Ever wonder why a tiny brown speck sometimes drifts across your vision? Thats often iris pigment dispersion tiny pigment particles peeling off the back of your iris and floating around the front of the eye. In most folks its harmless, but when those particles clog the eyes drainage system they can nudge the pressure up and lead to pigmentary glaucoma.
Below youll find everything you need to know, from the subtle signs you might be missing to the best ways to keep your eyes healthy. Think of this as a friendly chat over coffee no jargon, just clear answers and a few reallife stories to make it stick.
Understanding the Condition
What Is Pigment Dispersion Syndrome?
Pigment Dispersion Syndrome (PDS) is the umbrella term for the whole process of pigment shedding. When we talk about iris pigment dispersion were zeroing in on that exact moment the pigment flakes off the iris. The American Academy of Ophthalmology notes that PDS is relatively common in young, often myopic men, but anyone can develop it.
How Does Pigment Move Inside the Eye?
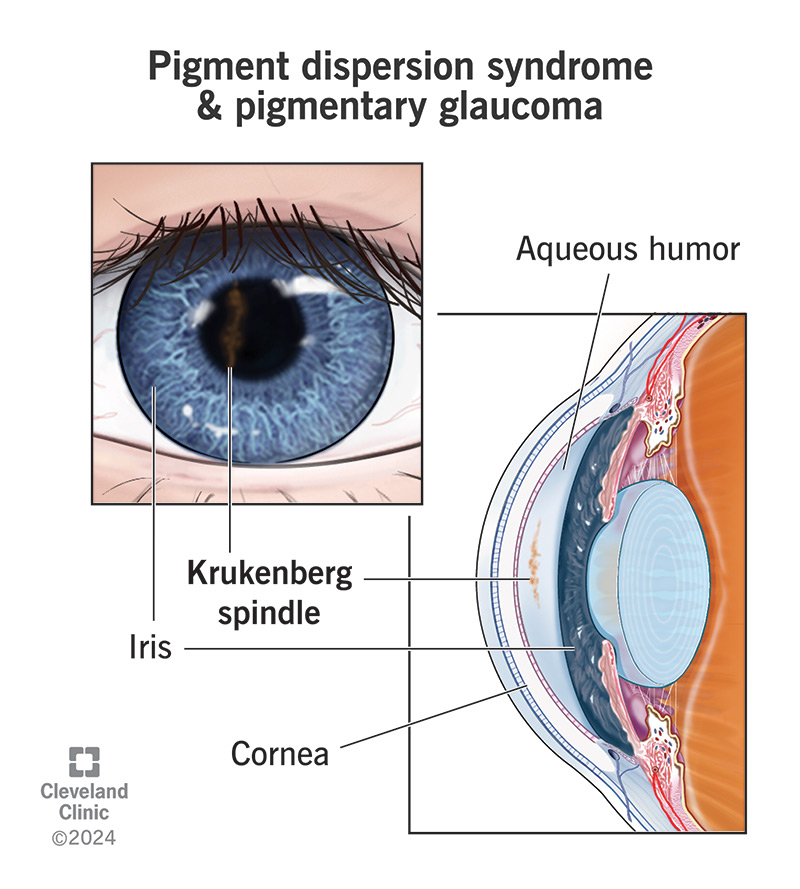
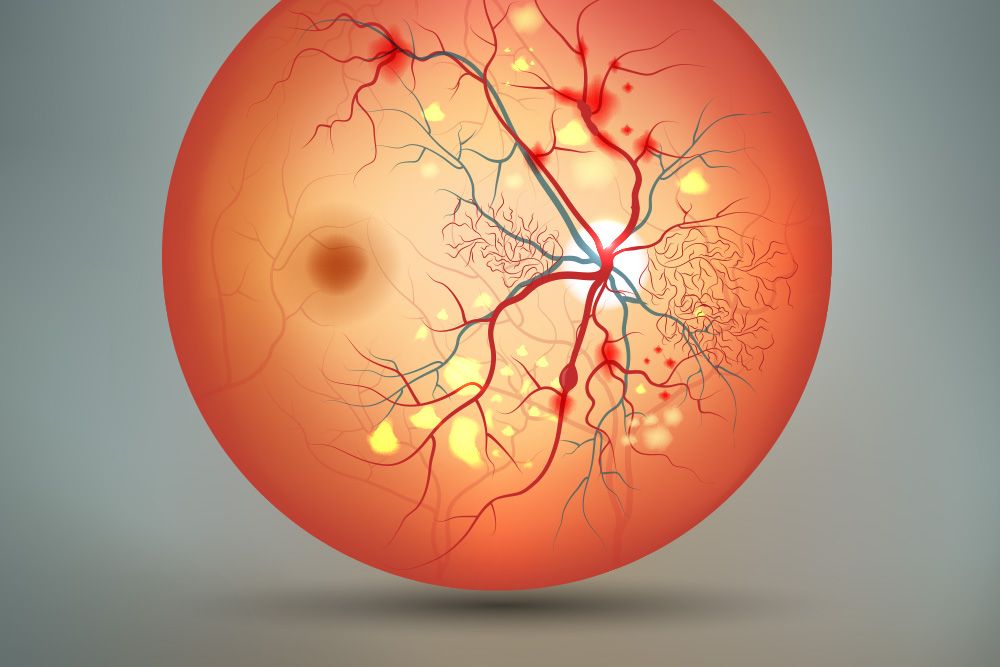
Picture the iris as a delicate paintstroke at the back of a window. Every time the iris rubs against the eyes zonules (the tiny fibers that hold the lens in place), a few microscopic specks of pigment can flake off. Those specks then drift in the aqueous humor the clear fluid that circulates in the front of the eye and may settle on the cornea or, more worryingly, in the trabecular meshwork where fluid drains out.
Who Is Most Likely to Develop It?
If youre in your 20s or 30s, have moderate to high myopia, and maybe enjoy activities that put your head upsidedown (think rock climbing or yoga inversions), youre in the higherrisk crowd. Some researchers even suggest a genetic hook, and a few recent studies hint at an autoimmune component ( found elevated HLADR markers in a subset of patients).
Difference Between PDS and Pigmentary Glaucoma
Not all pigment dispersion leads to glaucoma, but when enough pigment blocks the drainage pathways, intraocular pressure (IOP) can climb. That shift from just pigment to pigmentary glaucoma is what can threaten vision over time.
| Feature | Pigment Dispersion Syndrome | Pigmentary Glaucoma |
|---|---|---|
| Primary Issue | Pigment flakes off iris | Pigment blocks outflow IOP |
| Vision Loss Risk | Low (if monitored) | High (if untreated) |
| Typical IOP | 21mmHg | >21mmHg, often fluctuating |
| Management | Observation, lifestyle tweaks | Medications, laser, surgery |
Spotting the Signs
Common Symptoms You Might Notice
Most people first notice a faint brownish smear on the cornea or a sudden flare of light sensitivity. Others report occasional floaters that look different from the usual cobweb type these are pigment particles, not vitreous debris.
Clinical Signs an Eye Doctor Looks For
During a slitlamp exam an ophthalmologist may see a Krukenberg spindle a vertical, spindleshaped pigment deposit on the cornea. Theyll also check for midperipheral iris transillumination defects (tiny bright spots you cant see without the right equipment) and a pigmented trabecular meshwork.
When Do Floaters Appear?
Unlike the classic spider web floaters that come from the vitreous, pigment dispersion floaters are darker and may move more slowly. Mike, a 32yearold climber, first thought his new specks were dust until a routine eye exam revealed a classic Krukenberg spindle.
Light Sensitivity & Glare
The dispersed pigment scatters incoming light, making bright environments feel harsh. Simple fixes like polarized sunglasses or adjusting screen brightness can bring instant relief.
Why It Happens
Primary Mechanical Causes
The iris can literally rub against the zonules during everyday eye movements. Over time, that friction can loosen pigment cells a bit like a sandpaper rubbing against a painted surface.
Secondary/Contributing Factors
High myopia stretches the eye, bringing the iris closer to the zonules. Trauma (even a mild eye poke), certain medications, and intense physical activity that forces the eye into unusual positions can all accelerate pigment release.
Systemic Links Autoimmune Connection
While the exact link is still under investigation, some patients with autoimmune conditions (like rheumatoid arthritis) show a higher prevalence of PDS. The theory is that systemic inflammation may alter the pigment epitheliums stability, making it easier for pigment to dislodge.
AgeRelated Pigment Changes
As we age, the iris naturally darkens and the pigment may become more loosely held. Distinguishing normal agerelated changes from pathological dispersion is why regular eye exams are so valuable.
RealWorld Case Study (Experience)
Consider Jenna, 45, who ignored mild glare for years. A sudden spike in IOP pushed her into pigmentary glaucoma, requiring laser trabeculoplasty. Had she been monitored when the pigment first appeared, treatment could have stayed at the medication stage, sparing her a procedure.
Diagnosis Essentials
Eye Exam Basics
A comprehensive eye exam includes a slitlamp check, gonioscopy (looking at the angle where fluid drains), and a dilated fundus exam to view the retina and optic nerve.
Imaging & Tests
Modern practices often employ Anterior Segment OCT (Optical Coherence Tomography) to visualize pigment deposits on the iris and in the drainage meshwork. Regular IOP measurements and visual field tests help catch early glaucoma signs before vision loss occurs.
When to See an Ophthalmologist
If you notice new floaters, increasing glare, or a change in night vision, schedule an appointment within a week. Rapid IOP rise or sudden vision changes are redflag symptoms that need urgent attention.
Treatment Options
Observation & Lifestyle Adjustments
For many, simply watching the condition and making smart lifestyle tweaks does the trick. Aim for routine eye checks every 612 months, avoid extreme headdown positions for prolonged periods, and keep myopia under control with corrective lenses.
Medications (Pigment Dispersion Syndrome Treatment)
When IOP creeps up, doctors often start with prostaglandin analogues (like latanoprost) or betablockers. If one class isnt enough, a carbonic anhydrase inhibitor can be added. These meds help the eye drain fluid more efficiently.
Laser Therapy
Laser iridotomy creates a tiny hole in the iris, relieving the friction that pushes pigment out. Its a quick, outpatient procedure with a high success rate. If pigment has already built up in the drainage system, laser trabeculoplasty can open the meshwork further.
Surgical Interventions
When meds and lasers dont control pressure, surgery may be necessary. Options include trabeculectomy (creating a new drainage route), tube shunts, or minimally invasive glaucoma surgery (MIGS) which offers faster recovery.
DecisionTree Flowchart (Treatment Path)
Imagine a simple flow: mild PDS watchful waiting IOP rises start meds meds fail laser iridotomy or trabeculoplasty still high IOP surgery. This stepbystep approach helps keep treatment personalized and not overly aggressive.
Living with Iris Pigment Dispersion
Daily EyeCare Routine
Wear UVblocking sunglasses whenever youre outdoors, especially on bright days. Take screen breaks using the 202020 rule (every 20 minutes, look at something 20 feet away for 20 seconds) to reduce glare fatigue.
Monitoring Your Vision at Home
Keep a simple checklist: Are you seeing new specks? Is glare getting worse? Do you notice more difficulty at night? Jot these notes down and share them with your eye doctor at each visit.
Nutrition & Systemic Health
Foods rich in antioxidants leafy greens, berries, fish high in omega3s support overall eye health. Managing blood pressure and keeping inflammatory conditions in check also helps keep pigment dispersion from worsening.
When to Reach Out for Help
Support groups like the Glaucoma Foundations online community can provide comfort and practical tips. If you ever feel uncertain about a symptom, a quick call to your ophthalmologist can give peace of mind.
Conclusion
Iris pigment dispersion might sound technical, but at its core its just tiny pigment particles that can, if left unchecked, affect how well your eyes drain fluid. By recognizing the subtle signs, staying on top of regular eye exams, and embracing a balanced mix of lifestyle tweaks, medication, or laser treatment when needed, you can keep the risk of pigmentary glaucoma low and protect the vision you love.
Have you experienced any of these symptoms, or do you have a story about managing pigment dispersion? Share your thoughts in the comments below were all in this together. And remember, a quick checkup today could save you a lot of worry tomorrow.
FAQs
What are the early signs of iris pigment dispersion?
The first clues are often tiny brown specks that drift across vision, a subtle glare in bright light, or a faint brown‑gray line (Krukenberg spindle) on the cornea seen during an eye exam.
How is iris pigment dispersion diagnosed by an eye doctor?
A slit‑lamp examination reveals pigment on the cornea and iris transillumination defects. Gonioscopy checks the drainage angle, and imaging such as Anterior Segment OCT can visualize pigment deposits.
Can lifestyle changes prevent pigmentary glaucoma?
While you can’t stop pigment from shedding completely, avoiding prolonged inverted positions, protecting eyes from trauma, and keeping myopia corrected can reduce the amount of pigment that reaches the drainage meshwork.
What treatment options are available for increased eye pressure caused by pigment dispersion?
Initial management usually involves prostaglandin analogues or beta‑blockers. If pressure remains high, laser iridotomy or trabeculoplasty may be performed, and surgery is reserved for resistant cases.
How often should I have my eyes checked if I have pigment dispersion syndrome?
Most specialists recommend a comprehensive eye exam every 6–12 months to monitor intra‑ocular pressure, optic nerve health, and any progression toward glaucoma.