Did you know a thorough arthritis physical exam can be wrapped up in about 15 minutes and often uncovers the first clues that differentiate rheumatoid from osteoarthritis? In the next few minutes I'll walk you through exactly what a rheumatologist looks for, why each step matters, and how you can get the most out of your appointmentno jargon, just the facts you need right now.
Whether you're newly diagnosed, suspecting joint pain, or simply curious about what will happen behind the exam room door, this guide is your friendly companion. Let's dive in, chat about the exam's purpose, and equip you with tools that turn a routine checkup into a collaborative, confidence-building experience.
Why the Exam Matters
What does a musculoskeletal exam cover?
- Inspection: looking for swelling, redness, or deformities.
- Palpation: feeling for tenderness, warmth, and joint line irregularities.
- Range-of-motion (ROM): testing how far each joint can move actively and passively.
- Strength assessment: checking the power of surrounding muscles.
- Gait & functional tests: observing how you walk, climb stairs, or lift objects.
How long does the exam usually take?
Most rheumatology clinics schedule a focused arthritis physical exam for 1020 minutes. The exact timing depends on how many joints are involved and whether the doctor needs to perform additional special tests. In practice, a well-organized session often wraps up in about 15 minutes, leaving a few minutes for discussion.
Benefits and risks of the exam
- Early detection: Spotting subtle swelling or decreased ROM can prompt treatment before irreversible damage occurs.
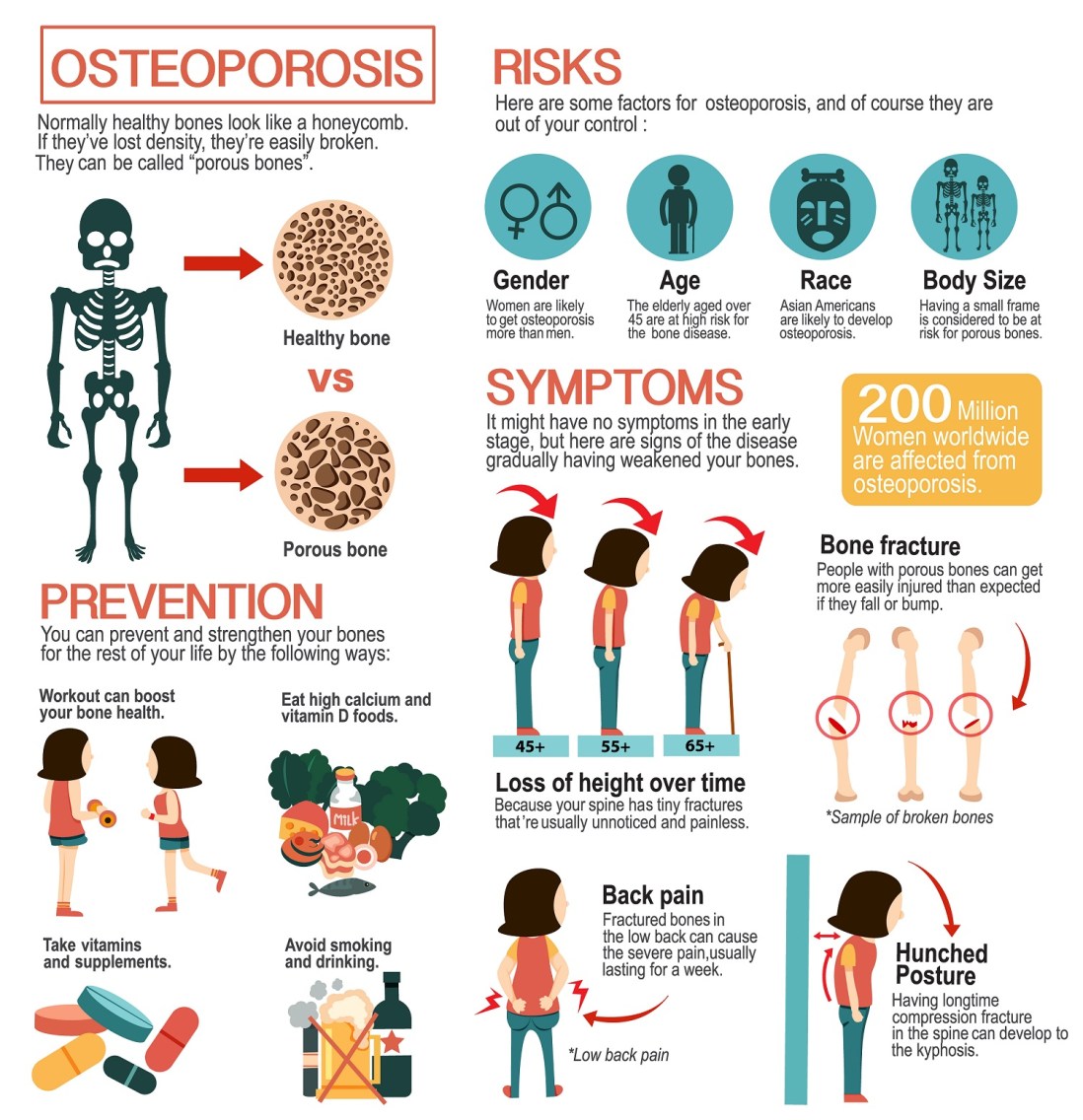
- Tailored treatment planning: Physical findings guide medication choices, physical therapy, and lifestyle recommendations. If osteoporosis is a concern, your provider may recommend specific osteoporosis exercises to protect bone density.
- Monitoring disease activity: Repeating the exam over time shows whether the disease is flaring or settling.
- Potential discomfort: Some palpation or ROM maneuvers may cause mild soreness, especially if joints are already inflamed.
- Limitations: An exam alone can miss deep joint pathology; imaging or labs may still be needed.
Exam Step-by-Step Guide
How should I prepare before the exam?
- Write down any medications you're taking, including over-the-counter supplements.
- Wear comfortable clothing that allows easy access to your arms, legs, and torso.
- Bring a brief symptom diary: note which joints hurt, when the pain started, and what makes it better or worse.
- If you have recent X-rays or lab results, bring copies along.
What does the doctor inspect first?
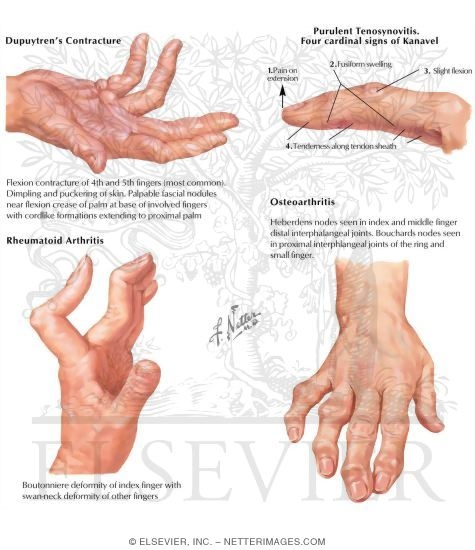
The clinician usually starts with a visual sweep of the whole musculoskeletal system. They'll note any obvious swelling of the hands, wrists, knees, or feet, and look for skin changes, nodules, or postural shifts that hint at chronic joint stress.
How is palpation performed?
Using gentle pressure, the doctor feels each joint line for warmth, tenderness, and any irregular bony prominences. For rheumatoid arthritis, a classic squeeze test of the metacarpophalangeal (MCP) joints often reveals pain that the patient may not notice otherwise. A handy reference is the guide, which demonstrates the exact hand placement.
How is range-of-motion tested?
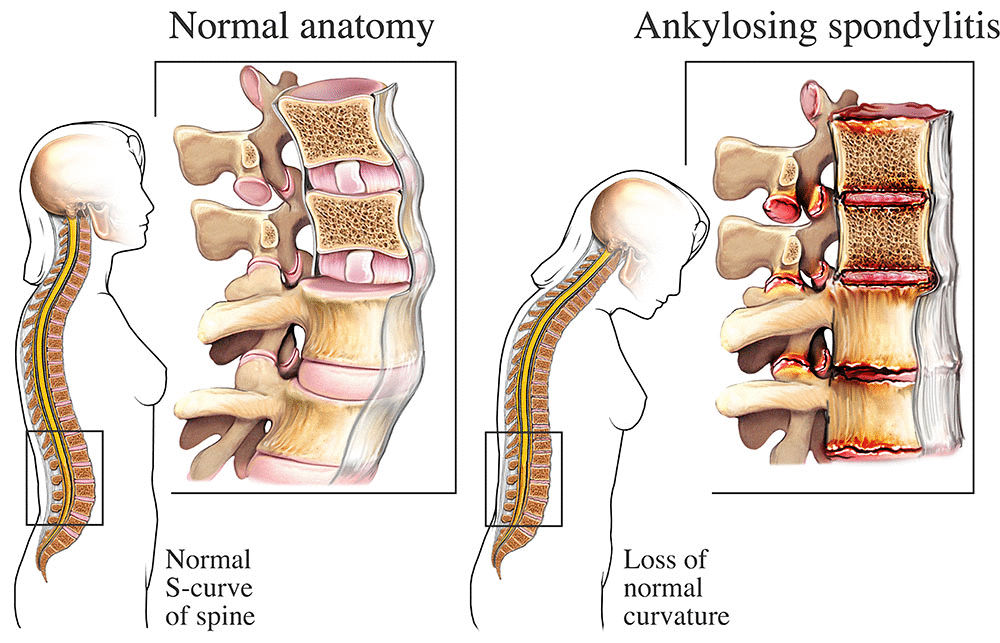
Active ROM asks you to move the joint yourself (e.g., bending the elbow). Passive ROM has the examiner move the joint while you stay relaxed, allowing detection of stiffness that you might compensate for. Normal degrees of motion are compared against age-adjusted ranges; reduced flexion in the knee or limited extension in the fingers often points toward osteoarthritis. Sometimes, interpretation of these findings may overlap with ankylosing spondylitis criteria, depending on the pattern and distribution of joint involvement.
How is strength evaluated?
The examiner grades muscle power on a 05 scale, where 5 means full strength and 0 indicates no contraction. They'll ask you to push against their hand or lift a light weight, focusing on muscles that stabilize the examined joints (e.g., quadriceps for the knee, forearm extensors for the wrist).
Which special tests indicate RA or OA?
- Rheumatoid squeeze test: pain on squeezing the MCP joints suggests inflammatory arthritis.
- Crepitus test: a gritty grinding sensation during joint movement is typical of osteoarthritis.
- Heberden's/Bouchard's nodes: bony enlargements at the distal and proximal interphalangeal joints are classic OA signs.
- Morning stiffness check: stiffness lasting longer than 30 minutes is more common in RA.
RA vs OA Differences
What are typical findings in rheumatoid arthritis?
RA usually presents with symmetric swelling of the small jointsespecially the MCP and proximal interphalangeal (PIP) joints. You may notice:- Warm, tender joints that look puffy.
- Morning stiffness that lasts >30 minutes.
- Ulnar deviation of the fingers and possible rheumatoid nodules.
These clues align with the classic peer-reviewed study on standardized joint examination, which emphasizes the importance of symmetry and tenderness in early RA detection.
What are typical findings in osteoarthritis?
OA tends to affect larger, weight-bearing joints and is often asymmetric. Key signs include:- Joint space narrowing visible on X-ray (though you won't see this in the exam).
- Crepitus felt during flexion/extension.
- Limited range of motion but relatively little warmth or tenderness.
- Knobbly bony outgrowthsHeberden's (distal) and Bouchard's (proximal) nodes.
Unlike RA, morning stiffness in OA usually resolves within 1015 minutes.
When should I worry about red-flag signs?
Red flags suggest an urgent or non-arthritic cause, such as infection or crystal arthritis. Look out for:
| Red-Flag Symptom | Possible Cause |
|---|---|
| Severe, rapidly worsening pain | Septic arthritis |
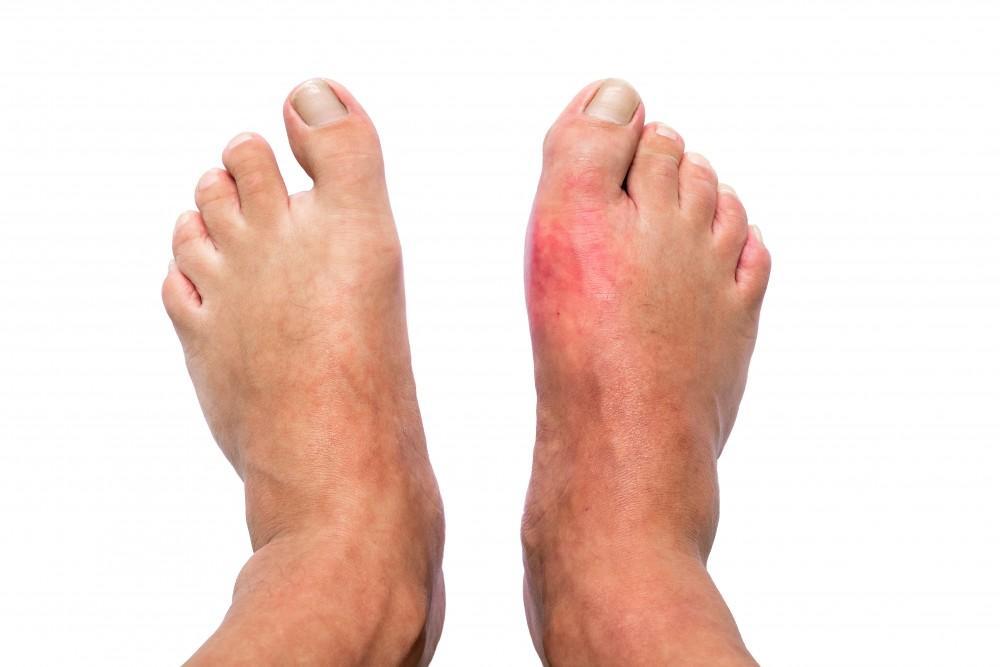
| Joint swelling with fever | Gout or infection |
| Nighttime pain awakening you | Inflammatory arthritis or tumor |
| Sudden loss of joint function | Fracture or severe synovitis |
Tools & Resources
Where can I find a printable checklist?
Many clinics hand out a one-page rheumatology examination checklist. You can also download a free PDF from reputable orthopedic societiesjust search rheumatology examination checklist pdf. Having this sheet in hand helps you remember what to discuss and ensures no joint is overlooked.
Which video tutorials are reliable?
High-quality demonstrations are available on , a site praised by medical students and practitioners alike. Their short clips break down each maneuver, from the squeeze test to gait analysis, making it easy to visualize what will happen during your visit.
Are there apps for ROM measurement?
Yes! Apps like Goniometer Pro and Joint Angle Tracker turn your smartphone into a digital goniometer, letting you record ROM angles at home. This can be useful for tracking progress between appointments, especially if you're doing a structured exercise program.
What peer-reviewed studies support the exam?
The literature underscores that a systematic joint exam improves diagnostic accuracy. For instance, a 2023 article in Rheumatology International showed that using a standardized checklist increased early RA detection by 18% compared with unstructured exams (PMCID10178289).
Common Exam Questions
What is examined during an arthritis physical exam?
The clinician looks at:- Skin and subcutaneous tissue for redness or nodules.
- Joint swelling, deformity, and alignment.
- Temperature and tenderness on palpation.
- Active and passive ROM for each affected joint.
- Muscle strength surrounding the joint.
- Gait, posture, and functional tasks (e.g., rising from a chair).
How long does the exam take?
Typically 1020 minutes. A focused review of a few painful joints can be quicker, while a comprehensive screen of the entire musculoskeletal system may stretch toward the 20-minute mark.
What are the 4 stages of rheumatoid arthritis?
Rheumatoid arthritis commonly progresses through:- Stage 1 Early: Minimal swelling, mild stiffness.
- Stage 2 Moderate: Visible joint swelling, morning stiffness >30 min, early erosions on X-ray.
- Stage 3 Severe: Significant deformities, reduced ROM, notable bone erosion.
- Stage 4 Erosive/Advanced: Irreversible joint damage, functional disability, possible need for joint replacement.
Can I do a self-check at home?
Yes, a gentle self-assessment can be helpful. Try:- Inspecting your hands and knees for swelling or nodules.
- Gently squeezing the MCP joints to see if pain arises.
- Testing finger flexion and extension for crepitus.
If you notice new or worsening findings, schedule a professional examself-checks are a supplement, not a substitute.
What should I ask my doctor during the exam?
Consider these conversation starters:- What does my joint swelling tell you about disease activity?
- Are there any red-flag signs I should watch for at home?
- What lifestyle changes could help protect my joints?
- Can we set specific goals for strength and ROM?
Being prepared shows you're an active partner in your care.
Prep for Appointment
How to create a symptom journal?
Write a small table each day that includes:- Date and time.
- Which joints hurt.
- Pain level (010).
- What made it better or worse (e.g., activity, rest, medication).
- Any morning stiffness duration.
A concise log helps the doctor spot patterns quickly.
What paperwork should I bring?
Gather:- List of all current medications and dosages.
- Recent blood work (CRP, ESR, RF, anti-CCP) if you have them.
- Copies of any recent X-rays or MRIs.
- Insurance card and referral forms (if required).
How to ask for a written plan?
After the exam, politely request a brief summary:- Diagnosis or provisional diagnosis.
- Next steps (labs, imaging, referrals).
- Medication changes with dosage.
- Home exercises or physical therapy recommendationsmore details can be found in our article on osteoporosis physical therapy.
- Follow-up timing.
Having everything on paper reinforces what you discussed and reduces the chance of miscommunication.
Conclusion
Understanding what happens during an arthritis physical exam empowers you to be an active participant in your care. From the quick visual sweep to the nuanced squeeze test, each step is designed to catch early signs, guide treatment, and keep your joints as happy as possible. By preparing a symptom journal, bringing the right paperwork, and asking thoughtful questions, you turn a routine 15-minute visit into a collaborative roadmap toward better joint health. Feel free to download the printable checklist, try a ROM app, or share your own exam stories in the commentsyour experience may help someone else feel more confident before their next appointment.
FAQs
What steps are included in a typical arthritis physical exam?
The exam usually follows inspection, palpation, active and passive range‑of‑motion testing, muscle‑strength grading, gait assessment, and a few special maneuvers to differentiate inflammatory from degenerative joint disease.
How should I prepare for my arthritis physical exam?
Bring a list of current medications, wear loose clothing, write down which joints hurt and when, and carry any recent imaging or lab reports. A brief symptom diary helps the doctor see patterns.
What are the key differences a doctor looks for between rheumatoid arthritis and osteoarthritis?
Rheumatoid arthritis often shows symmetric swelling, warmth, and morning stiffness >30 minutes, while osteoarthritis is usually asymmetric, with crepitus, bony nodes, and stiffness that eases within 10‑15 minutes.
Can an arthritis physical exam be uncomfortable?
Some palpation or range‑of‑motion moves may cause mild soreness, especially if joints are inflamed, but the examiner will adjust pressure to keep discomfort minimal.
What red‑flag signs mean I should seek urgent care?
Severe, rapidly worsening pain, joint swelling with fever, nighttime pain that wakes you, or sudden loss of joint function can indicate infection, crystal arthritis, or other urgent conditions.