Why Family History Matters
What does the research say?
Large population studies consistently show that having a firstdegree relative with lymphoma modestly raises your own risk. According to the , the relative risk for nonHodgkin lymphoma (NHL) is about 1.82.3 times higher compared with someone without a family history. That sounds scary, but put it in perspective: the baseline lifetime risk for the general population is roughly 12%.
How big is the risk increase?
Think of risk like a ladder. If the average person stands on rung 1, a family history might nudge you up to rung 1.5. In absolute terms, that translates to an extra 12% chance over a lifetime. Its a real increase, yet its far from a guarantee.
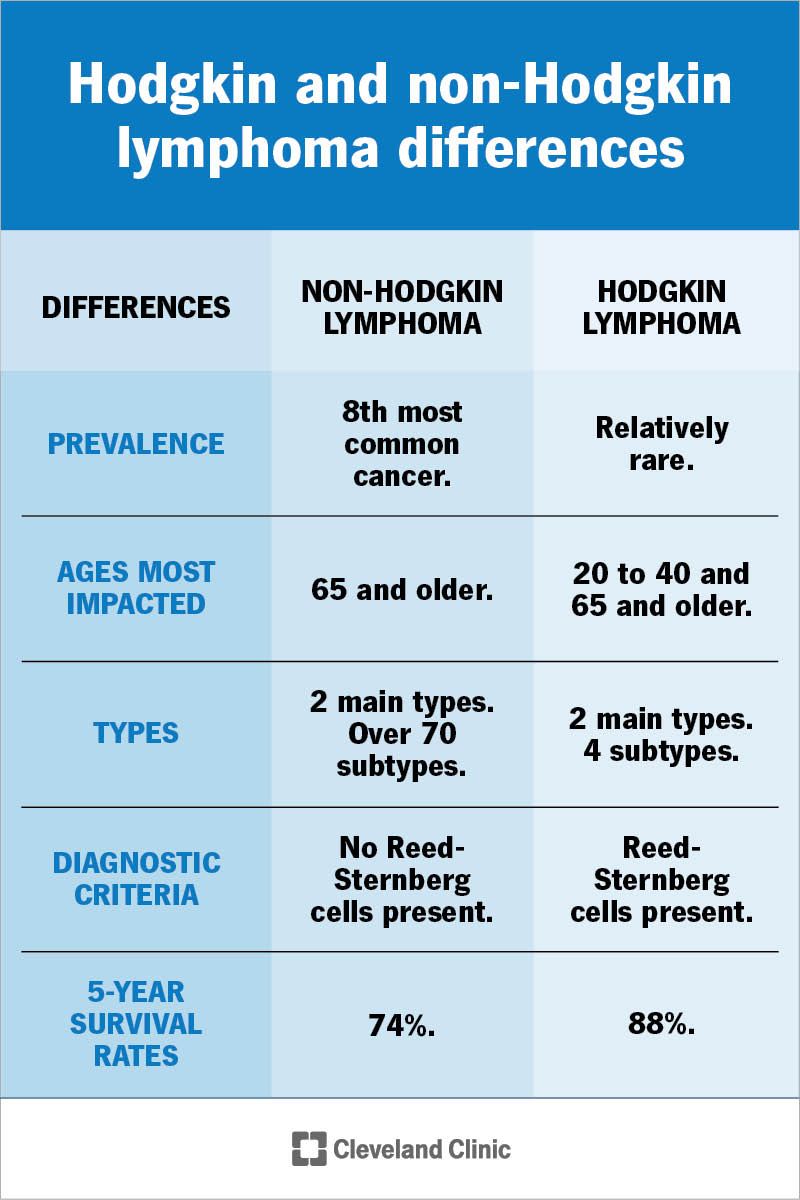
Does the risk differ by lymphoma type?
Yes. Hodgkin lymphoma (HL) shows a slightly lower familial clustering than NHL. For diffuse large Bcell lymphoma (a common NHL subtype), studies report a standardized incidence ratio (SIR) around 2.0, meaning youre twice as likely as the average person if a close relative had that exact type.
Is the risk the same for men and women?
Overall, the increase is similar across genders, but women may notice certain symptoms more readily. For instance, swelling in the neck or axillary (underarm) region can sometimes be mistaken for a breast issue, which is why symptoms of lymphoma in females deserve particular attention.
| Lymphoma Type | Relative Risk (Family History) | Typical Lifetime Risk (General Population) |
|---|---|---|
| Hodgkin Lymphoma | 1.51.8 | 0.2% |
| NonHodgkin Lymphoma (overall) | 1.82.3 | 12% |
| Diffuse Large BCell | 2.0 | 0.6% |
Genetics vs Environment
Is lymphoma genetic or environmental?
Lymphoma is a classic example of a disease where both genes and the environment dance together. Inherited DNArepair defects (like those seen in ataxiatelangiectasia) can predispose you, while viral infections such as EpsteinBarr virus (EBV) or chronic inflammation from autoimmune conditions also play a big part.
Key hereditary syndromes
Rare familial syndromes that raise lymphoma risk include:
- Lynch syndrome primarily linked to colorectal cancer, but also a modest NHL risk.
- Ataxiatelangiectasia a strong association with both HL and NHL.
- Common variable immunodeficiency (CVID) weakened immune surveillance can let malignant cells slip through.
NonHodgkins lymphoma genetic or environmental?
Research published in points to a blend: about 2030% of cases have a clear hereditary component, while the rest are driven by exposures (pesticides, certain chemicals) and infections.
Hodgkins lymphoma familybased risk factors
Twin studies reveal that identical twins share a roughly 3fold higher risk compared with fraternal twins, confirming a substantial genetic component.
Can you get a genetic test for lymphoma risk?
Genetic panels exist, but theyre more about ruling out known highpenetrance syndromes than predicting lymphoma outright. A typical test might include genes like ATM, BRCA2, and TP53. The bottom line? A positive result signals a need for vigilant monitoring, not a definitive diagnosis.
RealWorld Impact Stories
Case study: A family with multiple NHL cases
Johns father and uncle both battled diffuse large Bcell lymphoma in their 50s. When John noticed persistent, painless swelling in his neck, he remembered the family pattern. Early imaging caught the disease at stageII, leading to a successful chemoimmunotherapy regimen and, today, John is in remission.
Patient voice: Living with a known family risk
I grew up hearing about my aunts chemo. When I finally got a genetic counselors appointment, she helped me understand that I wasnt doomedjust that I should stay on top of my health checks, says Maya, a 34yearold teacher. Her story underscores how knowledge transforms anxiety into proactive care.
How early detection helped
Early detection isnt a guarantee of cure, but it dramatically improves outcomes. For many indolent lymphomas, catching the disease before it spreads can mean a simple watchandwait approach instead of aggressive treatment.
Common Questions Answered
How bad is lymphoma cancer?
Lymphoma covers a spectrum. Some types are slowgrowing (indolent) and may never cause severe problems, while otherslike aggressive diffuse large Bcell lymphomarequire prompt, intensive therapy. Prognosis varies widely, but many patients enjoy long survivals, especially when diagnosed early.
Is lymphoma curable?
Yes, a large proportion of Hodgkin lymphoma cases (over 80% 5year survival) are curable with modern chemoradiation. Several nonHodgkin subtypes, especially when caught early, also have high cure rates. The key is accurate staging and tailored treatment.
Is nonHodgkins lymphoma genetic or environmental?
Both. Genetics may set the stage, but exposureslike certain pesticides or chronic virus infectionsoften act as the trigger that pushes cells over the edge.
Is nonHodgkins lymphoma genetic testing available?
Targeted panels exist for hereditary cancer syndromes, but they cant predict NHL with certainty. Theyre most useful if you have a strong family history of multiple cancers or known syndromes.
What causes lymphoma?
Key culprits include:
- Immune system dysregulation (e.g., HIV, organ transplants)
- Viral infections (EBV, HTLV1)
- Chronic inflammation (autoimmune diseases)
- Inherited DNArepair defects
- Environmental exposures (pesticides, solvents)
Symptoms of lymphoma in females
While many signs are genderneutral, women often notice:
- Painless swelling in the neck, armpit, or groin
- Unexplained night sweats
- Persistent fatigue
- Unusual bruising or bleeding
- Breastarea swelling that doesnt resolve
Balancing Benefits & Risks
Benefits of awareness
Knowing your family history lets you and your doctor design a personalized monitoring planthink regular physical exams, blood work, and, when appropriate, imaging. Early vigilance can catch disease at a stage where treatment is most effective.
Potential downsides
Constant worry can turn into anxiety, and some may pursue unnecessary tests. Insurance discrimination, though less common after the Genetic Information Nondiscrimination Act (GINA), still lingers in some minds. Its vital to weigh peace of mind against the emotional toll of overtesting.
How to discuss family history with healthcare providers
Bring a simple chart to your appointment that lists:
- Who was diagnosed (relationship)
- Type of lymphoma (if known)
- Age at diagnosis
- Outcome/treatment received
This familyhealth timeline makes the conversation clear and helps your doctor decide if referral to a hematologist or genetic counselor is warranted.
When to seek a second opinion
If you receive a vague recommendationlike just keep an eye on itand you feel uneasy, asking for a second opinion from a lymphoma specialist (ideally at a comprehensive cancer center) is a smart move.
Action Plan for You
Create a familyhealth timeline
Start a spreadsheet or notebook that captures every relatives cancer history. Even if youre unsure of the exact subtype, note what you do know; patterns often emerge over time.
Schedule a riskassessment appointment
Book time with a hematologist or a genetic counselor. Bring your timeline and be ready to discuss:
- Whether genetic testing makes sense for you
- What screening schedule (e.g., annual physicals, occasional PET scans) is appropriate
Adopt evidencebased lifestyle changes
While you cant change your genes, you can influence other risk factors. Studies show that quitting smoking, maintaining a healthy weight, and limiting exposure to known chemicals can lower overall cancer risk, including lymphoma.
Stay informed
Trusted sourceslike the and the American Cancer Societyregularly update guidelines. Bookmark their pages and revisit them yearly.
Join support communities
Online forums (such as ) and local patient groups provide emotional backing and practical tips. Sharing your story can be empowering for both you and others walking the same path.
Printable checklist FamilyHistory Lymphoma Action Sheet
Download a simple PDF (create it yourself using this outline) that includes:
- Relatives name, relationship, and diagnosis details
- Dates of diagnosis and treatment outcomes
- Questions to ask your doctor
- Lifestyle goals (exercise, diet, exposure limits)
Conclusion
Having a family history of lymphoma does raise your risk, but its far from a destiny. By understanding the genetic and environmental pieces, staying alert to early symptoms, and taking concrete stepslike building a familyhealth timeline and consulting a specialistyou can turn knowledge into power. Remember, youre not alone; countless families have walked this road and emerged stronger. If you have questions, personal stories, or just need a listening ear, drop a comment below. Lets keep the conversation going and support each other on the journey to health.
FAQs
Does a family history of lymphoma mean I will get lymphoma?
No, a family history of lymphoma increases your risk compared to the general population, but most people with a family history will never develop lymphoma. The increase in risk is modest, and many other factors also play a role[1][3][6].
How much does a family history of lymphoma raise my risk?
Having a first-degree relative with lymphoma raises your risk by about 1.7 to 2.3 times for non-Hodgkin lymphoma and around 1.5 to 1.8 times for Hodgkin lymphoma, depending on the specific subtype and your relationship to the affected relative[1][2][3].
Is the risk the same for all types of lymphoma?
No, the risk varies by subtype. For example, diffuse large B-cell lymphoma risk is higher if a close relative had that specific type, while Hodgkin lymphoma shows less familial clustering than non-Hodgkin lymphoma[3][4].
Can genetic testing tell me if I will get lymphoma?
Genetic testing can identify some high-risk syndromes, but it cannot predict with certainty whether you will develop lymphoma. Testing is most useful if you have a strong family history of lymphoma or related cancers[2].
What should I do if I have a family history of lymphoma?
Document your family health history, discuss it with your doctor, and consider consulting a hematologist or genetic counselor. There is no routine screening for lymphoma, but early detection of symptoms can improve outcomes[6].