Short answer: If the swelling appears suddenly, is painful, warm, red, or comes with chest pain, shortness of breath, fever, or a feeling of heaviness in the calf, call 911 or head straight to the emergency department.
For gradual, symmetric swelling without alarming signs, you can usually manage it at home first and schedule a visit with your primarycare doctor within a few days.
Quick Answer
Imagine you wake up, lift your foot, and it feels like a small balloon is pressing against your ankle. That wow, thats a lot of swelling moment is a signal to act fast if any of the following are true:
- Sudden oneleg swelling with sharp calf pain.
- Red, hot skin that feels like a fever on the leg.
- Chest tightness, difficulty breathing, or coughing up blood.
- Fever over 38C (100.4F) with swelling.
These are redflag symptoms that could mean a blood clot, infection, or a heartlung problemsituations that demand immediate medical attention.
If none of those are present, keep reading. Youll learn why most swelling isnt a lifethreatening emergency and what you can do right now to feel better.
Why Swelling Happens
What is edema?
Edema is the medical term for fluid that leaks out of blood vessels and pools in the tissue. Your body uses fluid to deliver nutrients and remove waste, but when the balance tips, you get that puffy feeling. A little edema after a long flight is normal; persistent swelling can be a sign that something deeper is offbalance.
Common causes of swelling from the knee down
Several conditions can make your feet and lower legs puff up:
- Heart failure: The heart cant pump blood efficiently, so fluid backs up in the legs. If you suspect worsening cardiac symptoms, resources about DI heart failure explain typical signs and when to seek care.
- Kidney disease: The kidneys struggle to remove excess sodium and water.
- Liver cirrhosis: Low albumin levels cause fluid to leak out of vessels.
- Venous insufficiency: Veins cant push blood back to the heart, leading to pooling.
- Lymphedema: The lymphatic system is blocked or damaged.
- Medication sideeffects: Some blood pressure pills, steroids, and antidepressants can retain fluid.
- Deepvein thrombosis (DVT): A clot forms in a deep vein, often the calf, and blocks flow.
That answer to what causes swollen legs from the knee down? covers the most common culprits, but the exact cause always needs a professionals eye.
Whos at higher risk?
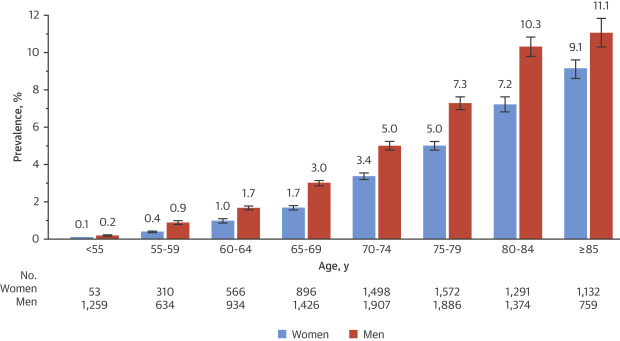
Older adultsespecially swollen legs in elderly female patientsare more prone because veins weaken with age and many take medications that affect fluid balance. Pregnancy, obesity, and a sedentary lifestyle also raise the odds.
According to a 2024 , about 15% of adults over 65 experience chronic edema at some point.
Red Flag Symptoms
When you notice swelling, scan for the following red flags. If any appear, treat it as an emergency.
| Symptom | Likely Cause | Action |
|---|---|---|
| Sudden oneleg swelling + calf pain | Deepvein thrombosis | Call 911 or go to the ER immediately |
| Swelling + chest pain / shortness of breath | Heart failure or pulmonary embolism | Emergency care required |
| Gradual bilateral swelling, no pain | Lowgrade edema (e.g., medication, mild venous insufficiency) | Schedule a primarycare appointment |
| Red, warm skin + fever | Cellulitis or infection | Seek urgent care or ER |
Sudden, unilateral swelling
A clot in the calf can grow quickly. The stress that early detection saves lives, so dont wait to see if it gets better.
Swelling with systemic signs
Chest tightness, a racing heartbeat, or breathlessness means the fluid problem isnt staying in your legsits affecting your whole circulatory system. Thats a classic can edema kill you? scenario, and yes, in severe cases it can.
Pain, discoloration, or open sores
If the skin turns bluepurple, feels like its on fire, or you notice a wound that wont heal, you could be dealing with cellulitis, compartment syndrome, or a severe venous ulcer. All of these merit urgent treatment.
When to Call PCP
Not every puffedup foot needs a copy of ER TV drama. Heres when a regular doctor visit is the right move:
Persistent but nonurgent swelling
Swelling that worsens slowly over weeks, feels heavy but not painful, and appears on both legs usually points to a chronic conditionlike mild heart insufficiency or medicationinduced fluid retention. Your PCP can adjust meds, order blood work, or refer you to a specialist.
Managing underlying conditions
If you already have heart, kidney, or liver disease, swelling may be a flareup. Your doctor can tweak diuretics, advise on salt intake, and monitor organ function. This ongoing care often prevents the swelling from becoming an emergency.
Lifestyle tweaks to reduce edema
Simple changes can make a big difference. Below are some evidencebased habits:
- Elevate your legs above heart level for 20 minutes a few times a day.
- Wear compression stockings (1530mmHg for mild, 3040mmHg for moderate).
- Cut back on sodiumaim for less than 2g per day.
- Stay active. Gentle ankle pumps and short walks keep blood moving.
- Hydrate wisely. Drinking enough water helps kidneys flush excess fluid; a cup of cucumbermint water can be refreshing.
Home Remedies & Care
Elevation & positioning techniques
Lie on a couch or bed, prop your legs on several pillows, and keep them higher than your heart. Even a halfhour session can drain a noticeable amount of fluid.
Compression therapy
Compression stockings compress the veins, forcing blood to flow upward. Choose the correct pressure levelyour doctor can measure your calf circumference to find the right fit. Put them on in the morning before swelling starts; they work best when worn all day.
Dietary & fluid strategies
Salt is the main villain. Try seasoning with herbs, lemon zest, or vinegar instead. Foods rich in potassiumbananas, oranges, sweet potatoeshelp counterbalance sodium. And yes, what to drink to reduce swelling in feet? Plain water is your best ally; aim for 2L a day unless your doctor says otherwise.
Gentle exercises & stretches
Daily ankle pumps (flex and point the foot) for 2minutes, calf raises, and a short walk can dramatically improve circulation. The key is consistency, not intensity.
3Day FastRelief Plan
- Morning: 5minute ankle pumps, then elevate for 20minutes.
- Midday: Slip on 2030mmHg compression stockings, walk around the house for 1015minutes.
- Evening: Lowsalt dinner, drink a glass of cucumber water, elevate legs again before bed.
Within a few days you should notice the heaviness lift, though the plan isnt a substitute for medical evaluation if red flags appear.
RealWorld Stories
Case study: 72yearold woman with sudden calf swelling
Maria (name changed for privacy) woke up with a tight, painful right calf that felt like a balloon. She also felt a little short of breath. Her daughter drove her to the ER, where an ultrasound confirmed a DVT. She received anticoagulants and was discharged with compression stockings and a followup appointment. Marias story illustrates why when should you go to the hospital for swollen feet and legs? has a clear answerrapid, focused action can prevent a clot from traveling to the lungs.
Reader tip: Grandmas edema breakthrough
One of our readers shared how her 80yearold mother finally saw improvement after switching to a lowsalt diet, adding a daily 30minute walk, and wearing properly fitted compression socks. The swelling went from massive to manageable in about three weeks. Realworld anecdotes like this remind us that lifestyle changes, while not a cureall, can be powerful allies.
Choosing Healthcare Setting
ER vs. urgentcare vs. telemedicine
For true emergenciessudden oneleg swelling, chest pain, or feverhead straight to the emergency department. Urgentcare clinics can handle moderate issues like cellulitis or mild DVT suspicion when youre not in immediate danger, but they might not have ultrasound equipment on site. Telemedicine is great for followup questions about diet, medication sideeffects, or when you need reassurance that home care is safe.
What to expect during a hospital evaluation
Once youre in the ER, the team will:
- Check vital signs and look for signs of infection or heart strain.
- Run a Ddimer blood test if DVT is suspected.
- Perform a bedside ultrasound of the leg veins.
- Order basic labs (renal function, liver enzymes, BNP) to assess organ involvement.
- Decide whether you need admission, medication, or can go home with a clear plan.
BottomLine Checklist
- Redflag list: Sudden swelling, pain, redness, warmth, fever, chest pain, shortness of breath Go to the hospital now.
- When to call 911: Any combination of the above with difficulty breathing or severe chest discomfort.
- When to see your PCP: Gradual, painless swelling lasting more than a week, especially if you have heart, kidney, or liver disease.
- Homecare steps: Elevate, compress, hydrate, lowsalt diet, gentle exercise.
Conclusion
Understanding the difference between scaryquickonset swelling and slowandsteady fluid buildup is the key to deciding when you should go to the hospital for swollen feet and legs. Redflag symptoms demand immediate emergency care, while most other cases can be tamed with lifestyle tweaks and a timely doctors visit. Trust your bodys signals, stay curious, and dont hesitate to reach out for professional help when you need it. If youve ever faced swelling yourself, what strategies worked for you? Share your experience belowyour story might be the lifeline someone else is searching for.
FAQs
When should I go to the hospital for swollen feet and legs?
If swelling is sudden, painful, warm, red, or accompanied by chest pain, shortness of breath, fever, or heaviness in the calf, go to the hospital immediately.
Can swollen feet and legs be a sign of a blood clot?
Yes, sudden swelling in one leg with sharp calf pain can indicate deep vein thrombosis (DVT), a serious condition needing emergency care.
What symptoms with swollen legs require calling 911?
Call 911 if you have swollen legs along with chest pain, difficulty breathing, coughing up blood, or severe dizziness.
When is it safe to manage swollen legs at home?
Gradual, painless, symmetric swelling without alarming symptoms can usually be managed at home with lifestyle changes and seen by a doctor later.
What lifestyle changes can help reduce swelling in feet and legs?
Elevate legs above heart level, wear compression stockings, reduce salt intake, stay active with gentle exercises, and stay well hydrated.