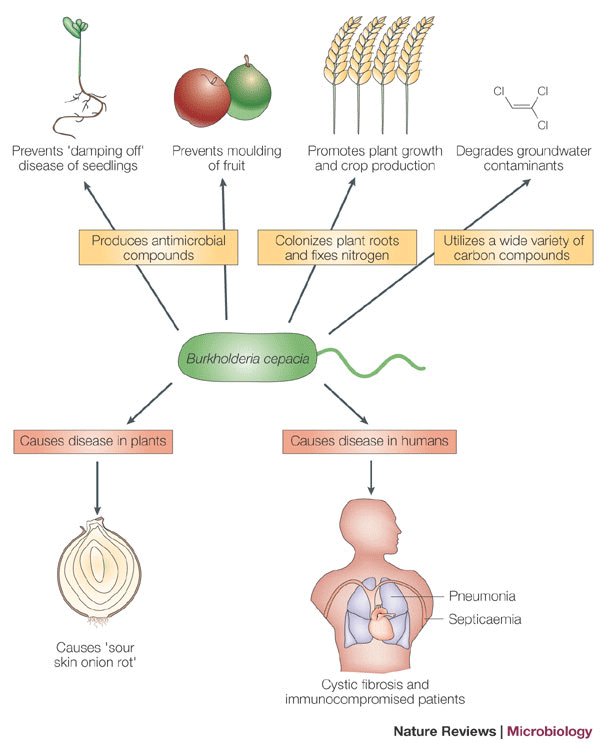
Lets cut to the chase: Bcepacia is a tough, drugresistant bug that can turn life with cystic fibrosis (CF) into a rollercoaster of lung infections, hospital stays, and big decisions about transplants. If you or someone you love is dealing with this, you deserve clear, honest answersfast. Below youll find the facts, practical tips, and a dash of encouragement to help you stay a step ahead.
Quick Answer Snapshot
Short answer: Bcepacia is a group of bacteria that can cause severe, drugresistant lung infections in people with cystic fibrosis. It can worsen lung function, trigger Cepacia syndrome, and limit transplant options, but early detection and tailored therapy can improve outcomes.
Why It Matters
You might wonder why this particular germ gets so much attention. The short answer? Its not just another coughcausing bug. Heres what makes Bcepacia a gamechanger for many CF families:
- Prevalence & risk: About 510% of people with CF in the US and UK carry Bcepacia at some point in their lives.
- Impact on lung health: Infections can accelerate lungfunction loss, sometimes leading to the dreaded Cepacia syndrome a rapid, necrotizing pneumonia.
- Effect on transplant eligibility: Some transplant centres will turn you away if the strain is the aggressive Burkholderia cenocepacia type.
- Emotional and social rippleeffects: Because the bacterium is highly contagious in clinical settings, patients may face isolation policies, added anxiety, and extra paperwork.
All of this sounds heavy, but knowing the risks gives you power to actso lets dig deeper.
Symptoms & Signs
Typical Bcepacia symptoms
When Bcepacia shows up, it often masquerades as a regular CF flare, but there are clues that set it apart:
- Persistent, thick sputum that turns green or white.
- Sudden increase in shortness of breath.
- Fevers above 38C that linger for more than a couple of days.
- Unexplained weight loss or a slowdown in growth (especially in kids).
How it differs from a regular CF flare
If you notice a fast drop in lung functionsay, a 10% or more fall in FEV1 over two weeksplus any of the signs above, you might be dealing with Bcepacia. The hallmark Cepacia syndrome adds:
- Sharp chest pain.
- Rapidly rising sputum volume.
- Signs of sepsis: low blood pressure, high heart rate.
Cepacia syndrome quickchecklist (downloadable PDF)
| Symptom | Redflag threshold |
|---|---|
| Fever | >38.5C |
| Chest pain | Any new, sharp pain |
| Sputum volume | Doubling from baseline |
| Blood pressure | Systolic <90mmHg |
When we first heard about Cepacia syndrome from a teen named Maya, she described it like watching your lungs go from a slow sunrise to a sudden storm in minutes. Her story reminds us that early warning signs are worth more than a thousand doctor visits.
Diagnosing Bcepacia
Quick, accurate diagnosis is the cornerstone of any treatment plan. Heres what labs usually do:
| Method | How it works | Turnaround time | Sensitivity / Specificity |
|---|---|---|---|
| Sputum culture | Grow bacteria on selective media | 4872h | 90% |
| PCRbased rapid test | Detect bacterial DNA directly | 46h | 95% |
| Wholegenome sequencing | Identify species & resistance genes | 12weeks | 99% |
Most CF centres start with a sputum culture, then add a PCR if the result is negative but suspicion stays high. According to the , combining methods improves detection, especially for lowgrade infections.
Treatment Options
Firstline antibiotic regimens
Because Bcepacia is notoriously resistant, doctors often begin with a doublecoverage approach:
- Ceftazidime + TrimethoprimSulfamethoxazole: This combo hits the bacterium from two angles.
- Tobramycin inhalation: Adds a high concentration of drug directly to the lungs.
When antibiotics arent enough
If the infection persists, specialists may turn to more aggressive or experimental therapies:
- IV meropenem + ceftazidime: A doublecarbapenem strategy often reserved for severe cases.
- Phage therapy: Using viruses that specifically kill Bcepacia. A recent study in Frontiers in Microbiology showed promising results for a handful of patients ().
- Liposomal inhaled antibiotics (e.g., amikacin): Provide a sustained release, reducing the need for daily nebulizers.
Every treatment plan should be personalized, and having a CFtrained pulmonologist on your team makes a world of difference.
Lung transplant considerations
For many, a transplant is the ultimate lifeline. However, Bcepacia throws a curveball:
- Eligibility criteria: Some centres reject patients with the aggressive B. cenocepacia strain, while others accept milder strains after a rigorous clearance protocol.
- Posttransplant infection risk: Studies show a >30% increase in mortality when Bcepacia is present at the time of surgery.
Decisiontree for transplant candidacy (visual)
| Step | What to ask | Possible outcome |
|---|---|---|
| Positive Bcepacia test? | Yes Identify species | Proceed with caution or seek alternative centre |
| Species = B. cenocepacia? | Yes Discuss with transplant team | May be denied; consider clinical trial |
| Other species? | Yes Review center policy | Often accepted with intensive prophylaxis |
When I chatted with Dr. Alvarez, a transplant surgeon at a major US centre, he told me we never say no without exploring every possible avenuesometimes a swift eradication protocol can flip the script. That optimism can be a lifeline in itself.
Life Expectancy & Outlook
Numbers can feel cold, but theyre useful for planning and hopesetting. Heres a snapshot from recent registry data:
| Metric | Bcepaciapositive CF patients | General CF population |
|---|---|---|
| Median survival (2023) | 35years (5) | 45years (4) |
| 5year lungfunction decline | ~10% FEV1 loss per year | ~5% per year |
| Posttransplant 5yr survival | 50% 60% | 70% 80% |
These figures come from a and the 2024 Cystic Fibrosis Foundation registry report. While the outlook may seem grim, many patients live well beyond these averages thanks to aggressive early treatment, vigilant monitoring, and supportive care networks.
Practical Tips for Everyday Life
Daily infectioncontrol habits
Small changes can make a huge difference:
- Hand hygiene: Wash for at least 20seconds after gardening, handling soil, or touching pet food bowls. Bcepacia loves moist environments.
- Personal nebulizer kits: Never share equipment. If a friend needs to borrow, sterilize the mouthpiece with hot water and a disinfectant wipe.
- Household cleaning: Use a bleachbased solution on bathroom tiles and kitchen counters weekly; the bacterium is resistant to many standard cleaners.
Travel and social life
Planning a vacation? Keep these in mind:
- Check the infectioncontrol policies of hospitals you might visitsome will quarantine Bcepaciapositive patients for up to two weeks.
- Stay uptodate on vaccinations (flu, COVID19, RSV) to reduce the risk of secondary infections that could open doors for Bcepacia.
- If youre attending a large gathering, bring your own portable air purifierclean air can reduce inhaled bacterial load.
Nutrition and lunghealth support
Good nutrition fuels both your immune system and your lungs:
- Highcalorie, highprotein diet: Aim for 1.52g protein per kilogram of body weight daily.
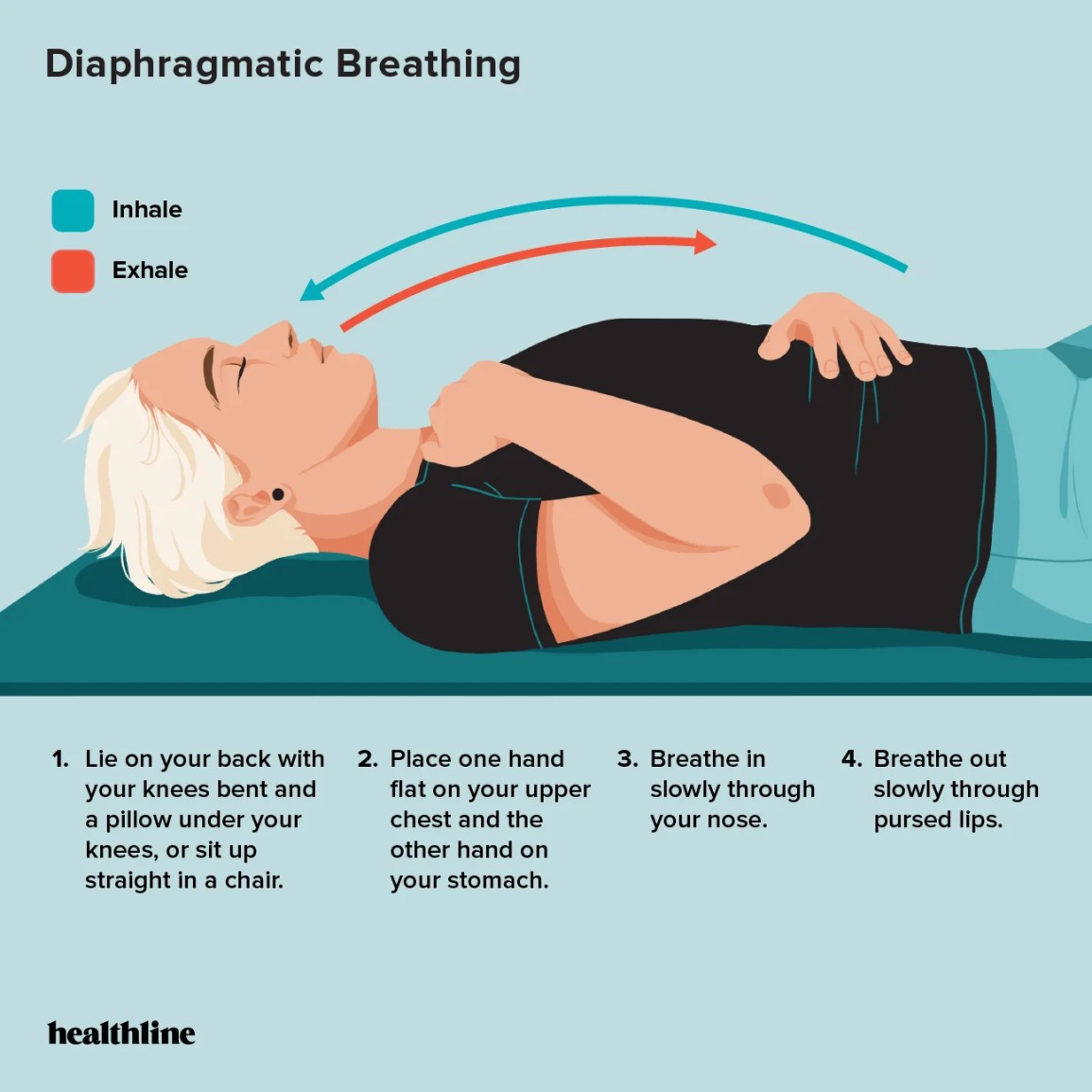
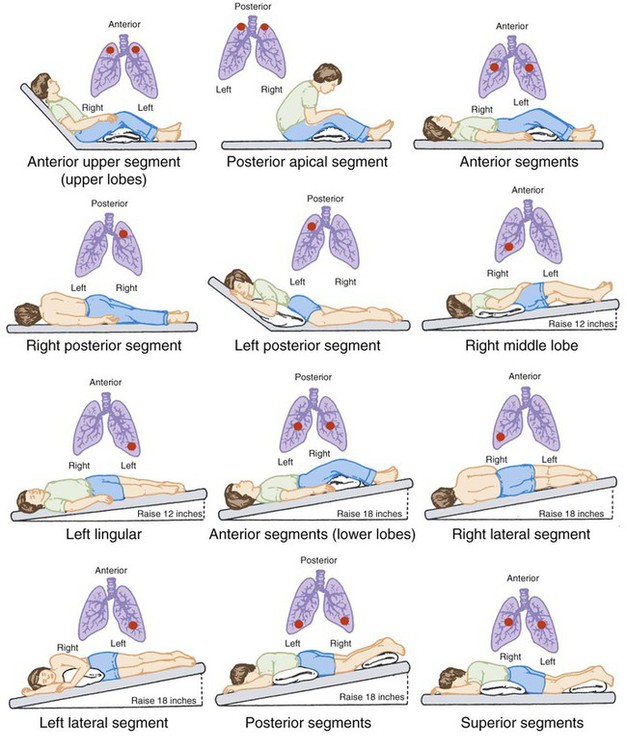
- Airway clearance: Use a vest or chest physiotherapy twice a day. Consistency keeps mucus thin and less hospitable for bacteria. For guidance on chest physiotherapy techniques and effective airway clearance methods, see this practical guide on chest physiotherapy cystic fibrosis.
- Hydration: Warm fluids (herbal teas, broth) help loosen sputum.
Quickreference cheatsheet (downloadable)
Feel free to print this handy onepager and stick it on your fridge. It lists daily habits, redflag symptoms, and emergency contact numbers.
Resources & Where to Get Help
Knowing where to turn can make the journey less lonely:
- Cystic Fibrosis Foundation (CFF): Offers a patient portal, support groups, and uptodate research summaries.
- CF Trust (UK): Provides infectioncontrol guidelines and a Stopping Bcepacia awareness campaign ().
- NIH Clinical Trials: Look for ongoing phagetherapy studies that might match your profile.
- Your local CF centre: Request a regular Bcepacia screening schedule and ask about individualized eradication protocols.
If youre ready to take the next step, click the button below to find a CF centre near you.
Conclusion
Bcepacia is a serious, drugresistant foe that can speed up lung decline, complicate transplant plans, and add emotional weight to daily life. Yet, early detection, aggressive multidrug therapy, meticulous infection control, and a supportive care team can tip the balance toward stabilityand even improvement. Remember, youre not alone: countless families, dedicated clinicians, and a growing body of research are all working to turn this challenge into a manageable part of the CF journey.
Whats your experience with Bcepacia? Have you discovered a tip that helped you breathe easier? Share your story in the comments, and lets keep the conversation going. If you have any questions, dont hesitate to asktogether were stronger.
FAQs
What is B cepacia in cystic fibrosis?
B cepacia is a group of bacteria that can cause severe, drug-resistant lung infections in people with cystic fibrosis, sometimes leading to rapid decline in lung function.
Why is B cepacia dangerous for CF patients?
B cepacia can accelerate lung damage, trigger cepacia syndrome, and complicate transplant eligibility, especially with aggressive strains like B. cenocepacia.
What are the symptoms of B cepacia infection?
Symptoms include persistent thick sputum, sudden shortness of breath, fever, weight loss, and in severe cases, sharp chest pain and signs of sepsis.
How is B cepacia diagnosed in CF?
Diagnosis is usually done with sputum culture, PCR tests, or whole-genome sequencing to identify the specific strain and resistance profile.
Can B cepacia be treated in cystic fibrosis?
Treatment often involves aggressive antibiotic combinations, inhaled therapies, and sometimes experimental options like phage therapy, tailored to the patient’s strain and health status.