When the liver cant do its job, bloodclotting power drops fast thats why doctors often give transfusions to keep you from bleeding out.
But a transfusion isnt a free pass; it comes with both benefits and risks, and its only used when the balance tips toward dangerous bleeding or severe anemia.
LiverBleeding Connection
What role does the liver play in clotting?
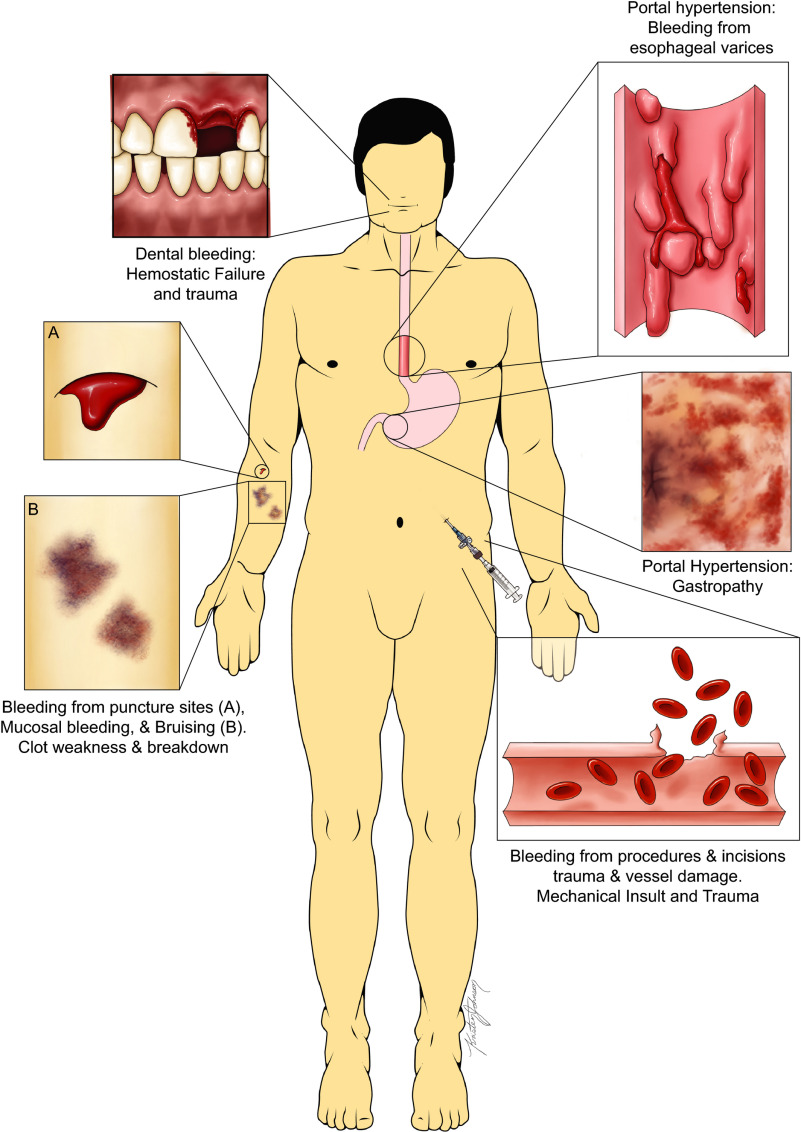
The liver is the bodys clotfactory. It produces most of the clotting factors (II, VII, IX, X, and fibrinogen) and the hormone thrombopoietin, which tells the bone marrow to make platelets. Without these, even a tiny cut can turn into a serious bleed.
Why does liver failure cause coagulopathy?
When the liver is damaged, several things go wrong:
- Less production of clotting factors.
- Platelet numbers drop because thrombopoietin falls and the spleen hoards platelets.
- Portal hypertension squeezes blood flow, worsening platelet sequestration.
- The balance of fibrinolysis (breaking down clots) is thrown off.
All of this means the blood cant clot when it needs to, and thats the main reason a transfusion may become lifesaving.
Which blood component is responsible for clotting the blood?
Its the clotting factors proteins largely made by the liver. When theyre low, the bodys ability to seal a wound drops dramatically.
When Transfusion Is Needed
Acute massive GI bleeding in cirrhosis
Gastrointestinal bleeding is common in cirrhosis because varices (enlarged veins) can rupture. Most guidelines suggest a transfusion trigger of hemoglobin <7g/dL, or <8g/dL if youre actively bleeding. Raising the hemoglobin helps carry oxygen to vital organs while you treat the bleed.
Specific liverrelated conditions that often need transfusion
Here are a few scenarios you mightve heard about:
- Alcoholic liver disease: Why would an alcoholic need a blood transfusion? often because an alcoholinduced ulcer or variceal bleed creates rapid blood loss.
- Endstage liver disease (ESLD): Patients awaiting transplant may need a bridge transfusion to keep them stable.
- Hepatic encephalopathy with coagulopathy: Before a neurocritical procedure, doctors may give plasma to correct clotting.
Practical checklist for clinicians and patients
| Situation | Recommended product | Goal |
|---|---|---|
| Severe anemia | Packed red blood cells (PRBC) | Raise Hb 8g/dL |
| Platelets 50k/L | Platelet concentrate | Prevent procedural bleeding |
| Prolonged PT/INR >1.5 | Fresh frozen plasma (FFP) | Supply clotting factors |
| Ongoing hemorrhage | Cryoprecipitate (fibrinogen) | Raise fibrinogen >150mg/dL |
Realworld case vignette
Imagine a 48yearold man with alcoholic cirrhosis who shows up with melena and a hemoglobin of 6.4g/dL. He receives two units of PRBC and a unit of FFP. Within an hour his blood pressure steadies, and endoscopy later shows a small variceal bleed that can be banded. The transfusion bought him the time needed for a definitive procedure, illustrating both the lifesaving potential and the need for careful monitoring.
Types of Blood Products
Packed red blood cells (PRBC)
These are your oxygen couriers. Theyre used when anemia threatens tissue oxygenation.
Fresh frozen plasma (FFP)
FFP carries all clotting factors. Its the goto when INR is high and bleeding is happening.
Platelet concentrates
When platelets dip below 50k/L, you risk spontaneous bleed. A platelet transfusion can halt that.
Cryoprecipitate
Contains fibrinogen and factorVIII, useful if fibrinogen falls under 150mg/dL during massive hemorrhage.
Pros & cons at a glance
| Product | Benefit | Risk | Typical indication in liver failure |
|---|---|---|---|
| PRBC | Increases O delivery | TRALI, volume overload | Hb<78g/dL |
| FFP | Replaces all clotting factors | Allergic reactions, TACO | INR>1.5 with active bleed |
| Platelets | Stops plateletrelated bleeding | Immune reactions | Platelets<50k/L |
| Cryo | Boosts fibrinogen quickly | Hypercoagulability | Fibrinogen<150mg/dL |
Balancing Benefits and Risks
Potential harms of transfusion in liver patients
Transfusing isnt without downsides. Volume overload can raise portal pressure, potentially worsening variceal bleeding. Theres also a risk of transfusionassociated circulatory overload (TACO), infections, and a higher chance of posttransplant complications. A 2023 study in found that aggressive transfusion strategies increased rebleeding rates.
How clinicians decide if and when to transfuse
Decisionmaking blends objective numbers with the patients story. Doctors look at hemodynamics, ongoing bleed, comorbidities, and the trend of labs. Many hospitals now use pointofcare viscoelastic testing (TEG/ROTEM) to tailor exactly which component is missing, instead of reflexively giving everything.
Simple algorithm (you could sketch on a napkin)
- Is the patient actively bleeding? Yes Check Hb, INR, Platelets.
- Hb<7g/dL PRBC.
- INR>1.5 FFP.
- Platelets<50k Platelets.
- Fibrinogen<150mg/dL Cryoprecipitate.
- Reassess after each unit; stop when goals are met.
Frequently Asked Questions
Why do liver failure patients need blood transfusions?
Because a failing liver cant make enough clotting factors or platelets, leading to dangerous bleeding. Transfusions replace what the liver cant, buying time for other treatments.
Can blood transfusion cure liver failure?
No. Its a supportive bridge, not a cure. The underlying liver disease still needs specific therapy whether thats medication, lifestyle change, or transplantation.
Whats the difference between PRBC and FFP?
PRBC gives you red cells for oxygen transport. FFP is a soup of plasma proteins, mainly clotting factors, used when the blood wont clot properly.
Are there alternatives to transfusion?
In some cases, iron supplements, erythropoietinstimulating agents, or medications like tranexamic acid can reduce the need for blood. However, in acute, lifethreatening bleeds, a transfusion is usually the fastest answer. For patients managing chronic liver conditions at home, attention to diet and supplements recommended for liver healthsuch as careful choices among ulcerative colitis supplements when relevant comorbid GI disease existscan be part of broader care planning with a hepatologist or gastroenterologist.
When should I call emergency services?
If you notice bright red vomit, black tarry stools, sudden dizziness, rapid heart rate, or a feeling that youre going faint, treat it as an emergency. Those are redflag signs that a bleed may be severe.
Signs of Severe Bleeding
Key warning signs in liver failure
Watch for melena or hematemesis, sudden drop in blood pressure, a racing pulse, confusion that gets worse quickly (often a sign of hepatic encephalopathy getting worse), and unexplained pallor. These clues signal that the body is losing blood faster than it can replace it.
How transfusion can buy time vs. when its too late
When caught early, a transfusion can reverse anemia and restore clotting, allowing doctors to perform endoscopy, medication, or surgery. If the bleed is massive and the patient is already in shock, even a rapid transfusion may not prevent organ damage. Thats why early recognition is vital.
Building Trust with Sources
All the information above is drawn from reputable institutions: the explains how liver disease disrupts clotting, while peerreviewed articles in journals like American Journal of Medicine and Wiley provide the latest thresholds for transfusion. When you read a medical article, always look for citations from these kinds of trusted sources.
TakeAway Checklist for Patients & Caregivers
- Know your baseline labs hemoglobin, INR, platelets.
- Watch for bleeding signs (vomit blood, black stool, sudden weakness).
- Ask your doctor about transfusion thresholds before a procedure.
- Understand the risks: fluid overload, infection, allergic reactions.
- Keep a copy of any recent transfusion record it helps new clinicians make better decisions.
Facing liver failure is overwhelming, but you dont have to navigate it alone. Talk openly with your hepatology team, ask questions about when a transfusion is truly needed, and keep an eye on those warning signs. A welltimed transfusion can be the difference between a rough night in the hospital and a steady path toward recovery or a safe bridge to transplant.
Conclusion
Liver failure disrupts the bodys natural clotting system, making bleeding a real danger. Blood transfusionswhether packed red cells, plasma, platelets, or cryoprecipitateserve as a lifesaving bridge until the underlying liver issue can be treated or stabilized. Yet they carry notable risks, so clinicians weigh benefits against potential harms, guided by evidencebased thresholds and each patients unique story. If you or a loved one are navigating liver disease, keep the conversation open with your care team about when transfusion is appropriate, what alternatives exist, and how to spot warning signs early. Staying informed, staying proactive, and staying connected with trusted experts can make all the difference.
FAQs
Why do liver failure patients need blood transfusions?
Liver failure patients need blood transfusions because their liver can't produce enough clotting factors or platelets, making them prone to dangerous bleeding.
What blood products are used for liver failure patients?
Common blood products include packed red blood cells, fresh frozen plasma, platelet concentrates, and cryoprecipitate, depending on the specific deficiency.
When is a transfusion necessary for someone with liver failure?
A transfusion is needed when there's severe anemia, low platelets, prolonged clotting times, or active bleeding, especially during procedures or GI bleeds.
Can blood transfusions cure liver failure?
No, blood transfusions are supportive care and do not cure liver failure; they help manage bleeding while treating the underlying liver disease.
Are there risks to blood transfusions in liver failure patients?
Yes, risks include volume overload, infections, allergic reactions, and increased portal pressure, which can worsen variceal bleeding.