Lets cut right to the chase: airway clearance techniques (often shortened to ACTs) are a set of breathingandmovement tricks that help loosen stubborn lung mucus so you can cough or huff it out. Theyre a lifeline for folks battling cysticfibrosis, COPD, bronchiectasis, pneumonia, and other conditions that love to clog the airways.
Do them right and youll notice fewer infections, better oxygen levels, and a sense that youve got a bit more control over each breath. Do them wrong and you might feel extra fatigue or even irritate the lungs. Below is a friendly, stepbystep walkthrough that balances the good with the cautionary because were all about realistic, helpful advice here.
What Are ACTs?
Definition & Core Principle
At its heart, an airway clearance technique is any method that moves mucus from the small airways to the bigger ones where you can expel it. Most ACTs combine three ingredients: a breathing pattern (like huff or deep inhale), a way to make the chest vibrate (percussion, vibrations, or a device), and a prompt to cough. Think of it like shaking a dustcovered bookshelf so the flakes fall off and you can sweep them away.
Who Needs Them?
Anyone whose lungs produce extra, sticky mucus can benefit. The most common groups are:
- Cystic fibrosis (CF) thick mucus is a hallmark. For advice on maintaining healthy personal connections while managing the condition, see cystic fibrosis relationships.
- Chronic obstructive pulmonary disease (COPD) airways narrow, mucus builds up.
- Bronchiectasis permanently dilated airways trap mucus.
- Pneumonia infection can cause a temporary surge in secretions.
RealWorld Snapshot
Take twelveyearold Anna, whos been living with CF since birth. After joining a pulmonary rehab program at JohnsHopkins, she started using the Active Cycle of Breathing Techniques (ACBT) twice a day. Within six months, her hospital admissions dropped from three to one, and she finally felt she could keep up with her friends at school. Stories like Annas underline why experience matters the right technique, practiced consistently, really does move the needle.
Benefits & Risks
Primary Benefits
When you clear mucus effectively, the lungs can:
- Reduce infection risk fewer bacteria love a dry surface.
- Improve oxygen exchange more air reaches the alveoli.
- Boost exercise tolerance you wont get winded as quickly.
- Enhance quality of life breathing feels less like a chore.
Potential Downsides
No technique is perfect. Overdoing percussion can cause bruising, and using a device at too high a pressure may irritate the airway lining. Some people feel dizzy after vigorous huffing, especially if theyre low on fluids. The key is to start gently, listen to your body, and adjust under a clinicians guidance.
Expert Tip
According to a pulmonologist at the Cystic Fibrosis Foundation, Never push-through pain. If a technique leaves you winded or sore, reduce the intensity or switch to a gentler method. Balance is the secret sauce.
Common Techniques
| Technique | Typical UseCase | Key Equipment | Approx. Time |
|---|---|---|---|
| Active Cycle of Breathing Techniques (ACBT) | CF, COPD | None | 1015min |
| Positive Expiratory Pressure (PEP) / Oscillating PEP | CF, bronchiectasis | Flutter, Acapella, Aerobika | 1020min |
| HighFrequency Chest Wall Oscillation (HFCWO) | Severe mucus load | Vest device | 30min |
| Postural Drainage | Pneumonia, acute exacerbations | Bed or chair | 2030min |
| Manual Percussion (Clapping) | All mucushypersecretive diseases | Hands or handheld percussion tool | 510min |
Active Cycle of Breathing Techniques (ACBT)
ACBT is a threestep rhythm: a deep breath in, a relaxed exhale (often with a huff), and a series of forced coughs. Its the goto for many clinicians because it needs no device, just a little practice. The sequence looks like this:
- Breathing control slow, relaxed diaphragmatic breaths for 35 cycles.
- Thoracic expansion a big sniff followed by a gentle huff to move mucus up.
- Forced expiration 23 coughs to clear the loosened material.
Try it out standing up with shoulders relaxed; youll feel a subtle tide moving through your chest.
Positive Expiratory Pressure (PEP) Devices
These handheld gadgets create resistance on the exhale, keeping small airways open longer so mucus can slide outward. Oscillating versions (like the ) add gentle vibrations, which many people find massages the lungs. For CF and bronchiectasis, studies show regular PEP use lowers sputum volume and improves FEV scores.
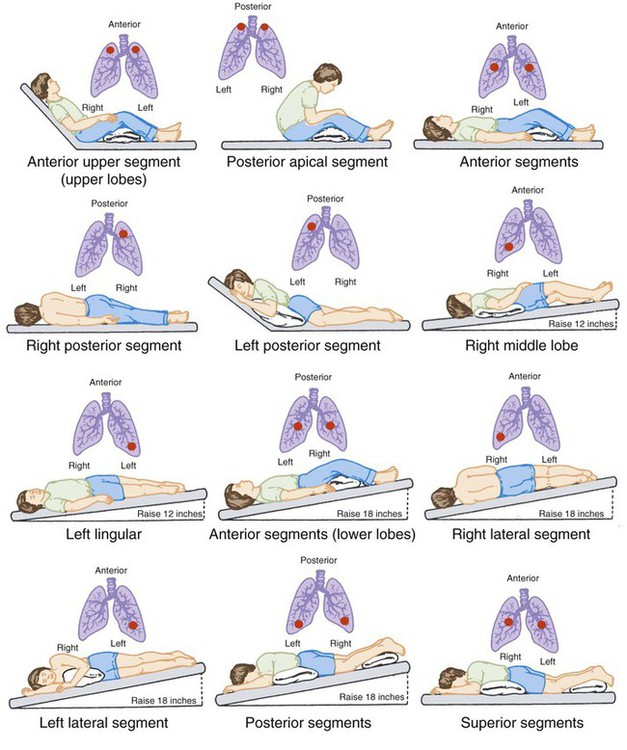
Postural Drainage & Vibration
Think of gravity as an ally. By lying on your side or stomach with the head lower than the chest, mucus drips toward the larger airways. Add a light percussion either manual clapping or a mechanical viber and the mucus loosens faster. This method shines during acute pneumonia when airways are inflamed and you want a lowintensity approach.
HighFrequency Chest Wall Oscillation (HFCWO)
Also called vest therapy, this technique wraps a pneumatic vest around the torso. It delivers rapid, lowamplitude vibrations (520Hz) that shake the chest wall, speeding up mucus transport. Its handy for patients who cant perform active techniques due to fatigue, though its pricier and often covered by insurance only for severe cases.
Choosing the Right Technique
Cystic Fibrosis
Best practice (per the ) is to pair ACBT with an oscillating PEP device. A typical daily routine looks like:
- Morning: 10min ACBT, followed by 5min using the Flutter.
- Midday: Light postural drainage while watching TV.
- Evening: 10min ACBT plus a quick vest session if mucus feels thick.
COPD
Patients often find gentle PEP and soft percussion easier on the lungs. A simple home plan could be:
- Twice daily, 5minute PEP breathing with the Acapella at low resistance.
- After each session, 34 gentle coughs to clear the loosened secretions.
Bronchiectasis
Start with ACBT, then layer on a device if sputum remains thick. If youre looking for extra power, the HFCWO vest can be a gamechanger once or twice a week.
Pneumonia (Acute Phase)
During the first few days, keep it lowkey: seated postural drainage (lying on a slightly inclined pillow) plus gentle huffing. Save the highintensity devices for after the infection settles, when the lungs are less inflamed.
Airway Clearance Devices
Oscillating PEP Devices
Popular models include:
- Flutter a steel tube with a ball that vibrates as you exhale.
- Acapella a mouthpiece with interchangeable valves for adjustable resistance.
- Aerobika a compact, electronic device offering visual feedback.
HighFrequency Chest Wall Oscillation Vests
Brands like and provide adjustable frequencies and are often prescribed for severe CF or bronchiectasis. Theyre noisy but effective; many users treat the sound like a whitenoise machine.
Portable Handheld Percussion Tools
Newer smart percussion devices sync with a phone app, giving you a timer and intensity guide. Theyre handy for travel, though they dont replace a full vest for heavy mucus loads.
Comparison Table
| Device | Cost | Noise Level | Ease of Use | Evidence Grade |
|---|---|---|---|---|
| Flutter (Oscillating PEP) | Low | Quiet | Very easy | Strong |
| Acapella (Oscillating PEP) | LowMedium | Quiet | Easy | Strong |
| Aerobika (Electronic PEP) | Medium | Moderate | Easy with visual feedback | ModerateStrong |
| VestAir (HFCWO) | High | Loud | Requires setup | Strong |
| Handheld Smart Percussion | Medium | Quiet | Easy | Emerging |
StepbyStep Airway Clearance Exercises
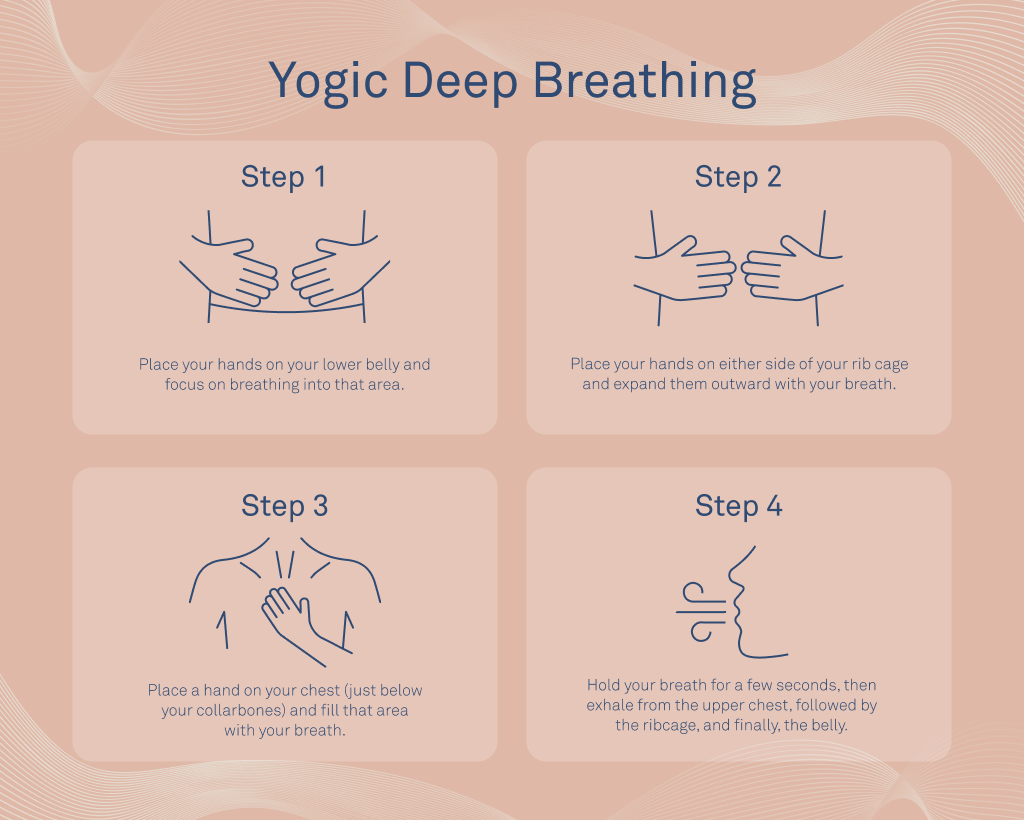
WarmUp Breathing (5min)
Start with diaphragmatic breathing: place one hand on your belly, inhale through the nose for a count of four, feel the belly rise, then exhale slowly through pursed lips for a count of six. This relaxes the accessory muscles and primes the lungs for the main technique.
Core ACT Sequence (Choose One)
Pick the method that matches your condition ACBT, PEP, or postural drainage and follow the numbered steps.
- Breathing control 35 relaxed breaths (nose in, mouth out).
- Thoracic expansion Take a deep sniff to the bottom of the lungs, then perform a gentle huff (open mouth, short forceful exhale) for 23 seconds.
- Forced cough Immediately after the huff, do 23 mediumstrength coughs, aiming to bring the mucus up.
- Repeat Cycle through steps 13 for 810 minutes, adjusting intensity based on comfort.
CoolDown (2min)
Finish with a few slow, deep breaths, letting the shoulders drop. This helps the airway muscles relax and reduces the chance of postexercise wheeze.
Helpful Resources
For visual learners, the walk you through each step. You can also download a printable from PhysioPedia for quick reference during home practice.
Resources & PDFs
Official PDFs
Two topquality PDFs worth bookmarking:
- European Respiratory Societys Airway Clearance Techniques and Devices a comprehensive guide with evidence tables.
- JohnsHopkins CF Centers Daily Airway Clearance Routine a concise, printable cheatsheet.
Trusted Sites
When you need the latest research, head to:
- The for peerreviewed studies.
- The for conditionspecific guidelines.
Apps & Tracking Tools
Apps like MyAirwayGuide let you log each ACT session, track sputum volume, and share data with your therapist. A simple log helps you see patterns (maybe youre clearing more on days you stay hydrated something to celebrate!).
Conclusion
Airway clearance techniques are not a onesizefitsall miracle; theyre a toolbox you can customize to match your lungs, lifestyle, and medical advice. When you pair the right method (or combo of methods) with consistent practice, youll notice fewer infections, easier breathing, and a sense of empowerment over a condition that can feel overwhelming.
Remember, the safest and most effective plan is built with your healthcare team. Share your experiences, ask questions, and dont shy away from tweaking the routine as your health evolves. Got a favorite technique thats helped you? Or a question about using a particular device? Drop a comment below wed love to hear your story and keep the conversation going.
FAQs
What exactly are airway clearance techniques (ACTs)?
ACTs are breathing and movement methods that move mucus from the small airways to the larger ones so it can be expelled by coughing or huffing.
How often should I perform ACTs?
Most clinicians recommend doing ACTs at least twice daily, but the exact frequency depends on your condition, mucus load, and personal tolerance.
Can I use ACTs without any equipment?
Yes. Techniques like the Active Cycle of Breathing Techniques (ACBT) require only your breath and a comfortable position, making them ideal for home use.
Are there risks to using devices like the vest or oscillating PEP?
When used correctly, risks are low. Too much pressure or intensity can cause airway irritation, bruising, or fatigue, so always follow your therapist’s settings.
Which ACT is best for cystic fibrosis?
Combining ACBT with an oscillating PEP device (e.g., Flutter®, Acapella®) is the current gold‑standard for most people with cystic fibrosis.