Gastroparesis happens when your stomach cant push food along the way its supposed to. The most common culprits are nerve damage, certain surgeries, and a handful of medications but there are plenty of other reasons that can slip under the radar. Below youll find a friendly, nojargon walkthrough of everything that can set this condition off, how doctors figure it out, and what you can actually do about it.
Why Causes Matter
What is gastroparesis?
In plain English, gastroparesis means slow stomach. Your stomach muscles or the nerves that tell those muscles to contract arent working properly, so food lingers, leading to nausea, bloating, and that dreaded fullafterabite feeling.
How a healthy stomach works
The stomachs muscular walls contract rhythmically, propelled by the vagus nerve, to grind food and push it into the small intestine. When the vagus nerve is damaged or the muscle layers weaken, that rhythm breaks down.
Why pinning down the cause is a gamechanger
Identify the trigger, and you can target treatment directly. If diabetes is the root, tighter bloodsugar control can dramatically improve symptoms. If a medication is to blame, swapping it out may almost erase the problem. Knowing the cause also helps you estimate and what lifestyle tweaks will make the biggest difference.
QuickFact Box: Top 5 Most Common Causes
| Cause | Typical % of Cases | Key Clue |
|---|---|---|
| Diabetes (type 1 & 2) | 30% | Longstanding high blood sugar, neuropathy |
| Postsurgical (e.g., gastric bypass) | 20% | Symptoms start weeksmonths after operation |
| Medications | 15% | New pain meds, anticholinergics, GLP1 agonists |
| Postinfectious | 10% | Recent viral/bacterial gastroenteritis |
| Idiopathic (unknown) | 30% | No clear trigger, still treatable |
Common Adult Triggers
Diabetesrelated gastroparesis
High blood glucose over years can scorch the vagus nerve. The American Diabetes Association notes that up to onethird of people with longstanding diabetes develop some degree of gastric emptying delay. If youve been juggling insulin or oral meds for a while and notice food stuck feelings, ask your doctor about a gastric emptying study.
How high sugar sabotages your stomach
Excess glucose creates oxidative stress, which damages the nerve fibers that coordinate stomach contractions. The result? A sluggish, uncoordinated pump.
Practical tip
Keep your A1C in the target range, and discuss regular GI checkups with your endocrinologist. Small improvements in glucose control can translate to big relief in gastroparesis symptoms.
Postsurgical gastroparesis
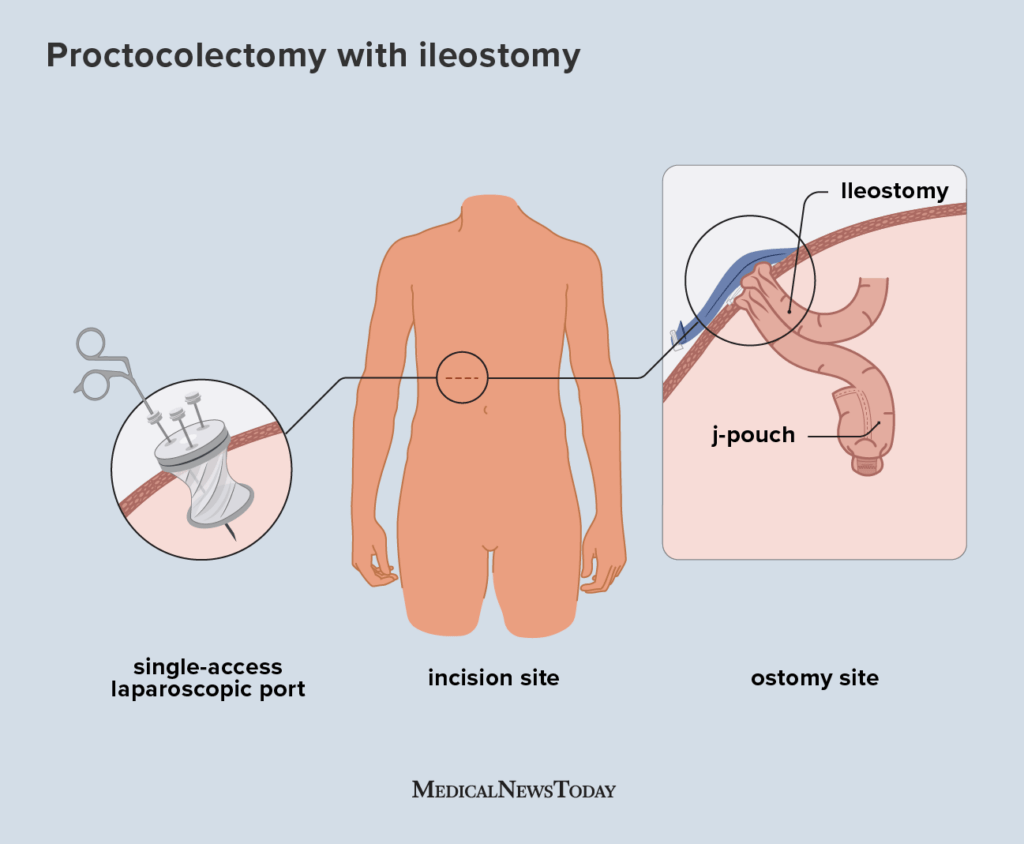
Surgeries that alter stomach anatomythink fundoplication, gastricbypass, sleeve gastrectomycan unintentionally injure the vagus nerve or change the way gastric muscles contract.
Typical timeline
Most people feel the first stomach is stuck episode within 212 weeks after the operation, but it can surface months later as scar tissue forms.
Medicationinduced gastroparesis (list of medications that cause gastroparesis)
Several everyday pills can slow your stomach down. The biggest culprits are:
- Opioids (morphine, oxycodone) they tighten smooth muscle.
- Anticholinergics (e.g., diphenhydramine, certain bladder meds).
- Some antidepressants (tricyclics, certain SSRIs).
- GLP1 receptor agonists for diabetes (exenatide, liraglutide) they purposely slow gastric emptying, which can tip over into gastroparesis.
If you suspect a medication, never stop it cold turkeytalk to your prescriber about alternatives or dose adjustments.
Postinfectious gastroparesis
After a nasty bout of viral gastroenteritis (norovirus, rotavirus) or bacterial food poisoning, the stomachs nerves can stay fried for weeks. Even COVID19 has been linked to delayed gastric emptying in some survivors.
Key clue
Symptoms appear suddenly after a clear infection, and they usually improve gradually over months.
Idiopathic gastroparesis
When doctors cant pinpoint a cause, they label it idiopathic. Roughly onethird of adults fall into this bucket. It sounds mysterious, but the good news: treatment works just as well because the therapy targets the symptom pathway, not the root cause.
Rare Triggers
Neurological disorders
Conditions like Parkinsons disease, multiple sclerosis, and stroke can disrupt the braingut communication line, slowing gastric motility.
Autoimmune diseases
Scleroderma, lupus, and mixed connectivetissue disease can cause fibrosis of the stomach wall, tightening it up and hampering movement.
Metabolic & endocrine issues
Hypothyroidism and hypercalcemia (high calcium) both meddle with smoothmuscle function, sometimes leading to mild gastroparesis.
Systemic infections
HIV, Lyme disease, and even chronic fungal infections can affect the autonomic nerves that control the gut.
Diagnosing the Cause
Symptom checklist
Typical include early satiety, nausea, vomiting of undigested food, bloating, and erratic blood sugar swings (especially in diabetics). Keep a simple diary: note what you ate, how long it took to feel full, and any nausea or vomiting episodes.
Imaging & functional tests
- Gastric emptying scintigraphy the goldstandard; you eat a radiolabeled meal and a scanner tracks how fast it leaves the stomach.
- Upper endoscopy rules out mechanical blockage.
- CT or MRI helpful if you suspect a tumor or severe scar tissue.
Lab work
Blood glucose, thyroid panel, calcium level, and inflammatory markers (CRP, ESR) can reveal underlying metabolic or autoimmune triggers.
Diagnostic flowchart (visual aid for readers)
Consider turning the steps into a simple flowchart:
Symptoms Medication review Blood tests Imaging Gastric emptying study Diagnosis.
Treating the Root
Address the underlying cause first
If diabetes is the driver, tighter glucose control often eases gastroparesis. If a medication is the offender, a switch can bring relief within weeks.
Medication adjustments
Prokinetics (e.g., metoclopramide, erythromycin) can boost stomach contractions, while antiemetics (ondansetron) tackle nausea. Always discuss sideeffectsmetoclopramide, for example, can cause tardive dyskinesia if used longterm.
Dietary strategies (gastroparesis diet)
Think small, frequent, lowfat, lowfiber. Heres a threeday sample plan:
- Day1: Smooth oatmeal with banana, lowfat Greek yogurt; baked cod with mashed potatoes; ricecooked applesauce.
- Day2: Scrambled eggs with a splash of milk, toast (white bread); chicken broth with pureed carrots; vanilla pudding.
- Day3: Lowfat cottage cheese with canned peaches; turkey meatballs in tomato sauce (no chunks); gelatin dessert.
Blend or puree anything that feels too chunky. Hydration is keysip clear broths or electrolyte drinks throughout the day.
For patients who also struggle with constipation related to pelvic floor dysfunction, considering techniques such as pelvic floor relaxation exercises and gentle stool softeners can help; see resources on pelvic floor constipation for practical pelvic strategies that pair well with a gastroparesis diet.
Advanced therapies
If diet and meds arent enough, consider:
- Gastric electrical stimulation (a pacemaker for the stomach).
- Botox injections into the pylorus to relax it.
- In severe cases, a feeding tube (jejunal) or even a gastric resection.
When to escalate
Weight loss >10% of body weight, frequent vomiting, or uncontrolled blood sugars despite optimal management are red flags that warrant a referral to a gastroenterology specialist for gastroparesis treatment options.
Life Expectancy Outlook (gastroparesis life expectancy)
How cause influences prognosis
Diabetesrelated gastroparesis tends to be chronic but manageable; surgically induced cases often improve once the nerve heals or scar tissue stabilizes. Idiopathic and postinfectious forms usually have a more favorable trajectory.
Statistics from leading centers
Recent data from Yale Medicine and the Cleveland Clinic (20232024) show that most patients live normal lifespans, especially when the underlying trigger is controlled. Complicationsmalnutrition, severe dehydration, or refractory diabetescan shorten life expectancy, but proactive management dramatically mitigates those risks.
Living well with gastroparesis
Early diagnosis, diet adaptation, and regular followups can keep you comfortable and active. Think of gastroparesis as a traffic jam in your digestive highway; with the right detours (diet, meds, lifestyle), you can still reach your destination.
RealWorld Stories
How I cured my gastroparesis a personal journey
Emily, a 38yearold teacher, blamed chronic nausea on stress. After a thorough review, her doctor discovered her new prescription for an opioid painkiller was the culprit. Switching to a nonopioid regimen and adopting a lowfat, blended diet erased her symptoms within three months. Her story highlights that cure in gastroparesis often means removing the offending trigger.
Expert interview snippet
Dr. Laura Chen, boardcertified gastroenterologist, says: Patients who think their condition is untreatable are often missing a simple piece of the puzzlemedication review or tighter glucose control. Even idiopathic cases respond well to prokinetics when paired with dietary tweaks.
Patient Q&A
Q: Can I ever stop taking prokinetics?
A: Many do, once symptoms are under control and the underlying cause is addressed. Work with your doctor to taper safely.
QuickReference Tools
Printable checklist: Do I have a causerelated gastroparesis?
| Potential Cause | Key Indicator | Next Step |
|---|---|---|
| Diabetes | Longstanding high A1C, neuropathy | Check gastric emptying, tighten glucose control |
| Recent Surgery | Onset 212 weeks postop | Review operative notes, consider nerve injury |
| Medication | New pain meds, anticholinergics, GLP1 agonist | Discuss alternatives with prescriber |
| Infection | Symptoms follow viral/bacterial gastroenteritis | Observe, supportive care, repeat study if persistent |
| Neurologic/Autoimmune | History of Parkinsons, scleroderma, lupus | Specialist referral for targeted therapy |
FAQstyle quick answers (for featured snippets)
- What are the main gastroparesis causes? Diabetes, postsurgical nerve injury, certain medications, postinfectious nerve damage, and idiopathic factors.
- Can medications cause gastroparesis? Yesopioids, anticholinergics, some antidepressants, and GLP1 agonists are common offenders.
- Is gastroparesis ever curable? While cure is rare, many people achieve symptomfree lives by removing the trigger and following diet/medication plans.
Conclusion
Understanding gastroparesis causes is the first, most empowering step toward relief. Whether the trigger is diabetes, a recent surgery, a medication, or something less obvious, pinpointing it lets you and your doctor craft a focused treatment plan. Remember, youre not alonereal stories, expert guidance, and practical tools are all at hand. If any part of this resonated with you, consider downloading the quickchecklist or chatting with a GI specialist. You deserve a stomach that feels like its doing its job, not sabotaging it.
FAQs
What are the most common causes of gastroparesis?
The most common causes are diabetes, postsurgical nerve injury, certain medications, viral infections, and idiopathic (unknown) factors.
Can medications cause gastroparesis?
Yes, opioids, anticholinergics, some antidepressants, and GLP-1 agonists are known to slow stomach emptying and can trigger gastroparesis.
Is gastroparesis caused by diabetes?
Yes, diabetes is a leading cause, especially when high blood sugar damages the vagus nerve over time.
Can surgery lead to gastroparesis?
Yes, surgeries involving the stomach or vagus nerve can result in gastroparesis due to nerve injury or altered anatomy.
What is idiopathic gastroparesis?
Idiopathic gastroparesis means the cause is unknown, but it accounts for about one-third of cases and is still treatable.