If youve bounced back from COVID19 but suddenly feel your heart race, your chest tighten, or youre wiped out after just a few steps, you might be wondering whether its just stress or something more serious. The truth is, those feelings can be warning signs of covid heart damage symptoms, and catching them early can make a world of difference.
In the next 1520 minutes well walk through exactly how the virus can mess with your ticker, what to look out for, when to call a doctor, and practical ways to give your heart a solid postCOVID reboot. No jargon, no fluffjust the information you need, delivered like a friendly chat over a cup of coffee.
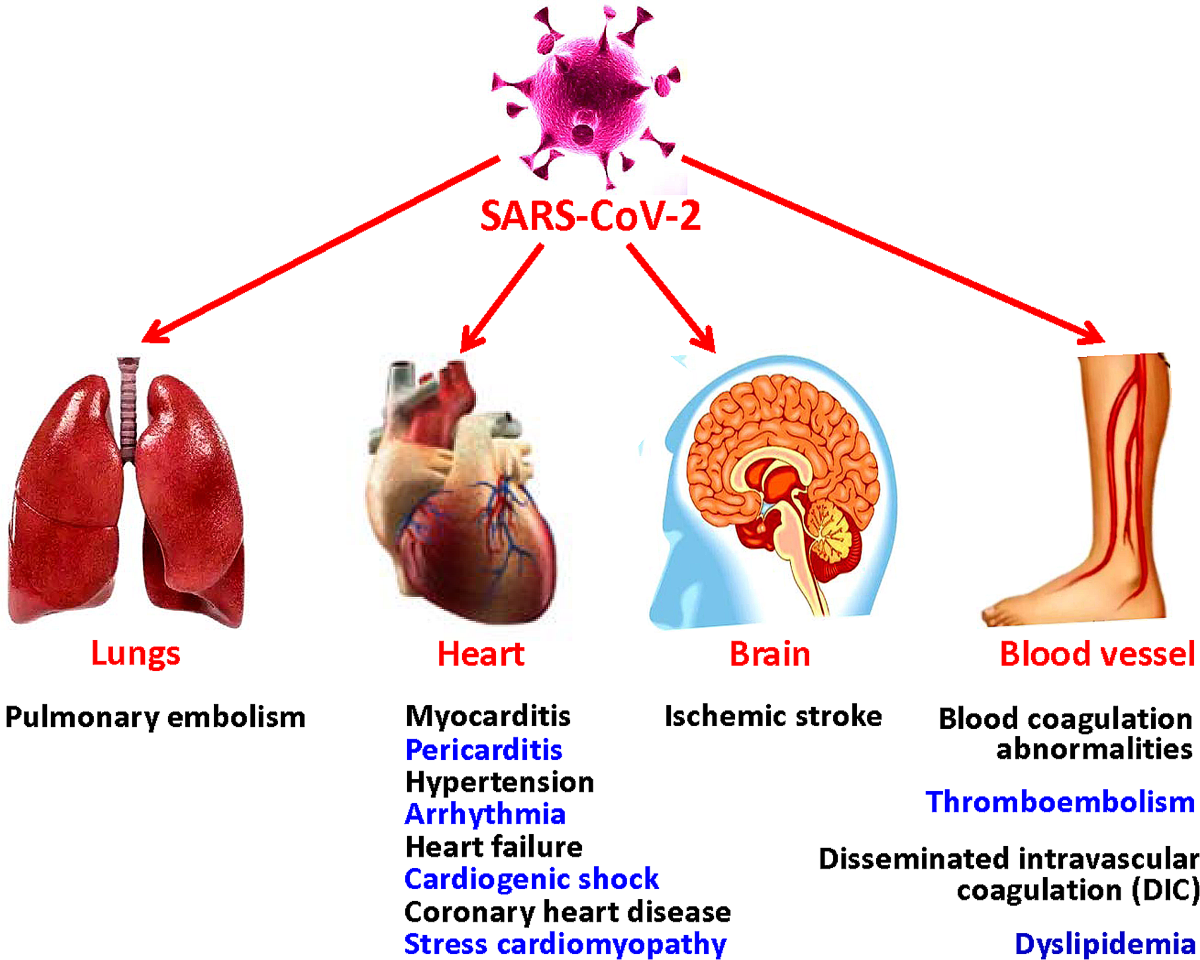
How COVID Affects Heart
What mechanisms cause heart injury in COVID19?
Inflammation (myocarditis) the virus can inflame the heart muscle itself. how this inflammation can lead to chest pain, arrhythmias, and reduced pumping ability.
Microvascular clotting tiny clots can block blood flow in heart vessels, a problem highlighted by the in its COVIDheart research.
Stressinduced cardiomyopathy sometimes called brokenheart syndrome, where the emotional and physical stress of the illness weakens the heart muscle temporarily.
How common are heart problems after COVID?
Data from the suggest that up to 20% of COVID survivors report at least one cardiovascular symptom, with palpitations being the most frequent.
Age makes a difference: older adults and those with preexisting heart disease see higher rates, while children tend to experience milder forms, according to a .
Whos at highest risk?
People with prior heart conditions, severe acute infection (hospitalization, oxygen support), and older age (>60) are the most vulnerable. Genetic factors that affect blood clotting and inflammation may also play a role.
Recognizing Symptoms
What are the most frequent covid heart damage symptoms?
PostCOVID heart palpitations a fluttering, racing, or skippedbeat feeling that often shows up weeks after the infection.
Chest pain or pressure, especially when breathing deeply or climbing stairs.
Shortness of breath on minimal exertion (you want to sit down after walking to the mailbox).
Persistent fatigue, dizziness, or fainting spells that feel out of proportion to your activity level.
Newonset arrhythmias such as atrial fibrillation, which can cause an irregular heartbeat that you can literally feel. If arrhythmias or ongoing weakness lead to poor circulation or swelling, consider checking resources on leg swelling cause for possible related issues.
How to differentiate normal postviral tiredness from heart trouble?
Timeline matters: if symptoms linger beyond four weeks, consider a cardiac cause.
Redflag signs include chest pain radiating to your arm or jaw, sudden shortness of breath, and episodes of fainting.
If your resting heart rate is consistently above 100bpm or below 50bpm without exercise, it could be a sign that covid has affected your heart rate.
Can COVID affect your heart rate even if you feel fine?
Yes. Many patients report autonomic dysregulationyour nervous systems automatic pilot gets confused, leading to unexplained tachycardia (fast heart) or bradycardia (slow heart) at rest.
When to Seek Help
Redflag symptoms that need emergency care
Sudden, crushing chest pain or pressure.
Severe shortness of breath that doesnt improve with rest.
Loss of consciousness or nearfainting episodes.
If you notice a rapid, irregular heartbeat accompanied by dizziness, call emergency services right away.
What tests will doctors order?
Electrocardiogram (ECG/EKG) the first look at your hearts electrical activity.
Blood tests for cardiac enzymes (troponin) to check for heart muscle injury.
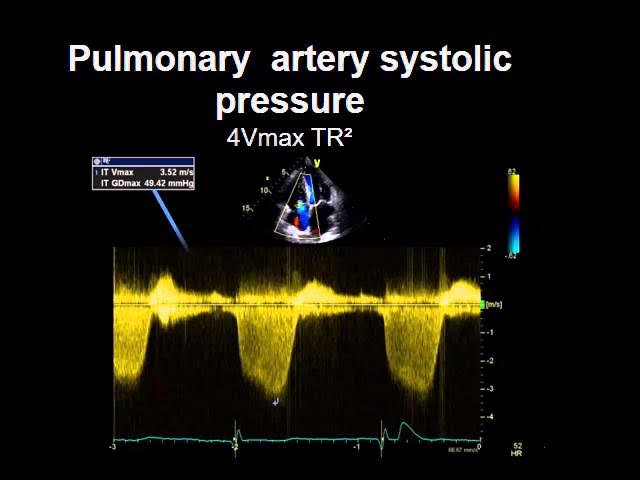
Echocardiogram an ultrasound that shows how well your heart pumps.
Cardiac MRI the goldstandard for spotting myocarditis and scarring.
Holter monitor or wearable patch for 2448hours to capture intermittent arrhythmias.
How to prepare for your appointment
Write down a timeline of symptoms (when they started, what makes them better or worse).
List any previous heart conditions, medications, and recent COVID19 test results.
Bring a trusted friend or family member if you feel anxiousyoull have an extra set of ears for the doctors instructions.
Improve Heart Health After COVID
Lifestyle changes that support recovery
Gentle aerobic activity: start with 1015 minutes of walking, cycling, or swimming, gradually building to 150minutes per week as tolerated.
Hearthealthy diet: aim for plenty of omega3 rich foods (salmon, walnuts), colorful vegetables, whole grains, and keep sodium under 1,500mg per day.
Managing stress & sleep
Mindbody tools like deepbreathing, guided meditation, or even a short yoga routine can lower heartrate variability and calm the autonomic nervous system.
Prioritize 79 hours of quality sleep; a consistent bedtime routine makes a huge difference for cardiac recovery.
Medical therapies & supplements
Betablockers or ACE inhibitors may be prescribed if your doctor detects lingering hypertension or arrhythmias.
Evidencebased supplements such as magnesium (helps with muscle relaxation) and CoQ10 (supports cellular energy) have shown modest benefit in postviral heart health, as noted in a recent .
What helps vs. what can worsen (quick reference table)
| Helps | Can Worsen |
|---|---|
| Light aerobic exercise | Intense workouts without clearance |
| Omega3 rich foods | Excess caffeine or energy drinks |
| Stressreduction techniques | Smoking or heavy alcohol use |
| Adequate sleep | Latenight screen time |
Treat Palpitations
Shortterm symptom control
Vagal maneuvers (e.g., holding your breath, coughing) can sometimes stop a sudden episode of rapid heartbeats.
Correcting electrolyte imbalancesespecially potassium and magnesiumhelps calm an overexcited heart.
Temporary antiarrhythmic medication may be prescribed while your doctor determines the underlying cause.
Longterm management
Cardiac rehabilitation programs provide supervised exercise, education, and monitoring to safely rebuild heart strength.
Autonomicnervoussystem retraining, such as graded exposure to upright positions, can reduce postural tachycardia that some longCOVID patients experience.
Emerging therapies (20242025)
Lowdose colchicine, an antiinflammatory drug, is being investigated for persistent myocarditis after COVID19 (see a recent ).
Wearable cardiac monitors (e.g., Apple Watch, dedicated patches) let patients share realtime rhythm data with their physicians, enabling quicker adjustments to treatment plans.
Prevent Future Damage
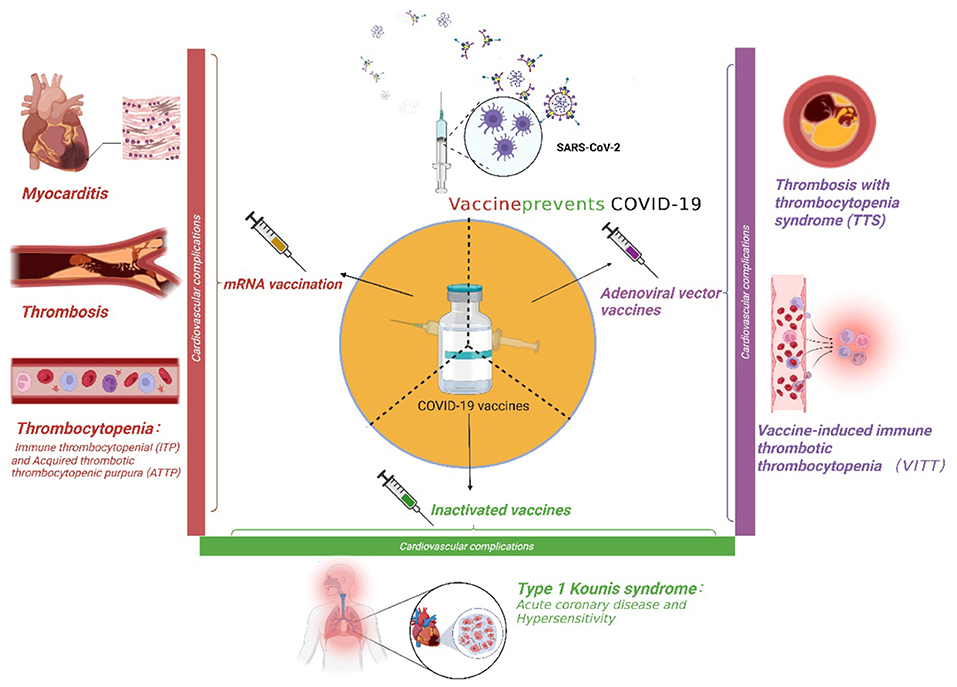
Vaccination & booster impact
Staying uptodate with COVID19 boosters reduces the severity of reinfection, which in turn lowers the risk of additional heart injury.
Routine followup schedule
For highrisk patients, doctors often recommend checkins at 1month, 3months, and 6months postinfection, with repeat ECG or echo as needed.
Who should avoid intense exercise?
If youve been diagnosed with myocarditis, most guidelines advise a 3 to 6month rest period before returning to highintensity sportsalways get clearance from a cardiology specialist.
Conclusion
Covid heart damage symptoms can range from a harmless flutter to serious chest pain, but the good news is that early detection, proper testing, and a blend of lifestyle tweaks plus medical care can keep your heart humming along. If any of the warning signs weve discussed sound familiar, dont waitschedule a checkup, start gentle movement, and keep an eye on your stress levels. Your heart has been through a lot; give it the care it deserves.
Have you experienced any postCOVID heart changes? Share your story in the comments or reach out to your healthcare provider. Together we can navigate this new territory and keep our hearts strong.
FAQs
What are the most common covid heart damage symptoms?
The typical signs include palpitations or a racing heartbeat, chest pain or pressure, shortness of breath with minimal activity, persistent fatigue, dizziness, and new‑onset arrhythmias such as atrial fibrillation.
How long after a COVID infection can heart symptoms appear?
Symptoms can show up during the acute phase, but many patients notice them weeks to months later, often after the initial illness seems resolved. If they persist beyond four weeks, a cardiac cause should be considered.
When should I see a doctor for post‑COVID chest pain?
Seek immediate medical attention if chest pain is crushing, radiates to the arm or jaw, is accompanied by shortness of breath, fainting, or an irregular, rapid heartbeat. Even milder pain that worsens with activity warrants a prompt evaluation.
Can regular exercise worsen covid‑related heart injury?
Gentle aerobic activity (e.g., walking, light cycling) is encouraged, but high‑intensity workouts or sports should be avoided until a healthcare provider clears you, especially if myocarditis has been diagnosed.
Are there any tests that can confirm myocarditis after COVID?
Diagnosis typically involves an electrocardiogram (ECG), blood tests for cardiac enzymes (troponin), an echocardiogram, and, when needed, a cardiac MRI—considered the gold standard for visualizing heart muscle inflammation.