Hey there, friend. If youve ever felt that stubborn ache behind your kneecap or noticed your leg wobbling a bit more than usual, youre not alone. Knee osteoarthritis isnt just a sore jointit can open the door to a whole suite of hidden challenges that affect everything from the way you walk to the mood you carry each day. Knowing these complications early gives you a fighting chance to keep moving, stay active, and maybe even sidestep the worst of them.
What Are the Complications?
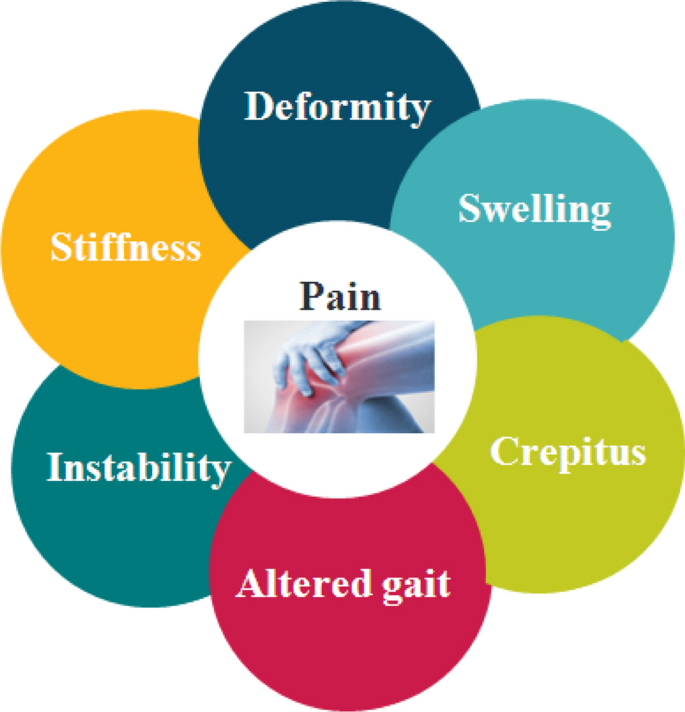
Pain & Stiffness That Keeps Growing
At first, the pain might feel like a light throb after a long hike. Over months, though, that throb can morph into a sharp, constant ache that spikes at night. The stiffness you notice first thing in the morning can also linger longer as the cartilage wears down. According to , this progression is typical when the protective cartilage thins and the bone underneath starts to rub together.
Joint Instability & Deformity
When the smooth surface disappears, the knee can feel wobbly, especially when you try to step onto a curb or stand up from a chair. Over time, the joint may develop a visible bowlegged or knockkneed shape. This isnt just an aesthetic issueinstability raises the risk of falls and further joint damage.
Reduced Range of Motion & Everyday Limits
Ever tried to squat and felt like you hit an invisible wall halfway down? Thats a reduction in range of motion, and it directly impacts everyday tasks: climbing stairs, getting in and out of a car, or even tying your shoes.
Secondary Health Issues
Living with chronic knee pain can sneakily lead to weight gain, because activity drops and comfort foods become a quick fix. Sleep can suffer toopain flares at night make it hard to slip into deep rest, and a lack of sleep fuels irritability and even anxiety. A study in notes that more than 60% of osteoarthritis patients report insomnia at some point.
BoneSpecific Complications
In severe cases, the loss of cartilage can expose the bone to reduced blood flow, leading to osteonecrosis (bone death). While rare, its a serious complication that often signals the need for surgical intervention.
| Stage | Typical Complications | Typical Symptoms |
|---|---|---|
| Stage1 Early | Mild pain, occasional stiffness | Knee feels okay most of the day |
| Stage2 Moderate | Joint instability, limited ROM | Pain after activity, slight swelling |
| Stage3 Severe | Deformity, osteonecrosis risk | Constant pain, night waking |
| Stage4 Endstage | Need for joint replacement | Total functional loss |
Stages and Risks
Understanding the four stages of knee osteoarthritis helps you spot red flags before they become emergencies. If you notice any of these warning signspain that scores 7or higher on a 10point scale, swelling that refuses to go down, or a noticeable change in knee alignmentits time to talk to a professional.
When Complications Signal Stage34
- Persistent, highintensity pain that disrupts sleep
- Reduced ability to fully straighten or bend the knee
- Visible deformity (bowlegged, knockknee)
- Frequent giving way episodes
These clues tell your body that the joint is under serious stress, and early intervention can still make a big difference.
Who Is at Risk?
Age, Gender & Genetics
People over 50 are the obvious crowd, but womenespecially after menopausetend to develop osteoarthritis faster. Hormonal changes affect cartilage health, a fact highlighted by research at the .
Weight & Metabolic Health
Every extra pound forces your knee to work harder. The Mayo Clinic estimates that losing just 10% of body weight can cut knee pain by up to 40%.
Activity Level & Past Injuries
Highimpact sports, previous meniscus tears, or ACL injuries often set the stage for early cartilage breakdown. Even a seemingly harmless sprain can start a chain reaction if the joint never fully heals.
Managing the Complications
Medical Treatments & New Options
Theres a growing toolbox of beyond the classic NSAIDs. Viscosupplementation injections, plateletrich plasma (PRP), and even stemcell therapies are being studied in 2024 trials, showing promise in slowing cartilage loss and reducing pain.
NonSurgical vs. Surgical Options
| Option | Typical Cost | Recovery Time | Complication Rate |
|---|---|---|---|
| Physical Therapy + Exercise | Low | Immediate | Minimal |
| Viscosupplementation Injection | Medium | Weeks | Low |
| PRP/StemCell Injection | High | WeeksMonths | LowModerate |
| Total Knee Replacement | High | 36months | 510% (infection, stiffness) |
Targeted Exercise Programs
Moving may feel counterintuitive when your knee hurts, but gentle strengthening can actually protect the joint. Focus on quadriceps and hamstring work, plus balance drills that improve proprioception. A typical fourweek routine might look like this:
- Week1: Straightleg raises (3sets15 reps) and seated knee extensions.
- Week2: Add wall sits (30seconds3) and standing hamstring curls.
- Week3: Introduce lowimpact cycling or pool walking for 20minutes.
- Week4: Balance exercisessingleleg stands on a soft surface, 10seconds each side.
These are proven to boost joint stability and reduce the giving way feeling.
Weight Management & Nutrition
Antiinflammatory foodsthink salmon, walnuts, turmeric, and leafy greenscan lower systemic inflammation that fuels cartilage breakdown. Pair that with a modest calorie deficit, and youll give your knee a lighter load to bear.
PainManagement Strategies
Topical NSAIDs (like diclofenac gel) work well for localized pain without the stomach upset of oral meds. For people who cant tolerate NSAIDs, lowdose duloxetinea serotoninnorepinephrine reuptake inhibitorhas shown benefit in chronic OA pain, according to a .
Psychological Support
Living with chronic pain can weigh heavily on the mind. Simple cognitivebehavioral techniqueslike keeping a pain diary, practicing deep breathing, or setting small, achievable activity goalscan help keep anxiety and depression at bay.
Real Stories & Tips
Story #1: Lifestyle Overhaul
Maria, 58, was told her knees were aging after a minor fall. She decided to act: she shed 20pounds, started the fourweek exercise plan, and swapped her morning bagel for a bowl of oatmeal topped with berries. Six months later, her pain dropped from a 7/10 to a 2/10, and shes back to gardening without the jojoeffect of pain.
Story #2: CuttingEdge Procedure
John, a former marathon runner, tried PRP after conventional treatments failed. He received three injections over six weeks, combined with supervised physio. By month4, his swelling was gone and his marathon time improved by 12 minutes. He still uses his strengthening routine to keep the benefits rolling.
Takeaway Checklist
- Schedule a doctors visit at the first sign of persistent knee pain.
- Ask about newer injection therapies if youre past the first line of treatment.
- Commit to a lowimpact exercise planconsistency beats intensity.
- Monitor weight and nutrition; even modest changes help.
- Consider a mentalhealth checkin if pain affects mood.
Quick Reference Tools
To keep everything in one place, download these free PDFs:
- Complications Checklist (PDF) a concise list of warning signs to watch for.
- StagebyStage Symptom Tracker printout you can fill in weekly.
- Exercise Log Sheet 4week planner to stay on track.
Conclusion
Understanding the complications of osteoarthritis of the knee isnt about scaring yourselfits about empowering you to act before the pain takes over. By recognizing early warning signs, staying active, managing weight, and exploring both conventional and newer treatments, you can keep your kneesand your lifemoving forward. Grab the free checklist, talk openly with your healthcare provider, and start a gentle strengthening routine today. Whats the biggest hurdle youve faced with knee pain? Share your story in the comments, and lets support each other on the road to healthier knees.
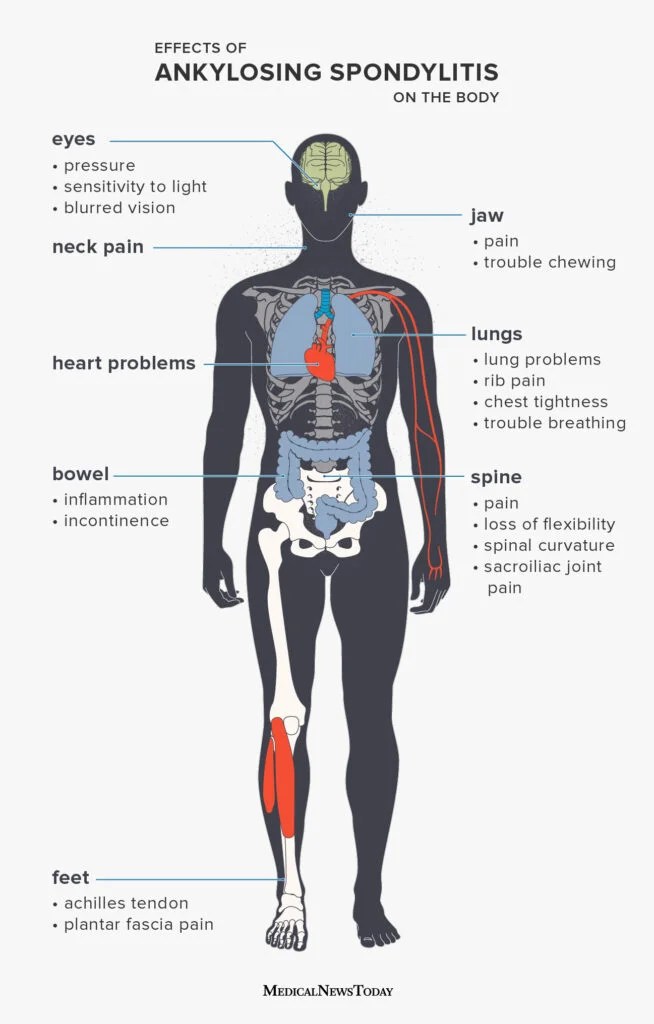
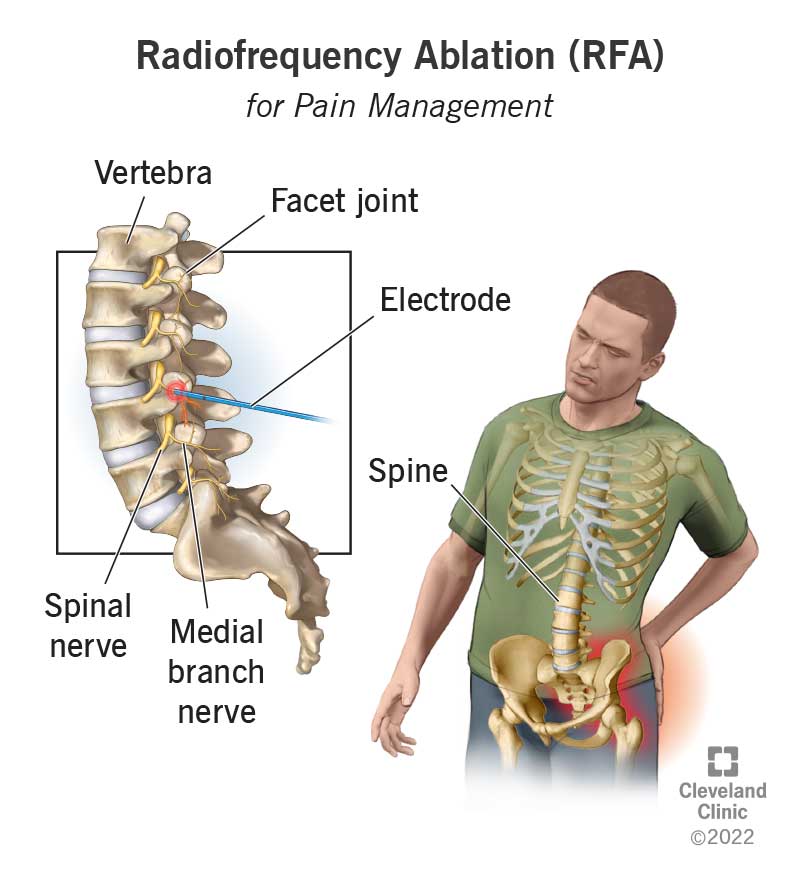
For readers who also manage other musculoskeletal conditions, resources on related spine problems may be helpful learn more about spine inflammation as it can sometimes coexist with knee issues and influence treatment decisions.
FAQs
What are the most common complications of osteoarthritis of the knee?
The most frequent issues are increasing pain, stiffness, joint instability, reduced range of motion, and bone‑related problems such as bone bruising or osteonecrosis.
How can joint instability be managed without surgery?
Strengthening the quadriceps and hamstrings, balance training, using a knee brace, and physical‑therapy‑guided exercises can significantly improve stability.
When should I consider advanced injection therapies like PRP or stem‑cell treatment?
If conservative measures (exercise, NSAIDs, weight loss) no longer control pain after 3‑6 months and imaging shows moderate cartilage loss, discuss PRP or stem‑cell options with an orthopedic specialist.
Does losing weight really lessen knee‑osteoarthritis symptoms?
Yes. Research shows that a 10 % reduction in body weight can reduce knee‑pain scores by up to 40 % because it decreases the mechanical load on the joint.
Can osteoarthritis of the knee lead to depression or anxiety?
Chronic pain often affects mood. Studies indicate that over 60 % of OA patients experience sleep problems, which can trigger anxiety or depression. Seeking psychological support or CBT can help.