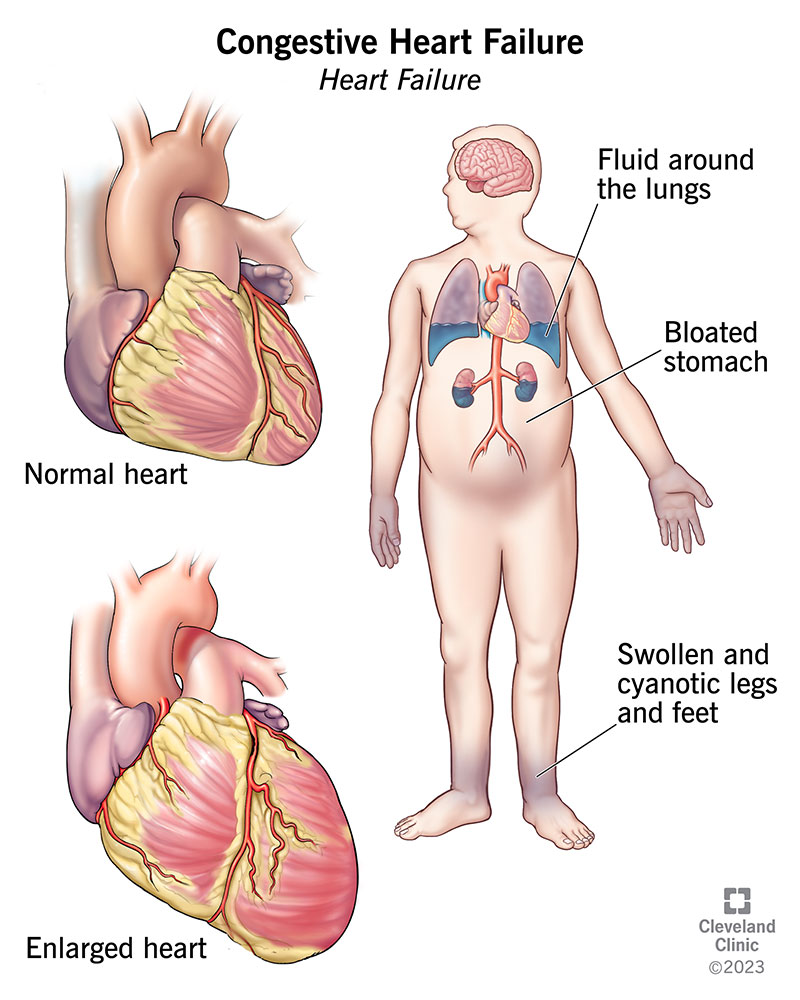
A 12lead ECG is the gold standard for catching an irregular rhythm. If the first test is inconclusive, a Holter monitor (2448hours) or an event recorder can catch intermittent episodes. An echocardiogram is also performed to rule out structural heart diseaseessential to label the arrhythmia as lone. If swelling or signs of heart failure are present during evaluation, clinicians will often investigate heart failure edema as part of the workup to ensure symptoms aren't from fluid overload.
ICD10 Coding
There isnt a dedicated code for lone AF. Doctors usually use I48.0 for paroxysmal AF or I48.1 for persistent AF, then note lone in the chart. This distinction matters for insurance and research purposes.
When to See a Specialist
If you experience syncope (fainting), chest pain, or signs of heart failure (swelling, severe shortness of breath), get a referral to an electrophysiologist right away. Redflag symptoms deserve prompt attention.
Risks & Prognosis
Is Lone AF Dangerous?
The short answer: generally low risk, but not zero. The CHADSVASc score, which predicts stroke risk, is usually 0 for lone AF patients, meaning the stroke risk is comparable to the general population. However, recent data suggest a small increase in stroke risk over long periods, especially if other risk factors develop later ().
Life Expectancy
Studies tracking thousands of lone AF patients show that, when properly managed, life expectancy mirrors that of agematched peers. The key is consistent monitoringsome individuals eventually develop structural heart changes, but early detection keeps outcomes favorable.
Can It Go Away?
Yes! About 2030% of people experience spontaneous conversion to normal rhythm within the first year. Lifestyle adjustments, weight loss, and treating sleep apnea dramatically increase the odds of a quiet heart. John, a 45yearold accountant, saw his episodes vanish after shedding 30pounds and using a CPAP machine for sleep apnea.
Treatment Options
Medication Choices
When symptoms bother you, doctors may start with ratecontrol drugsbetablockers (like metoprolol) or calciumchannel blockers (diltiazem). If youre hoping to stay in sinus rhythm, rhythmcontrol meds such as flecainide or propafenone are common for patients without structural heart disease.
Anticoagulation (blood thinners) is a gray area for lowrisk lone AF. Shared decisionmaking is essentialsome patients opt for a lowdose DOAC after discussing the slight stroke risk versus bleeding risk.
NonDrug Therapies
- Catheter ablation: A minimally invasive procedure that isolates the triggers in the pulmonary veins. Success rates in patients under 60 hover around 8090% with low complication risk.
- Lifestyle modifications: Weight management, limiting alcohol (<2 drinks per day), reducing caffeine, regular moderate exercise, and treating sleep apnea.
Emerging Directions
Researchers are exploring genetargeted therapies that could one day prevent AF before it starts. AIdriven ECG analysis platforms are also becoming adept at flagging subtle patterns that predict AF development ().
Everyday Management
4Week Action Plan
- Week1: Get a baseline ECG and Holter. Write down any triggers you notice (caffeine, stress, etc.).
- Week2: Schedule an appointment with a cardiologist. Bring your symptom diary.
- Week3: Implement one lifestyle changeswap nightly wine for sparkling water or start a short walking routine.
- Week4: Review treatment options. If medication is prescribed, set reminders and note any side effects.
Doctor Visit Checklist
- What tests are needed to rule out structural disease?
- Should I start a bloodthinner based on my CHADSVASc score?
- Is catheter ablation a realistic option for me?
- Which lifestyle changes will have the biggest impact?
Support & Resources
Connecting with others can make a huge difference. The American Heart Associations AF Alliance, online patient forums, and local support groups provide a space to share experiences, ask questions, and stay motivated.
Bottom Line
Lone atrial fibrillation is an irregular heartbeat that appears in otherwise healthy adults. While the immediate risk of stroke or heart failure is low, staying on top of monitoring, lifestyle tweaks, andwhen neededmedication or ablation is crucial. Understanding the causes, recognizing the symptoms, and having a clear plan with your doctor can keep you living normally and reduce the chance the rhythm swings back. Got more questions? Talk to your cardiologist, join a patient community, or explore the resources aboveyoure not alone on this journey.
FAQs
What is lone atrial fibrillation?
Lone atrial fibrillation is an irregular heartbeat that occurs in people without underlying heart disease or other common risk factors.
What are the symptoms of lone atrial fibrillation?
Symptoms include heart palpitations, fatigue, dizziness, shortness of breath, and chest pain, though some people have no symptoms at all.
What causes lone atrial fibrillation?
Causes may include genetics, lifestyle factors like alcohol or caffeine, sleep apnea, stress, and sometimes unknown triggers.
How is lone atrial fibrillation diagnosed?
Doctors use an ECG, Holter monitor, or event recorder to detect irregular rhythms and rule out structural heart disease.
What are the treatment options for lone atrial fibrillation?
Treatment includes medications, catheter ablation, lifestyle changes, and sometimes anticoagulants based on individual risk.