In the next few minutes we'll walk through why spine inflammation happens, how to spot it, what doctors look for on an MRI, and the full spectrum of inflammation of the spine treatment from simple NSAIDs to cutting-edge biologics and, when necessary, surgery. Think of this as a friendly chat over coffee, with a dash of science and a lot of empathy.
What Causes Inflammation?
Medical conditions that spark it
Inflammation isn't just a random ache. It often stems from underlying diseases such as:
- ankylosing spondylitis remission
- Rheumatoid arthritis
- Psoriatic arthritis
- Infections (like discitis)
- Trauma or repetitive microinjuries
When any of these irritate the spinal joints, the body launches an inflammatory response, leading to swelling, pain, and reduced mobility.
Lifestyle factors that add fuel
Even if you're not diagnosed with an autoimmune disease, everyday habits can light the fire:
- Poor posture while working on a laptop
- Long periods of sitting without breaks
- Carrying extra weight, especially around the abdomen
- Lack of regular, low-impact movement
These mechanical stressors strain the lumbar discs and facet joints, inviting inflammation.
Quick-look comparison table
| Condition | Typical Trigger | Age Range | Red-Flag Symptoms |
|---|---|---|---|
| Ankylosing spondylitis | Genetic (HLA-B27) | Late teens30s | Morning stiffness >30min |
| Rheumatoid arthritis | Autoimmune | 3060 | Symmetrical joint swelling |
| Mechanical strain | Poor ergonomics | All ages | Localized pain, worsens with activity |
Expert note: Dr. Elena Ruiz, a board-certified rheumatologist, says early identification of the underlying cause can dramatically change the treatment trajectory and improve long-term outcomes.
Spotting the Signs
General warning signs
When inflammation hits the spine, you'll often feel a deep, dull ache that doesn't fully disappear with rest. Morning stiffness that lasts more than 30 minutes, especially after a night of sleep, is a classic clue.
Lumbar-specific symptoms
If the lower back is involved, you might notice:
- Persistent lower-back pain that radiates to the hips or thighs
- Numbness or tingling down the legs (sometimes called sciatica)
- Reduced flexibility when you try to bend forward
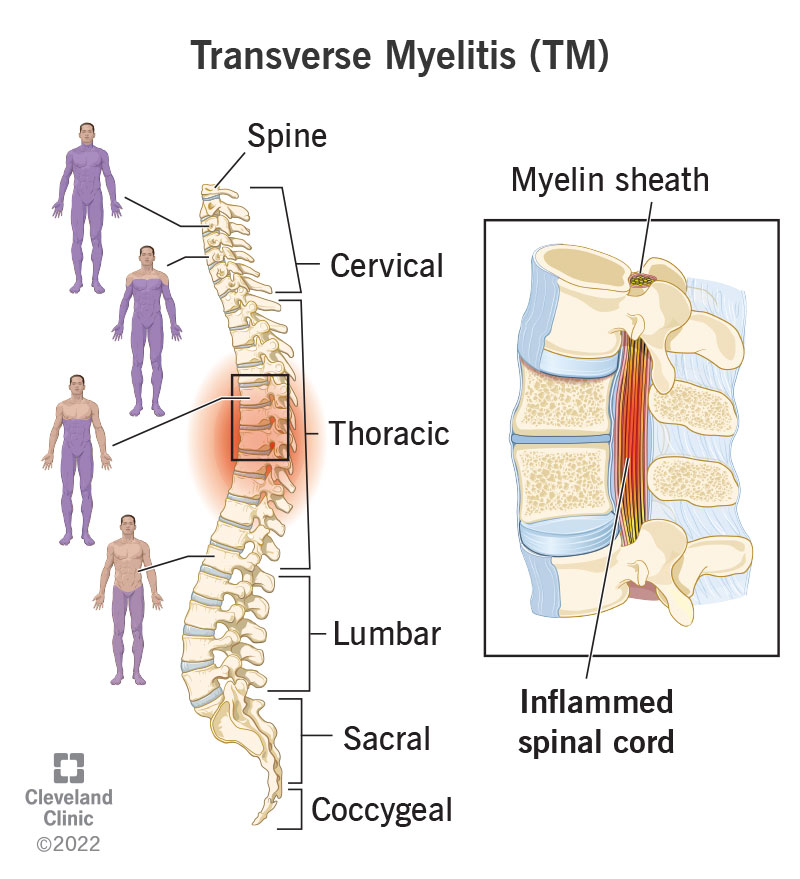
What the MRI reveals
An MRI is the gold standard for visualizing inflammation. Look for:
- Bone marrow edema (bright spots on T2-weighted images)
- Contrast enhancement of the vertebral bodies or facet joints
- Signs of disc degeneration that may coexist
According to , the presence of edema on an MRI strongly correlates with active inflammation.
MRI image checklist
- Did the radiologist comment on edema or inflammation?
- Are there any signs of infection such as abscess formation?
- Is there evidence of nerve root compression?
Diagnosing Inflammation
Clinical evaluation
Your doctor will start with a detailed history when the pain began, what makes it worse, and any extra-articular symptoms like eye inflammation or skin rashes. A physical exam will test range of motion, spinal tenderness, and neurological function.
Imaging studies
Besides MRI, an X-ray can reveal structural changes such as syndesmophytes (bony growths). A CT scan may be ordered if surgical planning is needed. Most importantly, the MRI tells us whether inflammation is active or chronic.
Laboratory tests
Blood work helps pinpoint the cause. Common markers include:
- ESR (Erythrocyte Sedimentation Rate) a general inflammation gauge
- CRP (C-reactive protein) rises quickly with acute inflammation
- HLA-B27 a genetic marker linked to ankylosing spondylitis
- Complete blood count to rule out infection
Decision-tree flowchart
If you have persistent back pain + morning stiffness, start with labs (ESR/CRP). If these are elevated, proceed to MRI. If MRI shows edema, consider a referral to a rheumatologist; if there's nerve compression, a spine surgeon may be involved.
Treatment Options
First-line, nonsurgical care
Medication basics
NSAIDs like ibuprofen or naproxen are often the first step. They reduce pain and swelling but should be used cautiously if you have stomach ulcers or kidney issues. For short bursts of severe pain, a doctor might prescribe a corticosteroid taper.
Physical therapy & exercise
Think of PT as the maintenance crew for your spine. Core-strengthening, gentle stretching, and posture training can dramatically cut inflammation. A study in the Journal of Orthopaedic & Sports Physical Therapy found that six weeks of supervised PT reduced pain scores by 40% in patients with inflammatory back pain.
Bracing & activity modification
When pain spikes, a soft lumbar brace can offer support without limiting movement. Use it sparingly overreliance can weaken surrounding muscles.
Targeted interventional procedures
Epidural and facet steroid injections
These injections deliver steroids directly to inflamed tissue, providing relief for weeks to months. Success rates hover around 6070% for properly selected patients.
Radiofrequency ablation (RFA)
RFA uses heat to disrupt the nerves transmitting pain signals. It's especially helpful when facet joint inflammation is the main culprit.
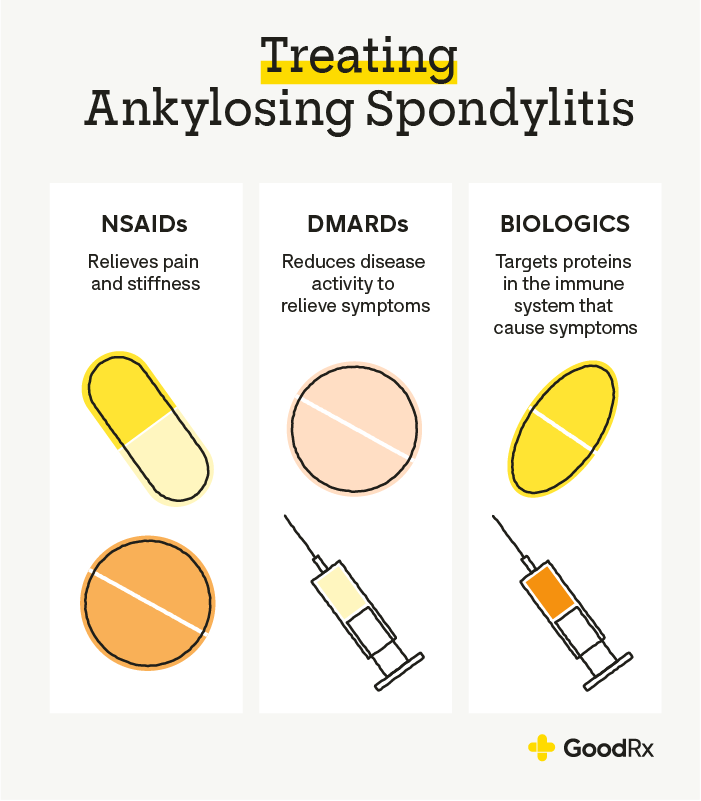
Disease-modifying options for inflammatory arthritis
Biologics & JAK inhibitors
Biologic drugs like TNF blockers (adalimumab, etanercept) or IL-17 inhibitors (secukinumab) target the immune pathways that fuel spinal inflammation. They've transformed lives; many patients report returning to full activities within months. For guidance on when remission is the goal and how it's assessed, see the practical AS remission criteria used by clinicians.
DMARDs (Disease-Modifying Antirheumatic Drugs)
Traditional DMARDs like sulfasalazine may be added for axial spondyloarthritis when biologics aren't suitable.
Surgical interventions (when conservative care fails)
Decompression & fusion
If inflammation leads to nerve compression that doesn't improve with injections, a surgeon may perform a decompression (removing bone or disc material) combined with a spinal fusion to stabilize the segment.
Minimally invasive techniques
Endoscopic decompression and navigation-assisted fixation reduce tissue trauma and speed up recovery compared with open surgery.
Real-world case study: Maria, a 42-year-old graphic designer, started with NSAIDs, progressed to PT, then began a TNF blocker after labs confirmed ankylosing spondylitis. When her pain plateaued, a minimally invasive lumbar decompression restored her mobility, letting her return to work within six weeks.
Balancing Benefits & Risks
Why early treatment matters
Addressing inflammation promptly can:
- Reduce pain and improve sleep
- Preserve spinal range of motion
- Slow or halt structural damage
Potential side-effects
No treatment is without tradeoffs. NSAIDs may cause stomach irritation or raise blood pressure. Biologics increase infection risk, so regular monitoring is essential. Surgery carries typical risks like bleeding, infection, and a recovery period that may require temporary assistance with daily tasks.
Long-term outlook
Data from long-term cohort studies (see ) show that patients who receive appropriate biologic therapy early enjoy a near-normal quality of life and reduced spinal fusion over a decade.
Lifestyle Hacks to Support Healing
Anti-inflammatory diet
Food can be a silent ally. Incorporate omega-3 rich fish, turmeric, ginger, and plenty of leafy greens. These foods help modulate the inflammatory cascade.
Weight management
Even a modest 510% reduction in body weight can lessen the load on the lumbar spine, easing pain and improving the efficacy of other treatments.
Ergonomic home & work setups
Small changes make a big difference:
- Chair: Adjust height so feet rest flat on the floor and knees are at 90.
- Monitor: Top of the screen at eye level to avoid forward head posture.
- Movement: Set a timer to stand and stretch every 45 minutes.
Checklist for a spine-friendly workstation
- Feet flat, hips slightly higher than knees
- Lumbar support or small cushion in the lower back
- Keyboard and mouse within comfortable reach
- Frequent microbreaks stand, roll shoulders, deep breaths
When to Call a Specialist
Know the red-flags that demand urgent attention:
- Sudden weakness in legs or loss of bladder/bowel control
- Night pain that awakens you from sleep
- Unexplained fever, weight loss, or night sweats
- Rapidly worsening mobility despite medication
Dr. Samuel Lee, a spine surgeon in New York, emphasizes any of these signs should prompt an immediate evaluation delays can lead to permanent nerve damage.
Conclusion
Spine inflammation is a treatable condition when identified early, and there's a full spectrum of options from simple over-the-counter pain relievers and targeted physiotherapy to biologic disease-modifying drugs and, if needed, minimally invasive surgery. By understanding the causes, recognizing the symptoms, and partnering with a trusted specialist, you can take control of your back health and return to the activities you love.
Got questions or personal experiences with spinal inflammation? Share them in the comments below, or consider scheduling a consultation with a qualified spine-care provider. Your journey to a pain-free back starts with the first step let's take it together.
FAQs
What are the first steps to treat inflammation of the spine?
Begin with NSAIDs for pain relief, followed by a tailored physical‑therapy program that focuses on core strength, flexibility, and posture correction.
When should I consider biologic medication?
Biologics are recommended if blood tests show high inflammation markers and imaging confirms active disease, especially in conditions like ankylosing spondylitis.
Can minimally invasive surgery cure spinal inflammation?
Surgery addresses structural problems such as nerve compression; it does not eliminate the underlying inflammatory process, but it can relieve severe symptoms when conservative care fails.
Are steroid injections safe for long‑term use?
Epidural or facet steroid injections provide temporary relief and are generally safe when limited to a few courses per year; repeated use may increase the risk of tissue damage.
What lifestyle changes support recovery?
Adopt an anti‑inflammatory diet, maintain a healthy weight, improve ergonomics at work, and stay active with low‑impact exercises like swimming or walking.