Quick answer: Verrucous carcinoma is a slowgrowing, lowgrade cancer that rarely spreads to distant organs, but if you ignore it, it can locally destroy tissue and lead to serious complications. Knowing the real risks, signs, and treatment options lets you act early and keep the disease from becoming a bigger problem.
Why care? Because early detection and proper care give you a very good chance of a full recovery. In the next few minutes well walk through everything you need to know from what the tumor looks like to how its treated in a friendly, nojargon style.
What Is Verrucous Carcinoma
Verrucous carcinoma is a special type of squamouscell carcinoma that shows a warty, cauliflowerlike surface. It most often shows up in the oral cavity (we call that verrucous carcinoma oral), on the genitals, or on the soles of the feet. Unlike classic squamouscell carcinoma, it grows very slowly and almost never spreads through the bloodstream or lymph system.
Think of it as a wellbehaved troublemaker it wants to stay where it started, but it can still cause a lot of local damage if its left unchecked. Pathology outlines describe it as having broad, pushing borders rather than the infiltrative fingers you see in more aggressive cancers.
How Dangerous Is It
The main danger isnt distant metastasis thats incredibly rare but the tumors ability to invade nearby bone, cartilage, or soft tissue. If a lesion sits in the mouth for months, it can erode the jawbone, make swallowing painful, and even affect speech.
When untreated, the lesion can ulcerate, become infected, and lead to significant functional loss. A small case I heard about involved a man who thought his sore was just a persistent canker sore. Six months later, he needed a partial jaw resection because the tumor had eaten into the bone. That story illustrates the balance between lowgrade and locally aggressive.
Who Is At Risk
Risk factors line up with many other headandneck cancers: heavy tobacco use, alcohol consumption, chronic irritation (like illfitting dentures), and in some regions, betelnut chewing. Certain viruses, especially highrisk HPV types, have also been linked to oral verrucous carcinoma.
Age matters, too most patients are over 50, and men are slightly more likely than women. Geographic hotspots (like parts of South Asia) see higher rates because of cultural habits that irritate the oral mucosa.
Symptoms & Signs
Typical oral warning signs include a persistent sore that doesnt heal after two weeks, a white or pinkish warty patch, occasional mild pain, and sometimes a feeling that something is stuck in the mouth. Outside the mouth, you might notice a thickened, wartlike lesion on the genitals or a crusty, raised patch on the foot.
These lesions can look like harmless warts or harmless leukoplakia, which is why a professional exam is essential. If you ever see a spot that keeps coming back after you try to shave it off, thats a good reason to get it biopsied.
Diagnosis & Staging
Doctors start with a thorough visual exam, often using a special light to highlight abnormal tissue. The gold standard is a biopsy either a small incisional sample or a complete excisional one. Pathologists look for the characteristic broad, pushing margins and lack of deep invasion.
If the biopsy confirms verrucous carcinoma, imaging (CT or MRI) may be ordered to see whether the tumor has reached bone or other structures. Staging follows the TNM system, but the T (tumor size) is the most important factor because nodal (N) and metastatic (M) involvement are rare. This is where verrucous carcinoma staging comes into play.
Treatment Options
The cornerstone of treatment is surgical removal. Wide local excision or Mohs micrographic surgery ensures that the entire tumor, plus a margin of healthy tissue, is taken out. Surgery offers the highest cure rates and the lowest chance of recurrence.
Radiation therapy can be used when surgery isnt feasible, but its approached cautiously. Some studies suggest that radiation might trigger a more aggressive transformation in verrucous carcinoma, so doctors weigh the risks carefully.
Adjunct therapies such as topical chemotherapy (e.g., 5fluorouracil) or newer immunotherapies are being explored, especially for patients who cant tolerate surgery. For oral lesions, oral verrucous carcinoma treatment often includes postoperative speech and swallowing rehabilitation to restore quality of life.
| Approach | Success Rate | Typical SideEffects | Recurrence Risk |
|---|---|---|---|
| Wide surgical excision | 8095% | Scarring, temporary difficulty chewing | Low (510%) |
| Mohs surgery | 9098% | Longer procedure, possible tissue loss | Very low (<5%) |
| Radiation therapy | 6075% | Skin changes, potential for secondary malignancy | Higher (1020%) |
According to a study in the , patients who receive surgery as the first line of therapy have the best longterm outcomes.
Survival & Prognosis
The fiveyear verrucous carcinoma survival rate exceeds 80% when the tumor is caught early and treated with clear surgical margins. Factors that can lower survival chances include large tumor size, involvement of bone, and positive margins after surgery.
Recurrence usually shows up within the first two years, so regular followup exams are critical. A typical surveillance schedule might involve a checkup every 36 months for the first two years, then annually.
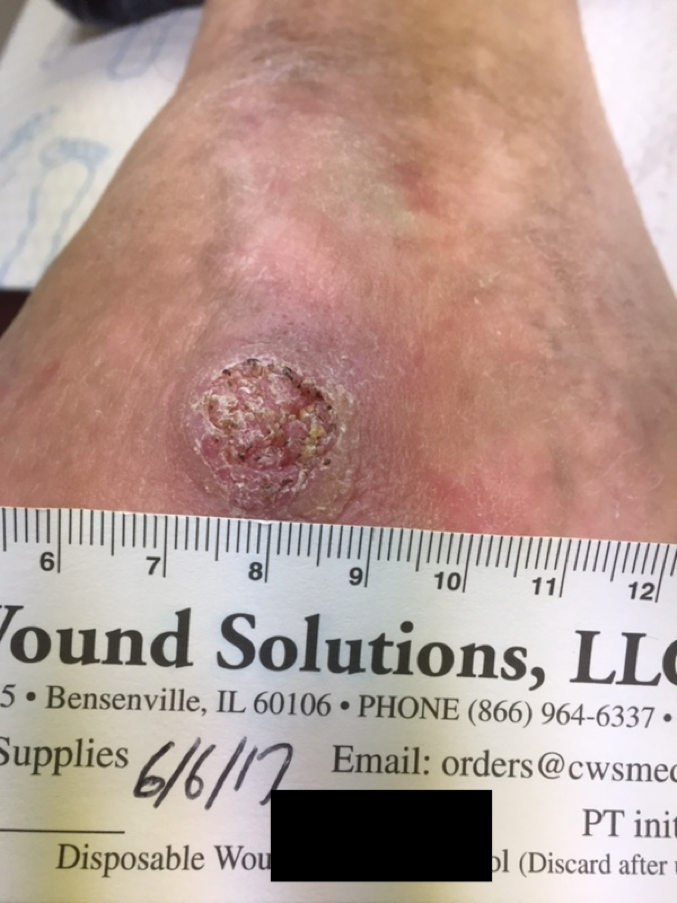
Visual Guide
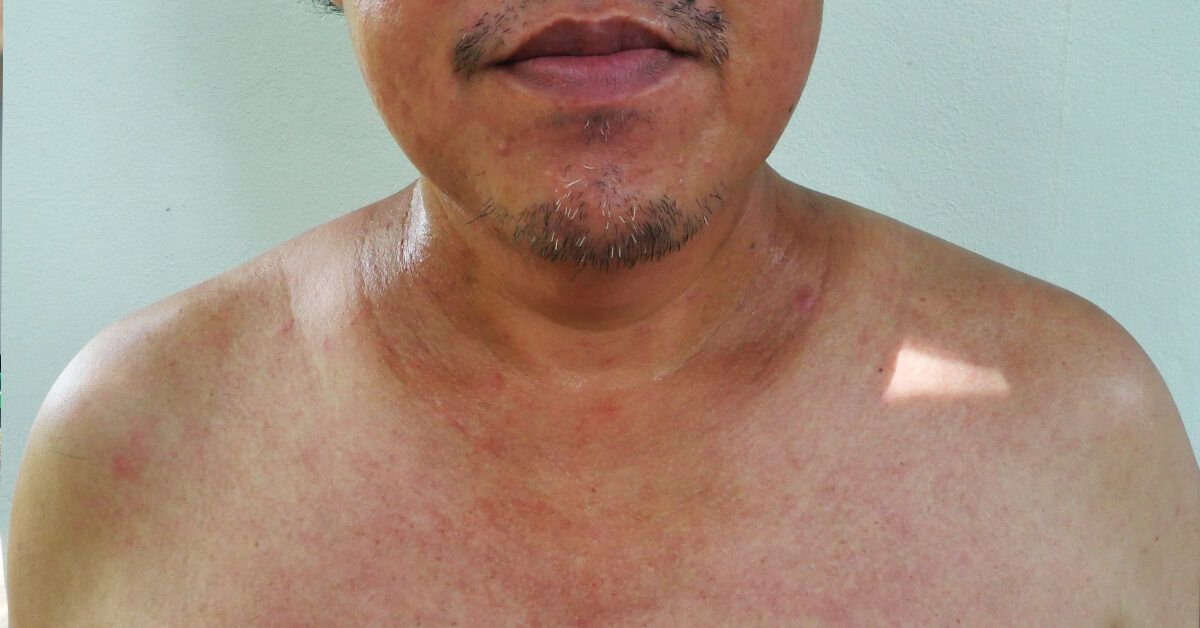
If youre a visual learner, looking at real verrucous carcinoma pictures can help you recognize what to watch for. Clinical photos often show a raised, warty lesion with a slightly irregular border. Theyre typically pink, white, or red, and may have a rough surface that bleeds when scraped.
Comparing those images sidebyside with common warts or leukoplakia highlights the subtle differences: verrucous carcinoma tends to be larger, firmer, and less likely to disappear on its own.
When to Seek Professional Help
Dont wait for a sore to go away on its own. If a lesion hangs around for more than two weeks, especially if its growing, painful, or changing color, schedule an appointment. Bring a list of questions like:
- What are the possible diagnoses?
- Do I need a biopsy?
- What are the surgical options?
- Whats the expected recovery time?
Finding a specialist experienced in headandneck oncology (or oral surgery for oral lesions) makes a big difference. The recommend treatment at highvolume cancer centers for the best outcomes.
Bottom Line Quick Takeaways
- Verrucous carcinoma is lowgrade but can cause serious local damage.
- Early detection + surgery = >80% fiveyear survival.
- Risk factors: tobacco, alcohol, chronic irritation, HPV.
- Watch for any persistent warty lesion that doesnt heal.
- Regular dental or medical checkups are key.
In short, while verrucous carcinoma isnt the most aggressive cancer under the microscope, its quiet nature can lull us into complacency. The best defense is staying vigilant, getting any suspicious spot checked promptly, and following through with recommended treatment. If youve ever wondered whether that odd patch in your mouth or on your skin needs a closer look, nows the time to act. Your future self will thank you.
Feel free to share your thoughts or experiences with verrucous carcinoma in the conversation. Knowledge grows when we talk about it, and every story helps someone else take the right step toward health.
FAQs
What makes verrucous carcinoma dangerous?
Verrucous carcinoma is dangerous mainly because it grows slowly but can locally invade nearby tissues such as bone, cartilage, and soft tissue, causing significant damage and complications if untreated. Its ability to metastasize to distant organs is very rare.
How is verrucous carcinoma usually treated?
Surgery, including wide local excision or Mohs micrographic surgery, is the treatment of choice, offering the highest cure rates and the lowest chance of recurrence. Radiation is used cautiously due to possible risks and is an option when surgery is not feasible.
What are the common symptoms of verrucous carcinoma?
Typical symptoms include a persistent sore or warty lesion that does not heal after two weeks, often with a rough surface, occasional mild pain, and a feeling of something stuck in the mouth or on other affected areas like the genitals or feet.
Who is at higher risk for developing verrucous carcinoma?
Risk factors include heavy tobacco and alcohol use, chronic irritation (such as ill-fitting dentures), betel nut chewing in some regions, and infections with high-risk HPV types. Most patients are over 50 years old, with men being slightly more affected.
What is the prognosis and survival rate for verrucous carcinoma?
The five-year survival rate exceeds 80% with early detection and surgical treatment with clear margins. Larger tumors, bone involvement, or incomplete excision can reduce the prognosis and increase the risk of recurrence.