The short answer is that it depends. Modern imaging can spare many men from an invasive procedure, yet in other situations the tissue sample is still the goldstandard for confirming cancer. In the next few minutes well walk through what the MRI tells us, when it can replace a biopsy, and how to make a balanced decision that feels right for you.
Quick Bottom Line
Short answer
Sometimes a biopsy is still required after an MRI, especially when the scan shows suspicious (highrisk) lesions. However, a lowrisk or negative MRI often allows doctors to adopt a watchful waiting approach, sparing you the discomfort and risks of a biopsy.
Key takeaways
- Negative or PIRADS12 MRI = strong case for monitoring instead of immediate biopsy.
- PIRADS45 lesions = biopsy usually recommended, often MRItargeted.
- Both MRI and biopsy have strengths; the best strategy blends them based on your individual risk factors.
How MRI Works
Types of prostate MRI
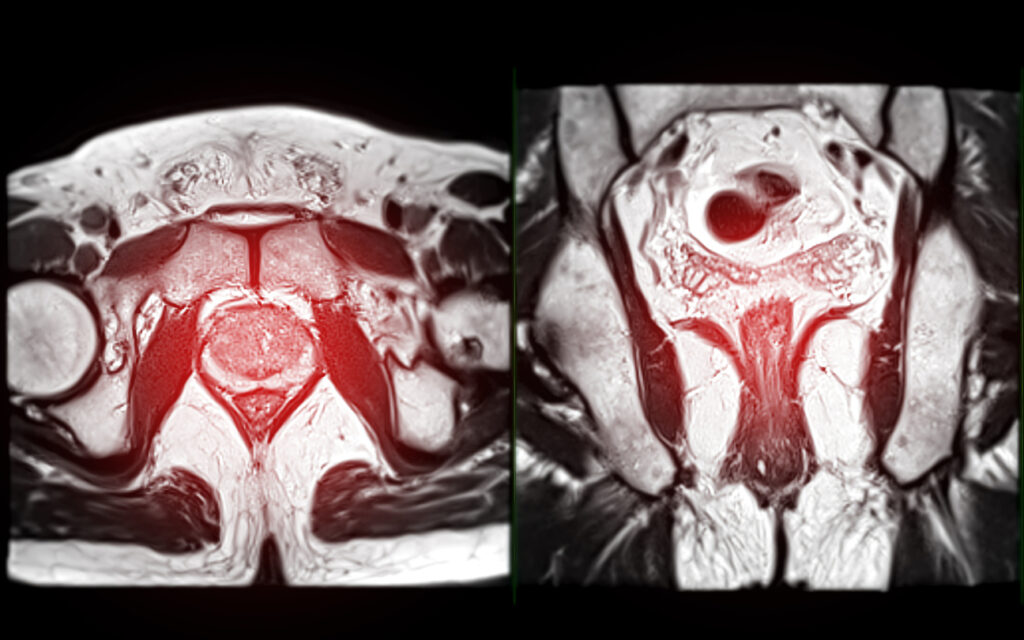
The most common protocol is multiparametric MRI (mpMRI), which combines anatomic, diffusionweighted, and dynamic contrastenhanced sequences. This triplelook gives radiologists a detailed map of the gland, highlighting areas that might harbor cancer.
PIRADS scoring (15)
Radiologists assign a PIRADS (Prostate ImagingReporting and Data System) score from 1 to 5:
| Score | Risk Interpretation |
|---|---|
| 12 | Very low to low suspicion; cancer unlikely. |
| 3 | Intermediate suspicion; further evaluation needed. |
| 45 | High suspicion; cancer likely. |
This system directly answers the related query prostate mri results 1-5 and guides the next step.
Accuracy of MRI
When youre wondering how accurate is MRI in diagnosing prostate cancer?, recent studies give us a clear picture. A large multicenter trial published in reported a sensitivity of 93% and a negative predictive value (NPV) of 96% for detecting clinically significant cancer in men with PIRADS12 scans.
Comparison table
| Metric | mpMRI (PIRADS3) | Standard systematic biopsy |
|---|---|---|
| Sensitivity | 8893% | 7080% |
| Specificity | 7080% | 6070% |
| NPV (negative result) | 96% | 85% |
| PPV (positive result) | 5060% | 4555% |
In plain language, a clear MRI is reassuring, but a positive MRI still benefits from a tissue check.
When MRI Can Replace Biopsy
Lowrisk MRI results
If your scan comes back as PIRADS1 or2, the chance of missing a clinically important cancer is tiny. According to an , men with lowrisk MRI were safely monitored without immediate biopsy, and only 2% later required a cancerdirected intervention.
Who may skip biopsy
- PSA under 10ng/mL
- No family history of aggressive prostate cancer
- Age<70 and good overall health
- PIRADS12 MRI
When these boxes are ticked, a watchful waiting or active surveillance plan is usually the most patientfriendly route.
When Biopsy Is Still Needed
Highrisk MRI findings
When the radiology report reads PIRADS4 or5, the odds tip heavily toward cancer. The question which is better MRI or biopsy for prostate cancer? becomes less about choice and more about partnership: MRI tells us where to look, biopsy tells us what is there.
Limitations of MRI
Even the best scans can miss something. Small lesions (<5mm), cancers in the anterior gland, or artifacts from bowel gas can lead to falsenegatives. A systematic review in found that about 510% of clinically significant cancers were not flagged by mpMRI.
Biopsy methods after MRI
Once a suspicious area is identified, doctors usually opt for an MRItargeted biopsyeither fusionguided (software merges MRI with realtime ultrasound) or inbore MRIguided. These approaches increase cancer detection rates while requiring fewer needle cores.
Fusionguided vs systematic
- Fusionguided: Higher yield for PIRADS45 lesions, fewer cores, less discomfort.
- Systematic: Samples the entire gland, catching cancers that MRI might miss.
Many urologists now perform a combined approachtargeted plus a limited systematic setto maximize confidence.
Risks and Benefits
Benefits of avoiding biopsy
Skipping an unnecessary biopsy spares you from infection, bleeding, urinary discomfort, and the anxiety that comes with a hospital procedure. A 2020 analysis in the noted a 30% reduction in biopsyrelated complications when MRI was used as the gatekeeper.
Reduced infection, anxiety
Even a simple transrectal biopsy can introduce bacteria, leading to prostatitis or sepsis. Avoiding that step when the MRI is reassuring means fewer antibiotics, less time off work, and a smoother mental road.
Potential harms of missing cancer
On the flip side, dont get a prostate biopsy isnt a blanket rule. Delaying tissue confirmation in a highrisk scenario could allow an aggressive tumor to grow unchecked. Studies show that a delayed diagnosis (beyond 612months) can modestly increase the chance of requiring more extensive treatment later.
Statistics on delayed treatment
The same JAMA Oncology paper reported that men who postponed biopsy after a PIRADS4 scan had a 12% higher rate of needing radical therapy within two years compared with those who proceeded promptly.
Sideeffects of biopsy
Common, usually mild, sideeffects include:
- Bleeding from the rectum or urine (1015%)
- Temporary urinary urgency or difficulty (510%)
- Lowgrade fever or prostatitis (12%)
Serious infection is rare (<0.5%) but not impossible, especially with traditional transrectal routes.
RealWorld Experiences
Case study: John
John, 62, went in for a routine PSA check that came back at 6ng/mL. His mpMRI scored PIRADS2. After a hearttoheart chat with his urologist, they chose active surveillancerepeat PSA every six months, a followup MRI in a year. Two years later, his PSA stayed stable, and the MRI remained lowrisk. John avoided a biopsy, the anxiety of a cancer label, and the occasional postprocedure soreness.
What his doctor asked
- Do you have any urinary symptoms right now?
- How comfortable are you with regular monitoring versus an invasive test?
- What are your personal goals if a cancer were foundaggressive treatment or a more measured approach?
These questions helped shape a plan that felt right for John, showing how shared decisionmaking can turn data into confidence.
Expert Guidance
What specialists say
Dr. Maya Patel, boardcertified radiologist at a major academic center, explains: MRI has become the first line for men with elevated PSA because it dramatically reduces unnecessary biopsies. But we never abandon the biopsy when the imaging points to a highrisk area; the pathology still tells us the Gleason score, which drives treatment.
Guidelines and sources
- National Comprehensive Cancer Network (NCCN) recommends MRI before initial biopsy for most men.
- American Urological Association (AUA) advises using PIRADS to stratify the need for tissue sampling.
- Recent NEJM trial (2022) showed MRItargeted biopsies detected 30% more clinically significant cancers than systematic biopsies alone.
These endorsements give weight to the balanced approach weve been outlining.
Practical Next Steps
Decision flowchart
Heres a quick mental map you can follow after your MRI results:
- PIRADS12: Discuss active surveillance with your doctor. No immediate biopsy needed.
- PIRADS3: Consider a repeat MRI in 612months or a targeted biopsy if you have additional risk factors.
- PIRADS45: Schedule an MRItargeted biopsy. Ask whether a combined systematic approach is recommended.
Preparing for MRI
Good preparation can improve image quality:
- Empty your bladder 30minutes before the scan.
- Follow any fasting instructions (usually no food for 4hours).
- Tell the technologist about any metal implants.
Questions for your doctor
- Based on my PIRADS score, how likely is it that I have a clinically significant cancer?
- If we decide on a biopsy, will it be MRItargeted, systematic, or both?
- What are the exact risks of infection or bleeding in my case?
- How often should we repeat imaging or PSA testing if we choose surveillance?
Having these questions ready shows youre engaged and helps your physician give you the most personalized answer.
Conclusion
In short, an MRI is a powerful ally that can spare many men from an unnecessary biopsy, but it isnt a universal replacement. If your scan is lowrisk, monitoring is often safe and less stressful. If the MRI flags suspicious lesions, a targeted biopsy remains the best way to confirm and grade the cancer.
Take the time to review your results, ask the right questions, and weigh both benefits and risks. Your health journey is uniquepartner with a trusted urologist, stay informed, and remember that youre not alone in navigating these decisions.
For patients concerned about recovery after any prostate procedure, practical tips on post op recovery can help set expectations and speed safe return to activity.