At first I thought it was nothing just a weird hiccup of the lungs, maybe a fleeting panic attack. But when the feeling kept popping up, especially during quiet moments on the couch, I realized something else was going on. If youve ever caught yourself stopping breathing for a second while awake, youre not alone, and its worth understanding what that pause really means.
Daytime breathing pauses, often called apneic breathing while awake, can be more than a quirky symptom. They may hint at underlying heart or brain signals that deserve attention. Below, Ill walk you through what to look for, why it happens, how dangerous it can be, and practical steps you can take right now. Think of it as a friendly chat over coffee no jargon, just the facts you need.
Recognizing Awake Apnea Symptoms
What does stop breathing for a second while awake feel like?
Imagine youre reading a book and, out of nowhere, your breath hiccups and you feel a brief airhungry gasp. Its usually only a second or two, but it can feel like youve just hit a mental pause button. Common sensations include lightheadedness, a sudden whoosh as air rushes back in, or a fleeting tingling in the fingertips. Some people even describe it as a miniblackout, though true loss of consciousness is rare.
Awake apnea symptoms vs. normal hiccups or sighs
Its easy to chalk a pause up to a hiccup or a deep sigh, but there are telltale differences. Hiccups are rhythmic, often accompanied by a hic sound, and usually last longer than a single breath. A sigh is a voluntary, relaxed exhale. Awake apnea, however, is involuntary, abrupt, and may be accompanied by a brief feeling of panic or chest tightness.
| Feature | Awake Apnea | Hiccup | Sigh |
|---|---|---|---|
| Duration | 12seconds | 0.53seconds, repeated | 12seconds, single |
| Sound | Usually none | Distinct hic | Often none |
| Trigger | Stress, heart/brain signals | Stomach distension, temperature change | Relaxation |
| Accompanying feeling | Lightheaded, gasp | None | Calm |
When should I be concerned?
Most of us will experience an occasional pause and never need medical help. However, keep an eye out for the following red flags:
- More than three pauses in a day.
- Each pause lasting longer than 10seconds.
- Associated chest pain, severe dizziness, or confusion.
- Episodes that happen while youre driving, working, or otherwise needing full attention.
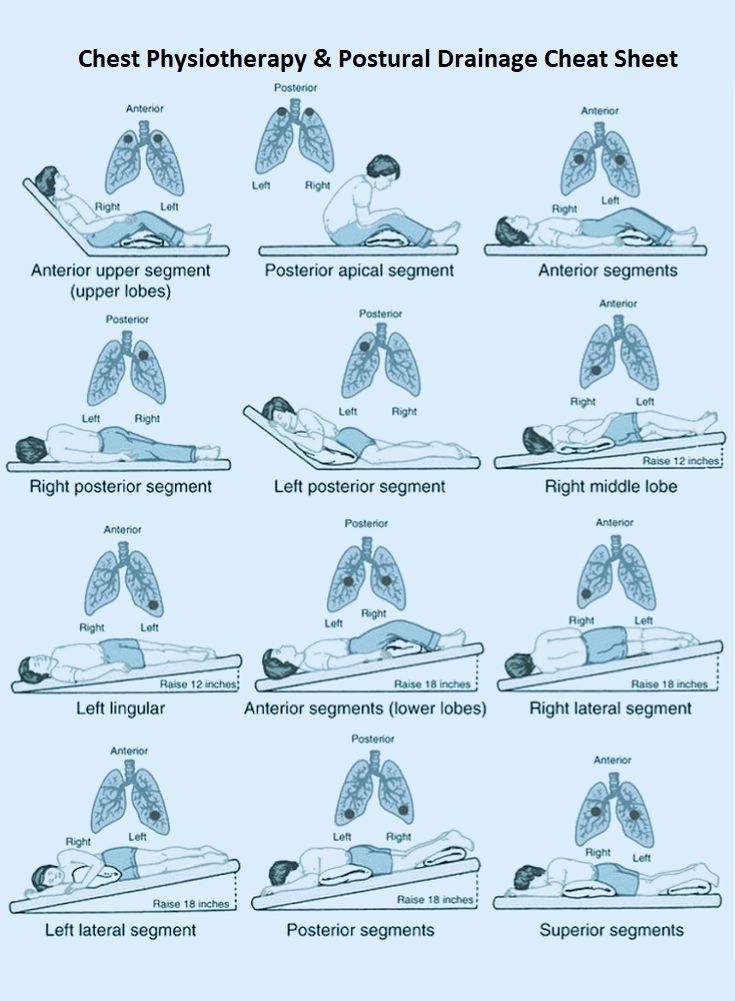
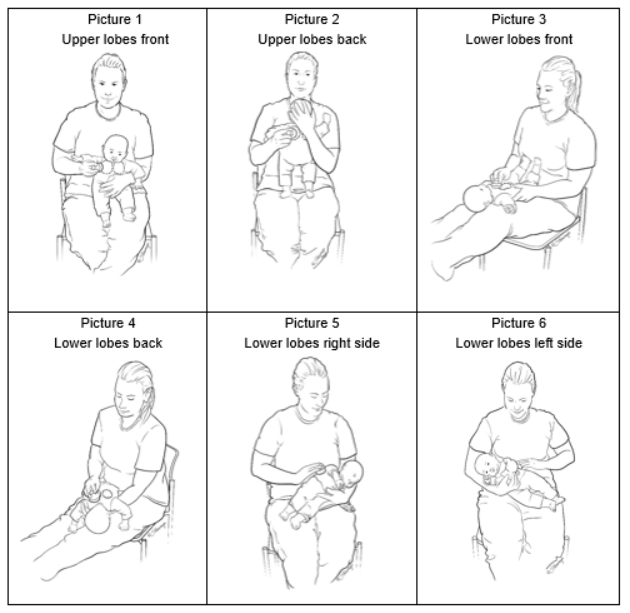
If any of these apply, its time to book a visit with a sleepmedicine or cardiology specialist. Early detection can prevent bigger problems down the road. For people managing chronic lung conditions, coordinating breathing evaluations with their routine airway clearance methods can be especially helpful; ask your clinician how daytime pauses might relate to your respiratory care plans and airway clearance methods by visiting airway clearance methods.
Why It Happens Underlying Causes
Is it central sleep apnea thats showing up while Im up?
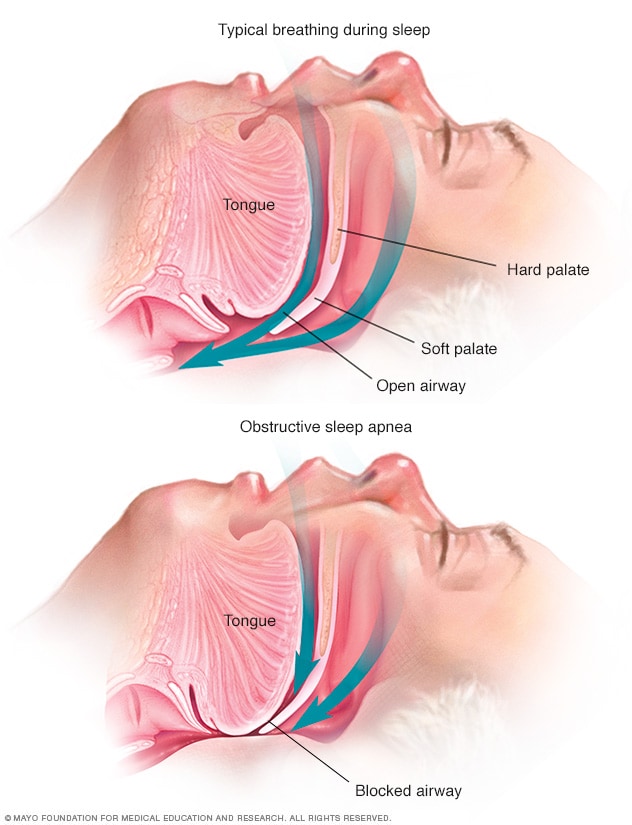
Yes, many daytime pauses are actually a form of central sleep apnea (CSA) spilling over into your waking hours. Unlike obstructive sleep apnea, where the airway is physically blocked, CSA occurs when the brains respiratory centers temporarily forget to send a breathing signal. The result? A brief, silent stop in airflow even when youre sitting up.
Neurological causes of central sleep apnea
Several brainrelated factors can trigger CSA:
- Brainstem injuries trauma, stroke, or tumors can disrupt the rhythmsetting centers.
- Neurodegenerative diseases conditions like Parkinsons or ALS can impair neural pathways.
- Medications opioids, benzodiazepines, and certain anesthetics depress the respiratory drive.
According to the , about 510% of all sleepdisordered breathing cases are central in origin, and the neurological component is often the key driver.
CheyneStokes respiration and its daytime version
CheyneStokes respiration is a characteristic pattern of gradually increasing and then decreasing breathing depth, followed by a pause. Its common in people with heart failure, and it can appear during wakefulness, especially when youre lying down or resting. If you notice a waxingandwaning breathing rhythm that ends with a brief silence, you might be experiencing a daytime CheyneStokes episode.
Other medical contributors
Besides the brain, other systems can provoke apneic breathing while awake:
- Cardiac arrhythmias irregular heartbeats can disrupt the timing of breaths.
- Chronic lung disease severe COPD can cause brief breathholding as the lungs struggle to exchange gas.
- High altitude lower oxygen levels trigger irregular breathing patterns.
- Anxiety or panic attacks hyperventilation can be followed by an involuntary pause.
Is It Dangerous? Risks & Outcomes
Can sleep apnea kill you when it happens while awake?
The short answer: yes, if the underlying cause is severe. A sudden pause can lead to a temporary dip in blood oxygen, which, if repeated often, may stress the heart and increase the risk of arrhythmias. In rare cases, an extended pause (over 20seconds) can cause fainting or, in extreme scenarios, cardiac arrest. Thats why persistent daytime apnea deserves a medical glance.
Is central sleep apnea dangerous compared with obstructive sleep apnea?
Both forms carry health risks, but they differ in outcomes:
| Aspect | Central Sleep Apnea | Obstructive Sleep Apnea |
|---|---|---|
| Mortality risk | Higher in heartfailure patients | Elevated, especially with severe OSA |
| Treatment response | Often requires adaptiveservoventilation | Usually CPAP works well |
| Typical cause | Neurological/cardiac signals | Physical airway blockage |
Both can be serious, but central apnea tends to be more directly linked with cardiac issues.
Longterm impact on quality of life
Frequent pauses can cause daytime fatigue, poor concentration, and even mood changes. Imagine trying to focus on a work project while your brain keeps sending breathreset signals its exhausting. Over time, the cumulative sleep fragmentation can impair memory, increase accident risk (especially behind the wheel), and strain relationships because youre constantly battling invisible symptoms.
Diagnosis & When to Seek Professional Help
How doctors confirm apneic breathing while awake
Diagnosis typically starts with a thorough history and a physical exam. The goldstandard test is an overnight polysomnography, which records brain waves, oxygen levels, heart rhythm, and breathing patterns. For daytime evaluation, doctors may use:
- Capnography measures CO during wakefulness.
- Pulseoximetry tracks oxygen saturation while you sit upright.
- Imaging (MRI/CT) to rule out neurological lesions.
What questions will your doctor ask?
Be ready to answer a checklist like:
- How many pauses per day? When do they occur?
- Any associated chest pain, dizziness, or fainting?
- Do you have a history of heart disease, stroke, or lung problems?
- What medications are you taking (especially opioids or sedatives)?
- How is your sleep quality at night?
Selfscreening tools (quick online quiz)
If you want a quick gauge before the appointment, answer these three questions:
- Do you experience a sudden airhungry gasp while sitting or standing?
- Does it happen more than three times a day?
- Do you feel lightheaded, chest tightness, or faint after the episode?
If you answered yes to at least two, consider booking that doctors visit. Its better to be proactive than to wait for a scary incident.
Treatment Options From Medical to SelfHelp
Apnea while awake treatment medical interventions
Medical treatment depends on the root cause:
- Adaptiveservoventilation (ASV) a sophisticated machine that adjusts pressure in real time, ideal for central sleep apnea.
- Continuous Positive Airway Pressure (CPAP) still useful if you have mixed obstructivecentral patterns.
- Acetazolamide a carbonicanhydrase inhibitor that stimulates breathing in select CSA cases.
- Cardiac resynchronization therapy for heartfailure patients with CheyneStokes breathing.
Lifestyle tweaks that reduce daytime pauses
Simple habits can make a big difference:
- Maintain a regular sleep schedule consistency stabilizes the brains breathing rhythm.
- Avoid alcohol and heavy meals close to bedtime both can blunt respiratory drive.
- Practice gentle breathing exercises (478 technique) during the day to train steadier patterns.
- Stay upright while reading or watching TV; lying flat can promote pauses.
When surgical options are considered
Surgery is rare for central apnea but may be indicated for specific neurological lesions (e.g., removal of a brainstem tumor) or for severe heartfailurerelated breathing disorders where device implantation (like a pacemaker) can improve cardiac output and reduce CheyneStokes episodes.
Alternative & complementary approaches
While evidence varies, some people find relief with:
- Yoga breathing (pranayama) promotes rhythmic, diaphragmatic breathing.
- Biofeedback devices teach you to recognize and correct irregular patterns.
- Cognitivebehavioral therapy (CBT) for anxietyrelated hyperventilation, which can indirectly curb pauses.
Always discuss alternative methods with your clinician to avoid conflicts with prescribed therapies.
Managing DaytoDay Practical Strategies
What to do the moment you feel a pause?
When that airhungry gasp hits, try this threestep rescue:
- Sit up straight opening the chest helps air flow.
- Take a slow, controlled inhale through the nose for 4seconds.
- Exhale gently through the mouth for 68seconds. Repeat twice if needed.
The goal is to reset your breathing rhythm without triggering panic.
Tools & gadgets that help
Modern wearables can be allies:
- Portable pulseoximeters give realtime O saturation.
- Smartwatch alerts some models detect bradypnea (slow breathing) and vibrate.
- Nasal dilators keep the airway open, especially if you have a mixed pattern.
When to call emergency services
These situations call for immediate help:
- Loss of consciousness or unresponsiveness.
- Chest pain that feels tight or radiates to the arm/jaw.
- Bluetinged lips or fingertips (cyanosis).
- Repeated pauses that last longer than 20seconds.
If any of these happen, dial emergency services right away better safe than sorry.
Frequently Asked Questions (FeaturedSnippet Friendly)
What is it called when you stop breathing while awake?
Its commonly referred to as apneic breathing while awake or simply awake apnea. In medical literature, it can be a manifestation of central sleep apnea spilling into wakefulness.
Is awake apnea the same as central sleep apnea?
Not exactly, but theyre closely linked. Central sleep apnea is a nighttime disorder where the brain fails to send breathing signals. When those same signal gaps happen during the day, we call it awake apnea.
Can stress trigger apneic breathing while awake?
Yes. Acute stress can cause hyperventilation followed by a brief rebound pause. Chronic anxiety may also sensitize the respiratory centers, making pauses more likely.
How long does a typical pause last?
Most pauses are short under 10seconds. Anything consistently longer should be evaluated by a professional.
Does treating nighttime apnea fix daytime pauses?
Often it does. Effective CPAP or ASV therapy can stabilize the breathing control system, reducing both nighttime and daytime episodes. However, if a specific neurological cause exists, additional treatment may be needed.
Conclusion
Apneic breathing while awake isnt just a quirky hiccup; it can be a sign that your heart, brain, or lungs are sending a subtle SOS. By learning the symptoms, recognizing the possible causesfrom central sleep apnea to stressinduced breath holdsand taking appropriate stepswhether thats a medical evaluation, lifestyle tweak, or a quick breathing resetyou empower yourself to breathe easier and live safer. If any of the redflag signs mentioned above sound familiar, book that appointment. You deserve clear, steady breaths, day and night.
FAQs
What exactly is apneic breathing while awake?
It’s a brief, involuntary pause in breathing that occurs during wakefulness, often linked to central sleep apnea or other cardio‑neurological signals.
How can I tell if my daytime breathing pause is serious?
Seek medical attention if pauses happen more than three times a day, last longer than 10 seconds, or are accompanied by dizziness, chest pain, or fainting.
Can stress or anxiety cause these breathing pauses?
Yes. Acute stress can trigger hyperventilation followed by a rebound pause, and chronic anxiety may increase the frequency of daytime apnea episodes.
What tests do doctors use to diagnose awake apnea?
Doctors typically start with a clinical interview and may order overnight polysomnography, daytime capnography, pulse‑oximetry, and brain imaging if a neurological cause is suspected.
Are there at‑home techniques that help stop a pause when it occurs?
Try sitting upright, inhaling slowly through the nose for 4 seconds, then exhaling gently through the mouth for 6‑8 seconds. Repeating this twice can reset your breathing rhythm.