If your vision suddenly gets blurry, a dark spot appears, or one eye feels like its slipping into a fog, dont try to wait it out. The fastest thing you can do is treat it as an emergencycall 911 or head straight to the nearest ER. Acting quickly can be the difference between a full recovery and permanent loss.
Once the immediate danger is handled, the next step is to understand why its happening and how you can stop further damage. Below youll find a friendly, stepbystep guide that tackles the what to do when you are losing your eyesight question from every angleemergency care, diagnosis, prevention, and everyday coping.
RedFlag Warning Signs
What subtle symptoms should never be ignored?
Even if the change feels small, certain signs scream for attention:
- Sudden blurry spot or floaters that dont go away
- Flashing lights, especially around the edges of your vision
- Loss of peripheral vision (you cant see things to the side)
- Pain that feels deep, pressurelike, or throbbing
- Rapid changes in how colors appear
When any of these pop up, grab your phone, call emergency services, and avoid driving yourself. Time is visioncritical.
How can I tell if the loss is an emergency?
Think of it like a fire alarm. If the alarm is loud (pain, sudden total blackout), you evacuate now. If its a faint beep (gradual blur), you still need a professional, but you can schedule a sameday appointment.
Quick What to Do NOW Checklist
| Situation | Action |
|---|---|
| Sudden, painless loss in one eye | Call 911 or go to ER immediately |
| Gradual blur over weeks | Schedule an ophthalmology appointment within 2448 hrs |
| Accompanying severe eye pain | Treat as emergency seek ER care |
| Temporary darkness after a migraine | Rest, note triggers, see doctor if it recurs |
Why does a singleeye loss feel different from loss in both eyes?
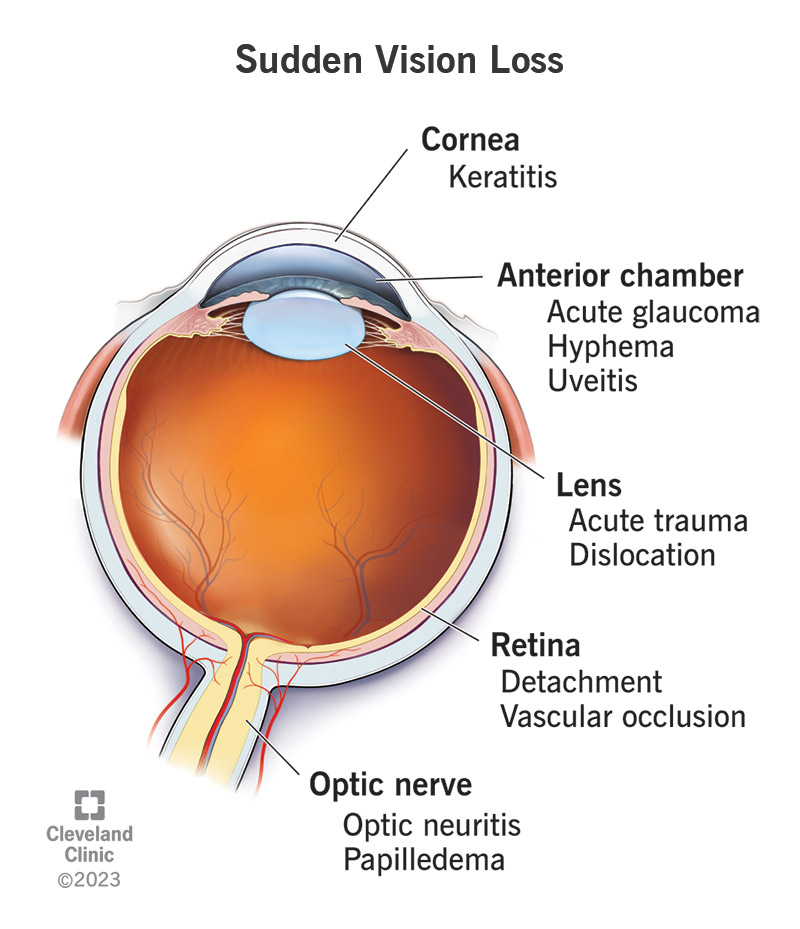
When only one eye is affected, the problem often lies in the retina, optic nerve, or blood vessels feeding that eye. When both eyes go dark, the brains visual pathways or systemic issues (like severe low blood pressure) are usually to blame. Knowing the difference guides the doctors toward the right tests.
Common Causes of Vision Loss
What causes sudden, painless loss of vision in one eye?
The most frequent culprits are vascular eventsthink of a tiny traffic jam in the eyes blood supply. A central retinal artery occlusion (CRAO) blocks oxygen and can cause immediate blackout. Retinal detachment, where the lightsensing layer pulls away, also appears painless at first but rapidly worsens.
SidebySide Comparison
| Cause | Typical Symptoms | Urgency |
|---|---|---|
| Central Retinal Artery Occlusion | Sudden, painless, total loss in one eye | Emergency (minutes to hours) |
| Retinal Detachment | Flashes, floaters, shadow/curtain effect | Urgent (within 24 hrs) |
| Optic Neuritis | Pain on eye movement, color loss | Urgent but not immediate |
What are the reasons for sudden painful loss of vision?
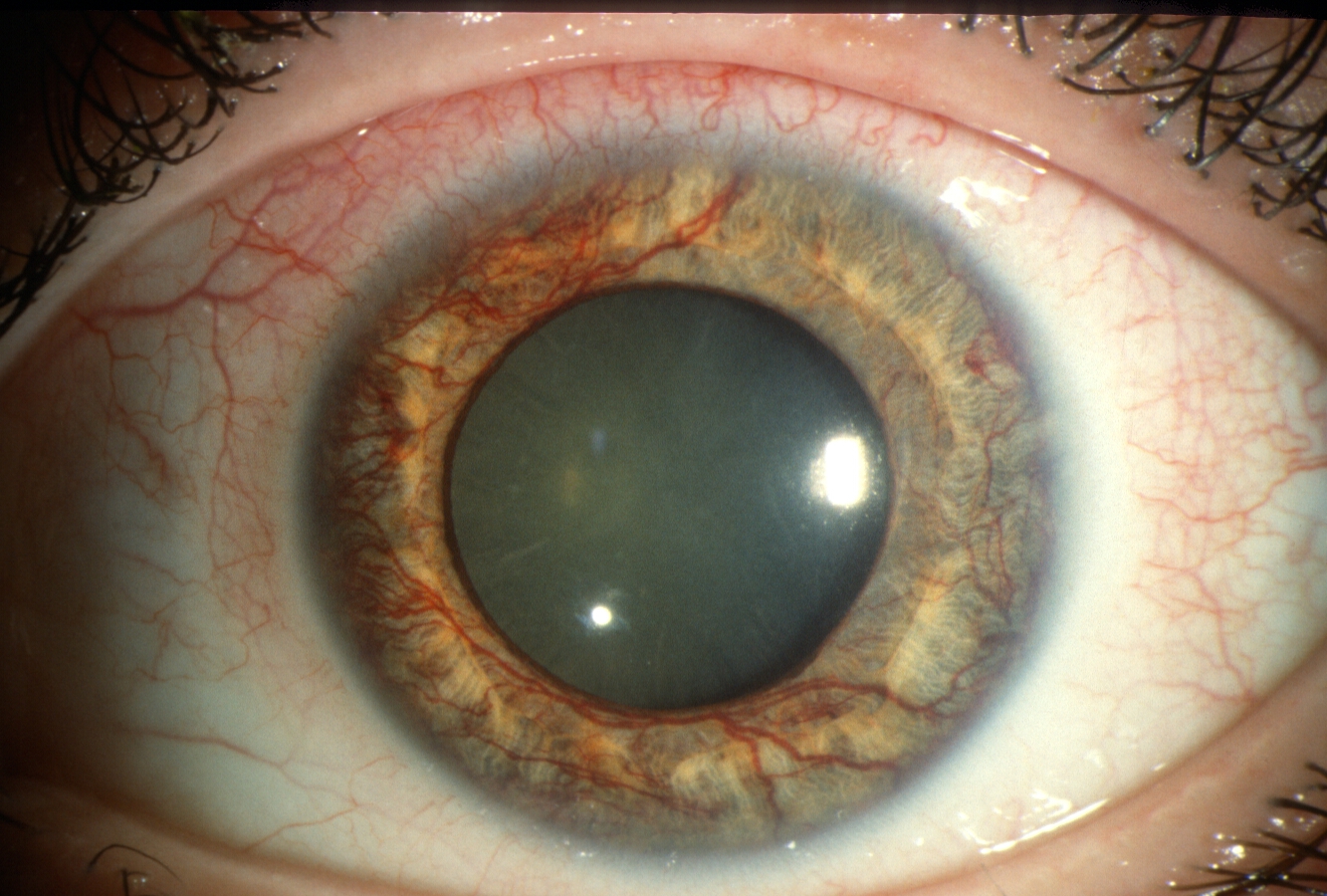
Pain usually indicates pressure or inflammation. Acute angleclosure glaucomawhere fluid cant drain and pressure spikescauses severe eye pain, halos around lights, and a rapid loss of vision. Ocular trauma or severe infections (endophthalmitis) also fit this pattern.
What can cause temporary blindness in both eyes?
Temporary blacking out of both eyes can happen during a migraine aura, a brief drop in blood pressure, or a transient ischemic attack (TIA). These episodes are scary but often resolve in minutes to hours. Still, they are warning signs that you should discuss with a doctor.
Which nutrient deficiencies lead to vision loss?
Deficiencies dont always make headlines, but they matter. Vitamin A deficiency can cause night blindness and, in severe cases, corneal ulcers. Low B12 can affect the optic nerve, and omega3 fatty acids support retinal health. If you suspect a dietrelated issue, a simple blood test can confirm it.
How do chronic diseases like diabetes and hypertension contribute?
High blood sugar damages tiny blood vessels in the retinaa condition called diabetic retinopathy. Uncontrolled hypertension can cause bleeding or swelling in the retina, known as hypertensive retinopathy. Managing these systemic conditions is often the most effective way to stop vision loss.
Immediate Action Plan What to Do Right Now
Should I call 911 or go to an ER?
Yesif you experience sudden loss, especially with pain, color loss, or a curtain effect. Emergency departments have the imaging (like OCT and fluorescein angiography) needed to diagnose retinal artery blockages within the critical window.
What firstaid steps can I take while waiting for help?
Keep the affected eye covered with a loose, clean clothdont press on it. Stay seated, avoid bright lights, and try not to rub the eye. Write down the exact time the symptoms started; this timeline is gold for doctors.
Can I use eye drops or overthecounter meds?
Only if a professional has prescribed them. Some drops (like those for glaucoma) can lower pressure quickly, but using the wrong medication can worsen the problem. When in doubt, wait for the doctor.
What information should I give the doctor?
Be ready to share:
- When the symptoms began (exact time if possible)
- Any recent injuries, infections, or head trauma
- Current medications, supplements, and recent changes
- Medical historydiabetes, hypertension, migraines
- Family eyehealth history (glaucoma, macular degeneration)
Professional Care Steps
Which specialists should I see?
Start with an ophthalmologistpreferably a retina specialist if the problem looks vascular. A neuroophthalmologist can help when the brains visual pathways are involved. Optometrists are great for routine followups and lowvision aids.
What tests will diagnose the problem?
Doctors use a toolbox that may include:
- Dilated eye exam: Lets the doctor see the retina and optic nerve.
- Optical Coherence Tomography (OCT): A noninvasive scan that shows crosssectional images of the retina.
- Fluorescein angiography: A dye injected into a vein highlights blood flow in the eye.
- MRI/CT scan: When a neurological cause (like a stroke) is suspected.
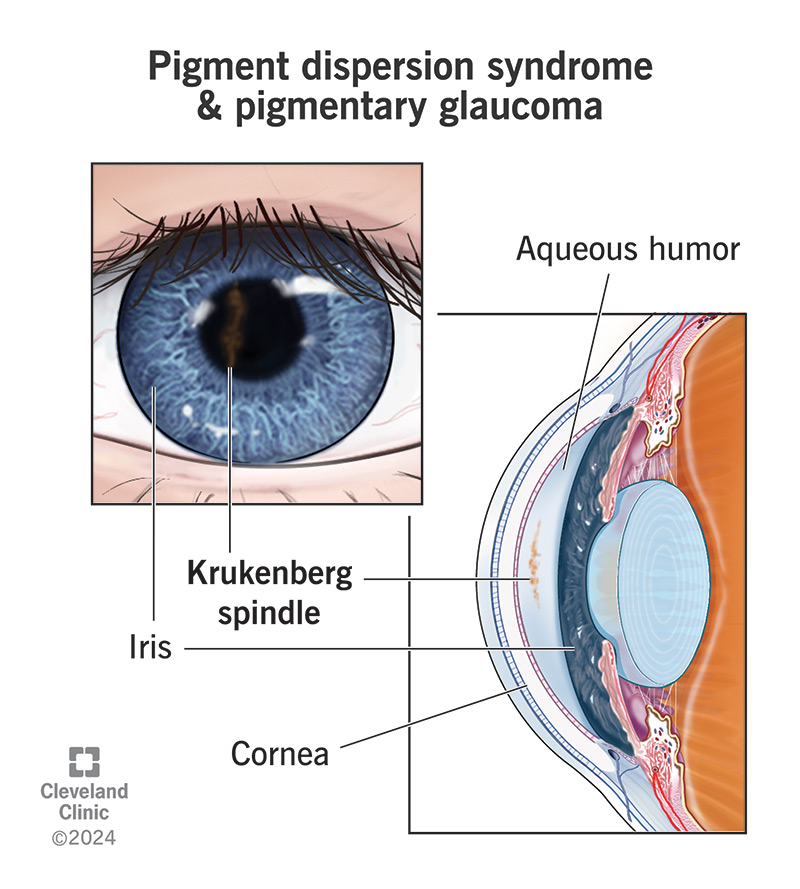
For patients with sudden peripheral vision loss or tunnellike symptoms, consider evaluation for conditions that cause tunnel vision glaucoma, which can be a clue to advanced optic nerve or retinal disease.
How soon should I schedule a followup?
For emergencies, youll be seen within the same day. For nonurgent cases, aim for an appointment within one to two weeks. Consistent followup is keysome conditions, like diabetic retinopathy, progress silently.
What questions should I ask my doctor?
Bring a short list:
- What is the most likely cause?
- Is the condition reversible?
- What treatment options are available now and in the future?
- What lifestyle changes can help?
- Should I be screened for systemic diseases?
Prevent Further Vision Loss Lifestyle & Medical Steps
How can I stop vision loss from getting worse?
Control the big three: blood sugar, blood pressure, and cholesterol. Smoking quits, regular exercise, and a balanced diet are proven to stop vision loss from accelerating.
Which nutrients protect my eyes?
Research from the highlights lutein, zeaxanthin, vitamins C and E, and omega3 fatty acids as eyeprotective powerhouses. Think leafy greens, colorful veggies, fatty fish, and nuts.
Do eyedrop medications help?
Prescription dropslike those for glaucoma or dry eyeare essential when a doctor recommends them. Overthecounter lubricants can soothe irritation but wont treat underlying disease.
What regular screenings should I have?
If youre over 40, schedule an annual dilated eye exam. If you have diabetes, get screened every six months. Highrisk family histories may warrant earlier or more frequent checks.
Coping With Vision Loss Emotional & Practical Support
How do I handle the emotional impact?
Loss of sight can feel like losing a piece of yourself. Its okay to grieve, feel angry, or even laugh at the absurdity of it all. Talking to a therapist or joining a support grouplike those listed by the provides a community that truly understands.
What lowvision aids can improve daily life?
Technology is a gift here:
- Handheld magnifiers for reading labels
- Screenreading software (VoiceOver, NVDA)
- Highcontrast keyboards and mouse pointers
- Tactile markers for appliances and stove knobs
- Smartphone apps that read text aloud or identify colors
How can I stay safe at home?
Simple tweaks go a long way. Keep pathways free of clutter, use nightlights in hallways, label medicine bottles with large print, and consider a vision buddysomeone you call when you need an extra pair of eyes for tasks like driving or grocery shopping.
What resources exist for independence?
Lowvision rehabilitation programs, often run through hospitals or universities, teach you skills like eccentric viewing (using the healthier part of your retina) and adaptive cooking. Many of these services are covered by insurance or offered at low cost.
Conclusion
When you notice your sight slipping, the fastest responsecalling emergency services and seeking professional carecan preserve your vision. Understanding the underlying cause, whether its a vascular event, nutrient deficiency, or chronic disease, guides you toward effective treatment. Longterm, controlling blood sugar, blood pressure, and adopting an eyehealthy diet are the best strategies to stop vision loss from progressing.
Beyond the medical side, emotional support and practical adaptations make daily life not just manageable but rewarding. Youre not alone in this journey; doctors, therapists, support groups, and a handful of clever tools are all on your side. So, if you or someone you love is facing vision changes, act now, get checked, and explore the resources that keep you living fully.
FAQs
What should I do if I suddenly lose vision in one eye?
Call 911 or go to the emergency room immediately. Sudden vision loss in one eye is a medical emergency and requires immediate diagnosis and treatment to prevent permanent damage.
Are there warning signs that indicate urgent eye problems?
Yes. Sudden blurry spots, floaters, flashing lights, loss of side vision, severe eye pain, or rapid color changes are red-flag symptoms that require emergency medical attention.
Can gradual vision loss be treated differently than sudden loss?
Gradual vision loss over weeks should prompt prompt scheduling of an ophthalmology appointment within 24–48 hours, while sudden changes with pain or total vision blackout require emergency care.
Which specialists should I see for vision loss?
Start with an ophthalmologist, especially a retina specialist for vascular causes. Neuro-ophthalmologists handle brain-related vision issues. Optometrists assist with routine care and low vision aids.
How can I prevent further vision loss if diagnosed with chronic eye disease?
Manage systemic conditions like diabetes and hypertension, maintain a healthy lifestyle including diet rich in lutein and omega-3s, quit smoking, and attend regular eye screenings.