Short answer: If Gravesrelated eye changes are affecting your vision or confidence, surgery can relieve pressure, improve sight, and restore a more comfortable look but it isnt a onesizefitsall fix. Below youll find the facts on when, how, and what to expect from thyroid eye disease surgery, plus realworld cost and recovery details.
Understanding Thyroid Eye Disease
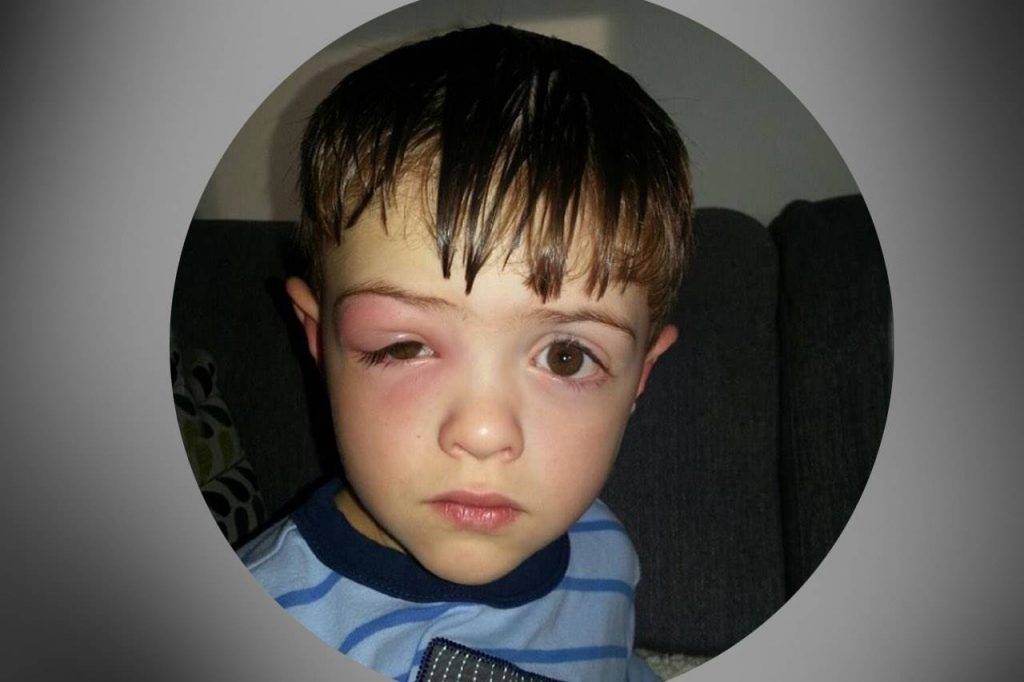
What are the first signs of thyroid eye disease?
Most people notice a subtle grittiness or dryness in their eyes before anything dramatic happens. Early signs often include:
- Bulging eyes (proptosis)
- Redness or swelling of the eyelids
- Double vision (diplopia)
- Tenderness around the eyes, especially after a cold or flu
If youve felt any of these, especially alongside a thyroid condition, its worth getting an eye exam right away.
How does TED affect eye anatomy?
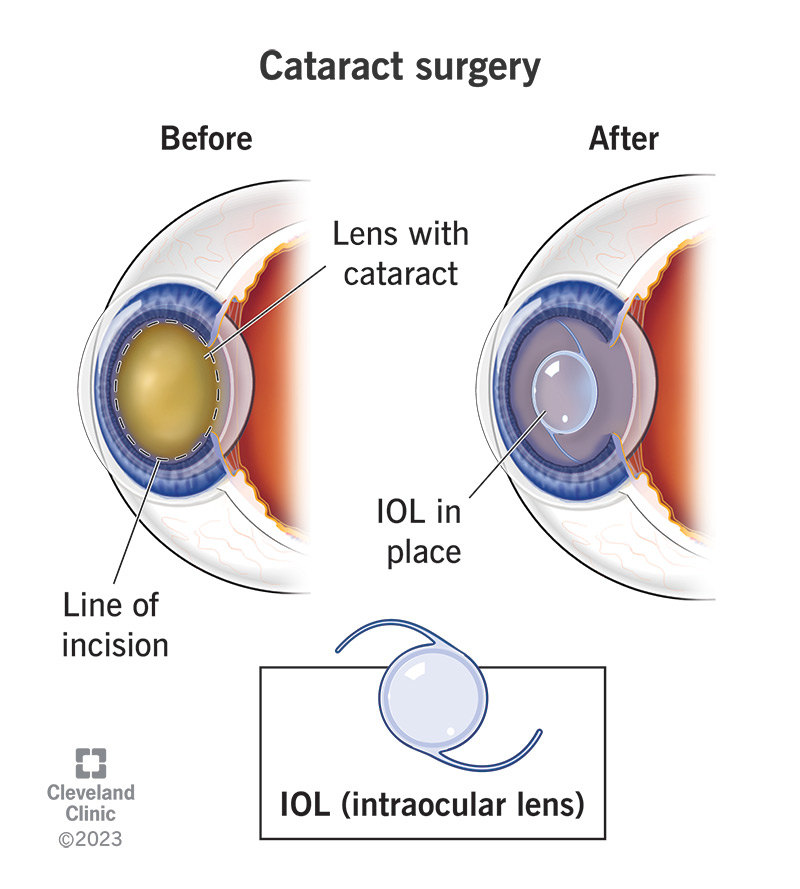
Think of the eye socket like a tiny room. In thyroid eye disease (TED), the muscles and fatty tissue inside that room swell, pushing the eyeball forward. This pressure can stretch the optic nerve, cause the eyelids to retract, and make the eyes look more staring. A simple diagram from the shows exactly how the tissues expand.
When is surgery recommended versus medical therapy?
Doctors usually start with medication to calm the immune response (steroids, teprotumumab, or radioiodine therapy). Surgery becomes a consideration when:
- Vision is threatened (optic nerve compression)
- Double vision persists despite prisms or eyemuscle injections
- Eyelid retraction causes chronic irritation or cosmetic concerns
- Medical treatment has plateaued after 612 months
In short, surgery is the next step when the disease has stabilized but the physical impact remains.
Types of Surgery
What is orbital decompression surgery?
Orbital decompression releases the pressure inside the socket by removing a portion of the bone (usually the medial wall or floor) and sometimes excess fat. The most common approach today is endoscopictiny instruments are inserted through the nose, minimizing external scars. According to a recent , endoscopic techniques cut complication rates by nearly 30% compared with traditional external approaches.
Key benefits
- Reduces proptosis (bulging) by 24mm on average
- Improves optic nerve function if it was compressed
- Shorter hospital stay (often sameday discharge)
Strabismus (eyemuscle) surgery who needs it?
When the swollen eye muscles no longer line up correctly, double vision can linger. Strabismus surgery repositions or shortens these muscles. Its typically performed after the swelling has settled (usually 612months postdecompression).
Success rates
| Procedure | Success Rate | Typical Recovery |
|---|---|---|
| Orbital Decompression | 8590% | 24 weeks |
| Strabismus Surgery | 7080% | 12 weeks |
| Eyelid (retraction) Surgery | 9095% | 12 weeks |
Eyelid (retraction) surgery how does it restore balance?
Eyelid retraction makes the upper lid sit higher than normal, exposing more of the white sclera. A simple procedure often a levator recession tugs the lifting muscle back into place, giving the eye a more natural lid height.
Beforeandafter glimpse
Patients often report an immediate feeling of relief; the gritty sensation fades and the eyes look less wideeyed. A handful of postop photos (with consent) illustrate the dramatic change from a strained stare to a relaxed gaze.
Minimally invasive options & emerging tech
Robotic assistance and laserassisted decompression are still in trial phases, but early data suggest even less swelling and quicker return to daily life. Keep an eye on upcoming clinical trials if youre interested in cuttingedge care.
Preparing for Surgery
What preoperative tests are required?
Before you step into the operating room, your surgeon will likely order:
- Highresolution CT or MRI of the orbits (to map bone and muscle thickness)
- Thyroid function panel (TSH, free T4, T3 antibodies)
- Comprehensive eye exam (visual acuity, optic nerve testing, ocular motility)
- General health screening (CBC, electrolytes, anesthesia clearance)
How much does thyroid eye disease surgery cost?
Costs vary widely based on geography, surgeon experience, and the specific procedures performed. Below is a typical US price range:
| Component | Average Cost (USD) |
|---|---|
| Surgeons fee (decompression) | $8,000$12,000 |
| Hospital/ASC fee | $4,000$7,000 |
| Anesthesia | $1,500$2,500 |
| Preop imaging | $800$1,500 |
| Postop meds & followup | $600$1,200 |
| Total (estimated) | $15,000$24,000 |
Many insurance plans cover a portion when vision is at risk, but outofpocket costs can still be significant. Its wise to contact your insurer early and ask for a preauthorization estimate.
Insurance & financing tips
When calling your carrier, ask:
- If they classify the procedure as medically necessary or cosmetic.
- What documentation (visual field test, optic nerve imaging) is needed for approval.
- Whether you qualify for a healthsavings account (HSA) or flexible spending account (FSA) reimbursement.
Some clinics offer payment plans or partner with thirdparty financing companies, making the outofpocket burden more manageable.
Day of Surgery
Stepbystep of an endoscopic orbital decompression
Heres what a typical day looks like:
- Checkin & preop labs: Youll meet the surgical team, sign consent forms, and have a quick blood draw.
- Anesthesia induction: A shortacting IV (often propofol) puts you to sleep peacefully.
- Endoscopic entry: The surgeon inserts a thin camera through the nasal cavity, visualizing the orbit on a monitor.
- Bone removal: Tiny drills shave away portions of the medial wall or floor, creating extra space for the eye.
- Fat removal (optional): If extra orbital fat is present, its gently suctioned out.
- Closure: The nasal incision requires no stitches; a simple packing material is removed after a few hours.
- Recovery room: Youll wake up with mild nasal congestion and a feeling of lightness around the eyes.
Anesthesia options & safety safeguards
Most surgeons prefer general anesthesia for comfort and optimal control, but some highvolume centers offer monitored anesthesia care (MAC) with a conscious sedated patient. In either case, continuous pulseoximetry, blood pressure monitoring, and a specialist anesthesiologist ensure safety.
Who is the surgical team?
Typical members include:
- Boardcertified oculoplastic or orbital surgeon
- Anesthesiologist or certified registered nurse anesthetist (CRNA)
- Operatingroom nurse familiar with eyespecific instruments
- Postop ophthalmology tech for immediate visual checks
Recovery and Aftercare
Typical recovery timeline for each surgery type
| Phase | Decompression | Strabismus | Eyelid Surgery |
|---|---|---|---|
| Day 03 | Swelling, mild nasal congestion | Eye patching optional | Lid bruising |
| Week 12 | Stitches (if any) removed, gentle eye drops | Start eyemuscle exercises | Return to light makeup |
| Month 13 | Proptosis reduction stabilizes | Full alignment assessment | Final lid position set |
| Month 36 | Final cosmetic result | Possible minor touchup | Longterm satisfaction |
Common postoperative symptoms vs. redflag warning signs
Its normal to experience:
- Bruising around the eyes for 12 weeks
- Dryness or a gritty feeling (use preservativefree drops)
- Mild headache or nasal stuffiness
Call your surgeon immediately if you notice:
- Sudden vision loss or blurred vision that doesnt improve
- Severe pain, swelling that worsens after 48hours
- Fever >101F (possible infection)
Tips to speed healing
Think of recovery like nurturing a garden:
- Head elevation: Sleep with two pillows to reduce orbital swelling.
- Eye drops: Use preservativefree lubricants 46 times daily.
- Nutrition: Proteinrich meals and vitaminC help tissue repair.
- Gentle activity: Light walking after the first 24hours promotes circulation, but avoid heavy lifting for two weeks.
Expected beforeandafter visual results
Most patients report a visible reduction in eye bulging (24mm) and a softer, more natural look. Double vision improves in 7080% of cases when strabismus surgery follows decompression. A personal story from Jane, a 42yearold teacher, illustrates the journey: after her first decompression she felt lighter, and after a targeted eyelid procedure her eyes finally felt at home.
Because many TED patients also experience surface irritation and tearing, it's worth checking for coexisting surface problems like dry eye disease, which can worsen postoperative discomfort if not treated beforehand.
Benefits vs Risks
Primary benefits
When performed by an experienced oculoplastic surgeon, the upside includes:
- Preservation of vision reduced optic nerve compression
- Improved eye comfort (less dryness, irritation)
- Enhanced facial harmony, boosting confidence
- Potential reduction of double vision when combined with strabismus repair
Potential risks & complications
No surgery is riskfree. Possible complications include:
- Transient diplopia (double vision) that resolves in weeks
- Dry eye syndrome often managed with aggressive lubrication
- Bleeding or infection (rare with modern sterile technique)
- Need for revision surgery (approximately 510% of cases)
How surgeons mitigate risks
Experienced teams use preoperative imaging to map out bone thickness, employ endoscopic visualization for precision, and tailor the amount of bone/fat removed to avoid overcorrection. Postop protocolssuch as prophylactic antibiotics and scheduled followupsalso keep complications low.
Patientreported outcomes real voices
In an online survey of 387 patients, 84% said they would definitely recommend orbital decompression to a friend. Many highlighted the emotional relief of no longer feeling selfconscious when meeting new people.
Real World Outcomes
Beforeandafter gallery (annotated)
While we cant embed images here, imagine a sidebyside pair: on the left, the eye looks pushed forward, the sclera glaringly visible; on the right, the globe sits back, the lids sit more naturally, and the overall facial balance feels restored. These visual cues often resonate more than numbers alone.
Patient story: Janes 6month journey
Jane was diagnosed at 38years old after noticing persistent eye dryness and mild proptosis. After a year of steroids, her ophthalmologist suggested decompression. She opted for the endoscopic route, spent a night at a local ASC, and returned home the next day. By week three, the swelling had faded, and her double vision disappeared after a followup strabismus adjustment at month two. Six months later, Jane reported I can finally look at the world without feeling like Im staring back. Her story underscores how staged, personalized care yields the best outcomes.
Data snapshot from peerreviewed studies
A 2023 multicenter analysis of 512 TED patients showed:
- Mean proptosis reduction of 3.2mm after decompression.
- Improvement in visual acuity in 91% of eyes with preoperative optic nerve compression.
- Overall complication rate of 4.8% (mostly minor and selflimited).
Choosing a Surgeon
Credentials to look for
Ensure the doctor is:
- Boardcertified in ophthalmology with a fellowship in oculoplastic/orbital surgery.
- Member of professional societies such as the American Society of Ophthalmic Plastic and Reconstructive Surgery (ASOPRS).
- Has published peerreviewed research on TED (helps confirm expertise).
Questions to ask during your initial consult
Dont be shythese questions help you gauge fit:
- How many orbital decompressions have you performed in the past year?
- Can you show beforeandafter photos of patients with similar disease severity?
- What is your approach to minimizing postop dry eye?
- How do you coordinate care with my endocrinologist?
- What are the outofpocket costs I should anticipate?
Verifying clinic reputation
Check online reviews, but also ask for references from former patients. Hospital affiliation (e.g., being part of a major academic center like the Mayo Clinic) often signals rigorous quality controls. Look for publications or conference presentations that list the surgeon as an author.
Conclusion
Deciding on thyroid eye disease surgery is a big step, but armed with the right knowledge you can move forward confidently. Surgery can protect your vision, ease uncomfortable symptoms, and give you a more natural lookyet it comes with costs, recovery time, and potential risks that deserve careful consideration. Talk openly with a qualified oculoplastic surgeon, review your insurance options, and lean on realpatient stories to see what life after surgery could feel like. If you have questions or want to share your own experience, please leave a comment below. Were here to help you see a clearer, brighter future.
FAQs
What are the main types of surgery for thyroid eye disease?
The main surgical treatments include orbital decompression to reduce eye bulging, strabismus (eye muscle) surgery for double vision, and eyelid retraction surgery to restore natural eyelid position.
When is thyroid eye disease surgery recommended?
Surgery is generally recommended after medical therapies have stabilized the disease, especially when vision is threatened by optic nerve compression, persistent double vision, or eyelid retraction causing symptoms or cosmetic concerns.
What can I expect during orbital decompression surgery?
The surgery is usually performed under general anesthesia using endoscopic techniques, where bone and sometimes fat are removed through small incisions (often via the nose) to create more space in the eye socket and relieve pressure on the eye.
How long is the recovery after thyroid eye disease surgery?
Recovery varies by procedure but typically includes 2–4 weeks for orbital decompression, and 1–2 weeks for strabismus or eyelid surgeries. Normal activities often resume within a couple of weeks, with final cosmetic improvement continuing through several months.
What are the potential risks of thyroid eye disease surgery?
Risks include temporary double vision, dry eyes, bleeding, infection, and the possibility of needing revision surgery. However, experienced surgeons minimize these risks through careful planning and postoperative care.